Baby gulping when not feeding
Choking, Gulping, Gagging - Symptoms
by Jan Gambino Patient Expert
Does your baby experience choking, gulping, gagging and coughing during a feeding? How about arching and fussiness? Sound like your baby? Then read on. These worrisome noises from the tiny digestive system of your baby may signal a swallowing problem, GERD or both.
Recently, I attended the North American Society of Pediatric Gastroenterology, Hepatology and Nutrition (NASPGHAN) meeting to learn more about pediatric Gastroesophageal Reflux Disease (GERD). I met a team of doctors and speech language pathologists who wanted to find out how common dysphagia (a medical term for a swallowing disorder) was in a group of babies diagnosed with GERD. The study was presented at the meeting and the results were surprising.
GERD and dysphagia have overlapping symptoms including: arching, gagging, coughing and feeding refusal.
The researchers identified a group of babies who had been diagnosed with GERD.
Out of the large group, the researchers studied a smaller group with symptoms of both GERD and dysphagia.
The symptoms of dysphagia include:
Irritable after feedings/colic symptoms
Milk dribbling from the mouth
Coughing with feeds
Gagging
Air intake/Gas
Big gulps when swallowing
Slow feeding
Congestion
Poor color with feeds (medical term: cyanosis)
Arching
Refusing to eat
Respiratory issues
Poor tongue control
A feeding evaluation was completed for all babies with symptoms suggestive of GERD and dysphagia. The researchers found that many babies were diagnosed with dysphagia upon testing. However, they were surprised to find that many of the babies evaluated had severe dysphagia. Risk factors for GERD and dysphagia include developmental delay and poor weight gain. Reflux medications were not found to prevent dysphagia and the vast majority of the infants were on a prescription medication at the time of the study.
Reflux medications were not found to prevent dysphagia and the vast majority of the infants were on a prescription medication at the time of the study.
Dysphagia may be under-diagnosed in infants since there are many similarities in symptoms. Certainly Gastroesophageal Reflux (GER) and Gastroesophageal Reflux Disease (GERD) are more common so doctors will be more inclined to treat reflux first. However, if a baby does not respond to medical treatment, it may be necessary to investigate other causes of the symptoms. A speech language pathologist with training and expertise in infant swallowing and feeding problems is skilled at identifying and treating feeding problems. Unfortunately, a feeding specialist may not be available in every community. It might be necessary to get a referral to a larger regional hospital, children's hospital or feeding clinic. Once the problem is identified, parents and caregivers can be trained to use special feeding techniques at home to help a baby eat and grow.
Meet Our Writer
Jan Gambino
Jan wrote for HealthCentral as a patient expert for Acid Reflux.
No one mentioned reflux
First of all silent reflux needs to be changed to screaming reflux. The word silent makes out that there is something serene and quiet about it. However if you've ever had a baby with severe silent reflux you’ll know there is definitely nothing silent about it….
The first two weeks with my first born were bliss; she fed and she slept like a dream, she was one of the sleepy newborn babies, I had tonnes of milk, I fed her, wrapped her up and she went off to sleep. Everything was going very very well. We were possibly in the honeymoon period that I had read about.
After two weeks things started to change a bit. I noticed there was something strange about the way she fed, but being a first time mother I had no idea what I was doing anyway. She would feed for a little bit then pull off, then feed and pull off; this happened at least 10-20 times per feed. My midwife said I had an oversupply of milk and a forceful let down and Millicent simply couldn't handle it. She explained it as having a fire hose turned on inside my mouth. Ok, I got it, this definitely explained why she couldn't swallow properly.
My midwife said I had an oversupply of milk and a forceful let down and Millicent simply couldn't handle it. She explained it as having a fire hose turned on inside my mouth. Ok, I got it, this definitely explained why she couldn't swallow properly.
My little baby started waking up a bit more now she wasn't that sleepy sleepy newborn and she started not settling as well as she had. My husband and I were up at night stroking her eyes or side settling by patting her bottom to get her to sleep now, whereas she hadn't needed this before. She was taking much longer to settle. Along with this fussy feeding and bad settling came a lot of wind as well. Every time she latched back on she would gulp in air, you could hear her swallowing it straight into her stomach.
Get your little one’s sleep back on track.
Get guidance, advice & exclusive support through the sleep regressions, nap transitions and big sleep changes to come.
Join Now
By 4 weeks she was still fussy feeding and it was getting worse. I started to wonder if I was trying to over-feed her; maybe she just didn't want any more milk? She was cutting right back on feeds and only feeding for maybe 15 minutes at a time. My midwife said "oh she is just an efficient feeder".
I started to wonder if I was trying to over-feed her; maybe she just didn't want any more milk? She was cutting right back on feeds and only feeding for maybe 15 minutes at a time. My midwife said "oh she is just an efficient feeder".
She also started not settling at all, starting to cry all the time, hating being in her carseat capsule, gulping in air when feeding, not taking a bottle anymore (when she had at first) and just generally not happy. She would stop breathing every now and again and she had really bad breath.
I called a lactation consultant. Again she said it's all because of your let down. Try different positions of feeding. Try laying down to feed her, or lying on your back with her on top of you. So I tried every position possible, even walking around while feeding. Now she was pretty much crying after every feed and by crying I mean for an hour and a half after every feed. I knew this wasn't right, surely this isn't right! Other people told me that babies cry and that it was normal for her to cry like this. But they hadn't seen it. They weren't with her for 24 hours a day seeing her scream her lungs out most of the day. Our days basically consisted of her waking, feeding, then screaming for an hour and a half until she went back to sleep, all for it to repeat again 2 hours later.
But they hadn't seen it. They weren't with her for 24 hours a day seeing her scream her lungs out most of the day. Our days basically consisted of her waking, feeding, then screaming for an hour and a half until she went back to sleep, all for it to repeat again 2 hours later.
Weeks 4 to 6 was hell! I called four different lactation consultants, Plunket, my midwife and we even had a Keratane nurse come. Everyone kept saying the same thing:
"It's your let down!"
But why was she doing to same with a bottle?? Why was she only feeding for 5 minutes? Why couldn't she swallow properly? The Keratane nurse said it's like she hasn't learnt how to swallow yet?? What? Really? I had NO idea.
None of my friends had babies like this, none of the girls at coffee group were having problems. No one would listen to me and by this stage I was VERY desperate. The only way I could calm my screaming baby was to lay down on my back with her on top and pat her on her back, and by pat I mean PAT! We were up all night. My husband and I would take 45 minute shifts of sleeping while the other tried to get our baby to sleep. Finally she would go to sleep but wake only 35 minutes later. The poor thing was loosing weight and fast. She wasn't feeding enough. She COULDN'T feed enough.
My husband and I would take 45 minute shifts of sleeping while the other tried to get our baby to sleep. Finally she would go to sleep but wake only 35 minutes later. The poor thing was loosing weight and fast. She wasn't feeding enough. She COULDN'T feed enough.
I was now not able to go out, the only way she would feed was by me laying down on my recliner (and remember she pulled off 20 times a feed). I could hardly do this in my local cafe with friends having a casual coffee. Not to mention I was exhausted from being up all night. I had tried all different feeding positions - standing up, distracting her, shunting her bum while feeding. All while every one of her little limbs were fighting me; she didn't want to feed.
It got to the point where I was feeding her, then getting my husband to bring top up bottles to try and get more milk into her, but even the bottles she was struggling with. I tried every single bottle and teat available, we spent a fortune. I was also wary as any first time mother is, maybe this is going to cause "nipple confusion" but she had to be fed!
5 weeks 5 days, it was a Saturday. I still remember it vividly even though it's 2.5 years later now. It had taken until 9pm to get her to sleep, although that was normal lately. She woke again at 11pm. Took until 1am to get her back to sleep. She woke at 3am. I'm feeding her, while I almost fall asleep, she starts screaming. I ask my very tired husband to get some expressed milk from the freezer. He's heating it up (taking what seems an age, while I'm holding screaming baby). I'm now crying and exhausted, as she just wont feed but even I, first time mother, could tell she was STARVING. Finally Luke comes in with the bottle of expressed milk, which of course he had to heat up by resting it in hot water. IT DID TAKE AN AGE, especially at 3am holding screaming baby. I'm crying, baby crying, husband flustered. I remember screaming/crying over the baby "THIS. IS. NOT. NORMALLLLLLLL!!"
I still remember it vividly even though it's 2.5 years later now. It had taken until 9pm to get her to sleep, although that was normal lately. She woke again at 11pm. Took until 1am to get her back to sleep. She woke at 3am. I'm feeding her, while I almost fall asleep, she starts screaming. I ask my very tired husband to get some expressed milk from the freezer. He's heating it up (taking what seems an age, while I'm holding screaming baby). I'm now crying and exhausted, as she just wont feed but even I, first time mother, could tell she was STARVING. Finally Luke comes in with the bottle of expressed milk, which of course he had to heat up by resting it in hot water. IT DID TAKE AN AGE, especially at 3am holding screaming baby. I'm crying, baby crying, husband flustered. I remember screaming/crying over the baby "THIS. IS. NOT. NORMALLLLLLLL!!"
I knew there was something wrong, I knew this wasn't normal, even my own husband thought that maybe I was being over the top. But I remembered something my mother in law said: "If you think there is something wrong, then you're probably right. You and only you are the one who spends 24 hours a day with her". I just had no idea what 'it' was.
You and only you are the one who spends 24 hours a day with her". I just had no idea what 'it' was.
I called lactation consultant number FIVE. She was on holiday but I guess could tell I was so desperate for some help, so she talked to me on the phone. In a passing comment after about half an hour she said "oh that sounds a bit refluxy but yes probably your let down". She was the first person to even mention reflux. I'd never seen my baby spill or spew so no one, I mean NO ONE, had even thought about it.
And then it happened, she fed, then burped then screamed. I could hear something come up with the burp that I'd never noticed before, but she swallowed it back down. Then screamed. Silent reflux.
6 weeks, Sunday: I started googling reflux. Finally maybe an answer. Thank goodness we were going to the GP the next day for her 6 week injections, I could tell him what was going on:
- Screaming after burping
- Mid-scream she would suck in what ever was coming up with the burp, back into her lungs, choke and scream for longer
- Apenea (stopping breathing while asleep and awake!)
- Feeding for only 5 minutes
- Only feed well when very sleepy
- Couldn't swallow properly on breast or bottle
- Tiny bubbles around her mouth constantly
- SEVERE bad breath
- Screamed in the car, constantly
- Constant hiccups, even in her sleep
- Waking constantly and catnapping
- Loss of weight
- Laying awake at night, for hours
- Preferred sleeping upright (in a swing/front pack)
- Took hours every single time to settle.
 I mean HOURS! As I said we would take shifts overnight
I mean HOURS! As I said we would take shifts overnight - Starting arching her back
- Voice had changed
I felt like the GP was the only person who took me seriously. He weighed her, listened to my list that I'd made. Even he was not sure what the problem was but said that whatever it was, it was extremely serious and that I was to go straight home and make an appointment with a pediatrician and it had to be TOMORROW.
I called the first of the pediatricians on the list my GP had given me, unfortunately he was a 6 week wait. The next doctor I called, when I explained the situation, squeezed us in the next day. Thank goodness!!
Luke, Millicent and I drove across town to see the pediatrician and I did the same as we had with the GP, went over the list above, went over our family history (both myself and my husband were severely allergic children). He checked her over, listened to her lungs (there was now acid in her lungs) and diagnosed our sweet 6 week old baby with SEVERE Gastro Oesophageal Reflux. Everything on my list was explained by her stomach acid coming up into her oesophagus (food pipe) and it was causing her severe pain and also damaging her lungs and voice box. Treatment: Losec and a breathing monitor for sleeping. Finally he gave us hope that things would get better. He said we were lucky to come in when we did, as any later she would have had permanent damage to her voice box, oesophagus, lungs and ears. In 5 days he said, the crying would stop! I was obviously counting down the hours.
Everything on my list was explained by her stomach acid coming up into her oesophagus (food pipe) and it was causing her severe pain and also damaging her lungs and voice box. Treatment: Losec and a breathing monitor for sleeping. Finally he gave us hope that things would get better. He said we were lucky to come in when we did, as any later she would have had permanent damage to her voice box, oesophagus, lungs and ears. In 5 days he said, the crying would stop! I was obviously counting down the hours.
Now I know there is a lot of controversy about administering Losec to a baby. Until you have a child with Silent or Screaming reflux and seen your weak, starving baby in the amount of pain that our baby was in, any parent would do whatever they could to stop that pain. Losec it was.
------------
Breastfeeding in the first month: what to expect
Not sure how to establish lactation and increase milk production? If you need help, support, or just want to know what to expect, read our first month breastfeeding advice
Share this information
The first weeks of breastfeeding are a very stressful period. If at times you feel like you can't handle it, know that you are not alone. Feeding your baby all day long is completely natural and helps produce breast milk, but can be quite tiring at times. Be patient, think about yourself and remember: after the first month, when milk production stabilizes, it will become easier.
If at times you feel like you can't handle it, know that you are not alone. Feeding your baby all day long is completely natural and helps produce breast milk, but can be quite tiring at times. Be patient, think about yourself and remember: after the first month, when milk production stabilizes, it will become easier.
How often should a baby be breastfed?
Babies are born with a small stomach that grows rapidly with increasing milk production: in the first week it is no larger than an apricot, and after two weeks it is already the size of a large chicken egg. 1.2 Let the child eat as much as he wants and when he wants. This will help him quickly regain the weight lost after birth and grow and develop further.
“Be prepared to feed every two to three hours throughout the day. At night, the intervals between feedings can be longer: three to four or even five hours, says Cathy Garbin, a recognized international expert on breastfeeding. Some eat quickly and are satiated in 15 minutes, while others take an entire hour to feed. Do not compare your breastfeeding regimen with that of other mothers - it is very likely that there will be nothing in common between them.
Do not compare your breastfeeding regimen with that of other mothers - it is very likely that there will be nothing in common between them.
At each feed, give your baby a full meal from one breast and then offer a second one, but don't worry if the baby doesn't take it. When the baby is full, he lets go of his chest and at the same time looks relaxed and satisfied - so much so that he can immediately fall asleep. The next time you feed, start on the other breast. You can monitor the order of the mammary glands during feeding using a special application.
Why does the child always ask for a breast?
The first month is usually the hardest time to breastfeed. But do not think that because the baby is constantly hungry and asks for a breast almost every 45 minutes, then you do not have enough milk.
In the first month, the baby needs to eat frequently to start and stimulate the mother's milk production. It lays the foundation for a stable milk supply in the future. 3
3
In addition, we must not forget that the child needs almost constant contact with the mother. The bright light and noise of the surrounding world at first frighten the baby, and only by clinging to his mother, he can calm down.
Sarah, mother of three from the UK, confirms: “Crying is not always a sign of hunger. Sometimes my kids just wanted me to be around and begged for breasts to calm them down. Use a sling. Place the cradle next to the bed. Don't look at the clock. Take advantage of every opportunity to relax. Forget about cleaning. Let those around you take care of you. And not three days, but six weeks at least! Hug your baby, enjoy the comfort - and trust your body."
Do I need to feed my baby on a schedule?
Your baby is still too young for a strict daily routine, so
forget about breastfeeding schedules and focus on his needs.
“Volumes have been written about how to feed a baby on a schedule, but babies don't read or understand books,” Cathy says. - All children are different. Some people can eat on a schedule, but most can't. Most often, over time, the child develops his own schedule.
- All children are different. Some people can eat on a schedule, but most can't. Most often, over time, the child develops his own schedule.
Some mothers report that their babies are fine with scheduled feedings, but they are probably just the few babies who would eat every four hours anyway. Adults rarely eat and drink the same foods at the same time of day - so why do we expect this from toddlers?
Offer your baby the breast at the first sign of hunger. Crying is already the last stage, so be attentive to early signs: the baby licks his lips, opens his mouth, sucks his fist, turns his head with his mouth open - looking for the breast. 4
What is a "milk flush"?
At the beginning of each feed, a hungry baby actively sucks on the nipple,
thereby stimulating the milk flow reflex - the movement of milk through the milk ducts. 5
“Nipple stimulation triggers the release of the hormone oxytocin,” explains Cathy. “Oxytocin is distributed throughout the body and causes the muscles around the milk-producing glands to contract and the milk ducts to dilate. This stimulates the flow of milk.
This stimulates the flow of milk.
If the flushing reflex fails, milk will not come out. This is a hormonal response, and under stress it may not work at all or work poorly. Therefore, it is so important that you feel comfortable and calm when feeding.
“Studies show that each mother has a different rhythm of hot flashes during one feed,” Kathy continues, “Oxytocin is a short-acting hormone, it breaks down in just 30-40 seconds after formation. Milk begins to flow, the baby eats, the effect of oxytocin ends, but then a new rush of milk occurs, the baby continues to suckle the breast, and this process is repeated cyclically. That is why, during feeding, the child periodically stops and rests - this is how nature intended.
The flow of milk may be accompanied by a strong sensation of movement or tingling in the chest, although 21% of mothers, according to surveys, do not feel anything at all. 5 Cathy explains: “Many women only feel the first rush of milk. If you do not feel hot flashes, do not worry: since the child eats normally, most likely, you simply do not understand that they are.
If you do not feel hot flashes, do not worry: since the child eats normally, most likely, you simply do not understand that they are.
How do you know if a baby is getting enough milk?
Since it is impossible to track how much milk a baby eats while breastfeeding, mothers sometimes worry that the baby is malnourished. Trust your child and your body.
After a rush of milk, the baby usually begins to suckle more slowly. Some mothers clearly hear how the baby swallows, others do not notice it. But one way or another, the child himself will show when he is full - just watch carefully. Many babies make two or three approaches to the breast at one feeding. 6
“When a child has had enough, it is noticeable almost immediately: a kind of “milk intoxication” sets in. The baby is relaxed and makes it clear with his whole body that he is completely full, says Katie, “Diapers are another great way to assess whether the baby is getting enough milk. During this period, a breastfed baby should have at least five wet diapers a day and at least two portions of soft yellow stool, and often more. ”
”
From one month until weaning at six months of age, a baby's stool (if exclusively breastfed) should look the same every day: yellow, grainy, loose, and watery.
When is the child's birth weight restored?
Most newborns lose weight in the first few days of life. This is normal and should not be cause for concern. As a rule, weight is reduced by 5-7%, although some may lose up to 10%. One way or another, by 10–14 days, almost all newborns regain their birth weight. In the first three to four months, the minimum expected weight gain is an average of 150 grams per week. But one week the child may gain weight faster, and the next slower, so it is necessary that the attending physician monitor the health and growth of the baby constantly. 7.8
At the slightest doubt or signs of dehydration, such as
dark urine, no stool for more than 24 hours, retraction of the fontanel (soft spot on the head), yellowing of the skin, drowsiness, lethargy, lack of appetite (ability to four to six hours without feeding), you should immediately consult a doctor. 7
7
What is "cluster feeding"?
When a baby asks to breastfeed very often for several hours, this is called cluster feeding. 6 The peak often occurs in the evening between 18:00 and 22:00, just when many babies are especially restless and need close contact with their mother. Most often, mothers complain about this in the period from two to nine weeks after childbirth. This is perfectly normal and common behavior as long as the baby is otherwise healthy, eating well, gaining weight normally, and appears content throughout the day. 9
Cluster feeding can be caused by a sharp jump in the development of the body - during this period the baby especially needs love, comfort and a sense of security. The growing brain of a child is so excited that it can be difficult for him to turn off, or it just scares the baby. 9 If a child is overworked, it is often difficult for him or her to calm down on his own, and adult help is needed. And breastfeeding is the best way to calm the baby, because breast milk is not only food, but also pain reliever and a source of happiness hormones. 10
And breastfeeding is the best way to calm the baby, because breast milk is not only food, but also pain reliever and a source of happiness hormones. 10
“Nobody told me about cluster feeding, so for the first 10 days I just went crazy with worry - I was sure that my milk was not enough for the baby,” recalls Camille, a mother from Australia, “It was a very difficult period . I was advised to pump and supplement until I finally contacted the Australian Breastfeeding Association. There they explained to me what was happening: it turned out that it was not about milk at all.
Remember, this is temporary. Try to prepare dinner for yourself in the afternoon, when the baby is fast asleep, so that in the evening, when he begins to often breastfeed, you have the opportunity to quickly warm up the food and have a snack. If you are not alone, arrange to carry and rock the baby in turns so that you have the opportunity to rest. If you have no one to turn to for help and you feel that your strength is leaving you, put the baby in the crib and rest for a few minutes, and then pick it up again.
Ask your partner, family and friends to help you with household chores, cooking and caring for older children if you have any. If possible, hire an au pair. Get as much rest as possible, eat well and drink plenty of water.
“My daughter slept a lot during the day, but from 23:00 to 5:00 the cluster feeding period began, which was very tiring,” recalls Jenal, a mother from the USA, “My husband tried his best to make life easier for me - washed, cleaned, cooked, changed diapers, let me sleep at every opportunity and never tired of assuring me that we were doing well.
If you are concerned about the frequency of breastfeeding, it is worth contacting a specialist. “Check with a lactation consultant or doctor to see if this is indicative of any problems,” recommends Cathy. “Resist the temptation to supplement your baby with formula (unless recommended by your doctor) until you find the cause. It may not be a matter of limited milk production at all - it may be that the child is inefficiently sucking it.
When will breastfeeding become easier?
This early stage is very special and does not last long. Although sometimes it seems that there will be no end to it, rest assured: it will get easier soon! By the end of the first month, breast milk production will stabilize, and the baby will become stronger and learn to suckle better. 2.3 Any problems with latch on by this time will most likely be resolved and the body will be able to produce milk more efficiently so inflammation and leakage of milk will begin to subside.
“The first four to six weeks are the hardest, but then things start to get better,” Cathy assures. It just needs to be experienced!”
The longer breastfeeding continues, the more benefits it brings, from saving on formula and improving sleep quality 11–13 to boosting your baby's immune system 14 and reducing your risk of certain cancers. 15
“When you feel like you're pushing yourself, try to go from feed to feed and day to day,” says Hannah, a UK mom. “I was sure I wouldn’t make it to eight weeks. And now I have been breastfeeding for almost 17 weeks, and I dare say it is very easy.”
“I was sure I wouldn’t make it to eight weeks. And now I have been breastfeeding for almost 17 weeks, and I dare say it is very easy.”
Read the resource Breastfeeding Beyond the First Month: What to Expect
Literature
1 Naveed M et al. An autopsy study of relationship between perinatal stomach capacity and birth weight. Indian J Gastroenterol .1992;11(4):156-158. - Navid M. et al., Association between prenatal gastric volume and birth weight. Autopsy. Indian J Gastroenterol. 1992;11(4):156-158.
2 Neville MC et al. Studies in human lactation: milk volumes in lactating women during the onset of lactation and full lactation .Am J Clinl Nutr . 1988;48(6):1375-1386. at the beginning and at the peak of lactation." Am F Clean Nutr. 1988;48(6):1375-1386.
3 Kent JC et al. Principles for maintaining or increasing breast milk production. J Obstet , Gynecol , & Neonatal Nurs . 2012;41(1):114-121. - Kent J.S. et al., "Principles for Maintaining and Increasing Milk Production". J Obstet Ginecol Neoneutal Nurs. 2012;41(1):114-121.
Principles for maintaining or increasing breast milk production. J Obstet , Gynecol , & Neonatal Nurs . 2012;41(1):114-121. - Kent J.S. et al., "Principles for Maintaining and Increasing Milk Production". J Obstet Ginecol Neoneutal Nurs. 2012;41(1):114-121.
4 Australian Breastfeeding Feeding cues ; 2017 Sep [ cited 2018 Feb ]. - Australian Breastfeeding Association [Internet], Feed Ready Signals; September 2017 [cited February 2018]
5 Kent JC et al. Response of breasts to different stimulation patterns of an electric breast pump. J Human Lact . 2003;19(2):179-186. - Kent J.S. et al., Breast Response to Different Types of Electric Breast Pump Stimulation. J Human Lact (Journal of the International Association of Lactation Consultants). 2003;19(2):179-186.
J Human Lact (Journal of the International Association of Lactation Consultants). 2003;19(2):179-186.
6) Kent JC et al . Volume and frequency of breastfeedings and fat content of breast milk throughout the day. Pediatrics. 2006;117(3): e 387-395. - Kent J.S. et al., "Amount and frequency of breastfeeding and fat content of breast milk during the day." Pediatrix (Pediatrics). 2006;117(3):e387-95.
7 Lawrence RA, Lawrence RM. Breastfeeding: A guide for the medical profession. 7th ed. Maryland Heights MO, USA: Elsevier Mosby; 2010. 1128 p . - Lawrence R.A., Lawrence R.M., "Breastfeeding: A guide for healthcare professionals." Seventh edition. Publisher Maryland Heights , Missouri, USA: Elsevier Mosby; 2010. P. 1128.
8 World Health Organization. [Internet]. Child growth standards; 2018 [cited 2018 Feb] - World Health Organization. [Internet]. Child Growth Standards 2018 [cited February 2018].
[Internet]. Child growth standards; 2018 [cited 2018 Feb] - World Health Organization. [Internet]. Child Growth Standards 2018 [cited February 2018].
9 Australian Breastfeeding Association . [ Internet ]. Cluster feeding and fussing babies ; Dec 2017 [ cited 2018 Feb ] - Australian Breastfeeding Association [Internet], Cluster Feeding and Screaming Babies; December 2017 [cited February 2018].
10 Moberg KU, Prime DK. Oxytocin effects in mothers and infants during breastfeeding. Infant . 2013;9(6):201-206.- Moberg K, Prime DK, "Oxytocin effects on mother and child during breastfeeding". Infant. 2013;9(6):201-206.
11 U.S. Department of Health & Human Services [Internet]. Surgeon General Breastfeeding factsheet; 2011 Jan 20 [cited 2017 Feb] - Department of Health and Human Services [Internet], "Breastfeeding Facts from the Chief Medical Officer", Jan 20, 2011 [cited Feb 2017]
12 Kendall-Tackett K et al. The effect of feeding method on sleep duration, maternal well-being, and postpartum depression. clinical lactation. 2011;1;2(2):22-26. - Kendall-Tuckett, K. et al., "Influence of feeding pattern on sleep duration, maternal well-being and the development of postpartum depression." Clinical Lactation. 2011;2(2):22-26.
The effect of feeding method on sleep duration, maternal well-being, and postpartum depression. clinical lactation. 2011;1;2(2):22-26. - Kendall-Tuckett, K. et al., "Influence of feeding pattern on sleep duration, maternal well-being and the development of postpartum depression." Clinical Lactation. 2011;2(2):22-26.
13 Brown A, Harries V. Infant sleep and night feeding patterns during later infancy: Association with breastfeeding frequency, daytime complementary food intake, and infant weight. Breast Med . 2015;10(5):246-252. - Brown A., Harris W., "Night feedings and infant sleep in the first year of life and their association with feeding frequency, daytime supplementation, and infant weight." Brest Med (Breastfeeding Medicine). 2015;10(5):246-252.
14 Hassiotou F et al. Maternal and infant infections stimulate a rapid leukocyte response in breastmilk. Clin Transl immunology. 2013;2(4). - Hassiot F. et al., "Infectious diseases of the mother and child stimulate a rapid leukocyte reaction in breast milk." Clean Transl Immunology. 2013;2(4):e3.
Clin Transl immunology. 2013;2(4). - Hassiot F. et al., "Infectious diseases of the mother and child stimulate a rapid leukocyte reaction in breast milk." Clean Transl Immunology. 2013;2(4):e3.
15 Li DP et al. Breastfeeding and ovarian cancer risk: a systematic review and meta-analysis of 40 epidemiological studies. Asian Pac J Cancer Prev . 2014;15(12):4829-4837. - Lee D.P. et al., "Breastfeeding and the risk of ovarian cancer: a systematic review and meta-analysis of 40 epidemiological studies." Asia Pas J Cancer Prev. 2014;15(12):4829-4837.
How to help the baby when regulating
Support Support iconKeywords for searching
Home ›› How to help a child in regurgitation
HOUSE ›› how to help a child in regurgitation
- a very special time for a mother and her newborn baby. Together with the feeling of closeness and affection that feeding brings, understanding its nuances cannot but raise many questions, including the question of how to help an infant spit up. Regurgitation in a newborn is by no means always the result of a simple pat on his back.
Together with the feeling of closeness and affection that feeding brings, understanding its nuances cannot but raise many questions, including the question of how to help an infant spit up. Regurgitation in a newborn is by no means always the result of a simple pat on his back.
In this article, we'll talk about the basics of helping a newborn spit up, as well as other questions you may have about spitting up.
Why do babies spit up?
Let's get it straight: Why do newborns need to burp in the first place? During feeding, children usually swallow extra air - this is called aerophagy. Spitting up helps prevent this air from entering the intestines, as well as vomiting, gas, and crankiness in the baby. To avoid the return of milk after feeding, you should give the baby the opportunity to burp more often.
How to help a newborn spit up?
During the first six months, the baby should be kept upright in a column for 10-15 minutes after each feed.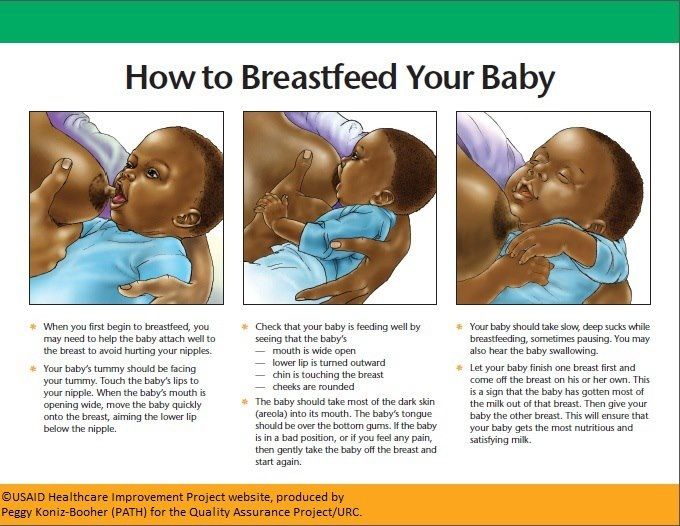 This will help keep the milk in his stomach, but if the baby occasionally burps anyway, parents need not worry. While carrying your baby in an upright position, you can put a baby diaper or wipes on your shoulder to keep your clothes clean.
This will help keep the milk in his stomach, but if the baby occasionally burps anyway, parents need not worry. While carrying your baby in an upright position, you can put a baby diaper or wipes on your shoulder to keep your clothes clean.
We've already seen why spitting up is important, now let's find out how to help your baby spit up. Parents should gently pat the baby on the back with a hand folded in a handful until he burps. Folding your hand into a handful is important because clapping with a flat palm may be too strong for an infant.
Every baby is different and there is no one right position for spitting up. To get started, you can try the following options:
- Sitting position with the baby on the chest. In this position, the parent puts the baby's head with his chin on his shoulder and with one hand supports the baby under the back. With the other hand, you can gently pat the baby on the back. This method is most effective in a rocking chair or when the baby is gently rocking.

- Holding the child upright on your legs. With one hand, parents can hold the baby by the back and head, supporting his chin and placing his palm on the baby’s chest, with the other hand, you can gently pat him on the back. At the same time, it is important to be careful: do not press the child on the throat, but only gently support his chin.
- Holding a baby on your lap while lying on your tummy. Make sure his head is above his chest and gently pat your baby on the back until he burps.
Here are some tips on how best to help your newborn spit up:
- Let your baby spit up while feeding. If the baby is restless or has swallowed air, it is worth giving him the opportunity to burp during feeding, and not just after.
- When bottle feeding, let the newborn burp after every 50-60 ml.
- When breastfeeding, let the baby burp at every breast change.
It is important to let your baby spit up after eating, even if he spit up during feeding!
If your baby is gassy, spit up more often. Also, if he vomits frequently or suffers from gastroesophageal reflux disease (GERD), have him spit up after every 30 ml bottle-feeding or every five minutes while breastfeeding.
Also, if he vomits frequently or suffers from gastroesophageal reflux disease (GERD), have him spit up after every 30 ml bottle-feeding or every five minutes while breastfeeding.
How long should a baby be held for it to burp? It's different for everyone, but generally keeping a newborn upright for 15 to 20 minutes after a feed helps the milk stay in the baby's stomach.
Minimize the amount of air you swallow. Gas production and regurgitation result from aerophagia during feeding. The baby will inevitably swallow air, but there are ways to prevent it from swallowing too much. Whether you bottle feed your baby or combine breastfeeding with bottle feeding, the Philips Avent anti-colic bottle with AirFree valve is designed so that the nipple is always filled with milk without excess air, even in a horizontal position, thus preventing the baby from swallowing excess air during feeding.
Reducing the amount of air your baby swallows can help reduce your baby's risk of colic, gas, and spitting up.











