Placenta not feeding baby
Placental insufficiency – what it is and how it can affect a pregnancy
Placental insufficiency – what it is and how it can affect a pregnancy | Pregnancy Birth and Baby beginning of content6-minute read
Listen
It’s important to see your doctor or medical team as soon as possible if you have any concerns when you are pregnant. If you have bleeding and/or significant pain, call triple zero (000) for an ambulance or go to your nearest hospital emergency department.
What is placental insufficiency?
The placenta delivers oxygen and nutrients to your baby. Placental insufficiency is when the placenta does not work properly. It’s not very common but it is serious, and can affect the growth and wellbeing of your baby.
If you have placental insufficiency, your baby may not grow as expected, leading to complications during pregnancy or birth.
What causes placental insufficiency?
Placental insufficiency occurs because the placenta doesn’t implant and grow properly in your uterus, or because it’s damaged. Sometimes there is no obvious cause.
The risk of placental insufficiency can be increased if you have medical conditions or other risk factors, such as:
- diabetes
- pre-eclampsia
- blood clotting conditions
- certain infections
- if you smoke drink alcohol or use illegal or recreational drugs
- high blood pressure, kidney problems or heart disease
- if you have had complications earlier in this pregnancy, particularly heavy bleeding
- older age during pregnancy (older than 40 years)
- if you have previously had a small baby, pre-eclampsia or stillbirth
How is placental insufficiency diagnosed?
Placental insufficiency may be picked up during your routine antenatal visits and tests.
Your doctor or midwife will measure and track the growth of your uterus and the baby.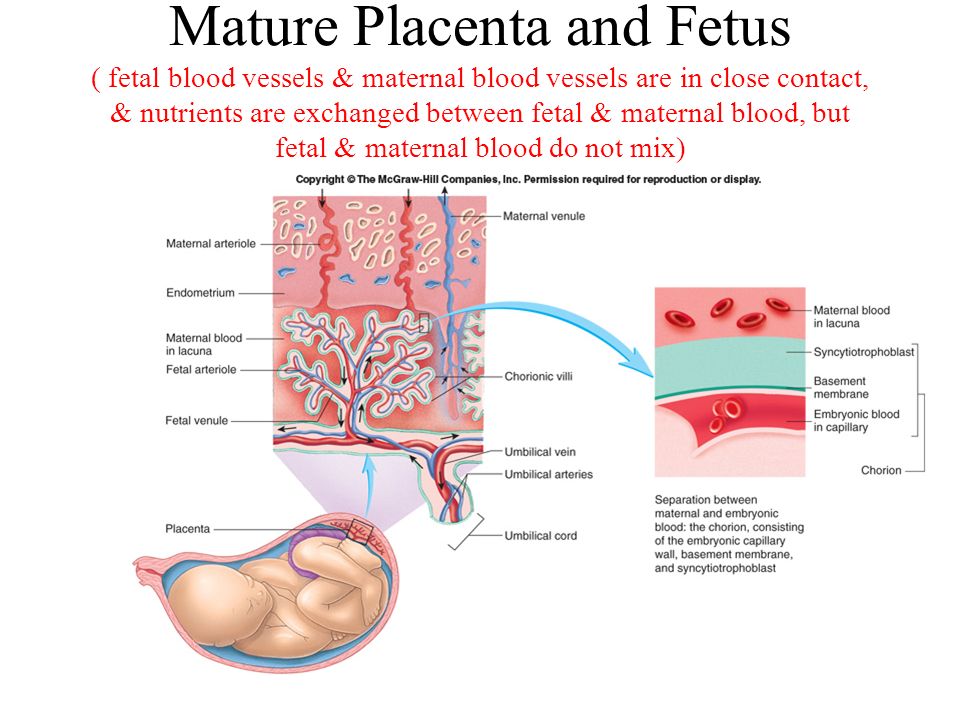 Placental insufficiency may be diagnosed during a routine ultrasound if your baby isn’t growing as expected.
Placental insufficiency may be diagnosed during a routine ultrasound if your baby isn’t growing as expected.
Sometimes pregnant women may notice that their tummy isn’t growing, is smaller than in previous pregnancies or their baby isn’t moving as much. If you have any concerns during your pregnancy, contact your midwife or doctor immediately.
Diagnosing placental insufficiency early is important for the health of the mother and baby.
FIND A HEALTH SERVICE — The Service Finder can help you find doctors, pharmacies, hospitals and other health services.
What are the risks to you and your baby?
Placental insufficiency can lead to problems both for mother and baby.
For the mother, it can be linked to conditions such as:
- pre-eclampsia
- other problems with the placenta, including placental abruption (when the placenta comes away from the wall of the uterus)
- preterm labour and delivery
If the placenta does not develop properly, it can also lead to problems for your baby.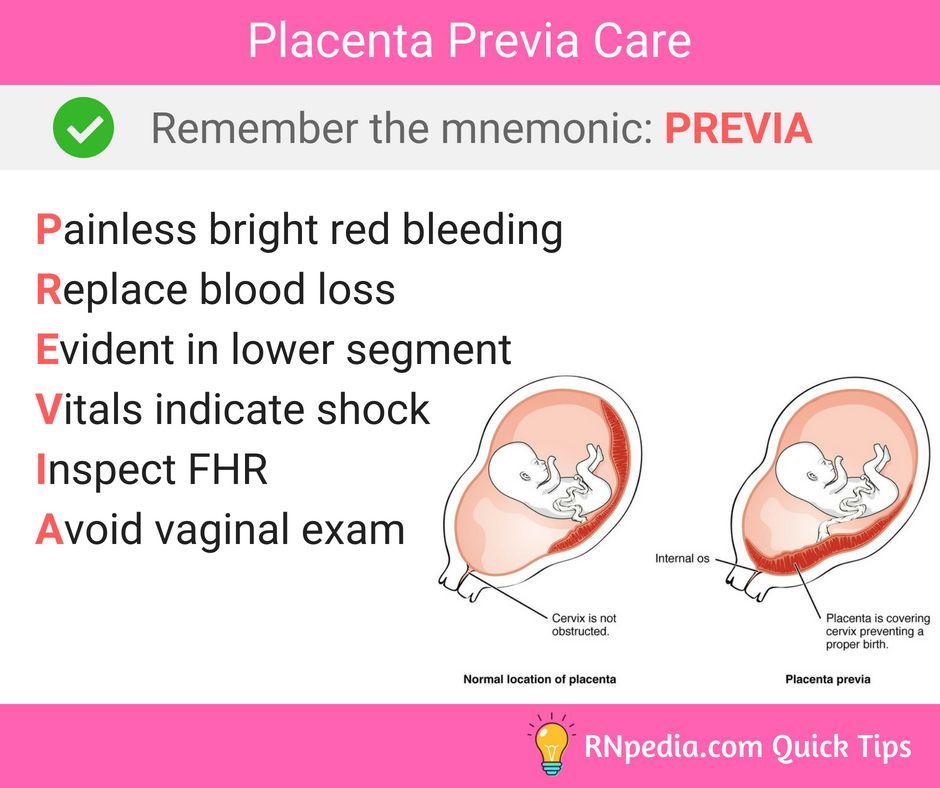 When the baby doesn’t get enough oxygen and nutrients, it can prevent normal growth and development. This is known as fetal growth restriction (FGR).
When the baby doesn’t get enough oxygen and nutrients, it can prevent normal growth and development. This is known as fetal growth restriction (FGR).
Some of the challenges that babies with FGR can have include:
- breathing or heart problems
- low oxygen levels at birth
- difficulty maintaining body temperature
- trouble feeding and gaining weight
- infection
- bleeding on the brain (called ‘intraventricular haemorrhage’)
- problems with their eyes and vision
- problems with their bowel
These conditions are more likely in premature babies.
How is placental insufficiency managed?
If your doctor suspects placental insufficiency, they will keep a close eye on how your baby is growing and developing. They will monitor you and your baby regularly and may arrange for you to give birth in a major hospital with appropriate medical support.
You will be asked to keep a record of your baby's movements and let your medical team know if you notice any changes.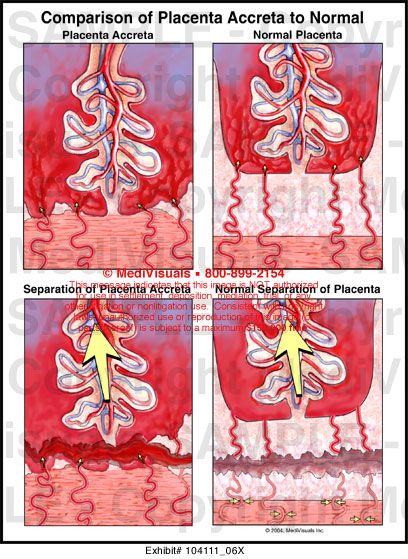
At any stage of your pregnancy, if you are concerned about your baby's movements, contact your midwife or doctor immediately. Do not wait until the next day. A slowing down of movement may be a sign that your baby is unwell.
You will likely need more frequent ultrasounds and have regular monitoring of your baby’s heart rate to assess their growth and wellbeing.
Treatment will depend on the stage of the pregnancy. If you’re under 37 weeks, your doctor may recommend waiting for as long as possible and keeping a close eye on the baby. But if there are signs that your baby is not well, it may be safest to induce labour or deliver your baby with a caesarean.
If your baby hasn’t been growing as expected, they may require additional support from the medical team at birth. The team will care for your baby, keep them warm and may help them to breathe with an oxygen mask or breathing tube.
Your baby may need to be transferred to the neonatal intensive care unit (NICU) or special care nursery for extra care.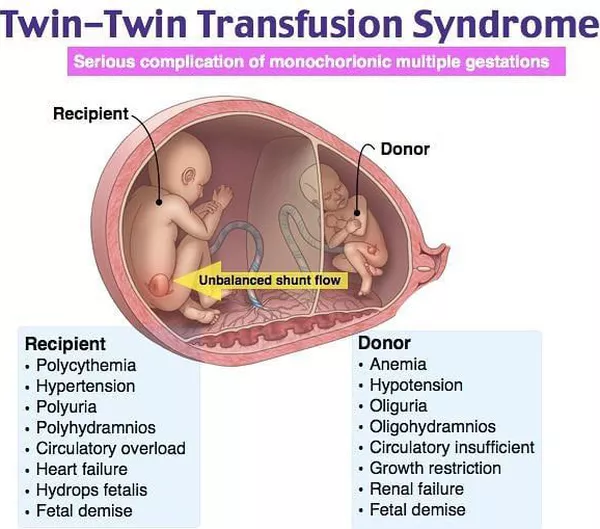
It’s important to see your doctor or medical team as soon as possible if you have any concerns when you are pregnant. If you have bleeding and/or significant pain, call triple zero (000) for an ambulance or go to your nearest hospital emergency department.
Speak to a maternal child health nurse
Call Pregnancy, Birth and Baby to speak to a maternal child health nurse on 1800 882 436 or video call. Available 7am to midnight (AET), 7 days a week.
Sources:
Department of Health and Aged Care (Fetal growth restriction and well-being), Clinical Medicine Insights: Pediatrics (Intrauterine Growth Restriction: Antenatal and Postnatal Aspects), Elsevier, ScienceDirect (Placental Insufficiency), Perinatal Society of Australia and New Zealand/Stillbirth Centre of Research Excellence (Position Statement: Detection and Management of Fetal Growth Restriction in Singleton Pregnanciex)Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: July 2022
Back To Top
Related pages
- Placenta complications in pregnancy
- About the placenta
Need more information?
Causes of Preterm Labour - Miracle Babies
There are many causes of preterm birth
Read more on Miracle Babies Foundation website
Causes - Miracle Babies
Every year in Australia around 48,000 newborn babies require the help of a NICU or SCN, there are many factors linked to premature birth and also many that remain unexplained
Read more on Miracle Babies Foundation website
Disclaimer
Pregnancy, Birth and Baby is not responsible for the content and advertising on the external website you are now entering.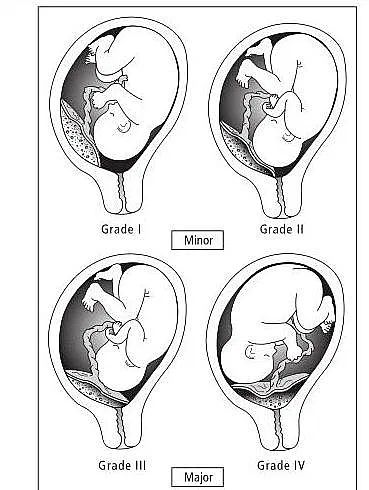
Need further advice or guidance from our maternal child health nurses?
1800 882 436
Video call
- Contact us
- About us
- A-Z topics
- Symptom Checker
- Service Finder
- Linking to us
- Information partners
- Terms of use
- Privacy
Pregnancy, Birth and Baby is funded by the Australian Government and operated by Healthdirect Australia.
Pregnancy, Birth and Baby is provided on behalf of the Department of Health
Pregnancy, Birth and Baby’s information and advice are developed and managed within a rigorous clinical governance framework. This website is certified by the Health On The Net (HON) foundation, the standard for trustworthy health information.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.
This information is for your general information and use only and is not intended to be used as medical advice and should not be used to diagnose, treat, cure or prevent any medical condition, nor should it be used for therapeutic purposes.
The information is not a substitute for independent professional advice and should not be used as an alternative to professional health care. If you have a particular medical problem, please consult a healthcare professional.
Except as permitted under the Copyright Act 1968, this publication or any part of it may not be reproduced, altered, adapted, stored and/or distributed in any form or by any means without the prior written permission of Healthdirect Australia.
Support this browser is being discontinued for Pregnancy, Birth and Baby
Support for this browser is being discontinued for this site
- Internet Explorer 11 and lower
We currently support Microsoft Edge, Chrome, Firefox and Safari. For more information, please visit the links below:
For more information, please visit the links below:
- Chrome by Google
- Firefox by Mozilla
- Microsoft Edge
- Safari by Apple
You are welcome to continue browsing this site with this browser. Some features, tools or interaction may not work correctly.
Placental Insufficiency: Causes, Symptoms, and Diagnosis
Placental Insufficiency: Causes, Symptoms, and Diagnosis- Health Conditions
- Featured
- Breast Cancer
- IBD
- Migraine
- Multiple Sclerosis (MS)
- Rheumatoid Arthritis
- Type 2 Diabetes
- Articles
- Acid Reflux
- ADHD
- Allergies
- Alzheimer's & Dementia
- Bipolar Disorder
- Cancer
- Crohn's Disease
- Chronic Pain
- Cold & Flu
- COPD
- Depression
- Fibromyalgia
- Heart Disease
- High Cholesterol
- HIV
- Hypertension
- IPF
- Osteoarthritis
- Psoriasis
- Skin Disorders and Care
- STDs
- Featured
- Discover
- Wellness Topics
- Nutrition
- Fitness
- Skin Care
- Sexual Health
- Women's Health
- Mental Well-Being
- Sleep
- Product Reviews
- Vitamins & Supplements
- Sleep
- Mental Health
- Nutrition
- At-Home Testing
- CBD
- Men’s Health
- Original Series
- Fresh Food Fast
- Diagnosis Diaries
- You’re Not Alone
- Present Tense
- Video Series
- Youth in Focus
- Healthy Harvest
- No More Silence
- Future of Health
- Wellness Topics
- Plan
- Health Challenges
- Mindful Eating
- Sugar Savvy
- Move Your Body
- Gut Health
- Mood Foods
- Align Your Spine
- Find Care
- Primary Care
- Mental Health
- OB-GYN
- Dermatologists
- Neurologists
- Cardiologists
- Orthopedists
- Lifestyle Quizzes
- Weight Management
- Am I Depressed? A Quiz for Teens
- Are You a Workaholic?
- How Well Do You Sleep?
- Tools & Resources
- Health News
- Find a Diet
- Find Healthy Snacks
- Drugs A-Z
- Health A-Z
- Health Challenges
- Connect
- Breast Cancer
- Inflammatory Bowel Disease
- Psoriatic Arthritis
- Migraine
- Multiple Sclerosis
- Psoriasis
Medically reviewed by Debra Rose Wilson, Ph.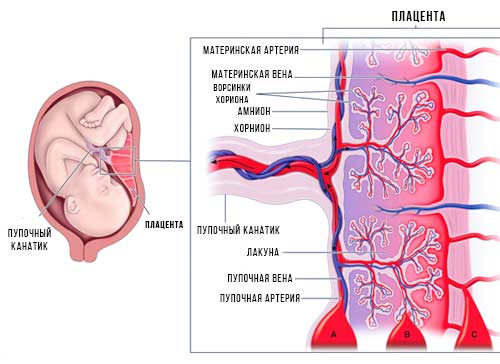 D., MSN, R.N., IBCLC, AHN-BC, CHT — By Sandy Calhoun Rice on January 8, 2018
D., MSN, R.N., IBCLC, AHN-BC, CHT — By Sandy Calhoun Rice on January 8, 2018
Overview
The placenta is an organ that grows in the womb during pregnancy. Placental insufficiency (also called placental dysfunction or uteroplacental vascular insufficiency) is an uncommon but serious complication of pregnancy. It occurs when the placenta does not develop properly, or is damaged. This blood flow disorder is marked by a reduction in the mother’s blood supply. The complication can also occur when the mother’s blood supply doesn’t adequately increase by mid-pregnancy.
When the placenta malfunctions, it’s unable to supply adequate oxygen and nutrients to the baby from the mother’s bloodstream. Without this vital support, the baby cannot grow and thrive. This can lead to low birth weight, premature birth, and birth defects. It also carries increased risks of complications for the mother. Diagnosing this problem early is crucial to the health of both mother and baby.
Vital functions of the placenta
The placenta is a highly complex biological organ.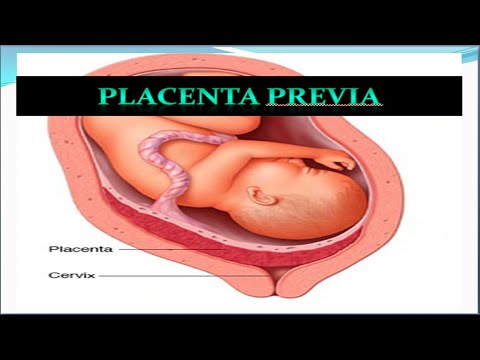 It forms and grows where the fertilized egg attaches to the wall of the uterus.
It forms and grows where the fertilized egg attaches to the wall of the uterus.
The umbilical cord grows from the placenta to the baby’s navel. It allows blood to flow from mother to baby, and back again. The mother’s blood and the baby’s blood are filtered through the placenta, but they never actually mix.
The placenta’s primary jobs are to:
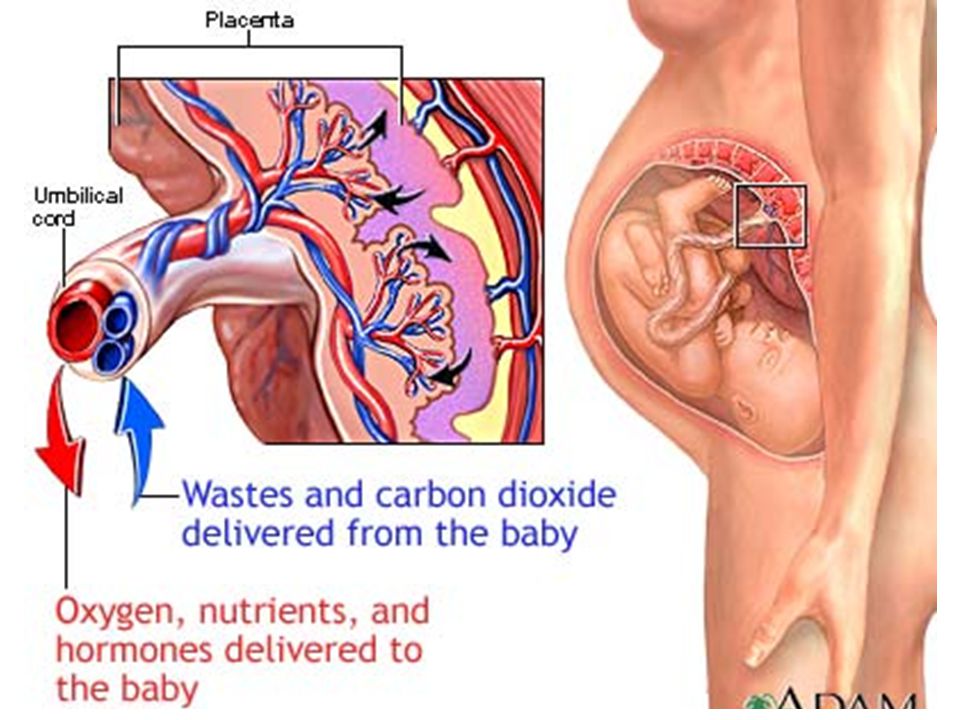
- move oxygen into the baby’s bloodstream
- carry carbon dioxide away
- pass nutrients to the baby
- transfer waste for disposal by the mother’s body
The placenta has an important role in hormone production as well. It also protects the fetus from harmful bacteria and infections.
A healthy placenta continues to grow throughout the pregnancy. The American Pregnancy Association estimates that the placenta weighs 1 to 2 pounds at the time of birth.
The placenta is removed during labor. According to the Mayo Clinic, it’s delivered between 5 and 30 minutes after the baby.
Causes of insufficiency
Placental insufficiency is linked to blood flow problems.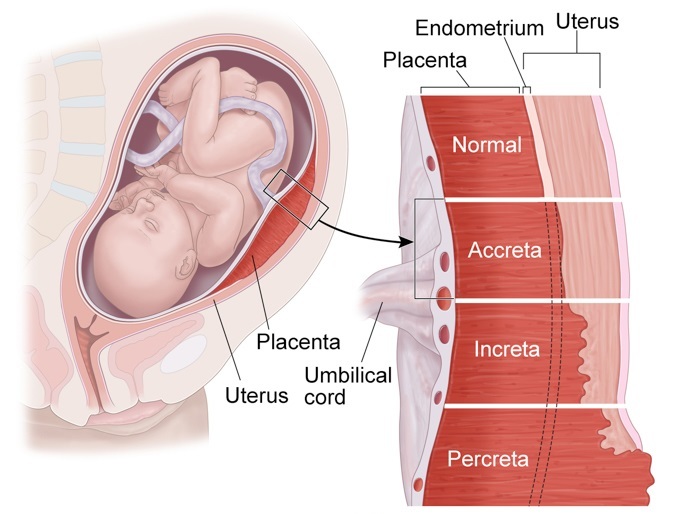 While maternal blood and vascular disorders can trigger it, medications and lifestyle habits are also possible triggers.
While maternal blood and vascular disorders can trigger it, medications and lifestyle habits are also possible triggers.
The most common conditions linked to placental insufficiency are:
- diabetes
- chronic high blood pressure (hypertension)
- blood clotting disorders
- anemia
- certain medications (particularly blood thinners)
- smoking
- drug abuse (especially cocaine, heroin, and methamphetamine)
Placental insufficiency may also occur if the placenta doesn’t attach properly to the uterine wall, or if the placenta breaks away from it (placental abruption).
Symptoms
There are no maternal symptoms associated with placental insufficiency. However, certain clues can lead to early diagnosis. The mother may notice that the size of her uterus is smaller than in previous pregnancies. The fetus may also be moving less than expected.
If the baby isn’t growing properly, the mother’s abdomen will be small, and the baby’s movements will not be felt much.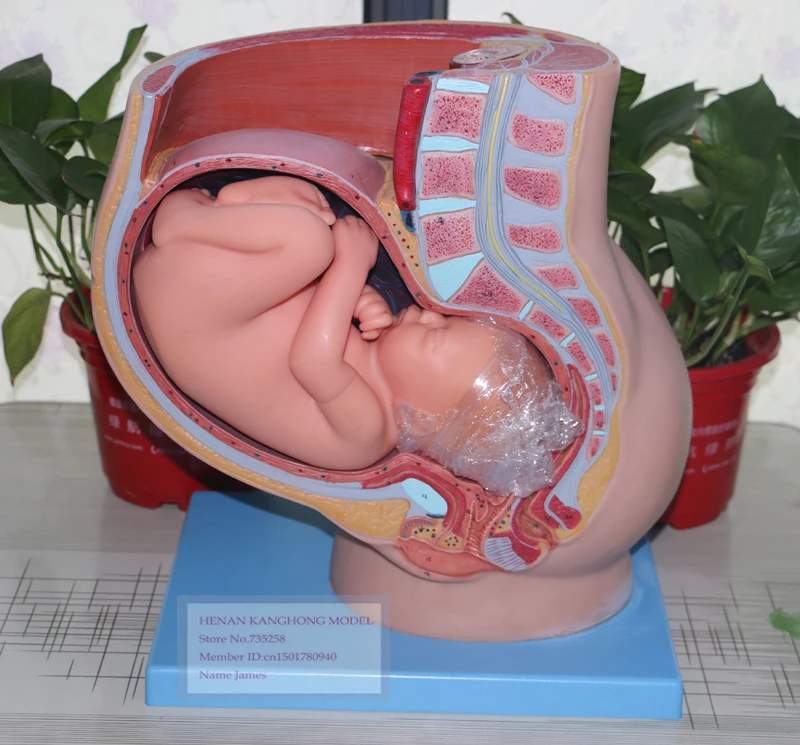
Vaginal bleeding or preterm labor contractions may occur with placental abruption.
Complications
Mother
Placental insufficiency is not usually considered life-threatening to the mother. However, the risk is greater if the mother has hypertension or diabetes.
During pregnancy, the mother is more likely to experience:
- preeclampsia (elevated blood pressure and end-organ dysfunction)
- placental abruption (placenta pulls away from the uterine wall)
- preterm labor and delivery
The symptoms of preeclampsia are excess weight gain, leg and hand swelling (edema), headaches, and high blood pressure.
Baby
The earlier in the pregnancy that placental insufficiency occurs, the more severe the problems can be for the baby. The baby’s risks include:
- greater risk of oxygen deprivation at birth (can cause cerebral palsy and other complications)
- learning disabilities
- low body temperature (hypothermia)
- low blood sugar (hypoglycemia)
- too little blood calcium (hypocalcemia)
- excess red blood cells (polycythemia)
- premature labor
- cesarean delivery
- stillbirth
- death
Diagnosis and management
Getting proper prenatal care can lead to an early diagnosis. This can improve outcomes for the mother and the baby.
This can improve outcomes for the mother and the baby.
Tests that can detect placental insufficiency include:
- pregnancy ultrasound to measure the size of the placenta
- ultrasound to monitor the size of the fetus
- alpha-fetoprotein levels in the mother’s blood (a protein made in the baby’s liver)
- fetal nonstress test (involves the wearing of two belts on the mother’s abdomen and sometimes a gentle buzzer to wake the baby) to measure the baby’s heart rate and contractions
Treating maternal high blood pressure or diabetes can help improve the baby’s growth.
A maternity care plan may recommend:
- education on preeclampsia, as well as self-monitoring for the disease
- more frequent doctor visits
- bed rest to conserve fuel and energy for the baby
- consultation with a high-risk maternal fetal specialist
You may need to keep a daily record of when the baby moves or kicks.
If there is concern about premature birth (32 weeks or earlier), the mother may receive steroid injections.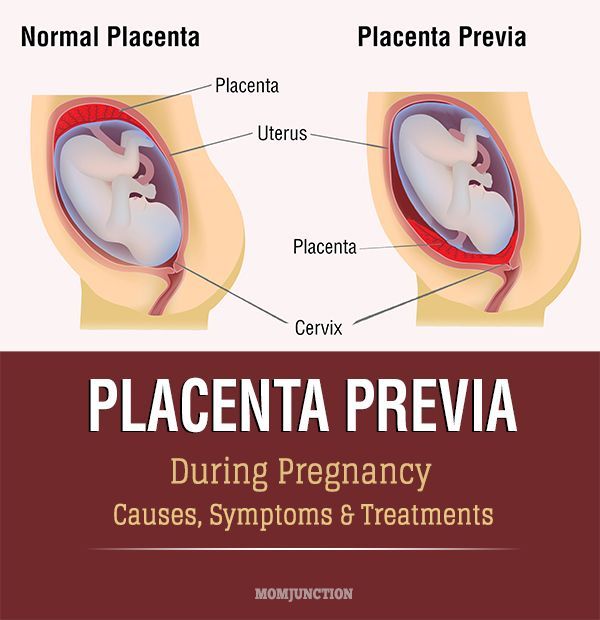 Steroids dissolve through the placenta and strengthen the baby’s lungs.
Steroids dissolve through the placenta and strengthen the baby’s lungs.
You may need intensive outpatient or inpatient care if preeclampsia or intrauterine growth restriction (IUGR) become severe.
Outlook
Placental insufficiency can’t be cured, but it can be managed. It’s extremely important to receive an early diagnosis and adequate prenatal care. These can improve the baby’s chances of normal growth and decrease the risk of birth complications. According to Mount Sinai Hospital, the best outlook occurs when the condition is caught between 12 and 20 weeks.
Last medically reviewed on January 9, 2018
- Parenthood
- Pregnancy
- Pregnancy Complications
How we reviewed this article:
Healthline has strict sourcing guidelines and relies on peer-reviewed studies, academic research institutions, and medical associations. We avoid using tertiary references. You can learn more about how we ensure our content is accurate and current by reading our editorial policy.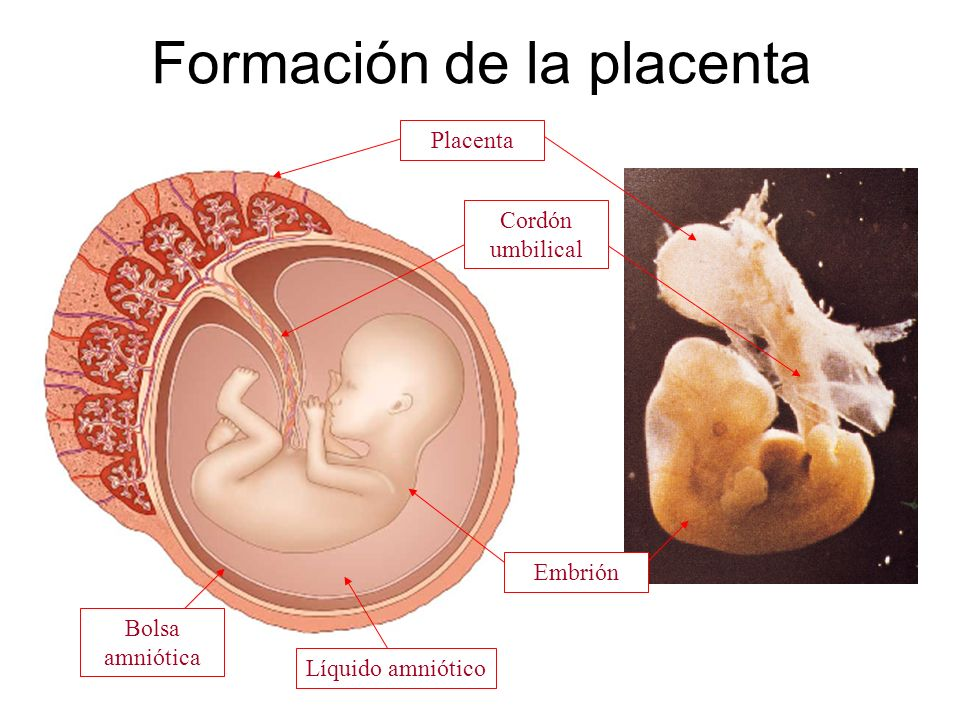
- Eating for two when over or under weight. (2015).
americanpregnancy.org/pregnancy-health/eating-for-two/ - Mayo Clinic Staff. (2015). Pregnancy week by week.
mayoclinic.org/healthy-lifestyle/pregnancy-week-by-week/in-depth/placenta/art-20044425 - Placental insufficiency. (n.d.).
mountsinai.on.ca/care/placenta-clinic/complications/placentalinsufficiency
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
Current Version
Jan 9, 2018
Written By
Sandy Calhoun Rice
Edited By
Nizam Khan (TechSpace)
Medically Reviewed By
Debra Rose Wilson, PhD, MSN, RN, IBCLC, AHN-BC, CHT
Share this article
Medically reviewed by Debra Rose Wilson, Ph.D., MSN, R.N., IBCLC, AHN-BC, CHT — By Sandy Calhoun Rice on January 8, 2018
related stories
Birth Defects
When Baby Comes Early: What Is Your Risk?
Why You Shouldn’t Worry About an Anterior Placenta
Preeclampsia: Causes, Diagnosis, and Treatments
Second Trimester Pregnancy Complications
Read this next
Birth Defects
Medically reviewed by Karen Gill, M.
 D.
D.Find information on birth defects, including what causes them, how they're diagnosed, and how they can be prevented.
READ MORE
When Baby Comes Early: What Is Your Risk?
Medically reviewed by Tyler Walker, MD
A number of social factors affect a woman's risk for preterm labor. Discover what they are here.
READ MORE
Why You Shouldn’t Worry About an Anterior Placenta
Medically reviewed by Valinda Riggins Nwadike, MD, MPH
An anterior placenta positioning during pregnancy isn’t usually cause for concern. Here’s what your doctor will keep an eye on leading up to labor and…
READ MORE
Preeclampsia: Causes, Diagnosis, and Treatments
Medically reviewed by Mia Armstrong, MD
Preeclampsia is when you have high blood pressure and protein in your urine during pregnancy or after delivery.
 Learn about symptoms, treatment, and…
Learn about symptoms, treatment, and…READ MORE
Second Trimester Pregnancy Complications
Medically reviewed by Debra Rose Wilson, Ph.D., MSN, R.N., IBCLC, AHN-BC, CHT
By the second trimester of your pregnancy, you should be feeling better than you did in the first trimester. However, every pregnancy is different…
READ MORE
Placenta Delivery: What to Expect
After delivering your baby, you’re not quite done. There’s still the placenta to contend with. Here’s what to expect.
READ MORE
What Is Placental Abruption?
Medically reviewed by Debra Rose Wilson, Ph.D., MSN, R.N., IBCLC, AHN-BC, CHT
Placental abruption occurs during a pregnancy when the placenta detaches from the uterine wall too early. This can cause bleeding and complications…
READ MORE
Pregnancy Complications
Medically reviewed by Michael Weber, MD
Sometimes a pregnant woman’s existing health conditions can contribute to problems, and other times new conditions arise because of body and hormonal…
READ MORE
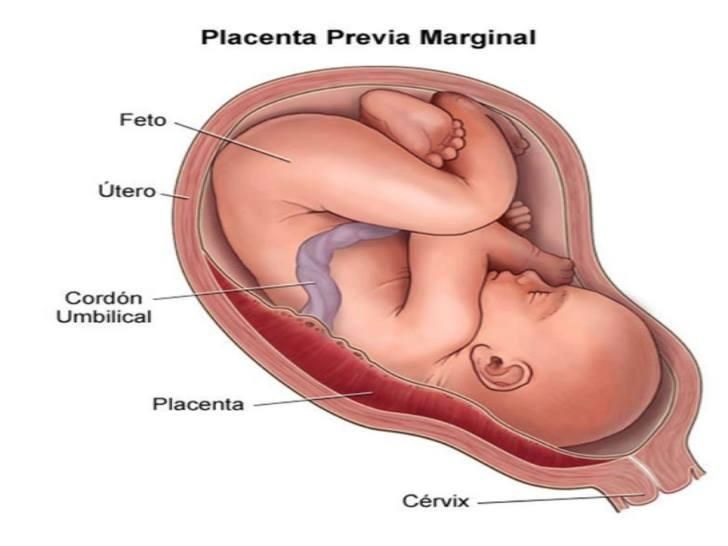
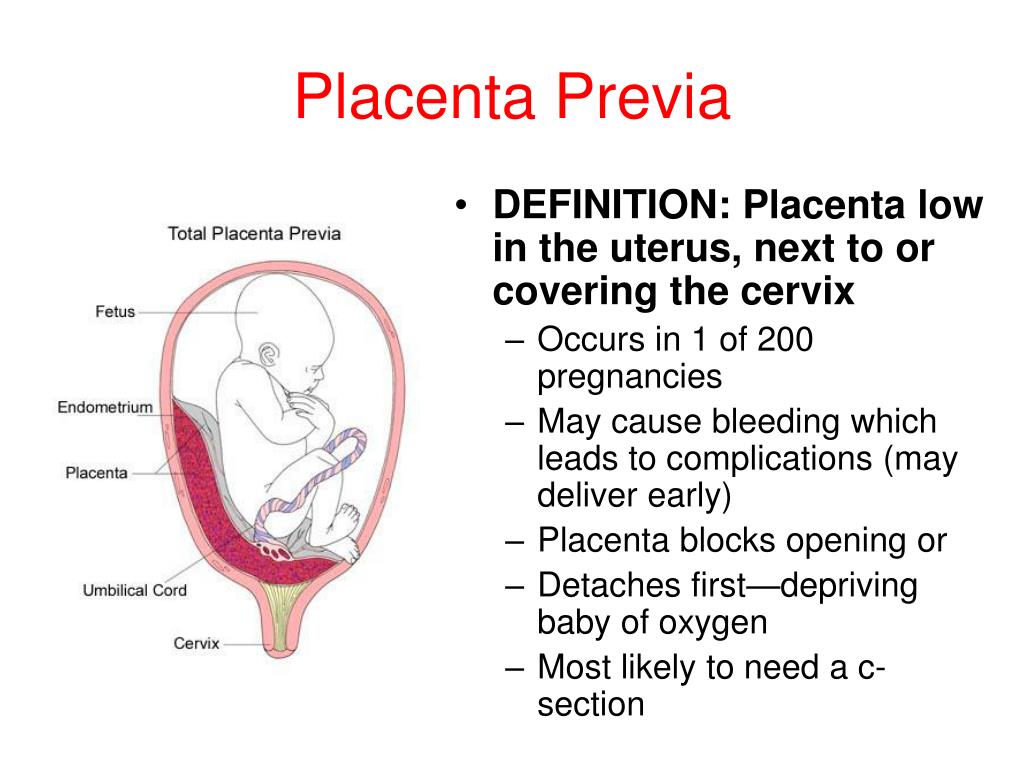
Placenta Previa
Medically reviewed by Fernando Mariz, MD
Placenta previa is when the placenta covers the opening of the cervix during the last months of pregnancy.
 Find out about symptoms and treatment.
Find out about symptoms and treatment.READ MORE
Your Guide to a Pregnancy-Safe Skin Care Routine
When you're expecting, pregnancy-safe skin care can help ensure the health of you and your baby. We'll tell you what to avoid — and some good…
READ MORE
10 amazing facts about the placenta
Home "News" 10 amazing facts about the placenta
10.10.2020
Liat Ben -Senior, MBA MSC
Placenta - this is a rescue circle between mother and her child, the organ in which the connection between them is first established. Scientists consider the placenta the least studied human organ, but one of the most important organs of the body. It affects the health of a woman and her baby during and even after pregnancy. In honor of the incredible properties of the placenta, we list 10 amazing facts about it. nine0003
nine0003
Emma Jean Photography
- Small but powerful - the parachute-shaped placenta is a highly specialized organ that helps support your baby's development. The middle placenta is 23 cm across, about 3 cm thick and usually weighs 500-600 grams. The blood of mother and baby passes through the placenta but never mixes. At term, about 500 ml of mother's blood passes through the placenta every minute. This alone is amazing (and also explains why pregnancy is so exhausting). nine0022
- One organ, many functions - Your developing baby does not eat or breathe and relies solely on its mother for nutrients and oxygen. The placenta acts like a baby's lungs, supplying oxygen and removing carbon dioxide. It also acts like a baby's kidneys, filtering waste products from the bloodstream.
- The placenta is not a maternal organ - In fact, the placenta develops from a fertilized egg, which means that, like a child, it is genetically half from mom and half from dad.
 The placenta begins to form as soon as a fertilized egg implants in the uterine wall, about 6-7 days after conception, and continues to grow with your baby to meet her growing needs. nine0022
The placenta begins to form as soon as a fertilized egg implants in the uterine wall, about 6-7 days after conception, and continues to grow with your baby to meet her growing needs. nine0022
- The placenta is also a gland - The placenta acts like a gland, releasing hormones during pregnancy that are important in supporting your growing baby and preparing your body for motherhood.
- The placenta is an immune mediator - The placenta helps the mother's and baby's immune systems to talk to each other without fighting. During pregnancy, the placenta prevents the mother's body from perceiving the child as foreign and from attacking it. During the 3rd trimester, the placenta allows mom's antibodies to pass to the baby, giving your baby a booster immune system, and this protection lasts up to 6 months after birth. nine0022
- Identical twins can share a placenta - Fraternal twins develop from two separate fertilized eggs and will always have two placentas.
 But the number of placentas in identical twins is determined by whether the fertilized egg splits before or after the formation of the placenta.
But the number of placentas in identical twins is determined by whether the fertilized egg splits before or after the formation of the placenta. - Your baby's stem cells are coming to you - baby's stem cells can cross the placenta and seem to target areas where the mother has been damaged. Even years later, small amounts of cells from previous pregnancies can be found in the mother's skin, organs, and bone marrow. This phenomenon is called "microchimerism of the fetus and mother." nine0022
- The only disposable organ - the placenta will re-develop with each pregnancy to support your baby's growth. After completing its mission, the placenta comes out after the baby is born, which is why it is called the "afterbirth".
- The placenta prepares your body for breastfeeding - The placenta produces a hormone that inhibits the production of breast milk. After the placenta is delivered, the mother's body receives a signal that it is time to produce milk.
 nine0022
nine0022
- The placenta can help us fight cancer - The placenta has the unique ability to grow and enter the mother's body without being attacked by the immune system. This ability to evade the immune system is highly regulated, and the placenta knows how to stop intrusion before harming the mother. The researchers hope that a better understanding of how the placenta works will help us fight cancers that elude the immune system.
The placenta is not only a wonderful organ during pregnancy, but for life. If you choose to donate or save placental stem cells, they will not be disposed of as biological waste.
Liat Ben-Senior holds an MBA and MSc in Human Genetics from the Sackler School of Medicine of Tel-Aviv University, Israel. She has over 15 years of experience in Marketing and Digital Marketing in the field of Biotech and Life Sciences. Her scientific background includes immunology and molecular biology research, both in academia as well as industry. Her management background includes business development and commercialization of early stage medical devices, cellular, and small molecule therapies. For over a decade, Liat worked with CReATe Cord Blood Bank as Business Manager. At CReATe, Liat focused on educating expectant parents and health care professionals about the cord blood banking options available in the Canadian market. Starting in 2020, Liat is the Marketing Manager at Anova Fertility & Reproductive Health. Liat strongly believes in empowering expectant parents so they can make an informed decision. nine0003
Her management background includes business development and commercialization of early stage medical devices, cellular, and small molecule therapies. For over a decade, Liat worked with CReATe Cord Blood Bank as Business Manager. At CReATe, Liat focused on educating expectant parents and health care professionals about the cord blood banking options available in the Canadian market. Starting in 2020, Liat is the Marketing Manager at Anova Fertility & Reproductive Health. Liat strongly believes in empowering expectant parents so they can make an informed decision. nine0003
Significance of the placenta, or "other side" of the baby, during pregnancy
The placenta begins to form at the site of implantation of a fertilized egg at 6-7 weeks of pregnancy, it is fully formed at the 4th month of pregnancy. In the future, the placenta gradually increases, and at the end of pregnancy, its diameter reaches 15–18 centimeters, and its weight is 500 grams.
The placenta consists of placental tissues and blood vessels. On the one hand, with small blood vessels, it is attached to the wall of the uterus, and on the other hand, it is covered with fetal membranes, to which the umbilical cord is attached. Genetically and biologically, the placenta is of fetal origin, and its functionality depends on the blood composition and circulation of the mother. nine0003
On the one hand, with small blood vessels, it is attached to the wall of the uterus, and on the other hand, it is covered with fetal membranes, to which the umbilical cord is attached. Genetically and biologically, the placenta is of fetal origin, and its functionality depends on the blood composition and circulation of the mother. nine0003
The function of the placenta is to feed and protect
The main function of the placenta is to provide various metabolic processes between mother and fetus. In addition, the placenta secretes into the mother's blood circulation hormones - choriongonadotropins, progesterone - necessary for the normal course of pregnancy. From the 7th to 8th weeks of pregnancy, the placenta begins to produce estrogen. Delivering nutrients to the fetus from the mother and removing the waste products of the fetal metabolism, the placenta ensures the exchange of oxygen and carbon dioxide. nine0003
The function of the placenta is also to provide passive immunity to the fetus.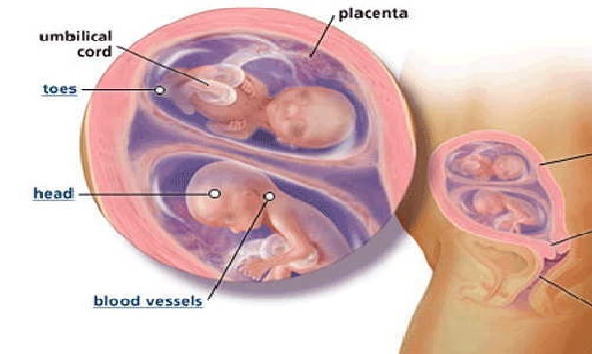
For example, if a mother is vaccinated against influenza, the resulting antibodies are transferred to the fetus through the placenta and protect the newborn and infant from severe influenza illness for 6 months after birth.
The immune system works in a similar way if a mother receives a whooping cough vaccine and a vaccine against Covid-19 infection during pregnancy. The doctor points out that this principle does not work against all infections - not all vaccines against infectious diseases provide the transfer of antibodies to the fetus. nine0003
For example, influenza and Covid-19 may or may not cross the placenta. It is known that the probability of infection with the Covid-19 virus is quite small for the fetus - only 0.4-5% of cases. The devastating effect of Covid-19 on pregnancy is harm specifically for the woman’s body – the mother’s lack of oxygen leaves consequences for the child.
In general, the placenta protects against many infections, but does not protect against syphilis, toxoplasmosis, listeriosis, Zika virus. If the mother gets these infections during pregnancy, the fetus can be born with serious congenital abnormalities. The period of pregnancy in which the woman fell ill is also important. nine0003
If the mother gets these infections during pregnancy, the fetus can be born with serious congenital abnormalities. The period of pregnancy in which the woman fell ill is also important. nine0003
When the placenta begins to protect the baby
An egg that has been fertilized and begins to divide takes time to reach the uterus and implant itself in its soft tissues, or endometrium. Only when this has happened does the placenta begin to form and choriongonadotropin is released. Thus, in the tissues of the uterus, the placenta begins to form from the moment when the fertilized egg is implanted in the wall of the uterus. Placental tissues during the entire pregnancy are transformed and continue to grow. nine0003
As soon as a woman finds out that she is pregnant (most often this is the 5-6th week of pregnancy), it is necessary to start living in the healthiest way possible. In the first weeks, the child's organs are formed, the genesis of organs occurs, when it is critically important to live in the most healthy way and follow the doctor's recommendations on lifestyle. The placenta also begins to work.
The placenta also begins to work.
“We can say that the placenta performs a transport function rather than protection. It lets medicines, infections, nutrients, alcohol, etc. through. How much it passes and what it filters depends on various circumstances. Higher molecular weight drugs cross the placenta less. For example, insulin and heparin, which is a blood-thinning drug, cross the placenta minimally. In general, absolutely any medication crosses the placenta, ”explains doctor Katrina Kalnina. nine0003
When the placenta finishes its job
The placenta is not a perpetual organ. If the pregnancy is overdue, then at the birth of the placenta, you can see that there are such small pieces of pebbles in it - calcifications. With a sonographic examination, it is possible to determine what the degree of age of the placenta is. There are three stages - from 0 to 3.
The last - third - stage indicates that the placenta is so mature that it can signal to the brain that labor can begin. nine0003
nine0003
Calcifications can be seen even a few weeks before delivery, but there is no reason to worry. This does not mean that preterm labor is approaching or that the baby is not getting enough oxygen.
During childbirth, the placenta does its work until the third stage of labor. That is, after the birth of the child, which is the second stage of labor, the third, or the birth of the placenta, follows, which lasts about 30 minutes.
There are situations in which, as soon as the baby is born, the woman is given an injection of oxytocin, which helps the uterus to contract. This is called active management of the placental period, and it is an effective method of preventing bleeding. At the birth of the placenta, the mother continues to push, and if you pull a little on the umbilical cord, the placenta comes out by itself. When the placenta is born, it is examined and assessed for any piece left in the uterus. If the placenta still does not separate, it is removed manually.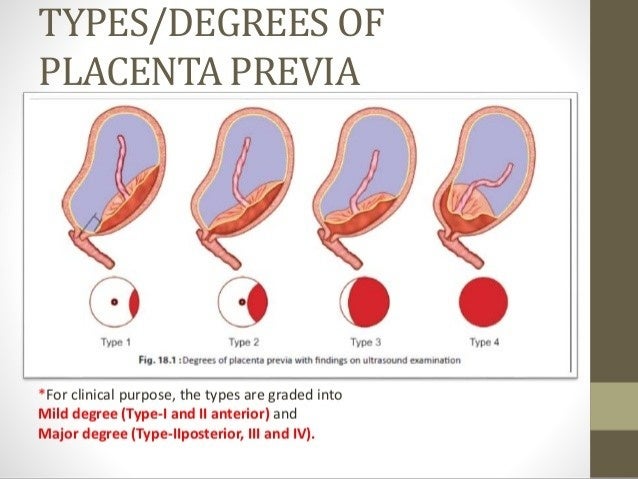 If any piece of the placenta or fetal membrane remains in the uterus, it is necessary to abrade the uterine cavity. nine0003
If any piece of the placenta or fetal membrane remains in the uterus, it is necessary to abrade the uterine cavity. nine0003
Possible problems and pathologies
There are more serious and less serious pathologies of the placenta. In the anatomical sense, there may be changes and deviations in the shape of the placenta from the norm, for example, it has an additional lobe or the umbilical cord is attached not in the middle, but in the membranes of the fetus or at the very edge. Sometimes this can be seen on ultrasonography, and sometimes these features are only discovered after childbirth. But there are more serious pathologies that require medical supervision or intervention. nine0003
Location of the placenta
Advertisement
Advertisement
Usually the placenta forms in the upper part of the uterus, but there are cases when it is attached directly to the front of the mother's abdomen in the uterus. In this case, the woman will feel the movements of the baby later, but this in no way affects the process of pregnancy or the development of the fetus.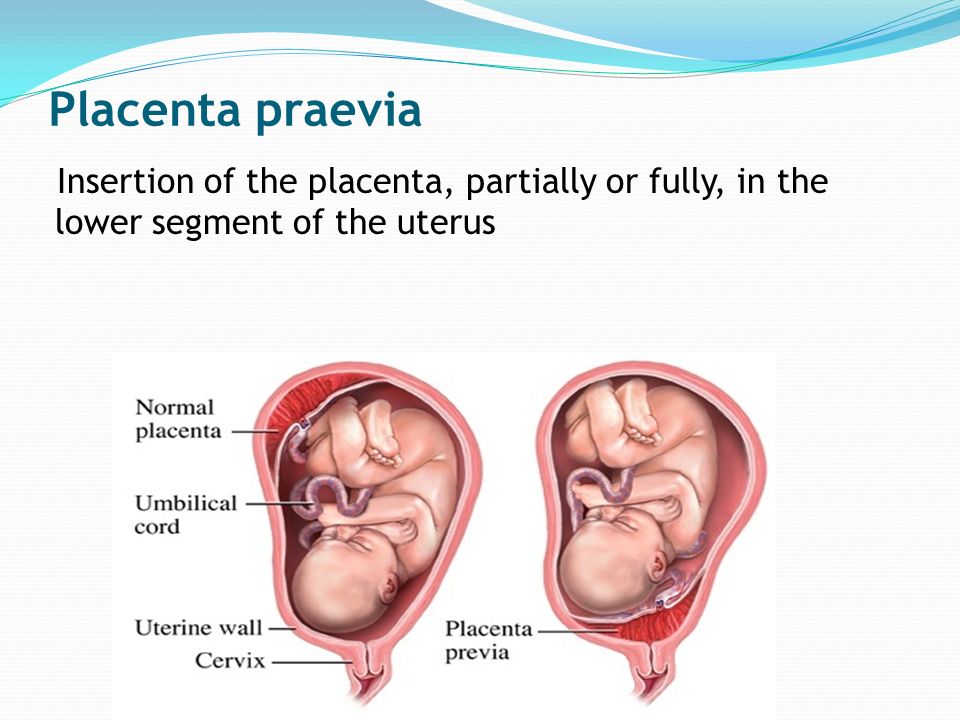 Worse, if the placenta is located low or even closes the mouth of the uterus, that is, it is presenting. True, how the birth will take place can only be said in the last trimester of pregnancy, since along with the growth of the uterus over time, the placenta can “rise”. nine0003
Worse, if the placenta is located low or even closes the mouth of the uterus, that is, it is presenting. True, how the birth will take place can only be said in the last trimester of pregnancy, since along with the growth of the uterus over time, the placenta can “rise”. nine0003
If even in the third trimester USG shows that the placenta is too low, then it is unlikely that it will rise higher. This means that the woman herself will not be able to give birth and will have to have a caesarean section, because when the cervix opens, the placenta can exfoliate and bleeding can begin. In the worst case scenario, neither mother nor child may survive. The woman herself cannot influence the location of the placenta or its elevation.
Preeclampsia
Disease of the placenta - preeclampsia - possible only in pregnant women. If a woman has preeclampsia, her entire body, including the placenta, narrows and spasms the blood vessels, which also significantly complicates the placental circulation and thus directly affects the well-being and growth of the fetus.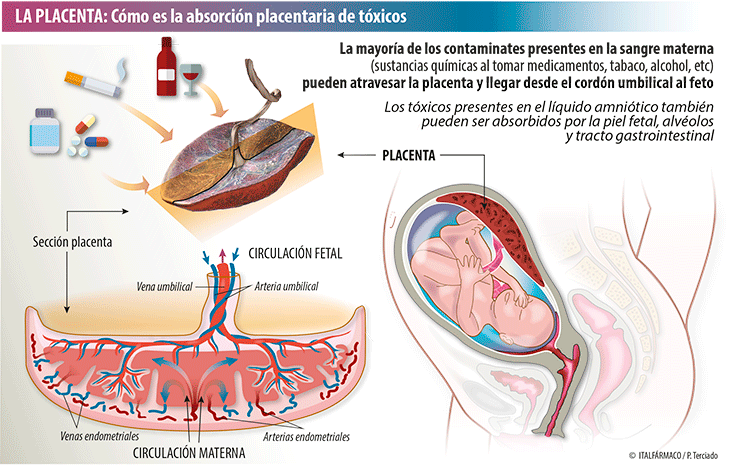
The baby is not getting enough nutrients and oxygen, so fetal growth retardation may occur. In turn, the mother has a greater risk of placental abruption, which threatens her life and the life of the baby. nine0003
Globally, high-risk pregnant women are advised to take prophylactic aspirin early in pregnancy (weeks 12-16), which reduces the risk of preeclampsia. The high-risk group includes women who have high blood pressure during pregnancy; the older the mother, the greater the risk of preeclampsia; in cases of multiple pregnancy; in the presence of systemic autoimmune and chronic kidney disease, diabetes and obesity.
Placental abruption
Placental abruption is a life-threatening condition for mother and baby. Usually it is associated with adverse circumstances during pregnancy, but the reasons why this can happen can most often not be foreseen in advance. If most of the placenta has separated, there may be abdominal pain and bleeding.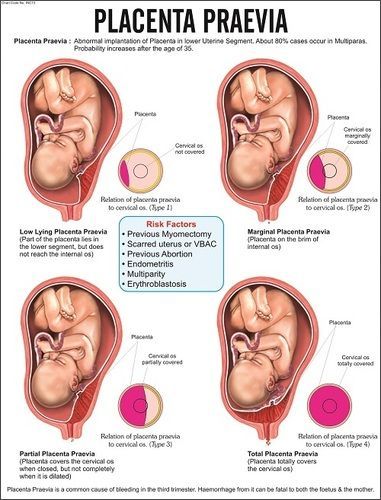 Sometimes the blood does not come out and remains at the placenta.
Sometimes the blood does not come out and remains at the placenta.
A pregnant woman begins to have pain in the lower part of her abdomen, then the pressure drops sharply, she feels cold and sweats. If the pain is severe, the pregnant woman should be taken to the hospital immediately. nine0003
If the placenta separates, the pregnant woman may lose consciousness. If only a small part of the placenta is separated, coagulation occurs and then recovery. In this case, the symptoms may be minimal. If a pregnant woman begins to bleed, she should be examined immediately, as the baby may not be getting enough oxygen. This can lead to distress and death of the fetus. In case of suspected placental abruption, you should immediately go to the hospital! If placental abruption is extensive, a caesarean section is performed. nine0003
Placenta accreta
Pathological placenta ingrowth into the uterine wall is a condition that threatens the health and life of a woman, which can result in a hysterectomy, or removal of the uterus.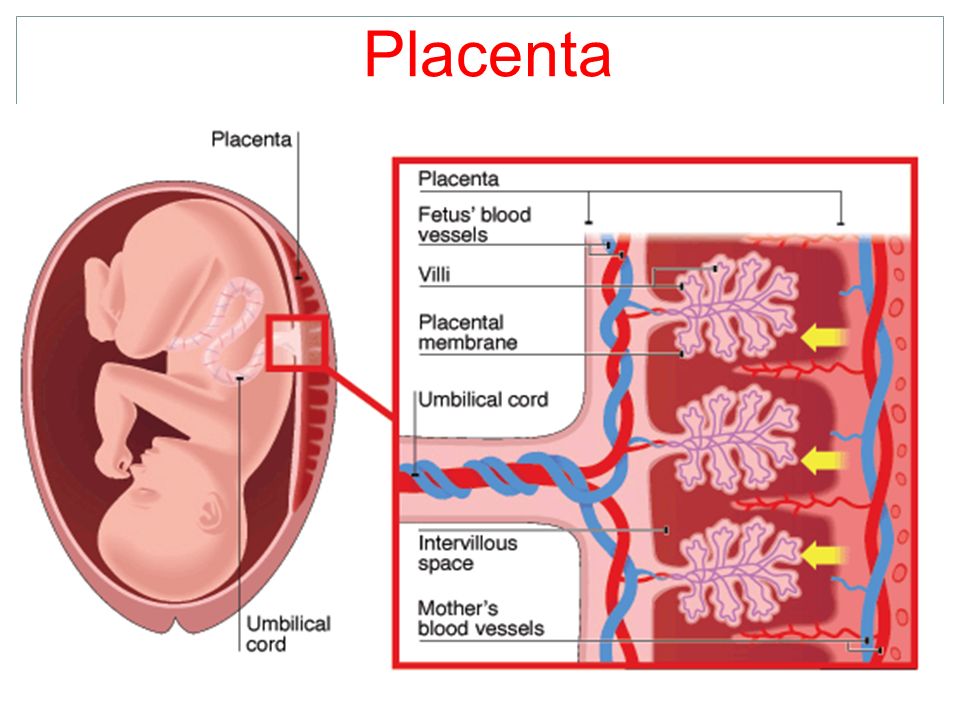 Most often, these are the consequences of previous caesarean sections or other manipulations in the uterine cavity - abortion, abrasion of the uterine cavity, removal of polyps, or any activity that affects and affects the condition of the uterine wall.
Most often, these are the consequences of previous caesarean sections or other manipulations in the uterine cavity - abortion, abrasion of the uterine cavity, removal of polyps, or any activity that affects and affects the condition of the uterine wall.
Dr. Katrina Kalnina notes that many women today do not appreciate how far-reaching the consequences of a caesarean section can be. Each subsequent pregnancy is associated with greater risks of placenta accreta. nine0003
If, during a caesarean section, it is determined that the placenta has grown in, it is estimated in what area and how deep this happened. Previously, to save their lives, women made the decision to remove the uterus, but in recent years they have been trying to follow a different tactic - the uterus is sutured, leaving the placenta in it, and in the coming weeks the placenta separates itself. The risk of inflammation and complications increases, but this is an opportunity to preserve the uterus and the woman's fertility.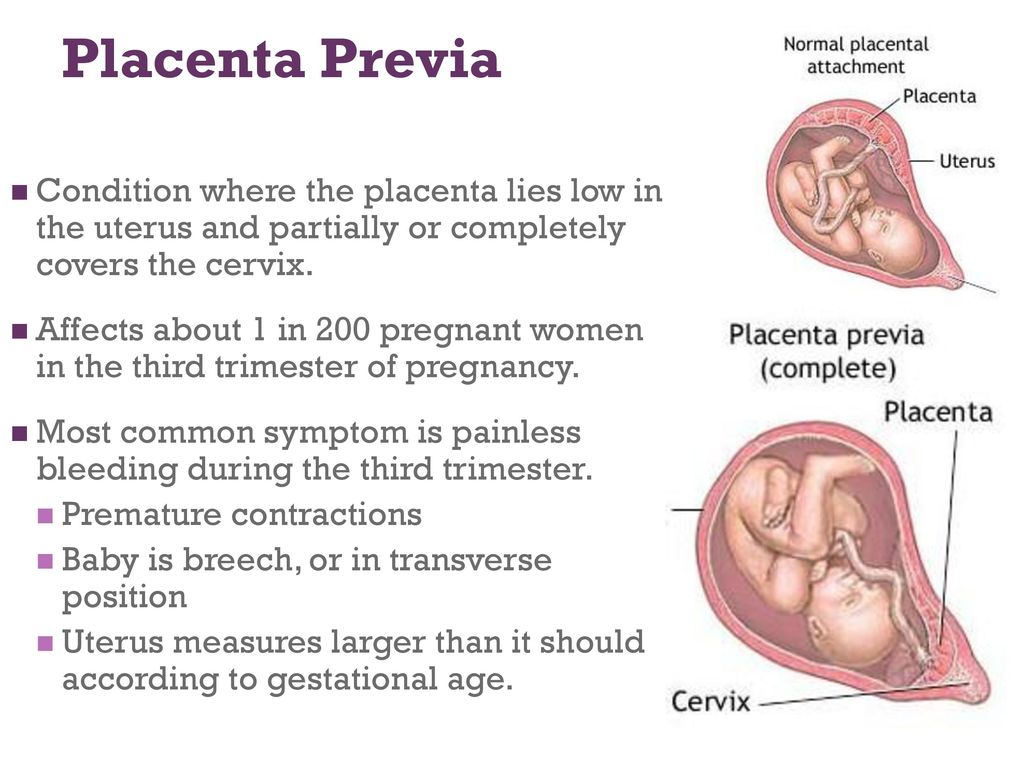
Another method that is gentle on the uterus - the placenta is cut out together with the wall of the uterus into which the placenta has grown, the scar is sewn up and the uterus is preserved. If there was placenta ingrown, then there is a higher risk that this problem will recur next time. Placenta ingrowth can be detected by ultrasonography, and sometimes magnetic resonance is also performed. nine0003
If twins are expected
If there is only one fetus, then there is one placenta that supplies it with everything it needs. It is more difficult if the pregnancy is multiple.
The best option is if each twin has their own placenta, or bichorionic placenta. If two twins share the same placenta, it is a monochorionic placenta. In such pregnancies, there is a possibility that the vessels of both fetuses are connected, and one twin receives more nutrients and oxygen than the other. As a result, it turns out that one twin has too much of everything, and the other does not have enough. Such difficult pregnancies can be quickly corrected. nine0003
Such difficult pregnancies can be quickly corrected. nine0003
NOTICE
Genetic tests
Since the placenta contains the same genetic material as the baby, pieces of placenta are used in genetic screening. A biopsy of the chorionic villi, if necessary, is carried out from the 11th to the 14th week - tissue from the placenta is taken with a needle. This is a fairly accurate method for determining the hereditary diseases of a child. There is a threat of spontaneous abortion in 0.2–1% of cases. Most often, this is checked for common pathologies of trisomies, if possible problems are identified at the first screening. nine0003
Wondering about the placenta
- Mother and baby's blood is filtered through the placenta but never mixed. At the end of pregnancy, 500 ml of the mother's blood passes through the placenta every minute.
- The placenta is an immune system messenger that helps the mother's and baby's immune systems communicate.












