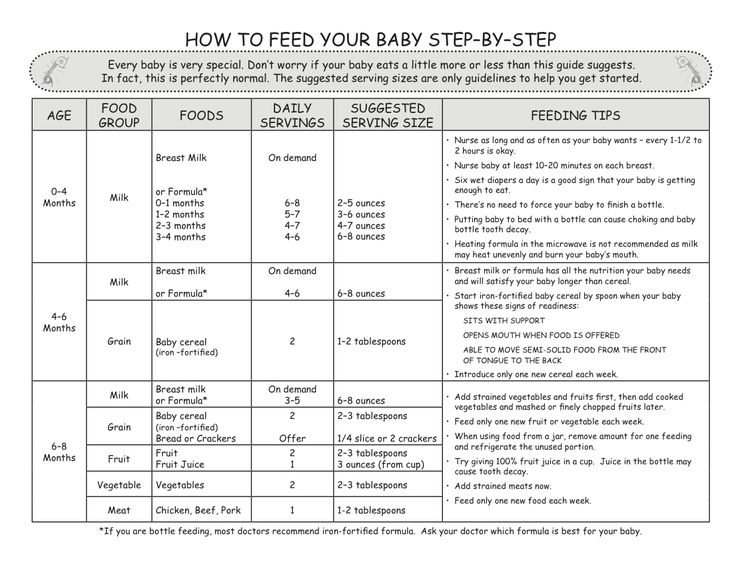
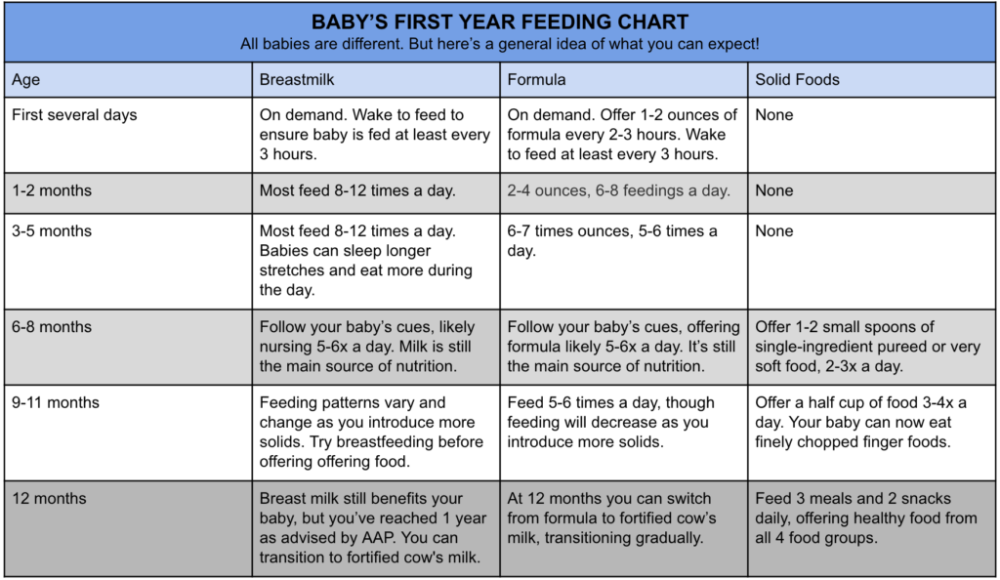
Pumping exclusively to feed baby
What You Should Know About Exclusive Pumping
Written by WebMD Editorial Contributors
In this Article
- Why Would You Pump Exclusively?
- How to Pump Breast Milk
- What Are the Pros and Cons of Exclusive Pumping?
Exclusive pumping is when you feed your baby only pumped milk, as opposed to direct breastfeeding.
In practice, you express (i.e., squeeze out) milk from your breast using a pump and then put the milk inside a bottle. You then feed your baby using the bottle or a nasogastric tube if they are premature. Just as you would when breastfeeding, you observe a pumping routine every time your child needs to feed, or you can express a lot of milk and store it in the fridge to warm when the baby needs it.
In most cases, exclusive pumping is done when the baby is not getting enough milk as they would when they are being breastfed (nursed) normally. This may happen if you are not producing enough milk or if your baby is not breastfeeding the right way.
Why Would You Pump Exclusively?
Exclusive breastfeeding is not for everyone. Although it is recommended that you feed your baby directly from the breast for the first six months, sometimes it may not be possible. As a result, you are left with no choice but to pump and feed your baby breast milk from a bottle. The most common reason for exclusive pumping is when your baby is not latching as they should. Latching is how the baby fastens onto the breast while nursing. Your lactation expert may advise you to pump every few hours or as your schedule allows.
When distance separates you and your baby. In some cases, a situation may arise that puts you away from your baby for a long time. For instance, the U.S. federal law provides up to 12 weeks of unpaid leave for the birth of a baby. You may be required to be back at work before it is time to wean your baby (i.e., make your baby used to food other than breast milk). If you are in such a position, pumping and leaving your baby’s caretaker with the pumped milk is almost inevitable. Pumping allows you to feed your baby on breast milk even when you are away.
Pumping allows you to feed your baby on breast milk even when you are away.
When you have tried your best to breastfeed and it does not work, pumping is the best option to feed your baby with breast milk. However, there are other reasons why you may find yourself adopting the practice. They include the following:
- Child adoption
- Congenital condition
- Breast anomalies
- Weight loss strategy
- Infant illness
- Oral anomalies
- Maternal choice
How to Pump Breast Milk
Pumping might feel strange if you have never done it before. You can always ask for suggestions from experienced mothers to help you. To do it best, start by finding a comfortable place with no distractions. It is important to be relaxed when collecting milk. Some mothers prefer looking at pictures of their children or listening to relaxing music.
Others get better results when they do hand expressing for 1 or 2 minutes before using the pump. The touch of your hand gives stimulation that helps to produce enough milk. Remember to stay hydrated by drinking plenty of water or alternative fluids.
Remember to stay hydrated by drinking plenty of water or alternative fluids.
Choosing a breast pump. Different breast pumps are good in different situations. To pump well, match your and your baby’s needs to a pumping system that meets them. You can consider the pump’s efficiency, ease of movement, and how much noise it makes.
You may find that a hand-operated pump works best for you if you only need to express occasionally. They are usually small, cheap, and easy to carry. If you will be pumping more often, go for an electric or double electric pump. These are recommended if the time you have to pump is limited and you will be pumping three or more times a day.
Electric pumps are automatic and quiet, and they usually mimic or imitate the suck-release pattern of a baby while breastfeeding. A double electric pump can be large, and it comes with a carrying case that resembles a handbag.
Another type of pump is the hospital-grade pump. This pump is only used in a hospital setting when you are separated from a prematurely born baby. Another instance when this type of pump can be used is when you need strong stimulation to produce enough milk. Since you cannot buy one of these, you can locate a hospital that rents theirs out if you are in need.
Another instance when this type of pump can be used is when you need strong stimulation to produce enough milk. Since you cannot buy one of these, you can locate a hospital that rents theirs out if you are in need.
What Are the Pros and Cons of Exclusive Pumping?
Pros. Exclusive pumping has certain advantages, including the following:
- Bonding: Breastfeeding requires privacy and can draw your attention away from other family members. Pumping allows your baby to feed without taking you away from your family.
- Someone else can help: Unlike breastfeeding where only the mother is involved, pumping allows you to give charge of feeding to someone else while you rest or do other things.
- Uninterrupted work: With exclusive pumping, you can work a demanding job and still manage to feed your baby on breast milk.
- Protect your milk supply: If you are unable to nurse for a period of time, pumping helps to keep your milk levels in check.

Cons. There are also some disadvantages of exclusive pumping, including the following:
- Expensive: Most good pumps are a bit pricey. When you consider other costs, like getting bottles and sanitizing products, breastfeeding directly is way cheaper.
- A lot of extra cleaning: The extra tools used for pumping need regular cleaning to make sure that you and your baby are protected from germs.
- Time-consuming: As opposed to picking your baby and holding them your breast to nurse (feed), pumping involves additional tasks, like thawing frozen milk you stored in the freezer.
- Lifestyle change: Because it is recommended that you pump at least once every night to ensure a good milk supply, waking up every night can change your sleep patterns. Also, you may find it boring to wake up every night to pump all by yourself.
When you begin to exclusively pump, it is normal to feel overwhelmed. Seek professional information and create a schedule that works for you and your baby.
If you need to use lubrication, consider olive oil and lanolin. Utilizing a lubricant helps you to avoid nipple damage and to reduce friction.
Why Do It, and How to Get Started
Need ALL the tips and tricks, right now? Use EP15 for 15% off! Shop Now
Are you thinking about exclusively pumping breast milk for your baby? When I started out, I had no idea what I was doing and pieced together information from internet searches. Here is all of the information you need in one place – what exclusive pumping is, the pros and cons of exclusive pumping vs nursing, and how to exclusively pump breast milk.
This post may contain affiliate links, which means that if you click a link and take action, I may make a small commission at no additional cost to you. I only recommend products I love! More info here.
What is Exclusive Pumping?
Exclusive pumping is breastfeeding using a breast pump and bottle.
Exclusively pumping moms pump breast milk around the clock to feed to their babies via a bottle. They do not nurse their babies for true feedings, though they may comfort nurse.
They do not nurse their babies for true feedings, though they may comfort nurse.
Exclusive pumpers may supplement with formula or feed their babies solid foods. “Exclusive” doesn’t refer to the baby only getting breast milk, like it does in the phrase “exclusively breastfeeding.”
The term “exclusive pumping” means that the baby is not nursed but is fed breast milk, and is meant to differentiate exclusive pumpers from (for example) moms that mostly nurse but pump at work.
Why Exclusively Pump?
Moms exclusively pump for many difference reasons. Some of the more common reasons for exclusively pumping include:
- Having a baby that refuses to nurse
- Difficulty with weight gain/baby doesn’t transfer milk well while nursing
- Physical reasons (such as cleft palate)
- Baby was in the NICU after birth and then had difficulty establishing nursing
- Baby has gotten teeth, and biting has become an issue
- Desire to provide baby with breast milk but aversion to nursing (sometimes due to sexual abuse, sometimes just personal preference)
Exclusively Pumping vs Nursing (aka Exclusively Pumping vs Breastfeeding)
First, exclusive pumping IS breastfeeding – it’s just not nursing. When you pump and feed your baby the milk you pumped, you are feeding from your breasts – just not directly. However, when people are asking this question, they often say “breastfeeding” when they mean “nursing.”
When you pump and feed your baby the milk you pumped, you are feeding from your breasts – just not directly. However, when people are asking this question, they often say “breastfeeding” when they mean “nursing.”
So – is it okay to just pump and not nurse?
Yes. Exclusive pumping is a perfectly valid option for feeding your baby.
However, there are advantages and disadvantages. Here are the exclusively pumping vs nursing pros and cons.
Exclusive Pumping Benefits
- You always know how much your baby is eating (so no “is she getting enough milk?” worries) – when you’re nursing, you have to guess unless you weigh your baby before and after feedings.
- You know how much milk you are producing and can see trends over time (especially if you track this data in an app). This way you can take action more quickly if your supply starts to drop. Nursing moms have to guess if supply is an issue or their baby is fussy for other reasons.
- You don’t have to worry about your baby biting, because breast pumps don’t have teeth!
- You are more in control of deciding when to wean, as breast pumps tend not to be as attached to the breastfeeding relationship.

Exclusive Pumping Challenges
- It’s a big time commitment – exclusive pumping requires about 120 minutes of pumping per day, in addition to the time you spend bottle feeding your baby breast milk. With nursing, the milk production and feeding steps are obviously combined.
- Pumping when you have a baby to take care of can be challenging.
- It requires a lot of energy and effort to wash all of the bottles and pump parts. Nursing moms have nothing to wash; formula feeding moms only have bottles.
More on pumping vs nursing here.
How Does Exclusive Pumping Work?
If you’re feeling overwhelmed by how to go about exclusively pumping, here is what you need to know.
How often should I be pumping? And for how long?This depends on how old your baby is.
When you’re exclusively pumping, you should be pumping for about 120 minutes per day (this is a minimum – you can pump more if you want to).
However, if your baby is a newborn, you’ll want to pump more often and for shorter periods of time than if you have an older baby. Read this if you have a newborn (0-3 months old), and this if your baby is older. Here are some sample pumping schedules.
Read this if you have a newborn (0-3 months old), and this if your baby is older. Here are some sample pumping schedules.
Once you’ve expressed your milk, here are guidelines for storing and using it.
What do I need to exclusively pump?The one thing you definitely need is a breast pump – preferably a double electric one (and hopefully covered by insurance)! I wrote about my opinions of some of the different options here.
There are also lot of breastfeeding products that can make the hours upon hours that you spend pumping much, much easier. The most important one is a hands-free pumping bra.
Other than that, some great investments include:
- Extra sets of pump parts
- Breast pads
- A nursing cover (so you can pump outside your house)
- A lactation massager (in case of plugged ducts or to help with letdowns)
 What should I do?
What should I do?Fear not! There are lots of things that you can do to get your milk supply up. I wrote up a long post about what you can do (what you can eat, herbs you can take, etc.) to increase your supply one about how to get the most milk out of each session (compressions, etc.), and one about how to get additional letdowns.
At a high level, some things that you can try include:
- Herbs (such as fenugreek or blessed thistle)
- Eating oatmeal
- Medication (such as domperidone or Reglan)
- Lactation cookies
- Power pumping
If you’re experiencing supply drops when you get your period, here are some things that you can do to try to mitigate the issue.
If you need to supplement with formula, here is how to do it if you are exclusively pumping.
I’m having nipple pain or breast pain. What is going on and how can I make it stop?Having breast pain as an exclusive pumper is the worst since you can’t take a break from pumping – you have to keep doing it every couple of hours regardless.
If you’re having breast pain related to pumping, the first thing that I would check is your breast shield size. Pumping with the wrong size breast shields can damage your nipples. Here is a great sizing guide from Medela that can help you determine if your flanges are too small or too big.
Here are some tips for how to treat and prevent a variety of issues that can occur when you’re breastfeeding:
- Clogged milk ducts
- Mastitis
- Galactoceles
- Thrush
- Milk blisters (otherwise known as blebs)
- Nipple vasospasms
- Cracked and Bleeding Nipples
- General nipple pain
It is hard, but there are so many little things that you can do to make it easier.
Some of the things you can do include: seeing if your baby will take the bottles that you pump into, setting up a “pumping station” so that everything you need is in one place, and getting comfortable with pumping on the go so you can get out of the house. (Speaking of getting out the house, you should also know how to pump and drive, travel with breast milk, and pump and fly.)
(Speaking of getting out the house, you should also know how to pump and drive, travel with breast milk, and pump and fly.)
As your baby gets older, one thing that can make exclusive pumping easier is to drop pumping sessions. Here’s how to do it without losing your milk supply.
I want to stop pumping and wean from the pump.When you’re wean from the pump, you’ll want to gradually drop pumping sessions – first you’ll go down to three sessions about eight hours apart, then to two pumping sessions 12 hours apart. Then you drop either the morning or night session – whichever is more annoying to you, and reduce the last remaining pumping session by time or volume. More info here.
Here is information on transitioning your baby off of breast milk when you wean.
I am the only person I know that is exclusively pumping and I feel alone.If you’re feeling alone, try reading some exclusive pumping stories from other exclusive pumpers. Also, join the newsletter and our Facebook group! You are not alone!
Also, join the newsletter and our Facebook group! You are not alone!
More exclusive pumping tips here.
Featured on:
As am Amazon associate I earn from qualifying purchases.
Feeding with expressed milk | breastfeeding
When can I start breastfeeding my baby with expressed breast milk? How to do it right? Is it worth worrying that the child will confuse the pacifier with the breast? In this article we will answer your questions.
Share this information
When can I start breastfeeding my baby?
If your baby is healthy and breastfeeding well, there is no need to give him expressed milk. For the first four weeks, you work together to start and increase milk production, and your baby also learns to suckle properly at the breast. There is not enough scientific data on this yet, 1 but there is an opinion that bottle feeding in the first month may adversely affect the process of establishing breastfeeding.
However, if the newborn is unable to latch on or suckle for some reason, start expressing milk as soon as possible after delivery. Read more about this in our articles on coping with problems in the first week, breastfeeding premature babies and babies with special needs, and seeking help from your healthcare provider. nine0003
How can I feed my baby with expressed breast milk?
There are many expert feeding solutions that allow you to give your baby expressed milk in a variety of ways, depending on your and your baby's needs.
For example, the innovative Calma smart pacifier only lets milk through when the baby creates a vacuum by suckling. This means that when feeding from a bottle, he will make the same movements with his tongue and jaws as when sucking at the breast. 2.3 Calma was developed with the help of breastfeeding experts from the University of Western Australia. When using this pacifier, the baby can suck, swallow, pause and breathe in the same way as when breastfeeding. 4 Preserving natural sucking habits allows baby to transition easily from breast to bottle and back.
4 Preserving natural sucking habits allows baby to transition easily from breast to bottle and back.
In addition, Medela also offers regular bottle teats* in two versions that produce milk at different rates. All Medela* nipples can be placed directly on bottles used for expressing milk, minimizing the risk of spillage. nine0003
If you need to feed your baby with expressed milk, but you do not want to bottle feed him until he is learning to breastfeed, you can use a sippy cup* for temporary feeding. The baby will be able to drink milk from such a mug, but you should be careful not to spill the milk. For the first time, it is advisable to feed the child from a drinking cup under the supervision of the attending physician in order to learn how to do it correctly.
If your baby needs to be supplemented with expressed milk in addition to regular breastfeeding, the Supplementary Feeding System (SNS)* can be used. It is equipped with a thin, flexible capillary that can be clipped close to the nipple to give your baby expressed milk while breastfeeding. Thanks to this, the baby suckles the breast for longer, thereby developing sucking skills and stimulating the production of milk from the mother. This can be helpful when there is a shortage of breast milk, as well as when feeding adopted or surrogate children. nine0003
Thanks to this, the baby suckles the breast for longer, thereby developing sucking skills and stimulating the production of milk from the mother. This can be helpful when there is a shortage of breast milk, as well as when feeding adopted or surrogate children. nine0003
If the baby is unable to breastfeed because he is too weak or has a congenital disease, you can use the Special Needs Cup*, which releases milk with gentle pressure, making it suitable for feeding these babies.
How to teach a child to bottle feed?
If breastfeeding is going well and you decide to start bottle feeding your baby with expressed breast milk, follow these guidelines.
Start early and take your time
Don't wait until the first day of work or the first time you leave the house to start bottle feeding your baby. Start accustoming your baby to small portions of expressed milk a couple of weeks before the desired date, calmly and without haste. Gradually build up to one full serving of pumped milk from a bottle.
Choose a time
Ideally, at the first bottle feeding, the baby should be hungry, but not too hungry - in this state, he is as relaxed as possible. nine0003
Let others feed
Your baby is used to feeding from your breast, so when you offer him a bottle it can be confusing. The process can go faster if the first time the baby is bottle-fed by someone else while you are not in the room, so that your sight and smell do not embarrass the baby.
Maintain optimal temperature
Your baby will be more willing to eat expressed milk if the temperature is around 37°C, close to body temperature. nine0003
Dip the nipple in milk
Try dipping the nipple in expressed milk before offering it to your baby. This way it will taste and smell like your breast milk. Lightly touch the baby's upper lip with the nipple to open the mouth.
Choose the right position for bottle feeding
Feed your baby on demand and keep him reclining during feeding. Never bottle feed your baby when he is lying or sitting, otherwise he may choke. Listen to the wishes of the child - take as many pauses as he needs. You can even try to shift it from one hand to another during feeding. nine0003
Never bottle feed your baby when he is lying or sitting, otherwise he may choke. Listen to the wishes of the child - take as many pauses as he needs. You can even try to shift it from one hand to another during feeding. nine0003
Be patient
Don't worry if your baby doesn't take the bottle right away - it may take several tries. If he pushes the bottle away or starts crying, calm him down, wait a few minutes and try again. If he still doesn't want to bottle feed, wait a few more minutes and breastfeed him as usual. Repeat the bottle experiment at a different time of day.
How much pumped milk should I give my baby? nine0009
All children are different. Research shows that between the ages of one and six months, a baby can consume between 50 and 230 ml of milk per feeding. To start, prepare about 60 ml and observe how much your baby needs - more or less. You will soon realize how much milk he usually eats. Just never force him to finish the cooked portion.
How can I keep my baby safe when bottle feeding?
Always clean and sterilize your pump and bottles according to the manufacturer's instructions. Wash your hands before expressing, pouring milk, and feeding your baby. Follow our instructions for safely storing and thawing your expressed milk. nine0003
If breastmilk needs to be warmed, place the bottle or bag in a bowl of warm water or a heater or under running water at a maximum of 37°C. Never heat breast milk in the microwave or on the stove.
Will the baby be able to transition from breast to bottle?
Some mothers worry that if they start bottle feeding too early, the baby will get used to the artificial nipple and not want to breastfeed. Others, on the contrary, are worried that if the child is not immediately accustomed to the bottle, then he will no longer eat from it. In general, in these cases, they say that the child confuses the nipple with the breast. nine0003
Experts disagree on whether such confusion is a problem. 1 Without a doubt, it is easier for a baby to suckle milk from a regular bottle with a nipple, which does not require a vacuum, than from the breast, since the milk flows faster, also under the influence of gravity. And some babies really have clear preferences: only the breast or only the nipple. However, many babies are comfortable suckling both the breast and the pacifier.
1 Without a doubt, it is easier for a baby to suckle milk from a regular bottle with a nipple, which does not require a vacuum, than from the breast, since the milk flows faster, also under the influence of gravity. And some babies really have clear preferences: only the breast or only the nipple. However, many babies are comfortable suckling both the breast and the pacifier.
If you are unable to feed your baby with expressed breast milk, seek help from a lactation consultant or specialist. nine0003
Literature
1 Zimmerman E, Thompson K. Clarifying nipple confusion. J. Perinatol. 2015;35(11):895-899. - Zimmerman I., Thompson K., "On the issue of breastfeeding." Zh Perinatol (Journal of Perinatology). 2015;35(11):895-899.
2 Geddes DT et al. Tongue movement and intra-oral vacuum of term infants during breastfeeding and feeding from an experimental teat that released milk under vacuum only. Early Hum Dev . 2012;88(6):443-449. - Geddes D.T. et al., "Language Movements and Oral Vacuum Generation in Term Infants During Breastfeeding and Feeding from an Experimental Vacuum-Delivery Teat". Airlie Hume Dev. 2012;88(6):443-449.
2012;88(6):443-449. - Geddes D.T. et al., "Language Movements and Oral Vacuum Generation in Term Infants During Breastfeeding and Feeding from an Experimental Vacuum-Delivery Teat". Airlie Hume Dev. 2012;88(6):443-449.
3 Segami Y et al. Perioral movements and sucking pattern during bottle feeding with a novel, experimental teat are similar to breastfeeding. J. Perinatol. nine0104 2013;33(4):319-323. - Segami I. et al., "Perioral movements and sucking during bottle feeding with a new experimental nipple are very similar to sucking from the breast." Zh Perinatol (Journal of Perinatology). 2013;33(4):319-323.
4 Sakalidis VS et al. Oxygen saturation and suck-swallow-breathe coordination of term infants during breastfeeding and feeding from a teat releasing milk only with vacuum. Int J Pediatr. 2012;2012:130769. - Sakalidis V.S. et al., "Oxygenation and Coordination of Sucking, Swallowing, and Breathing in the Term Infant During Breastfeeding and Feeding from a Purely Vacuum Teat". Int J Pediatrician 2012;2012:130769.
Int J Pediatrician 2012;2012:130769.
Read instructions before use. Consult a specialist about possible contraindications.
* RC № ФСЗ 2010/07353 of 07/19/2010
Storage, freezing and thawing of breast milk
Expressed breast milk is the best food for your baby when you are not around. How to store and use breast milk correctly?
Share this information
If you go to work, go to the gym or simply ask your partner to feed your baby and you want to get some sleep yourself, you can express breast milk so that the baby can eat even when you are not around. Most of the beneficial properties are retained in expressed breast milk, so if you are forced to skip breastfeeding, it will be a better replacement than any formula. But an important guarantee of the safety of expressed milk for your baby is hygiene. Read the article to learn how to properly store breast milk. nine0003
What is the best way to store breast milk?
Any type of breast milk is better for the baby than formula. But freshly expressed breast milk is better than chilled, and chilled breast milk is better than frozen. The fact is that freshly expressed milk fights bacteria better, it contains more antioxidants, vitamins and fats than chilled or frozen milk 4 .
But freshly expressed breast milk is better than chilled, and chilled breast milk is better than frozen. The fact is that freshly expressed milk fights bacteria better, it contains more antioxidants, vitamins and fats than chilled or frozen milk 4 .
How long expressed breast milk lasts
Once your breast milk is properly collected in a clean container, you can store it at room temperature, in the refrigerator or in the freezer, depending on how soon you plan to use it. Follow the guidelines below:
Recommendations for storing expressed breast milk (for feeding healthy term babies) 2, 3
| Storage location | Room temperature | Refrigerator | Freezer | Pre-frozen |
| Safe shelf life | Up to four hours Up to six hours for milk expressed under extra clean conditions* | Up to three days Up to five days for milk expressed under extra clean conditions* | Up to six months Up to nine months for milk expressed under extra clean conditions* | Up to two hours at room temperature Up to 24 hours refrigerated Do not freeze again! |
* "Very clean environment" refers to strict adherence to the instructions in the article on cleaning and sterilizing the Medela 9 breast pump0104 . These instructions for storing and thawing breast milk are guidelines only. For more information, contact a lactation consultant or healthcare professional.
These instructions for storing and thawing breast milk are guidelines only. For more information, contact a lactation consultant or healthcare professional.
If the baby is in the neonatal intensive care unit (NIU) or intensive care unit, stricter cleaning and storage guidelines may apply in accordance with the hospital's internal policies.
Before placing expressed milk in the refrigerator or freezer, be sure to mark the bottles or bags with the amount of milk and the date of expression. This will make it easier to manage your pumped milk supply. nine0003
Recommendations for feeding expressed breast milk
During storage, breast milk usually separates into layers and the fats (cream) it contains rise to the top. Shake the bottle lightly to mix the layers before giving it to your baby. Strong mixing and shaking can destroy some of the nutritional and protective components of breast milk 5 .
When a baby is fed expressed breast milk from a cup or bottle, bacteria from the mouth naturally enters the milk. Therefore, it is best to throw out all the unfinished milk one to two hours after the first feeding. In order to waste as little expressed milk as possible, it is best to store it in small portions and use just enough for one feeding 2 .
Therefore, it is best to throw out all the unfinished milk one to two hours after the first feeding. In order to waste as little expressed milk as possible, it is best to store it in small portions and use just enough for one feeding 2 .
How to Store Breast Milk in the Refrigerator
2, 3Follow the guidelines below to safely store expressed milk in the refrigerator.
- Refrigerate breast milk as soon as possible after pumping.
- Store milk in clean BPA-free breast milk bottles or breast milk storage bags. Its long-term effects on the human body are not well understood and manufacturers are now moving away from the use of this chemical in plastic containers and covers. nine0296
- After pre-cooling, a small amount of expressed milk can be added to the milk container stored in the refrigerator. Do not add warm breast milk to already chilled milk.
- Store breast milk in the coldest part of the refrigerator, on the back of the shelf above the vegetable drawer.
 Do not store milk in the refrigerator door where the temperature is not as constant.
Do not store milk in the refrigerator door where the temperature is not as constant.
How to store breast milk in the freezer
2, 3The following are guidelines for the safe freezing of breast milk.
- Freeze breast milk as soon as possible after pumping.
- After pre-cooling, expressed milk can be added to the already frozen milk container. Do not add warm breast milk to already frozen milk.
- To simplify defrosting and reduce waste, store milk in small portions (less than 60 ml). Once thawed, portions can be mixed. nine0296
- Make sure the breast milk container is suitable for freezing: some containers (eg glass bottles) may burst at low temperatures. Medela Breast Milk Storage Bags are ideal for storing frozen breast milk: they are ready to use, cold-resistant and easy to label.
- Do not fill bottles or bags more than 3/4 full as milk expands when frozen.
- Store frozen breast milk in the back of the freezer where the temperature is constant.
 Do not place it against the walls of freezers with automatic defrosting. nine0296
Do not place it against the walls of freezers with automatic defrosting. nine0296
Feeding frozen breast milk
2, 3Follow these guidelines when thawing breast milk to keep it safe for your baby.
- Breast milk can be thawed in the refrigerator, usually takes about 12 hours. You can place the bottle or bag of frozen milk under running warm water (max. 37 °C). Do not thaw breast milk at room temperature.
- Fully thawed breast milk can be stored for up to two hours at room temperature and up to 24 hours in the refrigerator. nine0296
- Do not thaw or reheat frozen breast milk in a microwave oven or in boiling water. This can negatively affect the nutritional and protective properties of breast milk, and due to uneven heating, the baby can burn.
- If, after defrosting, you left breast milk at room temperature, but did not feed it to the baby within two hours, the milk must be discarded.
- Do not refreeze breast milk.

How to warm up expressed breast milk
2, 3Healthy full-term babies can be given breast milk at room temperature or heated to body temperature. Some children care about the temperature of the milk, while others drink milk at any temperature.
- To warm breast milk, place the bottle or bag in a cup, mug or bowl of warm water for a few minutes until the milk is at body temperature (37°C). You can use a bottle warmer. Do not heat milk above 40°C or microwave it to avoid overheating. nine0296
- Slightly shake the milk in the bottle or bag to mix the separated fat (see above). Do not stir or shake the milk too hard.
Why does milk smell strange after storage?
Chilled or thawed breast milk may smell different from fresh
. This is due to the action of lipase, an enzyme that breaks down fats into fatty acids, preventing the growth of dangerous bacteria.
Some mothers report that their milk smells rancid or soapy after storage. But if you followed all the recommendations for safe storage given in this article, such milk is absolutely safe 2 .
But if you followed all the recommendations for safe storage given in this article, such milk is absolutely safe 2 .
Storing breastmilk on the road
If you need to transport your breastmilk from work to home or nursery, use the cool bag with ice packs 2 . For more information on pumping and storing breastmilk on the go, see the article on pumping on the go.
Literature
1 US Food & Drug Administration. Using a breast pump. [Internet]. Silver Spring, MD, USA: US Department of Health and Human Services; 2018 [updated 2018 Feb 04; cited 2018 Apr 12] Available from: www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/HomeHealthandConsumer/ConsumerProducts/BreastPumps/ucm061944.htm. "Instructions for using the breast pump". [Internet] Silver Spring, Maryland, USA: Department of Health and Human Services; 2018 [updated February 4, 2018; cited April 12, 2018] Article referenced: www. fda.gov/MedicalDevices/ProductsandMedicalProcedures/HomeHealthandConsumer/ConsumerProducts/BreastPumps/ucm061944.htm
fda.gov/MedicalDevices/ProductsandMedicalProcedures/HomeHealthandConsumer/ConsumerProducts/BreastPumps/ucm061944.htm
3 Eglash,A., Simon,L., & The Academy of Breastfeeding Medicine. ABM clinical protocol #8: human milk storage information for home use for full-term infants, revised 2017. Breastfeed Med 12, (2017). - Eglash A, Simon L and Academy of Breastfeeding Medicine, AVM Clinical Protocol #8: Home Storage of Milk for Term Infants 2017 Revision. Brestfeed Med (Breastfeeding Medicine) 12 (2917).
4 Human Milk Banking Association of North America. 2011 Best practice for expressing, storing and handling human milk in hospitals, homes, and child care settings. (HMBANA, Fort Worth, 2011).- North American Breast Milk Banks Association. Fort Worth: SABGM; 2011.
5 García-Lara NR et al. Effect of freezing time on macronutrients and energy content of breastmilk.