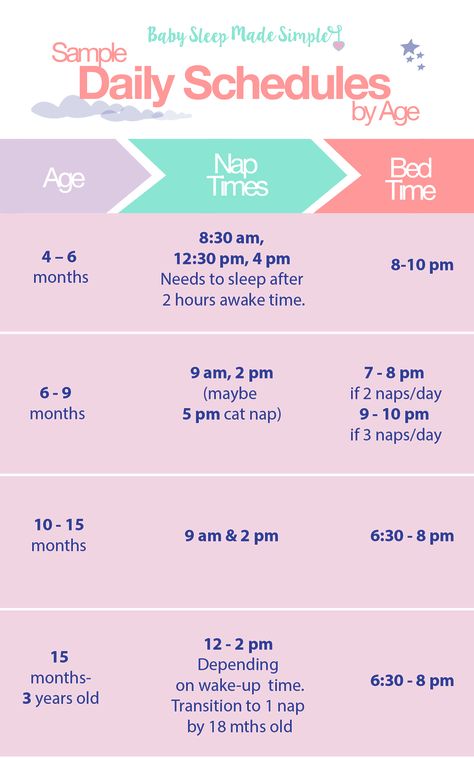
Artificial feeding baby
Breastfeeding vs. Formula Feeding (for Parents)
Choosing whether to breastfeed or formula feed their baby is one of the biggest decisions expectant and new parents will make.
Healt experts believe breast milk is the best nutritional choice for infants. But breastfeeding may not be possible for all women. For many, the decision to breastfeed or formula feed is based on their comfort level, lifestyle, and specific medical situations.
For moms who can't breastfeed or who decide not to, infant formula is a healthy alternative. Formula provides babies with the nutrients they need to grow and thrive.
Some mothers worry that if they don't breastfeed, they won't bond with their baby. But the truth is, loving mothers will always create a special bond with their children. And feeding — no matter how — is a great time to strengthen that bond.
The decision to breastfeed or formula feed your baby is a personal one. Weighing the pros and cons of each method can help you decide what is best for you and your baby.
All About Breastfeeding
Nursing can be a wonderful experience for both mother and baby. It provides ideal nourishment and a special bonding experience that many mothers cherish.
A number of health organizations — including the American Academy of Pediatrics (AAP), the American Medical Association (AMA), and the World Health Organization (WHO) — recommend breastfeeding as the best choice for babies. Breastfeeding helps defend against infections, prevent allergies, and protect against a number of chronic conditions.
The AAP recommends that babies be breastfed exclusively for the first 6 months. Beyond that, breastfeeding is encouraged until at least 12 months, and longer if both the mother and baby are willing.
Here are some of the many benefits of breastfeeding:
Fighting infections and other conditions. Breastfed babies have fewer infections and hospitalizations than formula-fed infants. During breastfeeding, antibodies and other germ-fighting factors pass from a mother to her baby and strengthen the immune system. This helps lower a baby's chances of getting many infections, including:
This helps lower a baby's chances of getting many infections, including:
- ear infections
- diarrhea
- respiratory infections
- meningitis
Breastfeeding also may protect babies against:
- allergies
- asthma
- diabetes
- obesity
- sudden infant death syndrome (SIDS)
Breastfeeding is particularly beneficial for premature babies.
Nutrition and ease of digestion. Often called the "perfect food" for a human baby's digestive system, breast milk's components — lactose, protein (whey and casein), and fat — are easily digested by a newborn.
As a group, breastfed infants have less difficulty with digestion than do formula-fed infants. Breast milk tends to be more easily digested so that breastfed babies have fewer bouts of diarrhea or constipation.
Breast milk also naturally contains many of the vitamins and minerals that a newborn requires. One exception is vitamin D — the AAP recommends that all breastfed babies begin receiving vitamin D supplements during the first 2 months and continuing until a baby consumes enough vitamin D-fortified formula or milk (after 1 year of age).
The U.S. Food and Drug Administration (FDA) regulates formula companies to ensure they provide all the necessary nutrients (including vitamin D) in their formulas. Still, commercial formulas can't completely match breast milk's exact composition. Why? Because milk is a living substance made by each mother for her individual infant, a process that can't be duplicated in a factory.
Free. Breast milk doesn't cost a cent, while the cost of formula quickly adds up. And unless you're pumping breast milk and giving it to your baby, there's no need for bottles, nipples, and other supplies that can be costly. Since breastfed babies are less likely to be sick, that may mean they make fewer trips to the doctor's office, so fewer co-pays and less money are paid for prescriptions and over-the-counter medicines.
Different tastes. Nursing mothers usually need 300 to 500 extra calories per day, which should come from a wide variety of well-balanced foods. This introduces breastfed babies to different tastes through their mothers' breast milk, which has different flavors depending on what their mothers have eaten. By tasting the foods of their "culture," breastfed infants more easily accept solid foods.
This introduces breastfed babies to different tastes through their mothers' breast milk, which has different flavors depending on what their mothers have eaten. By tasting the foods of their "culture," breastfed infants more easily accept solid foods.
Convenience. With no last-minute runs to the store for more formula, breast milk is always fresh and available whether you're home or out and about. And when women breastfeed, there's no need to wash bottles and nipples or warm up bottles in the middle of the night.
Smarter babies. Some studies suggest that children who were exclusively breastfed have slightly higher IQs than children who were formula fed.
"Skin-to-skin" contact. Many nursing mothers really enjoy the experience of bonding so closely with their babies. And the skin-to-skin contact can enhance the emotional connection between mother and infant.
Beneficial for mom, too. The ability to totally nourish a baby can help a new mother feel confident in her ability to care for her baby. Breastfeeding also burns calories and helps shrink the uterus, so nursing moms may be able to return to their pre-pregnancy shape and weight quicker. Also, studies show that breastfeeding helps lower the risk of breast cancer, high blood pressure, diabetes, and cardiovascular disease, and also may help decrease the risk of uterine and ovarian cancer.
Breastfeeding also burns calories and helps shrink the uterus, so nursing moms may be able to return to their pre-pregnancy shape and weight quicker. Also, studies show that breastfeeding helps lower the risk of breast cancer, high blood pressure, diabetes, and cardiovascular disease, and also may help decrease the risk of uterine and ovarian cancer.
p
Breastfeeding Challenges
Breastfeeding can be easy from the get-go for some mothers, but take a while to get used to for others. Moms and babies need plenty of patience to get used to the routine of breastfeeding.
Common concerns of new moms, especially during the first few weeks and months, may include:
Personal comfort. Initially, many moms feel uncomfortable with breastfeeding. But with proper education, support, and practice, most moms overcome this.
Latch-on pain is normal for the first week to 10 days, and should last less than a minute with each feeding. But if breastfeeding hurts throughout feedings, or if their nipples and/or breasts are sore, it's a good idea for breastfeeding mothers to get help from a lactation consultant or their doctor. Many times, it's just a matter of using the proper technique, but sometimes pain can mean that something else is going on, like an infection.
Many times, it's just a matter of using the proper technique, but sometimes pain can mean that something else is going on, like an infection.
Time and frequency of feedings. Breastfeeding requires a big time commitment from mothers, especially in the beginning, when babies feed often. A breastfeeding schedule or the need to pump breast milk during the day can make it harder for some moms to work, run errands, or travel.
And breastfed babies do need to eat more often than babies who take formula, because breast milk digests faster than formula. This means mom may find herself in demand every 2 or 3 hours (maybe more, maybe less) in the first few weeks.
Diet. Women who are breastfeeding need to be aware of what they eat and drink, since these can be passed to the baby through the breast milk. Just like during pregnancy, breastfeeding women should not eat fish that are high in mercury and should limit consumption of lower mercury fish.
If a mom drinks alcohol, a small amount can pass to the baby through breast milk. She should wait at least 2 hours after a single alcoholic drink to breastfeed to avoid passing any alcohol to the baby. Caffeine intake should be kept to no more than 300 milligrams (about one to three cups of regular coffee) or less per day because it can cause problems like restlessness and irritability in some babies.
She should wait at least 2 hours after a single alcoholic drink to breastfeed to avoid passing any alcohol to the baby. Caffeine intake should be kept to no more than 300 milligrams (about one to three cups of regular coffee) or less per day because it can cause problems like restlessness and irritability in some babies.
Maternal medical conditions, medicines, and breast surgery. Medical conditions such as HIV or AIDS or those that involve chemotherapy or treatment with certain medicines can make breastfeeding unsafe. A woman should check with her doctor or a lactation consultant if she's unsure if she should breastfeed with a specific condition. Women should always check with the doctor about the safety of taking medicines while breastfeeding, including over-the-counter and herbal medicines.
Mothers who've had breast surgery, such as a reduction, may have difficulty with their milk supply if their milk ducts have been severed. In this situation, a woman should to talk to her doctor about her concerns and work with a lactation specialist.
p
All About Formula Feeding
Commercially prepared infant formulas are a nutritious alternative to breast milk, and even contain some vitamins and nutrients that breastfed babies need to get from supplements.
Manufactured under sterile conditions, commercial formulas attempt to duplicate mother's milk using a complex combination of proteins, sugars, fats, and vitamins that aren't possible to create at home. So if you don't breastfeed your baby, it's important to use only commercially prepared formula and not try to make your own.
Besides medical concerns that may prevent breastfeeding, for some women, breastfeeding may be too difficult or stressful. Here are other reasons women may choose to formula feed:
Convenience. Either parent (or another caregiver) can feed the baby a bottle at any time (although this is also true for women who pump their breast milk). This allows mom to share the feeding duties and helps her partner to feel more involved in the crucial feeding process and the bonding that often comes with it.
Flexibility. Once the bottles are made, a formula-feeding mother can leave her baby with a partner or caregiver and know that her little one's feedings are taken care of. There's no need to pump or to schedule work or other obligations and activities around the baby's feeding schedule. And formula-feeding moms don't need to find a private place to nurse in public.
Time and frequency of feedings. Because formula is less digestible than breast milk, formula-fed babies usually need to eat less often than breastfed babies.
Diet. Women who opt to formula feed don't have to worry about the things they eat or drink that could affect their babies.
page 7
Formula Feeding Challenges
As with breastfeeding, there are some challenges to consider when deciding whether to formula feed.
Lack of antibodies. None of the antibodies found in breast milk are in manufactured formula. So formula can't provide a baby with the added protection against infection and illness that breast milk does.
Can't match the complexity of breast milk. Manufactured formulas have yet to duplicate the complexity of breast milk, which changes as the baby's needs change.
Planning and organization. Unlike breast milk — which is always available, unlimited, and served at the right temperature — formula feeding your baby requires planning and organization to make sure that you have what you need when you need it. Parents must buy formula and make sure it's always on hand to avoid late-night runs to the store.
And it's important to always have the necessary supplies (like bottles and nipples) clean, easily accessible, and ready to go — otherwise, you will have a very hungry, very fussy baby to answer to. With 8-10 feedings in a 24-hour period, parents can quickly get overwhelmed if they're not prepared and organized.
Expense. Formula can be costly. Powdered formula is the least expensive, followed by concentrated, with ready-to-feed being the most expensive. And specialty formulas (such as soy and hypoallergenic) cost more — sometimes far more — than the basic formulas. During the first year of life, the cost of basic formula can run about $1,500.
And specialty formulas (such as soy and hypoallergenic) cost more — sometimes far more — than the basic formulas. During the first year of life, the cost of basic formula can run about $1,500.
Possibility of producing gas and constipation. Formula-fed babies may have more gas and firmer bowel movements than breastfed babies.
Making a Choice
Deciding how you will feed your baby can be a hard decision. You'll really only know the right choice for your family when your baby comes.
Many women decide on one method before the birth and then change their minds after their baby is born. And many women decide to breastfeed and supplement with formula because they find that is the best choice for their family and their lifestyle.
While you're weighing the pros and cons, talk to your doctor or lactation consultant. These health care providers can give you more information about your options and help you make the best decision for your family.
Bottle-feeding babies: giving the bottle
About bottle-feeding
If your baby can’t always feed directly from your breast, you might choose to bottle-feed with expressed breastmilk. Or you might need to feed your baby infant formula, which is the only safe alternative to breastmilk.
Or you might need to feed your baby infant formula, which is the only safe alternative to breastmilk.
Before you bottle-feed your baby, it’s important to know how to clean and sterilise bottle-feeding equipment, as well as how to prepare, store and warm bottles of formula. This will help to keep your baby safe from infection and make sure baby is getting the right nutrition.
Getting the right flow when bottle-feeding
To test the flow of the formula or breastmilk, hold the bottle upside down when it’s filled with liquid at room temperature. The liquid should drip steadily from the teat but not pour out.
If you have to shake the bottle vigorously to see the drip, the flow is too slow. Your baby might go to sleep before drinking what they need.
When you feed your baby, you might see a little leakage at the corners of your baby’s mouth. This doesn’t mean the flow is too fast. It’s nothing to worry about. It will stop as your baby gets older.![]()
If you have trouble finding a teat with a flow to suit your baby, try a faster teat rather than a slower one. You might need to try a few different teats before you find one that suits.
Giving baby the bottle
Make yourself comfortable and cuddle your baby close to you, holding baby gently but firmly. It’s better for your baby to be on a slight incline so any air bubbles rise to the top, making burping easier.
Put the teat against your baby’s lips. Your baby will open their mouth and start to suck. Keep the neck of the bottle at an angle so it’s filled with formula or breastmilk.
When your baby stops sucking strongly or when about half of the formula or breastmilk has gone, gently remove the bottle and see whether baby wants to burp. Once you’ve tried burping your baby, you can offer the bottle again.
Paced bottle-feeding
Babies who are normally breastfed might find it hard to pace themselves when bottle-feeding, particularly if they’re premature.![]() This is because they’re used to controlling the flow of breastmilk. Sometimes these babies can drink too much too quickly.
This is because they’re used to controlling the flow of breastmilk. Sometimes these babies can drink too much too quickly.
Paced feeding can sometimes help. This involves holding your baby in an upright position and letting them rest every few minutes. If you’re interested in paced bottle-feeding, it’s best to get help from your child and family health nurse or a lactation consultant.
Holding, cuddling and talking to your baby during feeding will help baby develop and grow. It’s also a great opportunity to bond with your baby.
When baby doesn’t finish the bottle or goes to sleep while feeding
Don’t worry if your baby doesn’t finish the bottle. Babies are very good at judging how much they need, so you can let your baby decide when they’ve had enough formula or breastmilk.
If your baby goes to sleep during a feed, put baby over your shoulder, rub their back, and stroke their head, legs and tummy. This can help your baby to wake up. A nappy change is a good way to wake up your baby if that doesn’t work.
Wait until your baby is properly awake before offering the rest of the formula or breastmilk.
If there’s any formula or breastmilk left in the bottle, throw it away after one hour. When your baby drinks from a bottle of formula or breastmilk, bacteria from their mouth get into the milk. The bacteria can grow and make your baby sick if you give your the baby the half-finished bottle later.
When baby refuses the bottle
Babies sometimes refuse a bottle altogether. Here are things to try if this happens:
- Try a new feeding position or change the feeding environment. For example, move around while you’re feeding, find a quieter place to feed, or play some relaxing background music.
- Try again later when your baby is more settled. For example, give your baby a bath and then try again.
- Ask your partner or another family member to give your baby the bottle.
- Try using a different teat. If the flow of formula or breastmilk is too slow, it might frustrate your baby.
- Let your baby open their mouth for the bottle when they’re ready, rather than putting the teat into their mouth.
- Offer the formula or breastmilk from a small cup or spoon. To do this, sit your baby up and offer them small sips.
If your baby is regularly refusing the bottle, you could try adjusting your routine.
If you think your baby is refusing the bottle because they’re unwell, treat your baby’s symptoms or take your baby to see your GP.
How much do bottle-feeding babies drink?
Newborn babies commonly have 6-8 feeds every 24 hours, but there’s no set amount of food or number of feeds your baby should have. Different babies drink different amounts of formula or breastmilk. Some might have feeds close together and others further apart. And it can change from day to day.
Just feed your baby whenever they’re hungry. You’ll see baby cues that say ‘I’m hungry’ – for example, your baby will make sucking noises or start turning towards the breast or bottle. If your baby stops sucking or turns their head away from the bottle, you’ll know they’ve had enough.
If your baby stops sucking or turns their head away from the bottle, you’ll know they’ve had enough.
As your baby eats more and more solid food, the total amount of breastmilk or formula they take in a day will decrease. The amount of breastmilk or formula will also decrease as your baby starts to drink from a cup instead of a bottle.
Some babies never drink the ‘recommended amount’ for their age and size, and others need more. Plenty of wet nappies, consistent healthy weight gains, and a thriving, active baby mean all is well. If you’re concerned about how much breastmilk or formula your baby is taking, talk to your child and family health nurse or GP.
Bottle-feeding in bed: issues and risks
Sleep associations
If your baby gets used to falling asleep with a bottle in bed, they might depend on it to get to sleep. This can make it more difficult for your child to fall asleep or settle for sleep independently.
Bottle-feeding in bed also has several risks for your baby.
Choking
Babies who fall asleep while bottle-feeding can draw liquid into their lungs. They might then choke on it or inhale it.
Tooth decay
Babies have less saliva in their mouths to protect their teeth during sleep. If your baby falls asleep with a bottle, the lactose in the milk can build up on your baby’s teeth, putting your baby at risk of tooth decay.
Ear infections
If your baby drinks while lying flat, milk can flow into the ear cavity, which can cause ear infections.
It’s best to put your baby to bed without a bottle or to take the bottle away after your baby has finished feeding.
Using a feeding cup
When your baby is around 6 months old, you can help your baby start leaning to drink from a cup. It’s best to stop using bottles by the time your baby is 12 months old.
You should continue to thoroughly wash and sterilise feeding cups containing infant formula or breastmilk until your baby is 12 months old.
12 questions about artificial feeding of newborns ❤️ KIDY.eu
I may be in the minority, but I decided not to breastfeed my baby. Does this mean I'm a terrible mother? Are there any benefits of artificial feeding? How to bottle feed properly?
1
Is breastfeeding really better for the baby than others?
If you are able to breastfeed your baby, it is best for him. What are the benefits of breastfeeding? Breast milk contains all the nutrients necessary for the baby's body and is better absorbed. A breastfed baby is less likely to get sick, less prone to infections, since breast milk helps to strengthen the immune system. In addition, breastfeeding instills in the child a sense of security and closeness to the mother. However, if for some reason you are unable to feed your child or simply do not want to, be sure that he will grow up well on artificial nutrition.
2
I may be in the minority, but I have decided not to breastfeed.
 Does this mean I'm a terrible mother?
Does this mean I'm a terrible mother? No, this does not mean that you are a bad mother. In fact, statistics show that most women refuse breastfeeding and prefer to feed their baby with artificial mixtures. Do not torture yourself and do not be tormented by guilt: the choice of feeding method is your own business.
3
I know all the benefits of breastfeeding. Are there any benefits of artificial feeding?
There are indeed some advantages to artificial feeding. Some women love the freedom that artificial nutrition gives them. In this case, the mother can be replaced by someone else, for example, the father, who is also useful to participate in the care of the child. The interval between feedings in children who are bottle-fed is longer, since the baby digests mixtures longer than breast milk. In addition, you can accurately measure the amount of food needed for one feeding.
4
I chose formula for my baby.
 How to bottle feed properly?
How to bottle feed properly? - Hold your baby.
- Warm the mixture to body temperature by placing the bottle in warm water.
- Position the bottle so that the nipple is on the side of the baby.
- Do not touch the pacifier. Move the nipple over the baby's lips and put it in the mouth. Don't insist.
- Tilt the bottle so that the neck is full during feeding and the baby does not swallow air.
- Take the bottle away to give your baby a break. Usually the whole feeding takes 10-15 minutes.
- Never leave a baby to suckle a bottle alone.
- Never put a baby in the crib with a bottle.
5
Do I need to warm the bottle before feeding?
There is no evidence that unheated food is harmful to a child. Another thing is that if you usually heat the mixture, then the child is used to eating warm. The same applies to children who are used to breast milk, they will also like warm milk more. Be careful not to let the mixture get too hot!
Be careful not to let the mixture get too hot!
6
I don't know which mix to use. Are they different?
Yes, of course. Most babies eat milk-based formulas just fine, but some need to tailor the formula.
7
What types of formulas are there other than milk-based formulas?
There are several types of infant formula available today:
- milk-based formula, lactose-free , - for feeding children whose digestive tract cannot cope with lactose, which causes anxiety, gas, diarrhea;
- soy-based formula, neither milk nor lactose , - for feeding children with hypersensitivity or allergy to milk;
- hypoallergenic protein formula, easy to digest, lactose free - for feeding babies with colitis or other symptoms of milk protein allergy.
8
Allergy to cow's milk protein in a child: what a mother needs to know?
In babies under one year old, the most common "culprit" of allergies is cow's milk proteins (CMP). Neither formula-fed babies nor babies are immune from unwanted reactions. In the first case, allergies can be caused by mixtures that contain BCM. In the second, mother's nutrition can become the cause of allergies: if a nursing woman eats dairy products, their proteins can get into breast milk.
Neither formula-fed babies nor babies are immune from unwanted reactions. In the first case, allergies can be caused by mixtures that contain BCM. In the second, mother's nutrition can become the cause of allergies: if a nursing woman eats dairy products, their proteins can get into breast milk.
9
How does cow's milk protein (CMP) allergy manifest itself, what are the symptoms?
The most common gastrointestinal disturbances (regurgitation, bloating, diarrhoea, blood in the stool, etc.), as well as skin rashes and respiratory problems. For example, the baby may have wheezing, coughing or sneezing, wheezing. Other symptoms of CMPA include restlessness, refusal to eat, arching while feeding, poor sleep, or failure to gain weight. If a child is bottle-fed and you notice one or more symptoms in him, there is a reason to seek advice from a pediatrician or a pediatric allergist.
10
What to do if everything points to ABKM?
If the baby is bottle-fed, the solution will be the complete exclusion of cow's milk proteins from the child's diet - the so-called elimination diet - the transfer of the baby from the standard mixture to a specialized medical one.
11
Which mixtures are suitable for an elimination diet? Lactose free, goat milk based, specialized?
Lactose-free formulas do not contain lactose, but cow's milk proteins are present in them. Goat's milk-based formulas contain the same proteins as cow's milk. Finally, even a hypoallergenic formula with partially hydrolyzed protein is not suitable for children diagnosed with CMPA. Such crumbs need special specialized medical nutrition.
12
How long does it take to feed a baby with formula milk?
Data from the American Academy of Pediatrics has shown that iron-fortified formula milk should be fed to the baby during the first year of life to ensure adequate levels of iron in the body.
Artificial feeding for the little ones
The advantages of breastfeeding are indisputable: the child receives the necessary vitamins and minerals, strengthens the immune system, besides, food invented by nature itself is the best suited for the stomach and intestines of the newborn. But there are circumstances when a woman cannot breastfeed: due to illness, stress, and also after a caesarean section, milk can disappear very quickly. The baby has to be transferred to artificial feeding, but this does not mean that he will not grow up healthy if you follow some simple rules.
But there are circumstances when a woman cannot breastfeed: due to illness, stress, and also after a caesarean section, milk can disappear very quickly. The baby has to be transferred to artificial feeding, but this does not mean that he will not grow up healthy if you follow some simple rules.
Only a pediatrician can advise which formula is best to give to a newborn, since only he and the mother herself know the baby and the state of his health best of all. And how to feed a baby from a bottle, the mother's intuition will tell. If a woman does not have milk at all, the first days will have to worry a little for both the mother and the child. It doesn’t matter if the baby doesn’t immediately take the nipple: newborns are usually fed only after 10-12 hours, and the first time the baby doesn’t drink a lot of milk - no more than 20 g. After discharge from the hospital, he will drink more, so you can artificially feed gradually and more often.
Hold the bottle so that there is milk in the nipple all the time so that the baby does not swallow air. Still, a baby who is not yet able to suck properly from a nipple will still swallow some air. He may stop sucking and become anxious when air interferes with milk flow to the stomach. The newborn needs to be lifted, putting his head on his shoulder, and hold it for several minutes. Perhaps he will burp and calm down, but if he does not want to eat more, no need to insist.
Still, a baby who is not yet able to suck properly from a nipple will still swallow some air. He may stop sucking and become anxious when air interferes with milk flow to the stomach. The newborn needs to be lifted, putting his head on his shoulder, and hold it for several minutes. Perhaps he will burp and calm down, but if he does not want to eat more, no need to insist.
It is important that the hole in the nipple is the correct size. You can check this by turning the milk bottle upside down and seeing how the mixture flows. It should come out in a thin stream for the first seconds, then drip. If it continues to pour, then the hole is too large, and if it only drips at first, then it is too small. The hole can be pierced with a hot needle of the required thickness. When the child grows up, but will continue to drink from the bottle, the hole can be made larger.
For older children, you can alternate artificial milk formula with liquid cereals. After 2-3 months, you can start giving your baby oatmeal. It is prepared in the following way. A little oatmeal is poured with hot boiled water and allowed to brew until a liquid paste is formed, then filtered through gauze. This paste is added to boiling milk, then cooled to a temperature normal for feeding a baby. Liquid oatmeal is ready, it can be given to the baby from the nipple in the amount that the baby usually drinks. By 6 months, you can cook semolina porridge and give it from a nipple with a slightly larger hole.
It is prepared in the following way. A little oatmeal is poured with hot boiled water and allowed to brew until a liquid paste is formed, then filtered through gauze. This paste is added to boiling milk, then cooled to a temperature normal for feeding a baby. Liquid oatmeal is ready, it can be given to the baby from the nipple in the amount that the baby usually drinks. By 6 months, you can cook semolina porridge and give it from a nipple with a slightly larger hole.
Vegetable and fruit purees can be started along with oatmeal. If the pediatrician does not mind, they can be bought ready-made, or you can cook it yourself. For example, applesauce is prepared like this. A peeled apple is simmered in an enamel saucepan with a small amount of water and sugar. If the apple is very sweet, you can skip the sugar. Then the whole mass must be wiped through a fine strainer and the puree should be given to the child from a spoon. At 3 months, the baby is already able to grab a little food from a teaspoon, then he will be able to eat from a spoon better.