Baby refuses to feed
Feeding Aversion - Why your baby is refusing bottles, breast or solids – Baby Care Advice
When we imagine what it should look like to feed a baby, we picture a scene of a hungry baby, gently cradled in our arms, who serenely gazes towards us as he contently feeds, peacefully stopping when satisfied. This is in stark contrast to the way in which babies who develop an aversion to feeding or eating behave. The scene is one of a screaming, hungry baby who acts like you're trying to poison him when you offer him a bottle of milk, breastfeed, or solid foods.
What is a feeding aversion?An aversion is the avoidance of a thing or situation because it is psychologically linked with an unpleasant, stressful, frightening, or painful experience. Basically, it’s fear that is displayed in anticipation of something bad happening again. A ‘feeding phobia’ and ‘feeding strike’ are other terms that may be used to describe a feeding aversion.
A feeding aversion refers to a situation where a physically well baby, repeatedly exhibits partial or full feeding refusal despite obvious hunger. A feeding-averse baby has a history that demonstrates he’s capable of feeding but for reasons yet to be identified and corrected, he refuses to feed or eats very little.
Babies as young as 7 weeks of age can develop an aversion to breastfeeding or bottle-feeding. Older babies can become averse to eating solids. Not just certain foods but the experience of eating solids. A baby could become averse to one, two, or all three feeding methods.
Feeding aversion signs and symptoms:A baby might display one or more of the following behaviors:
- Skips feedings or meals without distress.
- Appears hungry but refuses to eat.
- Fusses or cries when a bib is placed around his neck, or when placed into a feeding position, or when the bottle is offered or shown.
- Clamps his mouth shut or cries and turns his head away from the breast, bottle, spoon, or food.
- Takes a few sips or a small portion of the milk or food offered but then pulls away or arches back in a tense manner or cries.
 (NOTE: Babies back arch to distance themselves. Back arching does not provide evidence of acid reflux.)
(NOTE: Babies back arch to distance themselves. Back arching does not provide evidence of acid reflux.) - Feeds only while drowsy or asleep.
- Consumes less milk or food than expected.
- Refuses milk but eats solids.
- Displays poor or slow growth. May be diagnosed as 'failure to thrive'.
The type and intensity of behavior vary between babies. At one end of the spectrum, a baby might simply refuse to eat a particular food owing to a bad experience while eating that food. At the other end, a baby might display almost complete food refusal, eating very little, and require a feeding tube to ensure that he receives sufficient nourishment for healthy growth.
Feeding is not something that a baby can avoid entirely. A feeding-averse baby will reluctantly eat enough to survive but not voluntarily eat enough to thrive. Once averse to feeding a baby will try to ignore his hunger cues for as long as possible. Only willingly, but cautiously, eating when ravenous. Then eating quickly in fear of a repeat occurrence of whatever it is causing his fears. Eating just enough to soothe pangs of hunger, but not enough to feel completely satisfied.
Then eating quickly in fear of a repeat occurrence of whatever it is causing his fears. Eating just enough to soothe pangs of hunger, but not enough to feel completely satisfied.
A few behaviors displayed by some, but not all, feeding-averse babies require special mention due to the confusion they cause. These include:
- Conflicted feeding behavior
- Sleep-feeding
- Accepts water from a bottle
Many feeding-averse babies display conflicted feeding behavior - where the baby takes a few sucks, sharply turns away or arches back in a tense manner, possibly cries, quickly returns and wants to suck again, takes a few sucks, turns away or arches back, cries, and returns to feeding and so on. This disjointed feeding behavior is often interpreted by parents and others as an indication that the baby is experiencing pain, especially if he is intermittently crying, but it’s not necessarily due to pain. Babies who have become averse to feeding will behave in this tense or distressed manner regardless of the cause.
Feeding-averse babies often feed better or well when drowsy or during light sleep. When drowsy or asleep, a baby is not fully aware that he is being fed, and therefore he’s not on edge in anticipation of whatever it is that is causing him to fear feeding. In a drowsy or sleepy state, a hungry baby’s guard is down, instincts kick in, and he feeds well. A feeding-averse baby may refuse and fight feedings while awake but could complete a full feed without resistance when drowsy or asleep. (See other reasons for sleep-feeding.)
Accepting water from a bottleA small percentage of feeding-averse babies willingly accept water from a bottle but not milk. This causes parents to believe it’s the taste of the milk that baby objects to, which could be the case, but not necessarily so. It can be because the baby associates the taste of the milk with an unpleasant or stressful experience, for example, being pressured to feed.
Parents often pressure their baby to drink milk from a bottle but seldom pressure their baby to take water from the bottle. Babies are smarter than we give them credit for. They learn to link the taste of the milk with being pressured and therefore react as soon as they taste the milk.
Why babies become averse to feedingA baby could develop an aversion to feeding if an event occurring directly before, after, or while he is feeding triggers negative emotional responses, such as stress, pain, fear, or disgust. Several scenarios could potentially trigger such emotions. For example:
StressIf a baby is pressured or forced to feed against his will, this makes for an annoying, frustrating, or stressful experience depending on the feeding strategies parents employ, and how long they persist.
Being repeatedly pressured to feed against their will is without exception THE most common reason for babies to develop an aversion to feeding and then not want to eat. In most cases, it's the original and only cause of a baby's feeding aversion. However, in around 10 percent of cases, it's a secondary cause that develops after the baby's initial feeding refusal due to one or more of the reasons that follow.
In most cases, it's the original and only cause of a baby's feeding aversion. However, in around 10 percent of cases, it's a secondary cause that develops after the baby's initial feeding refusal due to one or more of the reasons that follow.
Sucking could be painful if a baby has mouth ulcers, and swallowing could be painful if a baby is suffering from esophagitis caused by acid reflux, or milk protein allergy. Chronic constipation or gastroparesis (delayed emptying of the stomach) could also cause a baby to associate eating with discomfort.
When a baby refuses to feed due to discomfort or pain, the parent might then pressure their baby by employing subtle or obvious forms of pressure to make him eat. This adds to the baby’s distress. The baby now has two reasons to want to avoid feeding – pain and the stress associated with being pressured to eat. It’s often the stress associated with being repeatedly pressured to feed that continues to reinforce the baby’s avoidant feeding behavior long after medications or dietary changes have removed pain from the feeding experience.
Medical procedures involving the baby's face or mouth, like nasal or oral suctioning, insertion of an NG (nasogastric) feeding tube, or intubation can be frightening, painful, and stressful.
Aspirating fluids or choking on solids would make for a frightening experience. A baby could aspirate owing to dysphagia (an uncoordinated sucking-swallowing pattern) or due to moderate or severe laryngomalacia (floppy vocal cords), or because the flow rate from the nipple of a bottle or breast is too fast, or due to poor head or bottle positioning negatively impacting on the baby’s latch, suction, and sucking and swallowing coordination, or when the parent persists in trying to make their baby eat while he is crying in distress.
Disgust at taste of milk or medicinesBeing forced to take foul-tasting medicines or milk (which can be the case for hypoallergenic formula or if a mother produces high levels of lipase in her breastmilk) could cause the baby to develop an aversion to feeding. If medications are added into a baby’s milk bottle, which then changes the flavor of the milk, or if given via a nipple-like device this could cause a baby to reject bottle-feeds. Parents often resort to pressure or force to get their baby to swallow something that tastes unpleasant, adding another reason for the baby to want to avoid feeding, or anything else the parent might try to place into his mouth.
If medications are added into a baby’s milk bottle, which then changes the flavor of the milk, or if given via a nipple-like device this could cause a baby to reject bottle-feeds. Parents often resort to pressure or force to get their baby to swallow something that tastes unpleasant, adding another reason for the baby to want to avoid feeding, or anything else the parent might try to place into his mouth.
Babies affected by a sensory processing disorder may find the sensation of the nipple, or anything else in their mouth, to be abhorrent. They can display aversive behavior to lumps in food or the smell, taste, or feel of certain foods.
The cause of an infant feeding problem could be due to one or a combination of different causes. A feeding aversion can become even more complex when other feeding problems are involved. (See bottle-feeding problems.)
Other reasons for why your baby won't take a bottle, breast or solidsThere are several other possible reasons for individual babies to display aversive behavior towards breastfeeding, bottle-feeding, or eating solid foods. Any situation that results in a baby becoming frightened, stressed or experience pain while feeding has the potential to trigger partial or complete food refusal.
Any situation that results in a baby becoming frightened, stressed or experience pain while feeding has the potential to trigger partial or complete food refusal.
A single occurrence of one of these events doesn't usually trigger an aversion, but it is possible, especially if the experience is traumatic for the baby. It would generally take repeated occurrences while feeding to cause a baby to become averse to feeding. When such episodes are repeated, the baby learns to link the sequence of events and expect a similar occurrence each time he feeds. And so, he tries to avoid feeding to avoid the situation that has caused him fright, stress, or pain in the past. It's at this stage he will react before the event because he knows what's going to happen. And so, he may become distressed as soon as he recognizes he is about to be offered a feed. Or even if he thinks he is about to be fed because of the position he is held.
Is pain the cause for your baby's feeding refusal?The distress displayed by many feeding-averse babies can be so intense that it appears like they are suffering from pain. Therefore, pain is typically the first thing blamed by parents, and by health professionals during brief consultations, when other causes for a baby's feeding refusal are not obvious. However, pain is not the only reason for babies to become distressed during feeds.
Therefore, pain is typically the first thing blamed by parents, and by health professionals during brief consultations, when other causes for a baby's feeding refusal are not obvious. However, pain is not the only reason for babies to become distressed during feeds.
So how can you tell if pain is the cause of your baby’s troubled feeding behavior?Check how he behaves at times outside of feeding as this will provide clues. For example:
- If your baby is happy once you stop trying to feed him, pain is unlikely. Pain fades away. It doesn't suddenly cease because the feed has ended.
- If your baby is content between feeds, pain is unlikely. Discomfort associated with acid reflux or milk protein allergy or intolerance, constipation or gastroparesis is not restricted to feeding times only. Your baby would display signs of discomfort or distress at other times in addition to feeding times.
- If your baby predictably feeds well in certain situations, for example during the night or while drowsy or asleep, pain is unlikely to be the cause of his oppositional feeding behavior.
 Sleep does not numb a baby to the sensation of pain. If it is painful for him to feed during the day or while awake, it’s reasonable to expect it would also be painful for him to feed at night or when sleep-feeding.
Sleep does not numb a baby to the sensation of pain. If it is painful for him to feed during the day or while awake, it’s reasonable to expect it would also be painful for him to feed at night or when sleep-feeding.
NOTE: If your baby displays any unusual signs that might indicate illness or a physical problem, or if you are worried that your baby is suffering from pain, have him examined by a doctor.
Conflicted feeding behavior where baby takes a few sucks, sharply turns away or arches back, cries, quickly returns and wants to suck again, takes a few sucks, turns away or arches back, cries, returns to feeding and so on, is often interpreted by parents and others as pain, but its not necessarily due to pain. Babies who have become averse to feeding will behave in this way regardless of the cause. If your baby is quickly soothed once the feed has ended, it's probably not pain.
Is pressure the cause of your baby's feeding refusal?Some parents will pressure or force their baby to feed out of loving concern for their baby’s physical wellbeing. They hate doing this but do so because they worry that their baby will fail to gain sufficient weight or become unwell if they don’t make sure he consumes what they believe, or have been told, is an acceptable amount of milk or food.
They hate doing this but do so because they worry that their baby will fail to gain sufficient weight or become unwell if they don’t make sure he consumes what they believe, or have been told, is an acceptable amount of milk or food.
Many of the feeding strategies that we believe are ‘encouraging’ or ‘supporting’ a baby to eat involve subtle forms of pressure. For example:
- Pushing the nipple into a baby’s mouth against his wishes.
- Preventing him from pushing the nipple out of his mouth with his tongue.
- Following his head with the bottle when he turns or arches back in tense manner.
- Restraining his head to prevent him from turning away.
- Restraining his arms to prevent him from pushing the bottle away.
- Offering repeatedly at a time when he's rejecting or upset.
- Upwards pressure under his chin in a bid to trigger his sucking reflex.
- Gently compressing his cheeks to apply pressure on his buccal pads (cheek pads).

- Jiggling or twisting the bottle to try and make him continue sucking.
- Squeezing milk into his mouth.
- Trying to trick him into accepting the nipple by switching his pacifier for the nipple.
If these things don’t upset your baby - which generally appears to be the case for babies under the age of eight weeks who due to immaturity have limited ability to complain during the feed but can after the feed – such strategies might be causing no harm. However, doing these things in a bid to control how much a baby eats has the potential to make the experience of feeding unpleasant or stressful for the baby. When repeated, a baby can develop an aversion to feeding.
As a result of developing a feeding aversion the baby will fuss or refuse to feed and the parents, not knowing any better, may then feel compelled to force their baby to eat, and by doing so they may be unknowingly reinforcing their baby’s feeding aversion.
Behavior that is reinforced will continue. Once averse to feeding, the situation spirals downwards as a result of the ‘fear-avoidance-cycle’.
Once averse to feeding, the situation spirals downwards as a result of the ‘fear-avoidance-cycle’.
The more the parent pressures their baby, the less their baby is willing to eat. The less their baby eats, the more the parent pressures. And around and around it goes. The 'fear-avoidance-cycle' can spiral downwards to complete feeding refusal while awake, poor growth, and possible hospitalization where a feeding tube might be inserted.
Direct and indirect reinforcementsAny pressure, even subtle forms, has the potential to directly reinforce a feeding aversion. However, there are other strategies, for example feeding a baby while sleeping, giving solids to compensate for the loss of calories from milk, providing milk in other ways such as spoon, syringe, or feeding tube, can indirectly reinforce a behavioral feeding aversion by enabling the baby to avoid feeding while awake during the day. All reinforcements – direct and indirect – need to be removed.
Medical treatments
A feeding-averse baby is often distressed at feeding times (an exception being those who mostly sleep-feed during naps and at night). Pain is typically the first thing blamed, but the least likely cause of aversive feeding behavior displayed by physically well, thriving babies.
If you go to the doctor with a fussy baby who cries and refuses to eat, he or she may tend to explore physical causes before all others. The following treatments are often recommended by medical practitioners in a bid to remedy a baby's fussy or distressed feeding behavior.
Medications: Acid suppressing medications may be prescribed to treat suspected esophagitis - inflammation of the baby’s feeding tube caused by repeated exposure to refluxed stomach acid. And perhaps prokinetic medication (also called propulsive agents) to treat gastroparesis - delayed emptying of the stomach.
Dietary changes: A hypoallergenic infant formula may be recommended to treat suspected eosinophilic esophagitis - inflammation caused by an allergic reaction to cow’s milk based infant formula or soy infant formula.
Once the condition causing the baby's discomfort is effectively treated, his troubled feeding behavior will fade and disappear.
NOTE: A doctor cannot see into a baby’s esophagus and therefore cannot confirm if he is suffering from esophagitis during a routine medical examination. h3 antagonists and proton pump inhibitors used in the treatment of acid reflux are extremely effective in reducing the production of stomach acid. If your baby is still fussing or fighting feeds two weeks after commencing medications, there's a good chance that acid reflux is not responsible for his troubled feeding behavior. Similarly, if your baby's avoidant feeding behavior continues two weeks after switching to a specialized hypoallergenic formula, the reason may be that milk protein allergy is not the cause. This does not imply that your baby is not affected by these conditions, rather that these conditions are unlikely to be the cause of his avoidant feeding behavior.
This does not imply that your baby is not affected by these conditions, rather that these conditions are unlikely to be the cause of his avoidant feeding behavior.
Band-Aid solutions: If medications and dietary change fail to resolve a baby's aversive feeding behavior, band-aid solutions such as high-calorie feeds, food thickeners, starting solids, sleep-feeding, might be recommended in an attempt to minimize the risk of poor growth caused by an unresolved feeding aversion. However, band-aid solutions are often ineffective in the case of a feeding aversion because they do not address the cause, which is the stimulus that is causing the baby to fear feeding.
If medical treatments fail to resolve your baby's feeding issues, consider the possibility of a misdiagnosis or that there is more than one cause involved. And extend your search to cover other potential causes, in particular behavioral reasons such as being pressured to eat.
Speech therapyIf your baby often chokes or experiences problems with aspiration while feeding, his doctor might refer him to a speech therapist to assess his ability to suck and swallow effectively.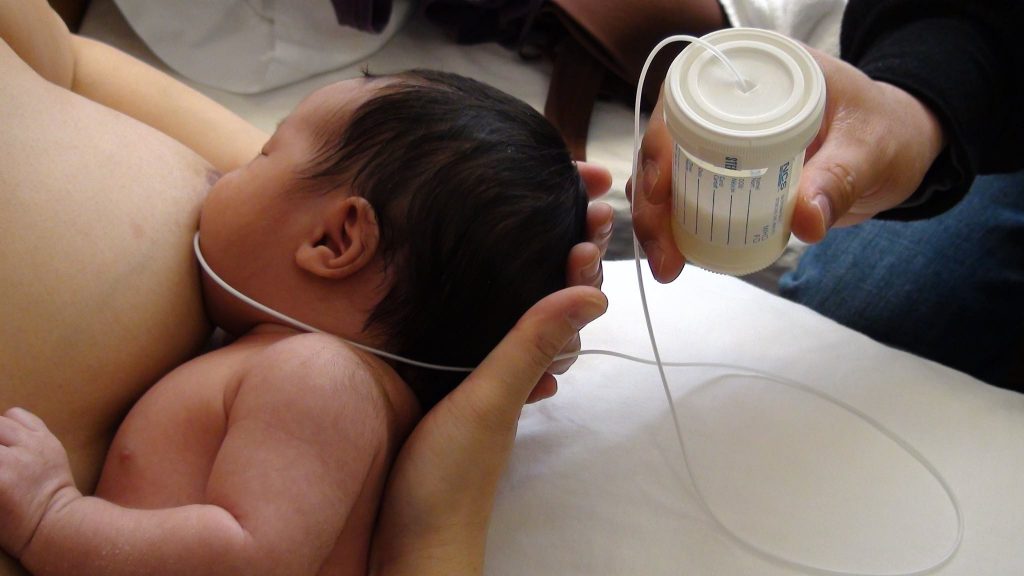 This can be helpful if choking episodes are reinforcing the baby's aversive behavior.
This can be helpful if choking episodes are reinforcing the baby's aversive behavior.
However, if your baby feeds well at some feeds for example in a sleepy state or has fed well in the past before developing a feeding aversion, it's unlikely that the source of his fussy feeding behavior or food refusal is due to a sucking or swallowing problem.
Occupational therapyIf an oral aversion due to a sensory processing disorder is suspected, your doctor might refer your baby to an occupational therapist for an assessment. Encouraging a child with oral aversion occurring due to a sensory processing disorder to feed as normally as possible requires a very long process that may last months or years.
An oral aversion is wide ranging with the baby not wanting anything near his mouth. A feeding aversion is specific, related to feeding, and requires very different treatment to resolve the problem compared to an oral aversion
NOTE: Some of the feeding strategies recommended to resolve an oral aversion, such as placing rubbery implements into the baby’s mouth to ‘desensitize’ him to the feel of things in his mouth, are counterproductive in the case of a behavioral feeding aversion that developed or is currently reinforced as a result of being pressured to feed. Placing things into a baby’s mouth without his permission will not regain his trust. Hence, the diagnosis must be correct. If your baby is happy to have anything other than the nipple of a bottle or food in his mouth, it’s probably a feeding aversion rather than an oral aversion.
Placing things into a baby’s mouth without his permission will not regain his trust. Hence, the diagnosis must be correct. If your baby is happy to have anything other than the nipple of a bottle or food in his mouth, it’s probably a feeding aversion rather than an oral aversion.
A behavioral approach views challenging infant behaviors such as incessant crying, fussy feeding behavior, feeding refusal, and sleeping problems in the context of the care the baby receives. In the case of physically well babies, it’s not assumed that the baby has a physical problem, rather the parent’s childcare practices are examined.
Infant behavior, whether this is desirable or undesirable behavior, is reinforced by the actions parents take or don’t take. To resolve a behavioral problem, and thus change a healthy baby’s behavior from fussy, distressed feeding refusal to enjoying feeding to satisfaction, it’s necessary for the parent to first make appropriate changes to their childcare practices.
The parent’s infant feeding practices are the last suspected cause of a healthy baby's aversive feeding behavior when it should be one of the first. You will know how thoroughly your baby’s healthcare professionals have assessed the possibility of behavioral reasons for his feeding issues by the number of questions asked of you regarding his feeding history. For example, feeding equipment, feeding frequency and duration, milk type, and concentration, feeding pattern, total daily milk intake, his sleeping patterns (sleep has a profound effect on feeding behavior and milk intake) and most important of all, your infant feeding and sleep settling practices. Our Baby Care Advice questionnaire includes 80+ questions to pinpoint the cause.
No questions asked = minimal to no consideration given to behavioral causes.
MisdiagnosisAccurate identification of the cause is essential to finding an effective solution. This is not something that can be achieved during a brief consultation with a health professional. And it definitely cannot be achieved without asking the parents multiple questions about their infant feeding practices. An accurate, and thorough diagnosis of the cause, or causes as is often the case, requires a comprehensive understanding of infant development and behavior, and age-appropriate infant feeding practices, as well as an understanding of the reasons and solutions to infant feeding aversion. At Baby Care Advice we allocate 2 hours for feeding problems.
And it definitely cannot be achieved without asking the parents multiple questions about their infant feeding practices. An accurate, and thorough diagnosis of the cause, or causes as is often the case, requires a comprehensive understanding of infant development and behavior, and age-appropriate infant feeding practices, as well as an understanding of the reasons and solutions to infant feeding aversion. At Baby Care Advice we allocate 2 hours for feeding problems.
Misdiagnosis occurs when assumptions are made about the cause in the absence of a comprehensive feeding assessment. Failure to accurately identify the stimulus causing and reinforcing the baby's feeding aversion - which can vary for individual babies - is likely to result in an ineffective treatment plan.
Not only will a misdiagnosis fail to address the cause, but many of the strategies recommended based on a misdiagnosis, such as those described as indirect reinforcements, have the potential to reinforce a baby’s aversive feeding behavior. A baby’s feeding aversion will continue while it’s reinforced. An unresolved breast- or bottle-feeding aversion increases the risk of the baby developing an aversion to eating solids for the same reasons. Feeding issues can persist for weeks, months or years.
A baby’s feeding aversion will continue while it’s reinforced. An unresolved breast- or bottle-feeding aversion increases the risk of the baby developing an aversion to eating solids for the same reasons. Feeding issues can persist for weeks, months or years.
Few health professionals are familiar with age-appropriate infant feeding practices and/or the process involved in resolving behavioral feeding aversions experienced by normal developing babies and young children. Therefore, they are ill-equipped to guide and support parents to resolve this complex and highly stressful situation.
A baby's avoidant feeding behavior, poor milk intake, and poor growth could be due to one or a combination of the causes already mentioned. However, a feeding aversion can become even more complex if other feeding issues are involved. For example, unsuitable or faulty equipment, poor feeding position, or the parent’s providing an inappropriate response to their baby’s feeding cues. (See bottle-feeding problems for more.)
(See bottle-feeding problems for more.)
If you suspect that your baby has developed a feeding aversion, there are a couple of ways we can help.
You might choose to see if you can figure things out on your own as a result of being guided by my book 'Your Baby’s Bottle-feeding Aversion’.
You might prefer to have one of our experienced consultants undertake a comprehensive assessment of all causes and provide individualized feeding advice. You also have the option to receive daily email guidance and support as you work towards resolving your baby’s feeding aversion.
You can purchase Rowena's Online Bottle-Feeding Aversion Program - six modules with clear step by step instructions on how to overcome your baby's bottle-feeding aversion. With a 95% success rate using Rowena's Bennett's method.
‘Your Baby's Bottle-Feeding Aversion’ bookIn my book, ‘Your baby’s Bottle-feeding Aversion’, I have described physical and behavioral reasons for babies to develop an aversion to bottle-feeding. How to identify the cause and the solutions to match. Included are step-by-step instructions on how to regain your baby’s trust and resolve a feeding aversion caused or reinforced by repeated pressure to feed.
How to identify the cause and the solutions to match. Included are step-by-step instructions on how to regain your baby’s trust and resolve a feeding aversion caused or reinforced by repeated pressure to feed.
While the book was written for bottle-fed babies, many nursing mothers have found that applying the same strategies has also helped them to successfully resolve a breastfeeding aversion.
You might find that reading this book is all you need to do to understand the steps you need to take to resolve your baby’s feeding aversion and get him back to the point of enjoying eating until satisfied.
Baby Care Advice ConsultationsIf you would like an individualized assessment of all reasons for infant feeding problems, not just feeding aversion, we also provide a consultation service. Baby Care Advice consultants have extensive experience in pinpointing the cause of feeding aversion and other behavioral feeding problems such as those related to equipment and the parent’s feeding practices. (For more on what’s included in a consultation).
(For more on what’s included in a consultation).
Six time-saving modules to help your family enjoy feeding again with Rowena's step-by-step plan. Enjoy additional tools to manage anxiety, troubleshoot any issues, introduce new carers, how to manage illness/teething and much more.
Join Our Facebook Support CommunityBaby Care Advice has facebook support groups in various languages, for those who have purchased either Rowena's 'Your Baby's Bottle-Feeding Aversion' book/ Online program/ consultation. They are made possible by a volunteer group of parents, who offer empathetic, compassionate support and guidance as you work your way through resolving your baby's feeding aversion.
English
Spanish
Dutch
Romanian
By Rowena Bennett, RN, RM, CHN, MHN, IBCLC.
Written Sept 2013. Revised July 2021.
Copyright www. babycareadvice.com 2021. All rights reserved. Permission from the author must be obtained to reproduce all or any part of this article.
babycareadvice.com 2021. All rights reserved. Permission from the author must be obtained to reproduce all or any part of this article.
Why is my baby refusing the breast? 8 tips that help | Baby & toddler, Feeding articles & support
Whether your baby refuses the breast as a newborn or when they’re older, it can be very stressful. Here’s why it might happen and what to try…
Why won’t my newborn baby breastfeed?
Sometimes, newborn babies struggle to latch on to breastfeed after they’re born. It can be worrying for new parents when this happens – you might think something’s wrong.
There may be a simple explanation. This information could help you find your own solution, or decide if you need further support.
Some of the more common reasons for newborn babies finding it difficult to latch onto the breast could be:
- a difficult labour or birth – your baby might feel sore or have a headache if the mother has had interventions in labour or if they were born very quickly
- medication used during labour – anaesthesia, epidural or pethidine can make your baby sleepy or groggy
- your baby being separated from you after birth – even for a few minutes
- discomfort due to a birth injury or bruising
- swallowing mucus at birth can make your baby feel congested, nauseous or uncomfortable
- an early unpleasant experience of attempting to breastfeed, such as being forced onto the breast
- the baby might have tongue-tie
(LLLGB, 2016)
Why won’t my baby breastfeed anymore?
Sometimes, older babies seem to refuse to breastfeed when they’d been breastfeeding just fine until then. This is known as a 'nursing strike.' They might refuse to breastfeed for 2-4 days, but it can be up to 10 days (Mohrbacher, 2013).
This is known as a 'nursing strike.' They might refuse to breastfeed for 2-4 days, but it can be up to 10 days (Mohrbacher, 2013).
Reasons that your older baby might refuse to feed at the breast could include:
- something has changed that makes it difficult for baby to latch
- a strong or fast flow of milk, which your baby is struggling to take
- a painful mouth, due to an infection like thrush or because they’re teething
- being more aware of their surroundings and being easily distracted, for example by noise
- a change in the taste of your milk, such as that due to your menstrual cycle
- the introduction of more solid food
- a small number of babies might struggle because of severe or persistent reflux, known as gastro-oesophageal reflux disease (GORD), so they may link feeding with pain.
(Mohrbacher, 2013; Gonzalez, 2014; BellyBelly, 2016; NICE, 2017; Public Health England, ND)
What can I do when my baby refuses to breastfeed?
8 top tips to help your baby who’s refusing to breastfeed:
1. Try to identify what’s going on for your baby. Knowing the cause can help not only with a plan but it can be reassuring to understand what is happening and know there’s a solution. You could think about the following:
Try to identify what’s going on for your baby. Knowing the cause can help not only with a plan but it can be reassuring to understand what is happening and know there’s a solution. You could think about the following:
- Do they have a cold or an infection?
- Was there something that might have caused them to not want to feed?
- Talk to one of our Breastfeeding Counsellors or contact our Infant Feeding Line on 0300 330 0700 (option 1) for further support. It can be a great way to get some help to find out what’s happening.
- You could also contact a health professional to investigate any medical reasons why your baby might not be feeding.
2. Try to stay calm and not force a feed. Instead, allow your baby to take the lead.
3. Especially for young babies, many mums find skin-to-skin contact in a laid-back position helps to take the pressure out of the situation. It allows your baby to use their own natural instincts to feed (Burbridge, 2017).
4. Don’t worry if your baby bobs their head or moves it from side to side, they’re not rejecting the breast as it might appear. These are your baby’s natural ways of finding your breast (Coulson, 2012).
5. Try a different feeding position to see if you can get your baby more comfortable. Some babies find a laid-back breastfeeding (also called biological nurturing) position helpful if they are struggling to get a deep latch or if you have a strong let-down of milk (Coulson, 2012).
6. Sometimes, feeding your baby while they’re sleepy or even asleep can be helpful. Many mums say that these ‘dream feeds’ can be very effective for a baby who is uninterested when awake (Pitman and Bennett, 2008).
7. You could try feeding your baby while rocking them or walking around, singing or playing with them or playing white noise or background music to them (Australian Breastfeeding Association, 2017).
8. You might want to try feeding in a quiet room, away from distractions, as some babies are so keen to be involved that they limit their feeds (Gonzalez, 2014).
You might want to try feeding in a quiet room, away from distractions, as some babies are so keen to be involved that they limit their feeds (Gonzalez, 2014).
What can I do if I’ve tried everything but my baby still won’t breastfeed?
One of the key things to consider is maintaining your milk supply. You might need to consider expressing, either by hand or with a pump. You can find more information about expressing and storing your milk here.
Another consideration is making sure your baby is getting enough milk. How might you know how much milk your baby is getting, you might ask. The answer lies in their dirty and wet nappies. You can expect six wet nappies in 24 hours if your baby is over a week old (UNICEF, 2016). If you’re unsure, it’s best to ask for support from your health visitor, GP or NCT breastfeeding counsellor.
In the short term, you might need to look at alternative ways to feed your baby if you think they’re not getting enough milk. A newborn baby needs to be fed regularly and parents can use syringe or cup feeding as an alternative to a bottle in the early days (Flint et al, 2016; NHS, 2016).
If you decide to use a bottle, it might be helpful to feed with plenty of skin-to-skin contact (UNICEF, 2018). Gently offering the bottle to your baby by tickling their top lip, waiting for the wide-open gape might also help mimic a breastfeed (UNICEF, 2019). That can support the transition back to the breast.
Taking frequent breaks during the bottle feed, and perhaps swapping sides, can be helpful (UNICEF 2018). Continuing to have skin-to-skin time with your baby and allowing them access to the breast will help this. It’ll also be a bonding and calming experience for you both.
How can I deal with the stress of my baby refusing to breastfeed?
When a newborn refuses the breast, or an older baby goes through a nursing strike, it can be very upsetting for both you and your baby. You’re definitely not alone in struggling with the emotions of breastfeeding problems. So here are some tips that might help:
- Try to take time to enjoy plenty of extra cuddles and quiet time together.

- Many mums find a ‘babymoon’ helpful for allowing their baby access to the breast in a non-pressurised way. A babymoon means spending some hours together in a relaxed setting, such as lying down snuggling in bed. This can allow you to enjoy your baby without worrying about feeding.
- For older babies, some mums find that having a bath with their baby or bringing their baby into bed with them helps their baby to latch.
- Try to find some support from other mums and trained breastfeeding supporters. Chatting with other people about this can help to unburden the stresses and worries you might be feeling. Breast refusal is not uncommon and you might find that chatting to someone who understands is invaluable while you’re struggling.
- For many mums, time and patience can help the situation. Your baby’s instincts and behaviour can change and develop, especially in the early days.
- If you’re struggling, do contact the NCT Infant Feeding Line and speak to a breastfeeding counsellor.
 They’ll listen, offer you information and will support you to find your own path.
They’ll listen, offer you information and will support you to find your own path.
This page was last reviewed in August 2019.
Further information
NCT supports all parents, however they feed their baby. If you have questions, concerns or need support, you can speak to a breastfeeding counsellor by calling our helpline on 0300 330 0700, whether you are exclusively breastfeeding or using formula milk. Breastfeeding counsellors have had extensive training, will listen without judging or criticising and will offer relevant information and suggestions. You can also find more useful articles here.
National Breastfeeding Line (government funded): 0300 100 021.
NHS information on mastitis.
Best Beginnings - Bump to Breastfeeding DVD Chapter 7 'Overcoming Challenges'.
Healthtalkonline.org: Managing Breastfeeding – dealing with difficult times.
References
Australian for Breastfeeding Association (2017) Breast refusal. https://www.breastfeeding.asn.au/bf-info/breast-refusal [Accessed 22nd February 2019]
https://www.breastfeeding.asn.au/bf-info/breast-refusal [Accessed 22nd February 2019]
BellyBelly. (2016) Breast refusal – 13 tips for a baby that refuses the breast.
https://www.bellybelly.com.au/breastfeeding/breast-refusal/ [Accessed 22nd February 2019]
Burbridge A. (2017) Nursing strikes. La Leche League GB. Available at: https://www.laleche.org.uk/nursing-strikes/ [Accessed 1st August 2019]
Coulson S. (2012) Biological nurturing: the laid-back breastfeeding revolution. Midwifery Today, 101 Available at: https://midwiferytoday.com/mt-articles/biological-nurturing/ [Accessed 1st August 2019]
Flint A, New K, Davies MW. (2016) Cup feeding versus other forms of supplemental enteral feeding for newborn infants unable to fully breastfeed. Cochrane Database Syst Rev. (8):CD005092. Available from: https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD005092.pub3… [Accessed 1st August 2019]
Gonzalez C. (2014) Breastfeeding Made Easy. London: Pinter &Martin
LLLGB. (2016) My baby won’t breastfeed. Available at https://www.laleche.org.uk/my-baby-wont-breastfeed/ [Accessed 1st August 2019]
(2016) My baby won’t breastfeed. Available at https://www.laleche.org.uk/my-baby-wont-breastfeed/ [Accessed 1st August 2019]
Mohrbacher N. (2013) Is your formerly nursing baby refusing to breastfeed? Breastfeeding Reporter Blog. Available at http://www.nancymohrbacher.com/articles/2013/1/26/is-your-formerly-nursing-baby-refusing-to-breastfeed.html?rq=refusing [Accessed 1st August 2019]
NICE. (2017) Breastfeeding problems. National Institute for health and Care Excellence, Clinical Knowledge Summaries. Available at: https://cks.nice.org.uk/breastfeeding-problems#!scenario [Accessed 1st August 2019]
Pitman T, Bennett H. (2008) 0-1 year: nursing strikes; breastfeeding while baby’s falling asleep may help end a nursing strike. Today’s Parent. 7:137.
Public Health England. (ND) Breastfeeding challenges. NHS, Start 4 life. Available at: https://www.nhs.uk/start4life/baby/breastfeeding/breastfeeding-challenges/reflux/ [Accessed 1st August 2019]
UNICEF. (2016) Breastfeeding checklist for mothers – How can I tell that breastfeeding is going well? UNICEF UK Baby Friendly Initiative. Available at https://www.unicef.org.uk/babyfriendly/wp-content/uploads/sites/2/2016/10/mothers_breastfeeding_checklist.pdf [Accessed 1st August 2019]
Available at https://www.unicef.org.uk/babyfriendly/wp-content/uploads/sites/2/2016/10/mothers_breastfeeding_checklist.pdf [Accessed 1st August 2019]
UNICEF. (2018) Skin-to-skin contact. Available from: https://www.unicef.org.uk/babyfriendly/baby-friendly-resources/guidance-for-health-professionals/implementing-the-baby-friendly-standards/further-guidance-on-implementing-the-standards/skin-to-skin-contact/ [Accessed 1st August 2019]
UNICEF. (2019) Responsive bottle feeding. Available from: https://www.unicef.org.uk/babyfriendly/wp-content/uploads/sites/2/2019/04/Infant-formula-and-responsive-bottle-feeding.pdf [Accessed 1st August 2019]
8 reasons why a child refuses to eat
Our life is impossible without food. From birth, a child has an instinct for eating. And with age, he does not cease to understand whether he wants to eat or not. Therefore, forcing a child to eat on the part of the parents is wrong. If the child grows and develops normally, then let him eat what he wants and how much he wants. Forcing the baby to eat, you can easily break his natural sense of proportion, and then fight overeating and being overweight. All children are different and it is important to give the child the amount of food that will satisfy his needs. And these needs depend on various factors. If the little one refuses to eat, try to understand the reason for this behavior.
Forcing the baby to eat, you can easily break his natural sense of proportion, and then fight overeating and being overweight. All children are different and it is important to give the child the amount of food that will satisfy his needs. And these needs depend on various factors. If the little one refuses to eat, try to understand the reason for this behavior.
1. The child is not hungry. Even if a long time has passed since the last meal, it is possible that the child is still full. Parents should take into account the calorie content of food and the energy consumption of the child. If the meal was high in calories, but after that the child watched cartoons and did not run in the yard, then he may not want to eat for a long time. Physical activity encourages the body to expend energy and the child will get hungry faster.
2. The child does not have a daily routine. It is advisable to feed the baby at about the same time. The optimal portion for a child is two of his palms folded together. In addition, it is necessary that the child every day spend time in the fresh air and go to bed on time. If the child has little active pastime, then do not be surprised that he does not eat well.
In addition, it is necessary that the child every day spend time in the fresh air and go to bed on time. If the child has little active pastime, then do not be surprised that he does not eat well.
3. The child is ill. Lack of appetite may be a symptom of some disease. Many children begin to eat badly when they are teething. Often the child refuses food when he has a fever. Before forcing a child to finish eating porridge, make sure that he is healthy.
4. The child "interrupts" the appetite. Sometimes snacking can cause a child to eat poorly at lunch or dinner. Do not give any cookies or sweets if you plan to sit down at the table soon.
5. The child does not like a particular dish. The baby may not refuse food in general, but simply milk porridge or borscht. Everyone has their preferences and kids have them too. Consider your child's preferences when planning menus. Accustom the little one to new tastes gradually, in the same way as complementary foods were introduced. Children are reluctant to perceive new tastes, but if given often and a little bit, they get used to it.
Children are reluctant to perceive new tastes, but if given often and a little bit, they get used to it.
6. The child has psychological problems. Children subtly feel the psychological situation in the family. Refusal to eat may be associated with a desire to attract the attention of parents to their person.
7. The child developed an eating neurosis. If parents force the child to eat regularly, without taking into account his desire, then the baby may develop food neurosis. Such children begin to cry at the sight of a plate, they can run away to another room and become hysterical.
8. All children are different. Do not compare your child with other children. All have their own physical characteristics. If the baby eats little, just make these small portions as healthy and nutritious as possible, but do not force him to eat more than he wants.
Do not treat the refusal of food as disobedience and whims. Try to understand what the problem is and solve it. Think and analyze your behavior, did you do everything as it should? If you realize what you did wrong, then try to quickly correct your mistakes. Use methods such as fairy tale therapy. Before going to bed, the child will listen with pleasure about his favorite fairy-tale hero, who ate well, so he was strong and courageous. Try to interest the child in the beautiful design of the dish. Ordinary products can become a castle, a car, a cute face - there is room for parental imagination to roam.
Try to understand what the problem is and solve it. Think and analyze your behavior, did you do everything as it should? If you realize what you did wrong, then try to quickly correct your mistakes. Use methods such as fairy tale therapy. Before going to bed, the child will listen with pleasure about his favorite fairy-tale hero, who ate well, so he was strong and courageous. Try to interest the child in the beautiful design of the dish. Ordinary products can become a castle, a car, a cute face - there is room for parental imagination to roam.
Refusal to eat | Nestlé Health Science
- Nestlé Health Science
- health care
- Refusal to eat
Refusal to eat is a feeding problem that usually occurs when the baby is six to nine months old. If the child does not eat due to excessive refusal to eat or lack of appetite, this can lead to growth problems.
Why is my child not eating?
As your baby develops, he will begin to establish a feeding routine with you. If you or your baby is not easily recognizing feeding signals, it can lead to confusion and refusal to eat.
An underlying medical condition may also be present, which can upset the child and lead to refusal to eat. A traumatic experience from eating a food that causes choking or vomiting can also lead a child to refuse to eat.
Symptom analysis
Could it be CMPA?
A child who does not eat or refuses to eat presents a typical symptom for infants with Cow's Milk Protein Allergy (CMP) .
Children with CMPA usually have more than one symptom, and these symptoms can be very different from each other.
If your child refuses to eat it could be CMPA.
You may have noticed other symptoms (besides refusal to eat) that may affect other parts of the child's body.
For a simple and easy way to check for typical symptoms associated with CMPA, you can use our Symptom Checker.
It will allow you to select all cow's milk symptoms your baby may have. You can then discuss this with your doctor.
In any case, if you have any doubts or concerns about your child's health, you should consult a healthcare professional as soon as possible.
Other symptoms of cow's milk protein allergy
ANAPHILACTIC SHOCK
View product
CRYING AND COLIC
View product
CONSTIPATION
View product
COUGH
View product
DIARRHEA
View product
ECZEMA
View product
GROWTH DISTURBANCE
View product
urticaria
View product
RASH
View product
REFLUX AND BUCK
View product
Runny nose and sneezing
View product
EDITEC
View product
VOMITING
View product
HRIP
View product
IMPORTANT NOTE: : It is possible to continue breastfeeding if the infant is allergic to cow's milk protein.











