Feeding baby after drinking
Alcohol | Breastfeeding | CDC
What is “moderate consumption”?
The Dietary Guidelines for Americans defines moderate consumption for women of legal drinking age as up to 1 standard drink per day.
What is a “drink”?
The Dietary Guidelines for Americans defines a standard “drink” as 12 ounces of 5% beer; 8 ounces of 7% malt liquor; 5 ounces of 12% wine; or 1.5 ounces of 40% (80 proof) liquor. All of these drinks contain the same amount (i.e., 14 grams, or 0.6 ounces) of pure alcohol. However, many common drinks contain much more alcohol than this. For example, 12 ounces of 9% beer contains nearly the same amount of alcohol as two (1.8) standard drinks. Consuming one of these drinks would be the equivalent of two standard drinks.
Is it safe for mothers to breastfeed their infant if they have consumed alcohol?
Not drinking alcohol is the safest option for breastfeeding mothers. Generally, moderate alcohol consumption by a breastfeeding mother (up to 1 standard drink per day) is not known to be harmful to the infant, especially if the mother waits at least 2 hours after a single drink before nursing. However, exposure to alcohol above moderate levels through breast milk could be damaging to an infant’s development, growth, and sleep patterns. Alcohol consumption above moderate levels may also impair a mother’s judgment and ability to safely care for her child.
Drinking alcoholic beverages is not an indication to stop breastfeeding; however, consuming more than one drink per day is not recommended.
Can alcohol be found in breast milk?
Yes. Alcohol levels are usually highest in breast milk 30-60 minutes after an alcoholic beverage is consumed, and can be generally detected in breast milk for about 2-3 hours per drink after it is consumed. However, the length of time alcohol can be detected in breast milk will increase the more alcohol a mother consumes. For example, alcohol from 1 drink can be detected in breast milk for about 2-3 hours, alcohol from 2 drinks can be detected for about 4-5 hours, and alcohol from 3 drinks can be detected for about 6-8 hours, and so on. However, blood alcohol levels and the length of time alcohol can be detected in breast milk after drinking will depend on a number of factors, including the amount of alcohol consumed, how fast the alcohol is consumed, whether it is consumed with food, how much a mother weighs, and how fast alcohol is broken down in a mother’s body.
However, blood alcohol levels and the length of time alcohol can be detected in breast milk after drinking will depend on a number of factors, including the amount of alcohol consumed, how fast the alcohol is consumed, whether it is consumed with food, how much a mother weighs, and how fast alcohol is broken down in a mother’s body.
What effect does alcohol have on a breastfeeding infant?
Moderate alcohol consumption by a breastfeeding mother (up to 1 standard drink per day) is not known to be harmful to the infant, especially if the mother waits at least 2 hours before nursing. However, higher levels of alcohol consumption can interfere with the milk ejection reflex (letdown) while maternal alcohol levels are high. Over time, excessive alcohol consumption could lead to shortened breastfeeding duration due to decreased milk production. Excessive alcohol consumption while breastfeeding could also affect the infant’s sleep patterns and early development.
Alcohol and Caregivers
Caring for an infant while intoxicated is not safe. Drinking alcohol could impair a caregiver’s judgement and his or her ability to safely care for an infant. If a caregiver drinks excessively, he or she should arrange for a sober adult to care for the infant during this time.
Drinking alcohol could impair a caregiver’s judgement and his or her ability to safely care for an infant. If a caregiver drinks excessively, he or she should arrange for a sober adult to care for the infant during this time.
Can expressing/pumping breast milk after consuming alcohol reduce the alcohol in the mother’s milk?
No. The alcohol level in breast milk is essentially the same as the alcohol level in a mother’s bloodstream. Expressing or pumping milk after drinking alcohol, and then discarding it (“pumping and dumping”), does NOT reduce the amount of alcohol present in the mother’s milk more quickly. As the mother’s alcohol blood level falls over time, the level of alcohol in her breast milk will also decrease. A mother may choose to express or pump milk after consuming alcohol to ease her physical discomfort or adhere to her milk expression schedule. If a mother decides to express or pump milk within two hours (per drink) of consuming alcohol, the mother may choose to discard the expressed milk. If a mother has consumed more than a moderate amount of alcohol, she may choose to wait 2 hours (per drink) to breastfeed her child, or feed her infant with milk that had been previously expressed when she had not been drinking, to reduce her infant’s exposure to alcohol. Breast milk continues to contain alcohol as long as alcohol is still in the mother’s bloodstream.
If a mother has consumed more than a moderate amount of alcohol, she may choose to wait 2 hours (per drink) to breastfeed her child, or feed her infant with milk that had been previously expressed when she had not been drinking, to reduce her infant’s exposure to alcohol. Breast milk continues to contain alcohol as long as alcohol is still in the mother’s bloodstream.
Drinking Alcohol and Breastfeeding - La Leche League International
Skip to: Overview
Skip to: Can Drinking an Alcoholic Beverage Help Me Relax and Stimulate Milk Production?
Skip to: What are the Risks To My Baby?
Skip to: What Other Effects Should I Consider When Deciding Whether and When To Drink?
Skip to: Can I Nurse My Baby and Still Drink Occasionally?
Skip to: How Is One Drink Defined?
Skip to: Important Considerations
Skip to: Do I Have To Pump And Dump After Drinking an Alcoholic Beverage?
Skip to: What if I Get Drunk?
Skip to: Can Alcohol Dependency/Self-medicating With Alcohol Affect A Breastfed Baby?
Skip to: Weighing The Risks And Benefits
Skip to: References
Skip to: Further resources
Breastfeeding mothers and lactating parents often receive conflicting advice about whether alcohol consumption can have an effect on their baby. While warnings are often given not to consume alcohol during pregnancy due to evidence that it could cause damage to an unborn child, the risks of consuming alcohol while breastfeeding have not received as much research attention. A number of studies have focused on the effects of alcohol on lactation and the infant, but long-term outcomes are still unknown.
While warnings are often given not to consume alcohol during pregnancy due to evidence that it could cause damage to an unborn child, the risks of consuming alcohol while breastfeeding have not received as much research attention. A number of studies have focused on the effects of alcohol on lactation and the infant, but long-term outcomes are still unknown.
Especially when it is consumed in large amounts, alcohol can cause drowsiness, deep sleep, weakness, and abnormal weight gain in the infant. There is also possibility of decreased milk-ejection reflex in the mother. No harmful effects to babies have been found when breastfeeding mothers drink no more than one drink a day.
Depending on how much alcohol you consume before you nurse your baby, may experience a number of effects from the alcohol in your milk. Even a small to moderate amount of alcohol may impair milk production and the milk ejection reflex. Some of the negative effects in the baby may be:
- Sleep disturbances,
- Increased crying
- Increased startling
- Increased arousal
- Increased REM sleep in the period from 3.
 5 hours to 24 hours after exposure to alcohol
5 hours to 24 hours after exposure to alcohol - Decreased milk intake by baby
- Decreased weight gain
Potentially, depending on how much you drink and when you nurse your baby after drinking, there may be other, more severe effects on your baby as well. As a result, the guidance on drinking and nursing is changing. According to the CDC, “moderate alcohol consumption is defined as having up to 1 drink per day for women and up to 2 drinks per day for men”.[1]. We go into more detail below.
In brief, LactMed® [2], a database that contains information on drugs and other chemicals to which those who are breastfeeding may be exposed, offers the following information:
“Breastmilk alcohol levels closely parallel blood alcohol levels. The highest alcohol levels in milk occur 30 to 60 minutes after an alcoholic beverage, but food delays the time of peak milk alcohol levels. Nursing after 1 or 2 drinks (including beer) can decrease the infant’s milk intake by 20 to 23% and cause infant agitation and poor sleep patterns. Nursing or pumping within 1 hour before ingesting alcohol may slightly reduce the subsequent amounts of alcohol in breastmilk.”
Nursing or pumping within 1 hour before ingesting alcohol may slightly reduce the subsequent amounts of alcohol in breastmilk.”
Infants exposed to a significant amount of alcohol (0.3 g/kg parent’s body weight) through drinking human milk, spend significantly less time in both active and total sleep. REM sleep is also disrupted. As infants are less able to process alcohol than adults due to their immature systems, some researchers believe that the dosage they receive through their mother’s/lactating parent’s milk may be stronger than it would be in an adult. In research conducted by Mennella and Garcia-Gomez, when an infant’s exposure occurred within 3.5 hours of a mother/lactating parent consuming a significant amount of alcohol, the effects were stronger. In the following 24-hour period, sleep patterns continued to be disrupted as the infant makes up for the earlier disruption. In addition, the research showed that during times when the infants were awake, they were less active [3].
Here are some common questions people ask with recommendations supported by the evidence available. Below, we will answer these questions and look at the possible impacts of drinking alcohol while breastfeeding in more detail. We will end with some tips for increasing safety if you want to drink alcohol while breastfeeding/chestfeeding/nursing (see How Can I Nurse My Baby and Still Drink Occasionally?). Pumping and dumping will not remove the alcohol from your bloodstream, so it will not affect the alcohol level in your milk.
CAN DRINKING AN ALCOHOLIC BEVERAGE HELP ME RELAX AND STIMULATE MILK PRODUCTION?A long-standing “old wives’ tale” regarding consumption of alcohol, particularly beer, while breastfeeding, is that it can help boost milk production. While a barley component in beer–not the alcohol–does boost prolactin production [4], alcohol alone does so as well [5] However, in one study, milk production was actually decreased [6]. In addition, in their research on alcohol consumption in lactating women Menella et al found alcohol also inhibits the milk ejection reflex and thus reduces the baby’s milk intake [5].
The research shows that nursing infants actually consumed less milk in the three-to-four-hour period after mothers consumed a small to moderate amount of alcohol [7,8,9]. When a mother/lactating parent drinks alcohol and then breastfeeds their baby, their perception is that the baby nurses normally and for a normal time, so they do not realize that their baby is not getting as much milk [7]. According to Menella, who conducted this research on this over a period of years, “infants consumed approximately 20% less breast milk”. This was the case even though the infants nursed a “similar number of times during the first 4 hr after exposure to alcohol in mothers’ milk” (pp. 591-592) compared with nursing infants not exposed to alcohol in their mother’s milk [9]. Similarly, additional research conducted by Menella and Beauchamp showed that infants consumed about 23% less milk [7]. Menella also found that when pumping milk two hours after drinking alcohol, mothers obtained significantly less milk [8].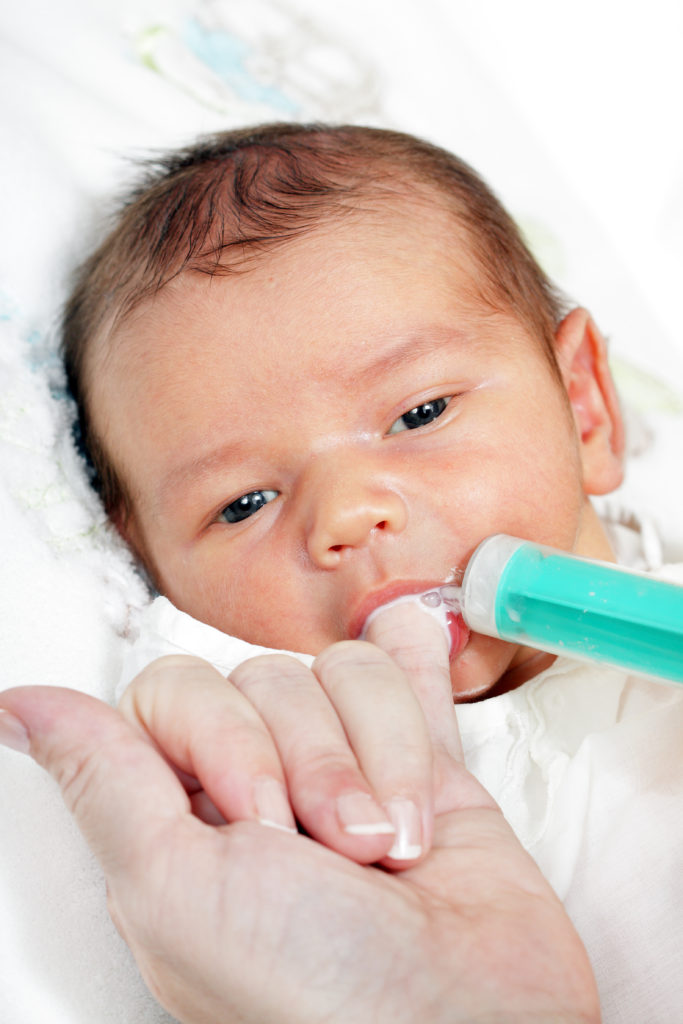
Current evidence shows that, rather than producing more milk for your baby by drinking alcohol, the effects of alcohol on your body actually mean your baby will get less of your valuable milk. Why is this?
Mennella, Pepino, and Teff [5] found that alcohol significantly reduces oxytocin levels while also increasing prolactin levels. Both hormones influence the milk ejection reflex. The lower the level of oxytocin, the longer the delay in ejection of milk. The higher the level of prolactin, the longer the delay. The combination of alcohol’s effect on the two hormones leads to a significant delay in milk ejection.
WHAT ARE THE RISKS TO MY BABY?Depending on the amount of alcohol consumed by the mother/lactating parent, and depending on when the baby is breastfed after alcohol consumption, various researchers have found the most common negative outcomes for the baby to be: [8,9,11,13,14,15,16]:
- Sleep disturbances, including shorter sleep periods, more frequent wakefulness, and less total active and REM sleep in the three-hour-period after consuming alcohol
- Increased crying
- Increased startling
- Increased arousal
- Increased REM sleep in the period from 3.
 5 hours to 24 hours after exposure to alcohol
5 hours to 24 hours after exposure to alcohol - Decreased milk intake by the baby
- Growth retardation
- Impaired immune function
- Delay of motor development
- Potential impairment of cognitive development
- Reduction in ability for abstract reasoning at school age (6-7 years)
The Academy of Breastfeeding Medicine state in Clinical Protocol #21 that consuming alcohol during lactation has several negative effects ranging from mild to severe. This is dependent on the amount of alcohol the mother/lactating parent has consumed and other factors related to how quickly their body processes alcohol [12].
As alcohol is completely water- and fat-soluble, it enters the bloodstream and human milk very easily [13]. The amount of alcohol in human milk after consumption of one standard drink is about 95% that of the amount of alcohol in the mother/lactating parent’s bloodstream.
Another review, conducted by Nonacs [14], showed that motor development of infants who were exposed to alcohol in human milk regularly was decreased or delayed.![]() The more alcohol the infants consumed through breast milk, the lower the infants scored on indices of motor development. Infants cannot metabolize alcohol as quickly as adults can; newborns can only metabolize alcohol at 25% to 50% of the rate at which adults can [14].
The more alcohol the infants consumed through breast milk, the lower the infants scored on indices of motor development. Infants cannot metabolize alcohol as quickly as adults can; newborns can only metabolize alcohol at 25% to 50% of the rate at which adults can [14].
Concerns about negative effects on the infant’s developing brain are based on animal research. Oei [15] notes that “robust animal data” indicate that “alcohol may be toxic to the developing brain, especially during periods of rapid brain development” such as occur in the first year after birth. Impairments to memory and inhibitory responses may also occur as a result of an infant’s consumption of alcohol.
Though research continues, Haastrup, Pottegård, and Damkier stated that “the possible long-term effects of alcohol in mother’s milk are unknown” (p. 171).
WHAT OTHER EFFECTS SHOULD I CONSIDER WHEN DECIDING WHETHER AND WHEN TO DRINK?Depending on how much you drink, in addition to the effects on your milk production and ejection reflex, you can expect some degree of other effects on yourself.
Alcohol produces sedative effects as well as some stimulant effects. There is some evidence that suggests that people who are currently lactating may metabolize alcohol more quickly than non-lactating people. There is clear evidence that eating food while consuming alcohol also reduces blood alcohol levels after consumption. Drinking alcohol on an empty stomach increases the effects of alcohol on prolactin and oxytocin as well as on your body [17]. You should not sleep with your baby if you have been drinking alcohol, as your natural reflexes have been impaired.
Information about bed-sharing and alcohol here:https://www.llli.org/breastfeeding-info/sleep-bedshare/ https://www.basisonline.org.uk/parents-bed/
By interfering with your milk ejection reflex, alcohol may further reduce your milk production: without this reflex, your baby cannot nurse and empty the breast effectively. When milk stays in the breasts, it tells your body to reduce production.
CAN I NURSE MY BABY AND STILL DRINK OCCASIONALLY?Several sources offer safety suggestions to consider when breastfeeding and drinking alcohol. [19]
[19]
- Be aware that newborns cannot metabolize alcohol well; if possible avoid drinking alcohol until your baby is at least 8 weeks old or older
- Breastfeed your baby immediately before drinking any alcoholic beverage, if possible, or pump and save your milk.
- Limit your alcohol intake to one (preferably) or two glasses of wine (8 ounces total) or one or two beers (see “How Is One Drink Defined” for more information on amounts of alcohol)
- Wait at least 2 hours after drinking one standard drink before breastfeeding your baby.
- Be aware that the more you drink, the longer it takes for the alcohol to clear your system.
- If your baby needs to be nursed before two hours or more is up, use your previously expressed milk to feed your baby.
- Drink juice when drinking alcohol
- Eat food when drinking alcohol–it will slow the rate at which alcohol enters your bloodstream.
- “Pump and dump” only if needed for comfort. As long as there is alcohol in your bloodstream, there will be alcohol in your milk.

A ‘standard drink’ is measured differently in different countries. It is important to understand what a ‘standard drink’ is if you choose to drink alcohol and breastfeed.
Please check with your Ministry of Health or other pertinent government resource for appropriate information in your country.
Some examples:
To determine standard drink measures in Europe, please refer to Standard Drink Measures in Europe[20].
In the UK, the NHS suggest using this unit calculator: https://alcoholchange.org.uk/alcohol-facts/interactive-tools/unit-calculator.
In the United States, it is defined by the National Institutes of Health (NIH) this way [21]:
In the United States, one “standard” drink (or one alcoholic drink equivalent) contains roughly 14 grams of pure alcohol, which is found in:
- 12 ounces of regular beer, which is usually about 5% alcohol
- 5 ounces of wine, which is typically about 12% alcohol
- 1.
 5 ounces of distilled spirits, which is about 40% alcohol
5 ounces of distilled spirits, which is about 40% alcohol
Thomas W. Hale, R.Ph. Ph.D, says this in his book Medications and Mothers’ Milk (17th ed., 2019):
“Alcohol transfers into human milk readily, with an average plasma/milk of about 1. This does not necessarily mean the dose of alcohol in milk is high, only that the levels in plasma correspond closely with those in milk. The absolute amount (dose) of alcohol transferred into milk is generally low and is a function of the maternal level. Older studies, some in animals, suggested that beer (or more likely barley) may stimulate prolactin levels. Significant amounts of alcohol are secreted into breastmilk although it is not considered harmful to the infant if the amount and duration are limited. The absolute amount of alcohol transferred into milk is generally low.
Excess levels may lead to drowsiness, deep sleep, weakness, and decreased linear growth in the infant. Maternal blood alcohol levels must attain 300 mg/dl before significant side effects are reported in the infant. Reduction of letdown is apparently dose-dependent and requires alcohol consumption of 1.5 to 1.9 gm/kg body weight. Other studies have suggested psychomotor delay in infants of moderate drinkers (2+ drinks daily). Avoid breastfeeding during and for 2 – 3 hours after drinking alcohol. Heavy drinkers should wait longer.
Reduction of letdown is apparently dose-dependent and requires alcohol consumption of 1.5 to 1.9 gm/kg body weight. Other studies have suggested psychomotor delay in infants of moderate drinkers (2+ drinks daily). Avoid breastfeeding during and for 2 – 3 hours after drinking alcohol. Heavy drinkers should wait longer.
In an interesting study of the effect of alcohol on milk ingestion by infants, the rate of milk consumption by infants during the 4 hours immediately after exposure to alcohol (0.3 g/kg) in 12 mothers was significantly less. Compensatory increases in intake were then observed during the 8 – 16 hours after exposure when mothers refrained from drinking.
Adult metabolism of alcohol is approximately 1 ounce in 3 hours, so mothers who ingest alcohol in moderate amounts can generally return to breastfeeding as soon as they feel neurologically normal. Chronic or heavy consumers of alcohol should not breastfeed.”
IMPORTANT CONSIDERATIONS-
- Your baby’s age
- A newborn has an immature liver, and will be more affected by alcohol
- Up until around three months of age, infants metabolize alcohol at about half the rate of adults
- An older baby can metabolize alcohol more quickly than a young infant but still not as well as an adult
- Your weight
- A person’s size has an impact on how quickly they metabolize alcohol
- A heavier person can metabolize alcohol more quickly than a lighter person
- Amount of alcohol
- Your baby’s age
- Know what constitutes a “standard drink”
-
- The effect of alcohol on the baby is directly related to the amount of alcohol that is consumed
- The more alcohol consumed, the longer it takes to clear the body.
 The CDC state “Alcohol from 1 drink can be detected in breast milk for about 2-3 hours, alcohol from 2 drinks can be detected for about 4-5 hours, and alcohol from 3 drinks can be detected for about 6-8 hours, and so on.”
The CDC state “Alcohol from 1 drink can be detected in breast milk for about 2-3 hours, alcohol from 2 drinks can be detected for about 4-5 hours, and alcohol from 3 drinks can be detected for about 6-8 hours, and so on.”
- Whether you will be eating
- An alcoholic drink consumed with food slows the rate of absorption of the alcohol into the bloodstream.
As alcohol leaves your bloodstream, it leaves your breastmilk. Since alcohol is not “trapped” in breastmilk (it returns to the bloodstream as your blood alcohol level declines), pumping and dumping will not remove it. Pumping and dumping, drinking a lot of water, resting, or drinking coffee will not speed up the rate of the elimination of alcohol from your body.
WHAT IF I GET DRUNK?If you are intoxicated, you should not breastfeed until you are completely sober, at which time most of the alcohol will have left your body. Drinking to the point of intoxication, or binge drinking, has been shown to impact the way infants sleep. The negative impact on sleep occurs when the infants are exposed to alcohol through milk containing alcohol at the level it would be found in human milk one hour after a mother consumed a significant amount of alcohol (0.3 grams per kilogram of their body weight).
Drinking to the point of intoxication, or binge drinking, has been shown to impact the way infants sleep. The negative impact on sleep occurs when the infants are exposed to alcohol through milk containing alcohol at the level it would be found in human milk one hour after a mother consumed a significant amount of alcohol (0.3 grams per kilogram of their body weight).
Yes. Alcohol dependence or self-medicating with alcohol by the mother/lactating parent can result in slow weight gain or failure to thrive in their baby. As noted earlier, even a small to moderate amount of alcohol negatively affects the milk ejection reflex (let-down) and reduces the baby’s milk intake. The baby can suffer significant disruption to their sleep [21] or may not suck effectively leading to decreased milk intake. The baby may even suffer from delayed motor development. If you are concerned that you or someone you know is self-medicating with alcohol excessively, contact your healthcare professional or a reputable organisation supporting people who are struggling with alcohol use.
Often, situations in which alcohol is being offered arise. Maybe you are going out with family, or on a date, or you have had an incredibly stressful week and someone suggests a beer. No matter the reason, you may have concerns about drinking and any possible effects on your baby. It is a good idea to weigh the benefits of breastfeeding against the benefits and possible risks of consuming alcohol. You might find the following suggestions helpful.
- Plan Ahead
- If you choose to drink alcohol, plan as well as you can to reduce your baby’s exposure to alcohol; If possible, store some expressed breastmilk in advance.
- Breastfeeding immediately before consuming any alcoholic beverage, then waiting to nurse again for about three hours, will help ensure that your baby gets very little alcohol from you.
- If your breasts become full while waiting for the alcohol to clear, you can hand express or pump, discarding the milk that you express.

- Alternatives
- If you plan to drink more than a moderate amount of alcohol, ensure that your baby has a responsible alternative caregiver.
- If you don’t really want to go to a family or work event talk to a trusted friend or with your local La Leche League Leader about the pros and cons of going.
- You might prefer to stick to non-alcoholic drinks.
- Have a trusted friend or an online La Leche League group on hand to message when at an event where everyone else is drinking.
- Whenever possible, ask for and take up offers of help that allow you to have a short break from mothering and parenting to focus on something you enjoy doing.
-
- Centers for Disease Control (CDC). https://www.cdc.gov/alcohol/faqs.htm#excessivealcohol
- LactMed. Retrieved 11 May 2020 from https://www.ncbi.nlm.nih.gov/books/NBK501469/
- Mennella, J. A., & Garcia-Gomez, P. L. (2001).
 Sleep disturbances after acute exposure to alcohol in mothers’ milk. Alcohol 25(3) pp. 153-158. DOI: 10.1016/s0741-8329(01)00175-6
Sleep disturbances after acute exposure to alcohol in mothers’ milk. Alcohol 25(3) pp. 153-158. DOI: 10.1016/s0741-8329(01)00175-6 - Koletzko, B., & Lehner, F. (2000). Beer and breastfeeding. Advances in Experimental Medicine and Biology 478 pp. 23-8. doi: 10.1007/0-306-46830-1_2. PMID: 11065057
- Mennella, J. A., Pepino, M. Y., & Teff, K. L. (2005). Acute alcohol consumption disrupts the hormonal milieu of lactating women. The Journal of Clinical Endocrinology & Metabolism 90(4) pp. 1979-1985. doi: 10.1210/jc.2004-1593.
- Mennella, J. A., & Pepino, M. Y. (2008). Biphasic effects of moderate drinking on prolactin during lactation. Alcoholism: Clinical and Experimental Research 32(11) pp. 1899-1908. Doi: 10.1111/j.1530-0277.2008.00774.x.
- Mennella, J. A., & Beauchamp, G. K. (1993). Beer, breast feeding, and folklore. Developmental Psychobiology, 26(8) pp. 459-466. doi: 10.1002/dev.420260804
- Haastrup, M.
 B., Pottegård, A., & Damkier, P. (2013). Alcohol and breastfeeding. Basic & Clinical Pharmacology & Toxicology 114 pp. 168-173. doi: 10.1111/bcpt.12149
B., Pottegård, A., & Damkier, P. (2013). Alcohol and breastfeeding. Basic & Clinical Pharmacology & Toxicology 114 pp. 168-173. doi: 10.1111/bcpt.12149 - Mennella, J. A. (2001). Regulation of milk intake after exposure to alcohol in mothers’ milk. Alcoholism: Clinical and Experimental Research 25(4) pp. 590-593.
- Mennella, J. A. (1998). Short-term effects of maternal alcohol consumption on lactational performance. Alcoholism: Clinical and Experimental Research 22(7) pp 1389-1392. doi: 10.1111/j.1530-0277.1998.tb03924.x
- Brown, R. A., Dakkak, H., & Seabrook, J. A. (2018). Is breast best? Examining the effects of alcohol and cannabis use during lactation. Journal of Neonatal-Perinatal Medicine, 11(4) pp. 345-356. Doi: 10.3233/NPM-17125.
- Reece-Stremtan, S., Marinelli, K. A., & The Academy of Breastfeeding Medicine. (2015). ABM Clinical Protocol #21: Guidelines for breastfeeding and substance use or substance use disorder, Revised 2015.
 Breastfeeding Medicine 10(3) pp. 135-141. doi: 10.1089/bfm.2015.9992
Breastfeeding Medicine 10(3) pp. 135-141. doi: 10.1089/bfm.2015.9992 - Anderson, P. O. (2018). Alcohol Use During Breastfeeding. Breastfeeding Medicine 13(5) pp. 315-317. DOI: 10.1089/bfm2018.0053.
- Nonacs, R. (2018). Alcohol and breastfeeding: What are the risks? Contemporary OBGYN Net December 2018 24-28.
- Oei, J-L. (2019). Risky maternal alcohol consumption during lactation decreases childhood abstract reasoning at school age. Evidence-based Nursing 22(10 p. 25. doi: 10.1136/ebnurs-2018-102999.
- Gibson, L., & Porter, M. (2018). Drinking or smoking while breastfeeding and later cognition in children. Pediatrics 142(2). doi: https://doi.org/10.1542/peds.2017-4266.
- Gibson, L., & Porter, M. (2020). Drinking or smoking while breastfeeding and later developmental health outcomes in children. BMC Res Notes 13:232. doi.org/10.1186/s13104-020-05072-8.
- Pepino, M. Y., Steinmeyer, A.
 L., & Mennella, J. A. (2007). Lactational state modifies alcohol pharmacokinetics in women. Alcoholism: Clinical and Experimental Research 31(6) pp. 909-918. doi: 10.1111/j.1530-0277.2007.00387.x.
L., & Mennella, J. A. (2007). Lactational state modifies alcohol pharmacokinetics in women. Alcoholism: Clinical and Experimental Research 31(6) pp. 909-918. doi: 10.1111/j.1530-0277.2007.00387.x. - Tay, R. Y., Wilson, J. McCormack, C., et al. (2017) Alcohol consumption by breastfeeding mothers: Frequence, correlates and infant outcomes. Drug and Alcohol Review 36 pp. 667-676. doi: 10.1111/dar.12473.
- Standard Drink Measures in Europe (2015). Published by RARHA (Reducing Alcohol Related Harm). Accessed 4 Dec 2020 from http://www.rarha.eu/Resources/Deliverables/Lists/Deliverables/Attachments/14/WP5%20Background%20paper%20Standard%20drink%20measures%20HRB.pdf
- National Institutes of Health. What Is a Standard Drink? Accessed 4 Dec 2020 from https://www.niaaa.nih.gov/alcohols-effects-health/overview-alcohol-consumption/what-standard-drink
- Drugs and Lactation Database (LactMed), Alcohol, May 11 2020 https://www.ncbi.nlm.nih.
 gov/books/NBK501469/
gov/books/NBK501469/
Accessed 27 October 2020
LLL France Article
LLL Greece Article
Reviewed and revised December 2020, with minor language changes March 2021.
Feeding when sick | Medela
If you or your baby are unwell, you may wonder if it is safe to breastfeed. The great news is that breastfeeding when you're sick is most often good for both of you. Read more about this in our article.
Share this information
Did you know that a breastfed baby is usually much less prone to illness? Although it is impossible to avoid them completely, the protective properties of breast milk help babies get sick less often 1 and recover faster than formula-fed babies.
Breast milk contains antibacterial and antiviral agents. 2 The longer you breastfeed your baby, the lower the risk of colds and flu, ear and respiratory infections, nausea and diarrhea. 1 Scientists are already exploring the use of breast milk to treat everything from conjunctivitis to cancer. 3.4
1 Scientists are already exploring the use of breast milk to treat everything from conjunctivitis to cancer. 3.4
Should a sick baby be breastfed?
Yes. Breastfeeding promotes recovery and also helps to calm the baby. Breast milk contains antibodies, white blood cells, stem cells, and protective enzymes that help fight infections and help your baby recover faster. 1,5,6 In addition, the composition of breast milk (the balance of vitamins and nutrients) is constantly adjusted to the baby's body to help him recover as soon as possible. Thus, you will spend less time on sick leave and visit the doctor less often. 7
“Breastfeeding gives the baby everything she needs when she is sick. This is his medicine, food, drink and comfort. For a baby, this is the best thing in the world,” says Sarah Beeson, a health visitor from the UK.
Surprisingly, when a child becomes ill, the composition of breast milk changes. When you come into contact with pathogens of bacterial and viral infections, your body begins to produce antibodies to fight them, which are then passed through milk to your baby. 8 When your baby is sick, your milk also spikes in immune-boosting cells (white blood cells). 5
When you come into contact with pathogens of bacterial and viral infections, your body begins to produce antibodies to fight them, which are then passed through milk to your baby. 8 When your baby is sick, your milk also spikes in immune-boosting cells (white blood cells). 5
In addition, breast milk is very easy to digest, making it ideal for babies with indigestion.
“At 12 months my daughter contracted norovirus and could only breastfeed,” recalls Maya, a mother of two in Spain. produce more milk. It was amazing. After 48 hours, I was able to meet the daily requirement for milk. It saved my baby from a drip."
It should be taken into account that sometimes during an illness it is necessary to change the habitual breastfeeding regimen. For example, with a cold, a baby may want to eat more often, but little by little, both to calm down and because of nasal congestion, which makes it difficult to apply to the chest for a long time. If your baby has a stuffy nose, an upright breastfeeding position may be more comfortable, so don't be afraid to try different breastfeeding positions.
What should I do if my baby is seriously unwell and cannot breastfeed?
Occasionally, if a child feels unwell, they may not have an appetite or the strength to feed. If your baby is not eating well, seek advice from your healthcare provider, nurse practitioner, or lactation consultant to help prevent dehydration.
You may be asked to express milk to feed your baby with a bottle, a Soft Cup*, or other suitable method that requires minimal effort from the baby. Pumping on a regular breastfeeding schedule will also help keep your milk supply stable.
You can express milk with one of our convenient breast pumps, such as the modern electronic Swing Flex** or the Harmony** manual breast pump. Rest assured, freshly expressed breast milk is just as good as breast milk, so your baby will get all the protection and support it needs.
If you have concerns about your baby's health or how much milk they are drinking, see your doctor as soon as possible.
Can I continue to breastfeed if I become ill myself?
You may not want to do this if you feel unwell, but in most cases it is best to continue breastfeeding. If you have a cold, runny nose, diarrhoea, vomiting, or mastitis, continue breastfeeding as normal with your doctor's approval. The baby is unlikely to become infected through breast milk. What's more, the antibodies in your milk will help reduce your baby's risk of contracting the same 13 virus.
If you have a cold, runny nose, diarrhoea, vomiting, or mastitis, continue breastfeeding as normal with your doctor's approval. The baby is unlikely to become infected through breast milk. What's more, the antibodies in your milk will help reduce your baby's risk of contracting the same 13 virus.
“Breastfeeding when sick is not only safe most of the time, but also beneficial. Your baby is the least at risk of catching your upset stomach or cold, as he is already in close contact with you and receives a daily dose of protective antibodies from milk, ”says Sarah Beeson.
If there is a risk of contracting a viral infection by airborne droplets, it is advisable to temporarily switch to expressing breast milk and bottle feeding.
In order not to lose the amount of milk produced when the body is still weakened by the disease, it is best to use the Swing Maxi Flex ** double breast pump, which helps to stimulate lactation, increase the amount of milk (by 18% on average) and increase its fat content (+1% ) 14 .
However, breastfeeding and pumping when sick can be very tiring. You need to take care of yourself so that you can take care of the baby. Try to drink more fluids, eat when you can, and get plenty of rest. Crawl under the covers for a few days and ask family or friends to help care for your baby if possible, so you can put all your energy into recovery.
“Don't worry about your milk supply, it will last. Most importantly, do not stop breastfeeding abruptly so that mastitis does not develop, ”adds Sarah.
Proper hygiene is very important to reduce the risk of spreading the disease. Wash your hands with soap and water before and after breastfeeding and pumping, preparing and eating food, using the toilet and changing diapers. Use a tissue when coughing and sneezing, or cover your mouth with the crook of your elbow (not your palm) if you don't have a tissue handy. Be sure to wash or sanitize your hands after coughing, sneezing, and blowing your nose.
Can I take medication while breastfeeding?
In agreement with the attending physician and compliance with the dosage, certain medications are allowed. 9.10
9.10
.
“When talking to a doctor or pharmacist for any reason, always state that you are breastfeeding,” she continues.
What about long-term treatment?
If you are on long-term treatment for diabetes, asthma, depression, or other chronic conditions, the benefits of breastfeeding may outweigh the risks. “Breastfeeding is often possible for almost any disease, with the exception of some very rare conditions,” Sarah says, “you will be very familiar with the drugs you are taking, and during pregnancy you can discuss them with your doctor or other specialist. There is guidance on the safe use of various medicines that all healthcare professionals use.” In any case, you should consult with your doctor.
“I was on high doses of epilepsy medication, but I was still able to breastfeed,” recalls Nicola, a mother from the UK. “I saw a neurologist to ensure my son was safe and to minimize the risk of a seizure. Seizures can happen due to lack of sleep, and I fed day and night, but I took good care of myself, and my husband supported me. It was a positive experience."
It was a positive experience."
What if I have to go to the hospital?
If you need to be hospitalized or urgently hospitalized, there are different ways to continue feeding your baby healthy breast milk so that you can return to normal breastfeeding after you are discharged.
“Express and freeze breast milk so that the caregiver can feed the baby. Practice at home ahead of time and be sure to let your doctors know that you are a breastfeeding mother, both before entering the hospital and while in it, ”recommends Sarah.
“If the baby is very small, you may be allowed to take him with you. Find out if the hospital has a supervising doctor or lactation consultant to contact. This specialist will support you, especially if you are in a general ward. If hospitalization is urgent, warn the doctors that you have a baby so that they take this into account.
Surgery under local or general anesthesia does not necessarily mean that breastfeeding will have to be stopped, or milk will need to be pumped and discarded. By the time you recover from surgery and can hold your baby, the amount of anesthetic in your breast milk will be minimal, so breastfeeding will be safe in most cases. 10 However, it is always best to consult your doctor or attending physician beforehand.
By the time you recover from surgery and can hold your baby, the amount of anesthetic in your breast milk will be minimal, so breastfeeding will be safe in most cases. 10 However, it is always best to consult your doctor or attending physician beforehand.
To ensure that the situation of treatment or departure does not affect the baby's diet, it is advisable to create a breast milk bank. This should be done daily by expressing one extra serving and freezing it in the handy, durable Medela Breast Milk Storage Bags. Even stored for several months and then thawed, your carefully prepared milk will still be incomparably healthier than formula.
For hygienic and easy pumping, use a breast pump with 2-Phase Expression technology for a fast, full flow of milk. For example, the ultra-comfortable Swing Flex** breastpump that adapts to the shape of your breasts and allows you to pump milk in a comfortable position, even lying back on the pillows 15 .
Don't forget to sterilize your breast pump with the Quick Clean microwave bags. Medela milk storage bags do not need to be handled as they are aseptically packaged and ready to use immediately.
Medela milk storage bags do not need to be handled as they are aseptically packaged and ready to use immediately.
Are there times when breastfeeding is not allowed?
In some cases, for the safety of the baby, breastfeeding should be stopped for a while, and instead, milk should be expressed and discarded to maintain milk production until the end of treatment. This includes radiotherapy and chemotherapy for cancer, herpes sores on the chest, and infections such as tuberculosis, measles, or blood poisoning that can be transmitted through breast milk. 11.12 Consult with a qualified professional about your condition to decide whether breastfeeding can continue in such cases.
For quality lactation support during this period, you can use the dual electronic breast pump with innovative Flex technology or rent a Symphony Clinical Breast Pump** if possible. A list of cities where you can rent a breast pump can be found on the "Rent a Medela Clinical Breast Pump" page.
Literature
1 Victora CG et al. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet . 2016;387(10017):475-490. - Victor S.J. et al., "Breastfeeding in the 21st century: epidemiology, mechanisms and long-term effects". Lancet 2016;387(10017):475-490.
2 Lönnerdal B. Bioactive proteins in breast milk. J Pediatric Child Health. 2013;49 Suppl 1:1-7. - Lönnerdahl B., "Biologically active proteins of breast milk". F Pediatrician Child Health. 2013;49 Suppl 1:1-7.
3 Australian Breastfeeding Association [Internet]. Topical treatment with breastmilk: randomized trials. [ cited 2018 Apr 4]. Available from https://www.breastfeeding.asn.au - Australian Breastfeeding Association [Internet]. "Topical treatment with breast milk: a randomized trial". [cited 4 April 2018] See article at https://www.breastfeeding.asn.au
"Topical treatment with breast milk: a randomized trial". [cited 4 April 2018] See article at https://www.breastfeeding.asn.au
4 Ho JCS et al. HAMLET–A protein-lipid complex with broad tumoricidal activity. Biochem Biophys Res Commun. 2017;482(3):454-458. - Ho J.S.S. et al., "HAMLET - a protein-lipid complex with extensive antitumor activity". Biochem Biophys Res Comm. 2017;482(3):454-458.
5 Hassiotou F et al. Maternal and infant infections stimulate a rapid leukocyte response in breastmilk. Clin Transl Immunology . 2013;2(4): e 3. - Hassiot F. et al., "Infectious diseases of the mother and child stimulate a rapid leukocyte reaction in breast milk." Clean Transl Immunology. 2013;2(4):e3.
6 Hassiotou F, Hartmann PE. At the dawn of a new discovery: the potential of breast milk stem cells . Adv Nutr . 2014;5(6):770-778. - Hassiot F, Hartmann PI, "On the threshold of a new discovery: the potential of breast milk stem cells." Adv. 2014;5(6):770-778.
Adv Nutr . 2014;5(6):770-778. - Hassiot F, Hartmann PI, "On the threshold of a new discovery: the potential of breast milk stem cells." Adv. 2014;5(6):770-778.
7 Ladomenou F et al. Protective effect of exclusive breastfeeding against infections during infancy: a prospective study. Arch Dis Child . 2010;95(12):1004-1008. - Ladomenu, F. et al., "The effect of exclusive breastfeeding on infection protection in infancy: a prospective study." Arch Dis Child. 2010;95(12):1004-1008.
8 Hanson LA. Breastfeeding provides passive and likely long-lasting active immunity. Ann Allergy Asthma Immunol . 1998;81(6):523-533. — Hanson, L.A., "Breastfeeding provides passive and likely long-term active protection against disease." Ann Allergy Asthma Immunol. 1998;81(6):523-533.
1998;81(6):523-533.
9 Hale TW, Rowe HE. Medications and Mothers' Milk 2017. 17th ed. New York, USA: Springer Publishing Company; 2017. 1095 p . — Hale T.W., Rowe H.I., Medications and Breast Milk 2017. 17th edition. New York, USA: Publishing House Springer Publishing Company ; 2017. p. 1095.
10 Reece-Stremtan S et al. ABM Clinical Protocol# 15: Analgesia and anesthesia for the breastfeeding mother, Revised 2017. Breastfeed Med . 2017;12(9):500-506. - Rees-Stromtan S. et al., AVM Clinical Protocol #15: Analgesia and Anesthesia for Nursing Mothers, 2017 edition. Brestfeed Med (Breastfeeding Medicine). 2017;12(9):500-506.
11 Lamounier JA et al. Recommendations for breastfeeding during maternal infections. J Pediatr 2004;80(5 Suppl ):181-188. - Lamunier J.A. et al., Guidelines for Breastfeeding during Maternal Infectious Diseases. J Pediatrician (Journal of Pediatrics) (Rio J). 2004;80(5 Suppl):181-188.
- Lamunier J.A. et al., Guidelines for Breastfeeding during Maternal Infectious Diseases. J Pediatrician (Journal of Pediatrics) (Rio J). 2004;80(5 Suppl):181-188.
12 Hema M et al., Management of newborn infant born to mother suffering from tuberculosis: Current recommendations & gaps in knowledge. Indian J Med Res . 2014;140(1):32-39. - Hema M. et al., "Working with the Infant Born to a Mother with Tuberculosis: Current Recommendations and Gaps." Indian W Med Res. 2014;140(1):32-39.
13 Lönnerdal B. Nutritional and physiologic significance of human milk proteins. Am JClin Nutr. 2003;77(6):1537S-1543S. Lönnerdahl B., "Biologically active proteins of breast milk". F Pediatrician Child Health. 2013;49 Suppl 1:1-7
14 Prime et al., Simultaneous Breast Expression in Breastfeeding Women Is More Efficacious Than Sequential Breast Expression, Breastfeed Med. Dec 2012; 7(6): 442–447. Prime DK and co-authors. "During the period of breastfeeding, simultaneous pumping of both breasts is more productive than sequential pumping." Brestfeed Med (Breastfeeding Medicine). 2012;7(6):442-447.
Dec 2012; 7(6): 442–447. Prime DK and co-authors. "During the period of breastfeeding, simultaneous pumping of both breasts is more productive than sequential pumping." Brestfeed Med (Breastfeeding Medicine). 2012;7(6):442-447.
15 ClinicalTrials.gov [Internet]. Bethesda MD: National Library of Medicine, USA, data on file: NCT03091985. Clinical Research.gov [Internet]. Bethesda MD: National Library of Medicine, USA, data on file: NCT03091985.
Check out the instructions, consult with a specialist
* Ru FSZ 2010/07353 dated 07/19/10
** RU No. FCZ 2010/06525 dated 17/03/2021
9000 9000 9000 9000 9000
000 Child's drinking regimen
Reviewer Kovtun Tatiana Anatolievna September 15, 2021
194022 views
Water calculator
Water calculator - calculate how much water your child needs.
The body of the child to maintain a certain amount of liquids must receive water from the outside (with food). A lot of controversy has been going on to date regarding the feeding of the baby before the introduction of complementary foods. Moreover, these disputes are conducted not only among mothers / grandmothers / nannies, but also among doctors.
Experts from the World Health Organization speak on this subject as follows: an exclusively breastfed child does not need additional fluid, since when fed on demand, the baby satisfies not only hunger, but also thirst.
http://www.who.int/mediacentre/factsheets/fs394/ru/
How and what to supplement your baby with
As we already understood, before the introduction of complementary foods, we supplement only with water. The best choice would be special bottled water for children, because. it is balanced in mineral composition and does not require boiling. We offer water to the baby: if he drinks, then he needs additional liquid, he doesn’t drink - he has enough of what he gets with milk or a mixture.
We offer water to the baby: if he drinks, then he needs additional liquid, he doesn’t drink - he has enough of what he gets with milk or a mixture.
After the introduction of complementary foods, we supplement the baby with water regularly, and when introducing fruit juices, we take them into account as an additional liquid, and not as food (that is, we do not sum them up to the daily amount of food).
Calculate the daily volume of juice
The daily volume of fruit juice depends on the age of the baby and is calculated very easily: multiply the child's age in months by 10 and get the number of milliliters of juice the baby should have per day (at 6 months - 60 ml, at 7 months - 70 ml, etc.) .
Here, drinking can already be given to the baby after feeding complementary foods or between feedings.
Hot weather fluids
Of course, the volume of liquid increases in hot weather - up to 500 ml per day. Also, an enhanced drinking regimen is required for a baby during an illness with fever, vomiting, and diarrhea.










