How long do you feed a baby breast milk
Frequently Asked Questions (FAQs) | Breastfeeding
What are the benefits of breastfeeding?
Breastfeeding is good for both infants and mothers. Breast milk is the best source of nutrition for most infants. As an infant grows, breast milk changes to meet the infant’s nutritional needs. Breastfeeding can also help protect the infant and mother against certain illnesses and diseases:
Benefits to Infants
Infants who are breastfed have a lower risk of:
- Asthma.
- Obesity.
- Type 1 diabetes.
- Severe lower respiratory disease.
- Acute otitis media (ear infections).
- Sudden infant death syndrome (SIDS).
- Gastrointestinal infections (diarrhea/vomiting).
- Necrotizing enterocolitis (NEC) for preterm infants.
Benefit to Mothers
Mothers who breastfeed their infants have a lower risk of:
- Breast cancer.
- Ovarian cancer.
- Type 2 diabetes.
- High blood pressure.
Families can visit CDC’s Infant and Toddler Nutrition website to learn more about what to expect while breastfeeding.
When should a mother avoid breastfeeding (contraindications)?
Breast milk provides the best nutrition for most infants, including premature and sick newborns. However, there are rare exceptions when breast milk or breastfeeding is not recommended. Learn more about contraindications to breastfeeding.
Only a few medications are contraindicated (not recommended) while breastfeeding. Although many medications do pass into breast milk, most have little or no effect on milk supply or on an infant’s well-being. However, health care providers should always weigh the risks and benefits when prescribing medications to breastfeeding mothers.
Learn more about safe prescription medication use while breastfeeding.
Top of Page
How is growth assessed for breastfed infants?
In the United States, the World Health Organization (WHO) Growth Standard Charts are recommended for use with both breastfed and formula-fed infants and children, from birth to 2 years of age, to monitor growth. The WHO growth charts reflect growth patterns among children who were predominantly breastfed for at least 4 months and were still breastfeeding at 12 months. The WHO growth charts establish the growth of the breastfed infant as the norm for growth and are the standards for how children should grow when provided optimal conditions. Clinicians should be aware that healthy breastfed infants typically gain weight faster than formula-fed infants in the first few months of life but then gain weight more slowly for the remainder of infancy, even after complementary foods are introduced.
The WHO growth charts reflect growth patterns among children who were predominantly breastfed for at least 4 months and were still breastfeeding at 12 months. The WHO growth charts establish the growth of the breastfed infant as the norm for growth and are the standards for how children should grow when provided optimal conditions. Clinicians should be aware that healthy breastfed infants typically gain weight faster than formula-fed infants in the first few months of life but then gain weight more slowly for the remainder of infancy, even after complementary foods are introduced.
For children older than 2 years (2 to 19 years of age) CDC and the American Academy of Pediatrics recommend that health care providers use the CDC Growth Reference Charts.
Visit the Growth Chart Training website for a set of self-directed, interactive training courses.
Source: Grummer-Strawn LM, Reinold C, Krebs NF. Use of the World Health Organization and CDC growth charts for children aged 0 to 59 months in the United States. MMWR Recomm Rep. 2010;59(RR-9):1–15.
MMWR Recomm Rep. 2010;59(RR-9):1–15.
Top of Page
How long should a mother breastfeed?
The U.S. Dietary Guidelines for Americans [PDF-30.6MB] recommend that infants be exclusively breastfed for about the first 6 months, and then continuing breastfeeding while introducing appropriate complementary foods until your child is 12 months old or older. The American Academy of Pediatrics and the World Health Organization also recommend exclusive breastfeeding for about the first 6 months, with continued breastfeeding along with introducing appropriate complementary foods for up to 2 years of age or longer.
Mothers should be encouraged to breastfeed their children for at least 1 year. The longer an infant is breastfed, the greater the protection from certain illnesses and long-term diseases. The more months or years a woman breastfeeds (combined breastfeeding of all her children), the greater the benefits to her health as well.
The American Academy of Pediatrics recommends that children be introduced to foods other than breast milk or infant formula when they are about 6 months old. To learn more about infant and toddler feeding, visit CDC’s Infant and Toddler Nutrition website.
To learn more about infant and toddler feeding, visit CDC’s Infant and Toddler Nutrition website.
Top of Page
What can happen if someone else’s breast milk is given to another child?
Very few illnesses are transmitted via breast milk. Learn more about what to do if an infant or child is mistakenly fed another woman’s expressed breast milk.
Top of Page
Are special precautions needed for handling breast milk?
CDC does not list human breast milk as a body fluid to which universal precautions apply. Occupational exposure to human breast milk has not been shown to lead to transmission of HIV or Hepatitis B infection. However, because human breast milk has been implicated in transmitting HIV from mother to infant, gloves may be worn as a precaution by health care workers who are frequently exposed to breast milk (e.g., people working in human milk banks (defined below). For additional information regarding universal precautions as they apply to breast milk in the transmission of HIV and Hepatitis B infections, visit the following resources:
Centers for Disease Control and Prevention. Perspectives in disease prevention and health promotion update: universal precautions for prevention of transmission of human immunodeficiency virus, Hepatitis B virus, and other bloodborne pathogens in health-care settings. MMWR Morb Mortal Wkly Rep. 1988;37(24):377–388.
Perspectives in disease prevention and health promotion update: universal precautions for prevention of transmission of human immunodeficiency virus, Hepatitis B virus, and other bloodborne pathogens in health-care settings. MMWR Morb Mortal Wkly Rep. 1988;37(24):377–388.
Top of Page
Where can mothers find more information about preparation and storage of breast milk?
CDC has guidelines for proper storage and preparation of breast milk to maintain the safety and quality of expressed breast milk for the health of the baby.
For more information about specific storage and preparation of breast milk questions, such as where to store breast milk at work, and what to do when the power goes out, visit CDC’s Storage and Preparation of Breast Milk Frequently Asked Questions.
Top of Page
What are human milk banks?
Human milk banks are a service established for the purpose of collecting milk from donors and processing, screening, storing, and distributing donated milk to meet the specific needs of individuals for whom human milk is prescribed by licensed health care providers. When possible, human milk banks also serve healthy infants who have been adopted or are not able to get their own mother’s milk.
When possible, human milk banks also serve healthy infants who have been adopted or are not able to get their own mother’s milk.
Milk banks accept donations directly at their deposit sites or they can arrange for safe, overnight transportation of human milk at no cost to the donor. Learn more about donating to a milk bank by visiting the Human Milk Banking Association of North America (HMBANA).
Top of Page
Is it safe for families to buy breast milk on the internet?
The American Academy of Pediatrics and the Food and Drug Administration recommend avoiding Internet-based milk sharing sites and instead recommend contacting milk banks. Research has demonstrated that some milk samples sold online have been contaminated with a range of bacteria.1
Nonprofit donor human milk banks, where processed human milk comes from screened donors, have a long safety record in North America. All member banks of the Human Milk Banking Association of North America (HMBANA) must operate under specific evidence-based guidelines that require extensive testing and processing procedures as well as self-reported health information and a health statement from both the donor’s health care provider and the infant’s health care provider. Because most of the milk from milk banks is given to hospitalized and fragile infants, milk banks may not have enough to serve healthy infants at all times. To find a human milk bank, contact HMBANA.
Because most of the milk from milk banks is given to hospitalized and fragile infants, milk banks may not have enough to serve healthy infants at all times. To find a human milk bank, contact HMBANA.
1Keim, SA, Hogan, JS, McNamara, KA, et al. Microbial contamination of human milk purchased via the internet. Pediatrics. 2013;132(5).
Top of Page
What legal rights do breastfeeding mothers have?
Breastfeeding Laws
- All 50 states, the District of Columbia, Puerto Rico and the Virgin Islands have laws that specifically allow women to breastfeed in any public or private location. Visit the National Conference of State Legislatures to learn more about federal and state laws that protect and support breastfeeding.
Workplace Laws
- The “Break Time for Nursing Mothers Provision” of the Patient Protection and Affordable Care Act (ACA) requires employers to support breastfeeding mothers to express breast milk for 1 year after each child’s birth by providing mothers with reasonable break time and a private, non-bathroom space to express their breast milk.
 Visit the United States Department of Labor to learn more.
Visit the United States Department of Labor to learn more.
Travel Laws
- Air travelers are permitted by the Transportation Security Administration (TSA) to bring breast milk, formula, and juice in excess of 3.4 ounces in their carry-on baggage and it does not need to fit within a quart size bag. Ice packs, freezer packs, and other accessories needed to keep the liquid cool are also allowed in carry-on bags. All liquids and partially frozen accessories are subject to being screened by X-ray. TSA is required by the Bottles and Breastfeeding Equipment Screening Act (BABES act) to provide ongoing training to ensure TSA staff receive consistent training related to traveling with breast milk, formula, and infant feeding equipment. Visit the TSA to learn more about traveling with breast milk, formula, and juice. For tips on travel and breastfeeding, visit Travel Recommendations for the Nursing Mother.
Visit the Federal Policies, Programs, & Initiatives website to learn more about laws related to breastfeeding protections.
Top of Page
How can a mother continue to provide breast milk to her infant after returning to work or school?
Being prepared for returning to work or school can help a mother ease the transition and continue to breastfeed after her maternity leave is over. The Office on Women’s Health has information for making this transition easier.
When a mother is away from her infant, she can pump or hand express her breast milk so that her infant can drink breast milk from a bottle. Mothers can visit CDC’s Infant and Toddler Nutrition website to learn more about pumping breast milk.
Mothers who are expressing their breast milk should visit the CDC’s Proper Storage and Preparation of Breast Milk website to learn how to prepare and store breast milk safely for her infant.
The Patient Protection and Affordable Care Act (ACA) requires employers to support breastfeeding mothers to express breast milk for 1 year after each child’s birth by providing mothers with reasonable break time and a private, non-bathroom space to express their breast milk. For more information about the types of employees and employers to which the requirements apply, refer to the United States Department of Labor’s Frequently Asked Questions.
For more information about the types of employees and employers to which the requirements apply, refer to the United States Department of Labor’s Frequently Asked Questions.
Top of Page
Where can mothers find breastfeeding support and additional Information about breastfeeding?
Help mothers find lactation support through the following resources:
- International Lactation Consultant Association (IBCLCs)
- United States Lactation Consultant Association (IBCLCs)
- Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) clinics
- La Leche League
Help mothers find resources about breastfeeding by directing them to the following websites:
- CDC— Infant and Toddler Nutrition
- Office on Women’s Health—Breastfeeding
- American Academy of Pediatrics—Healthy Children
- United States Breastfeeding Committee—State Coalitions Directory
- US Department of Agriculture—WIC Breastfeeding Support
Top of Page
Does breastfeeding during a child’s vaccine injections help with pain management?
Parents who are breastfeeding should be encouraged to breastfeed children age 2 years or younger before, during, and after their child’s vaccination. Several aspects of breastfeeding are thought to decrease pain by multiple mechanisms: being held by the parent, feeling skin-to-skin contact, suckling, being distracted, and ingesting breast milk. Potential adverse events such as gagging or spitting up have not been reported. Alternatives to breastfeeding include bottle-feeding with expressed breast milk or formula throughout the child’s procedure, which simulates aspects of breastfeeding.
Several aspects of breastfeeding are thought to decrease pain by multiple mechanisms: being held by the parent, feeling skin-to-skin contact, suckling, being distracted, and ingesting breast milk. Potential adverse events such as gagging or spitting up have not been reported. Alternatives to breastfeeding include bottle-feeding with expressed breast milk or formula throughout the child’s procedure, which simulates aspects of breastfeeding.
Top of Page
Does breastfeeding after a child’s rotavirus vaccine impact the vaccine’s efficacy?
There is not sufficient evidence to suggest that breastfeeding can have a negative effect on rotavirus vaccine efficacy. A previous study found that human milk from women who live in areas with endemic rotavirus contains antibodies that can neutralize live rotavirus vaccine virus. However, in licensing trials, the effectiveness of rotavirus vaccine in breastfed infants was comparable to that in non-breastfed infants.
CDC does not recommend restricting or discontinuing breastfeeding before or after a child receives the rotavirus vaccine. Breastfed infants should be vaccinated according to the same schedule as non-breastfed infants.
Breastfed infants should be vaccinated according to the same schedule as non-breastfed infants.
Learn More about prevention of Rotavirus Gastroenteritis among infants and children.
Top of Page
Breastfeeding and Returning to Your Workplace | Nutrition
Many parents have questions about expressing breast milk when returning to their workplace after having a baby. Whether returning to work from maternity leave or starting a new job after having your baby, you may be working from home, at a work site, or some combination of the two. Below you will find common questions with information and resources to help you prepare to return to your workplace. The Office on Women’s Healthexternal icon provides additional information.
What are my rights as a breastfeeding employee?
The federal Break Time for Nursing Mothers Provisionexternal icon of the Patient Protection and Affordable Care Act requires employers to support breastfeeding employees by providing:
- A reasonable break time to express breast milk for 1 year after your child’s birth.

- A private, non-bathroom space to express breast milk.
This law applies to most hourly employees and some salaried employees (nonexempt workers) who are covered by the Fair Labor Standards Actexternal icon. Most states also have laws that protect breastfeeding employees.
For breastfeeding people who work in settings with higher risk of potential exposure to COVID-19, such as health care settings, they should wear a mask while breastfeeding or expressing milk in the workplace. Learn more at Care for Breastfeeding People.
How do I talk with my employer about my needs as I return to work?
If you work outside your home, talk with your employer before you return to your workplace about expressing breast milk during work hours. Having this conversation early will help make sure a plan is in place.
Talk with your employer about:
- Where there is a private, non-bathroom space to express breast milk.
- Where breast milk can be stored (eg, refrigerator, insulated cooler).

- Where pump parts can be cleaned.
- What times are best for you during your work schedule for expressing milk.
The timing and length of breaks needed to express milk and clean breast pump parts may change from day to day and over time. It may be helpful to discuss this with your employer since they may not be familiar with the process of expressing milk or cleaning pump equipment.
Some bras and pumps are designed to be used hands-free! This allows you to collect milk for your baby while doing other things.
How should I clean my breast pump kit parts at my workplace?
For best practices on cleaning pump kit parts, visit CDC’s FAQ page on cleaning breast milk pump parts.
What if I don’t have time to wash pump parts or have access to a sink and water to wash parts?
Careful cleaning of your breast pump parts after every use is important to prevent germs from contaminating the milk you feed your baby. Cleaning breast pump parts at work may require creative solutions depending on your workplace. Here are some ways that you might handle these challenges:
Here are some ways that you might handle these challenges:
- Bring multiple breast pump kits to your workplace so that a clean kit can be used for each pumping session. Take used parts home after work and wash them all at once.
- If you have access to a microwave, rinse parts and then use steam bags made for cleaning breast pump parts. Some pump parts should not be steamed in the microwave, so be sure to check the manufacturer’s instructions.
- Learn how to hand express directly into milk collection containers.
Can I store my pump parts in the refrigerator between pump sessions while at my workplace?
The CDC and most breast pump manufacturers recommend cleaning pump parts after every use to help protect babies from germs.
More information about storing pump parts in the refrigerator between pumping sessions can be found on CDC’s FAQ page on breast pump cleaning.
Where can I store breast milk at my workplace?
- In the refrigerator: Expressed breast milk is a food and may be stored alongside other foods in any refrigerator that is appropriate for food storage.

- In an insulated cooler: You can store and carry freshly expressed milk in an insulated cooler bag with frozen ice packs for up to 24 hours. Once you get home use the milk right away, store it in the refrigerator, or freeze it.
Always label breast milk containers with your name and the date you expressed the milk. You can also label your cooler with your name and contact information.
How can I pump and store breast milk if my work requires travel?
For detailed information about travel, visit Travel Recommendations for Nursing Families
What else might help me continue breastfeeding after returning to work?
- Practice using your pump or hand expressing breast milk before returning to work so you are comfortable with the process.
- Build a supply of frozen breast milk before returning to work.
- Think about how much breast milk you will need to leave at home or at childcare for your baby before your first day back at work.

- Think about how often you will need to pump or express breast milk while at work to have enough for your baby while you are apart.
- Once breastfeeding is going well, practice bottle feeding your breast milk so your baby will be used to a bottle while you are away at work. If your baby is having trouble taking a bottle at first, try having another adult feed your baby with the bottle. You can also try different types of bottles and nipples.
Top of Page
- Break times and spaces to express milkexternal icon
- Helpful tips for pumping breast milkexternal icon
- General breast milk storage
- Breast milk storage at work
- FAQs on breast pump cleaning
- Types of employers that provide breastfeeding support in the workplaceexternal icon
- Traveling with Children | Transportation Security Administration (tsa.gov)external icon
Breastfeeding in the first month: what to expect
Not sure how to establish lactation and increase milk production? If you need help, support, or just want to know what to expect, read our first month breastfeeding advice
Share this information
The first weeks of breastfeeding are a very stressful period. If at times you feel like you can't handle it, know that you are not alone. Feeding your baby all day long is completely natural and helps produce breast milk, but can be quite tiring at times. Be patient, think about yourself and remember: after the first month, when milk production stabilizes, it will become easier.
If at times you feel like you can't handle it, know that you are not alone. Feeding your baby all day long is completely natural and helps produce breast milk, but can be quite tiring at times. Be patient, think about yourself and remember: after the first month, when milk production stabilizes, it will become easier.
How often should a baby be breastfed?
Babies are born with a small stomach that grows rapidly with increasing milk production: in the first week it is no larger than an apricot, and after two weeks it is already the size of a large chicken egg. 1.2 Let the child eat as much as he wants and when he wants. This will help him quickly regain the weight lost after birth and grow and develop further.
“Be prepared to feed every two to three hours throughout the day. At night, the intervals between feedings can be longer: three to four or even five hours, says Cathy Garbin, a recognized international expert on breastfeeding. Some eat quickly and are satiated in 15 minutes, while others take an entire hour to feed. Do not compare your breastfeeding regimen with that of other mothers - it is very likely that there will be nothing in common between them.
Do not compare your breastfeeding regimen with that of other mothers - it is very likely that there will be nothing in common between them.
At each feed, give your baby a full meal from one breast and then offer a second one, but don't worry if the baby doesn't take it. When the baby is full, he lets go of his chest and at the same time looks relaxed and satisfied - so much so that he can immediately fall asleep. The next time you feed, start on the other breast. You can monitor the order of the mammary glands during feeding using a special application.
Why does the child always ask for a breast?
The first month is usually the hardest time to breastfeed. But do not think that because the baby is constantly hungry and asks for a breast almost every 45 minutes, then you do not have enough milk.
In the first month, the baby needs to eat frequently to start and stimulate the mother's milk production. It lays the foundation for a stable milk supply in the future. 3
3
In addition, we must not forget that the child needs almost constant contact with the mother. The bright light and noise of the surrounding world at first frighten the baby, and only by clinging to his mother, he can calm down.
Sarah, mother of three from the UK, confirms: “Crying is not always a sign of hunger. Sometimes my kids just wanted me to be around and begged for breasts to calm them down. Use a sling. Place the cradle next to the bed. Don't look at the clock. Take advantage of every opportunity to relax. Forget about cleaning. Let those around you take care of you. And not three days, but six weeks at least! Hug your baby, enjoy the comfort - and trust your body."
Do I need to feed my baby on a schedule?
Your baby is still too young for a strict daily routine, so
forget about breastfeeding schedules and focus on his needs.
“Volumes have been written about how to feed a baby on a schedule, but babies don't read or understand books,” Cathy says. - All children are different. Some people can eat on a schedule, but most can't. Most often, over time, the child develops his own schedule.
- All children are different. Some people can eat on a schedule, but most can't. Most often, over time, the child develops his own schedule.
Some mothers report that their babies are fine with scheduled feedings, but they are probably just the few babies who would eat every four hours anyway. Adults rarely eat and drink the same foods at the same time of day - so why do we expect this from toddlers?
Offer your baby the breast at the first sign of hunger. Crying is already the last stage, so be attentive to early signs: the baby licks his lips, opens his mouth, sucks his fist, turns his head with his mouth open - looking for the breast. 4
What is a "milk flush"?
At the beginning of each feed, a hungry baby actively sucks on the nipple,
thereby stimulating the milk flow reflex - the movement of milk through the milk ducts. 5
“Nipple stimulation triggers the release of the hormone oxytocin,” explains Cathy. “Oxytocin is distributed throughout the body and causes the muscles around the milk-producing glands to contract and the milk ducts to dilate. This stimulates the flow of milk.
This stimulates the flow of milk.
If the flushing reflex fails, milk will not come out. This is a hormonal response, and under stress it may not work at all or work poorly. Therefore, it is so important that you feel comfortable and calm when feeding.
“Studies show that each mother has a different rhythm of hot flashes during one feed,” Kathy continues, “Oxytocin is a short-acting hormone, it breaks down in just 30-40 seconds after formation. Milk begins to flow, the baby eats, the effect of oxytocin ends, but then a new rush of milk occurs, the baby continues to suckle the breast, and this process is repeated cyclically. That is why, during feeding, the child periodically stops and rests - this is how nature intended.
The flow of milk may be accompanied by a strong sensation of movement or tingling in the chest, although 21% of mothers, according to surveys, do not feel anything at all. 5 Cathy explains: “Many women only feel the first rush of milk.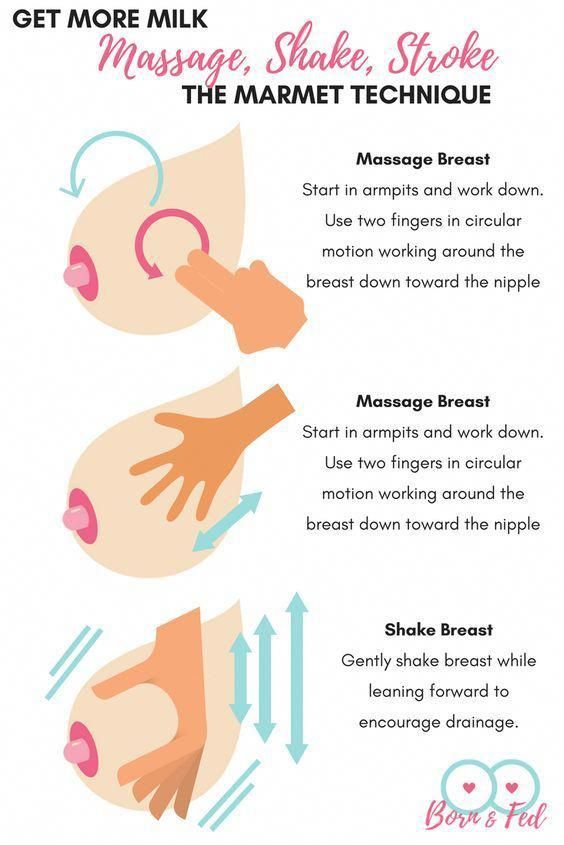 If you do not feel hot flashes, do not worry: since the child eats normally, most likely, you simply do not understand that they are.
If you do not feel hot flashes, do not worry: since the child eats normally, most likely, you simply do not understand that they are.
How do you know if a baby is getting enough milk?
Since it is impossible to track how much milk a baby eats while breastfeeding, mothers sometimes worry that the baby is malnourished. Trust your child and your body.
After a rush of milk, the baby usually begins to suckle more slowly. Some mothers clearly hear how the baby swallows, others do not notice it. But one way or another, the child himself will show when he is full - just watch carefully. Many babies make two or three approaches to the breast at one feeding. 6
“When a child has had enough, it is noticeable almost immediately: a kind of “milk intoxication” sets in. The baby is relaxed and makes it clear with his whole body that he is completely full, says Katie, “Diapers are another great way to assess whether the baby is getting enough milk. During this period, a breastfed baby should have at least five wet diapers a day and at least two portions of soft yellow stool, and often more. ”
”
From one month until weaning at six months of age, a baby's stool (if exclusively breastfed) should look the same every day: yellow, grainy, loose, and watery.
When is the child's birth weight restored?
Most newborns lose weight in the first few days of life. This is normal and should not be cause for concern. As a rule, weight is reduced by 5-7%, although some may lose up to 10%. One way or another, by 10–14 days, almost all newborns regain their birth weight. In the first three to four months, the minimum expected weight gain is an average of 150 grams per week. But one week the child may gain weight faster, and the next slower, so it is necessary that the attending physician monitor the health and growth of the baby constantly. 7.8
At the slightest doubt or signs of dehydration, such as
dark urine, no stool for more than 24 hours, retraction of the fontanel (soft spot on the head), yellowing of the skin, drowsiness, lethargy, lack of appetite (ability to four to six hours without feeding), you should immediately consult a doctor. 7
7
What is "cluster feeding"?
When a baby asks to breastfeed very often for several hours, this is called cluster feeding. 6 The peak often occurs in the evening between 18:00 and 22:00, just when many babies are especially restless and need close contact with their mother. Most often, mothers complain about this in the period from two to nine weeks after childbirth. This is perfectly normal and common behavior as long as the baby is otherwise healthy, eating well, gaining weight normally, and appears content throughout the day. 9
Cluster feeding can be caused by a sharp jump in the development of the body - during this period the baby especially needs love, comfort and a sense of security. The growing brain of a child is so excited that it can be difficult for him to turn off, or it just scares the baby. 9 If a child is overworked, it is often difficult for him or her to calm down on his own, and adult help is needed. And breastfeeding is the best way to calm the baby, because breast milk is not only food, but also pain reliever and a source of happiness hormones. 10
And breastfeeding is the best way to calm the baby, because breast milk is not only food, but also pain reliever and a source of happiness hormones. 10
“Nobody told me about cluster feeding, so for the first 10 days I just went crazy with worry - I was sure that my milk was not enough for the baby,” recalls Camille, a mother from Australia, “It was a very difficult period . I was advised to pump and supplement until I finally contacted the Australian Breastfeeding Association. There they explained to me what was happening: it turned out that it was not about milk at all.
Remember, this is temporary. Try to prepare dinner for yourself in the afternoon, when the baby is fast asleep, so that in the evening, when he begins to often breastfeed, you have the opportunity to quickly warm up the food and have a snack. If you are not alone, arrange to carry and rock the baby in turns so that you have the opportunity to rest. If you have no one to turn to for help and you feel that your strength is leaving you, put the baby in the crib and rest for a few minutes, and then pick it up again.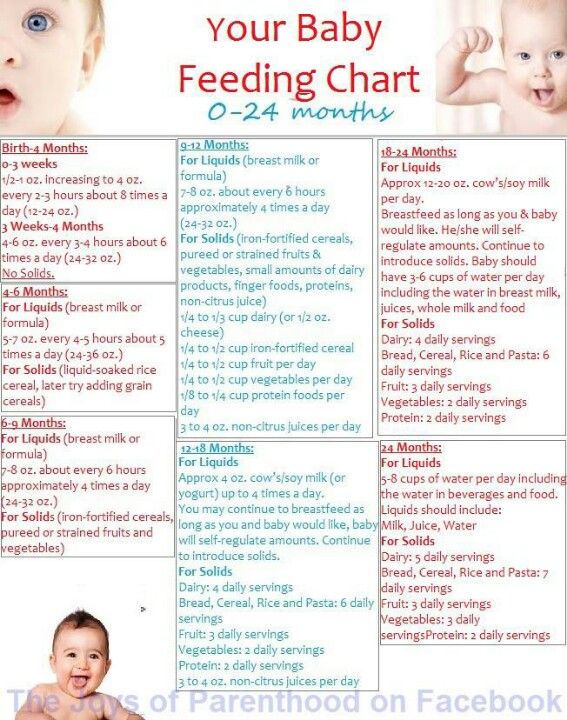
Ask your partner, family and friends to help you with household chores, cooking and caring for older children if you have any. If possible, hire an au pair. Get as much rest as possible, eat well and drink plenty of water.
“My daughter slept a lot during the day, but from 23:00 to 5:00 the cluster feeding period began, which was very tiring,” recalls Jenal, a mother from the USA, “My husband tried his best to make life easier for me - washed, cleaned, cooked, changed diapers, let me sleep at every opportunity and never tired of assuring me that we were doing well.
If you are concerned about the frequency of breastfeeding, it is worth contacting a specialist. “Check with a lactation consultant or doctor to see if this is indicative of any problems,” recommends Cathy. “Resist the temptation to supplement your baby with formula (unless recommended by your doctor) until you find the cause. It may not be a matter of limited milk production at all - it may be that the child is inefficiently sucking it.
When will breastfeeding become easier?
This early stage is very special and does not last long. Although sometimes it seems that there will be no end to it, rest assured: it will get easier soon! By the end of the first month, breast milk production will stabilize, and the baby will become stronger and learn to suckle better. 2.3 Any problems with latch on by this time will most likely be resolved and the body will be able to produce milk more efficiently so inflammation and leakage of milk will begin to subside.
“The first four to six weeks are the hardest, but then things start to get better,” Cathy assures. It just needs to be experienced!”
The longer breastfeeding continues, the more benefits it brings, from saving on formula and improving sleep quality 11–13 to boosting your baby's immune system 14 and reducing your risk of certain cancers. 15
“When you feel like you're pushing yourself, try to go from feed to feed and day to day,” says Hannah, a UK mom. “I was sure I wouldn’t make it to eight weeks. And now I have been breastfeeding for almost 17 weeks, and I dare say it is very easy.”
“I was sure I wouldn’t make it to eight weeks. And now I have been breastfeeding for almost 17 weeks, and I dare say it is very easy.”
Read the resource Breastfeeding Beyond the First Month: What to Expect
Literature
1 Naveed M et al. An autopsy study of relationship between perinatal stomach capacity and birth weight. Indian J Gastroenterol .1992;11(4):156-158. - Navid M. et al., Association between prenatal gastric volume and birth weight. Autopsy. Indian J Gastroenterol. 1992;11(4):156-158.
2 Neville MC et al. Studies in human lactation: milk volumes in lactating women during the onset of lactation and full lactation .Am J Clinl Nutr . 1988;48(6):1375-1386. at the beginning and at the peak of lactation." Am F Clean Nutr. 1988;48(6):1375-1386.
3 Kent JC et al. Principles for maintaining or increasing breast milk production. J Obstet , Gynecol , & Neonatal Nurs . 2012;41(1):114-121. - Kent J.S. et al., "Principles for Maintaining and Increasing Milk Production". J Obstet Ginecol Neoneutal Nurs. 2012;41(1):114-121.
Principles for maintaining or increasing breast milk production. J Obstet , Gynecol , & Neonatal Nurs . 2012;41(1):114-121. - Kent J.S. et al., "Principles for Maintaining and Increasing Milk Production". J Obstet Ginecol Neoneutal Nurs. 2012;41(1):114-121.
4 Australian Breastfeeding Feeding cues ; 2017 Sep [ cited 2018 Feb ]. - Australian Breastfeeding Association [Internet], Feed Ready Signals; September 2017 [cited February 2018]
5 Kent JC et al. Response of breasts to different stimulation patterns of an electric breast pump. J Human Lact . 2003;19(2):179-186. - Kent J.S. et al., Breast Response to Different Types of Electric Breast Pump Stimulation. J Human Lact (Journal of the International Association of Lactation Consultants). 2003;19(2):179-186.
J Human Lact (Journal of the International Association of Lactation Consultants). 2003;19(2):179-186.
6) Kent JC et al . Volume and frequency of breastfeedings and fat content of breast milk throughout the day. Pediatrics. 2006;117(3): e 387-395. — Kent J.S. et al., "Amount and frequency of breastfeeding and fat content of breast milk during the day." Pediatrix (Pediatrics). 2006;117(3):e387-95.
7 Lawrence RA, Lawrence RM. Breastfeeding: A guide for the medical profession. 7th ed. Maryland Heights MO, USA: Elsevier Mosby; 2010. 1128 p . - Lawrence R.A., Lawrence R.M., "Breastfeeding: A guide for healthcare professionals." Seventh edition. Publisher Maryland Heights , Missouri, USA: Elsevier Mosby; 2010. Pp. 1128.
8 World Health Organization. [Internet]. Child growth standards; 2018 [cited 2018 Feb] - World Health Organization. [Internet]. Child Growth Standards 2018 [cited February 2018].
[Internet]. Child growth standards; 2018 [cited 2018 Feb] - World Health Organization. [Internet]. Child Growth Standards 2018 [cited February 2018].
9 Australian Breastfeeding Association . [ Internet ]. Cluster feeding and fussing babies ; Dec 2017 [ cited 2018 Feb ] - Australian Breastfeeding Association [Internet], Cluster Feeding and Screaming Babies; December 2017 [cited February 2018].
10 Moberg KU, Prime DK. Oxytocin effects in mothers and infants during breastfeeding. Infant . 2013;9(6):201-206.- Moberg K, Prime DK, "Oxytocin effects on mother and child during breastfeeding". Infant. 2013;9(6):201-206.
11 U.S. Department of Health & Human Services [Internet]. Surgeon General Breastfeeding factsheet; 2011 Jan 20 [cited 2017 Feb] - Department of Health and Human Services [Internet], "Breastfeeding Facts from the Chief Medical Officer", Jan 20, 2011 [cited Feb 2017]
12 Kendall-Tackett K et al. The effect of feeding method on sleep duration, maternal well-being, and postpartum depression. clinical lactation. 2011;1;2(2):22-26. - Kendall-Tuckett, K. et al., "Influence of feeding pattern on sleep duration, maternal well-being and the development of postpartum depression." Clinical Lactation. 2011;2(2):22-26.
The effect of feeding method on sleep duration, maternal well-being, and postpartum depression. clinical lactation. 2011;1;2(2):22-26. - Kendall-Tuckett, K. et al., "Influence of feeding pattern on sleep duration, maternal well-being and the development of postpartum depression." Clinical Lactation. 2011;2(2):22-26.
13 Brown A, Harries V. Infant sleep and night feeding patterns during later infancy: Association with breastfeeding frequency, daytime complementary food intake, and infant weight. Breast Med . 2015;10(5):246-252. - Brown A., Harris W., "Night feedings and infant sleep in the first year of life and their association with feeding frequency, daytime supplementation, and infant weight." Brest Med (Breastfeeding Medicine). 2015;10(5):246-252.
14 Hassiotou F et al. Maternal and infant infections stimulate a rapid leukocyte response in breastmilk. Clin Transl immunology. 2013;2(4). - Hassiot F. et al., "Infectious diseases of the mother and child stimulate a rapid leukocyte reaction in breast milk." Clean Transl Immunology. 2013;2(4):e3.
Clin Transl immunology. 2013;2(4). - Hassiot F. et al., "Infectious diseases of the mother and child stimulate a rapid leukocyte reaction in breast milk." Clean Transl Immunology. 2013;2(4):e3.
15 Li DP et al. Breastfeeding and ovarian cancer risk: a systematic review and meta-analysis of 40 epidemiological studies. Asian Pac J Cancer Prev . 2014;15(12):4829-4837. - Lee D.P. et al., Breastfeeding and ovarian cancer risk: a systematic review and meta-analysis of 40 epidemiological studies. Asia Pas J Cancer Prev. 2014;15(12):4829-4837.
Breastfeeding after 1 month: what to expect
Do you know when breast milk production stabilizes? And how does the frequency and duration of feedings change as the baby grows? You will find answers to these questions in our recommendations for breastfeeding after the first month.
Share this information
Congratulations: You made it through the first month of breastfeeding. Your breast milk has reached full maturity 1 , its production stabilizes and it leaks almost or not at all from the chest. Don't worry, it's not getting less milk, it's just that your breasts are better able to produce and store it now. 2 At the age of six weeks, your baby will begin to delight you with his charming toothless smiles, and by two months you will already have 500-600 feedings behind you. With a favorable development of events, problems with latch on by this point will already be resolved, and you can simply enjoy the convenience and benefits of breastfeeding.
Your breast milk has reached full maturity 1 , its production stabilizes and it leaks almost or not at all from the chest. Don't worry, it's not getting less milk, it's just that your breasts are better able to produce and store it now. 2 At the age of six weeks, your baby will begin to delight you with his charming toothless smiles, and by two months you will already have 500-600 feedings behind you. With a favorable development of events, problems with latch on by this point will already be resolved, and you can simply enjoy the convenience and benefits of breastfeeding.
When does breastfeeding decrease?
The "normal" feeding frequency for babies aged one to six months varies considerably, with some needing four times a day, others asking to be breastfed 13 times a day. 3
“From the age of one month, the amount of milk a baby consumes per feed increases, so that he can go without food for longer,” explains Cathy Garbin, a recognized international expert on breastfeeding, “A baby’s stomach grows, so he eat more at one time. In addition, mature milk allows him to stay full longer.”
In addition, mature milk allows him to stay full longer.”
Feeding can last from 12 minutes to one hour -
the habits of babies vary so much! 3 But if the child is gaining weight and falls within this range, there is no cause for concern.
What is most surprising, no matter how often the baby eats, he consumes approximately the same amount of milk per day - both at one month and at six, when it is time to start complementary foods with solid food. 4
“However, sometimes the baby eats more and sometimes less, especially when he is unwell. It’s better to just listen to his needs,” Katie explains.
Is breastmilk sufficient for the first six months?
Yes. Breast milk contains everything a baby needs for the first 90,035 six months of life—exclusively breastfed babies don't even need to drink more water! 5 Until about six months of age, a child's digestive system is simply not adapted to the digestion of solid food, and he will be able to drink cow's milk only after a year.
In addition, breastfeeding during this period prepares the child for further development. It strengthens the muscles of the mouth, develops the jaw and helps straighten the teeth 6.7 . All this will come in handy when the baby begins to eat and talk. And because what you eat and drink affects how your breast milk tastes, your baby discovers new tastes even before he starts eating solid foods. 8
In addition, when your baby is sick, your body produces breast milk that is
rich in antibodies that help fight infection. 9 In other words, milk continues to protect the baby for many months as he grows and becomes more active.
Breastfeeding is also very comfortable once you get used to it. Claudia, a mother of two from the UK, notes: “No need to sterilize a mountain of bottles, prepare formula, carry it all with you, warm it up - in general, breastfeeding turned out to be very convenient, especially when my babies grew up and we began to leave the house more often. ".
".
At what age does a breastfed baby start sleeping through the night?
Waking up at night is normal for babies. Most babies between the ages of one and six months consume a fifth of their daily milk requirement at night, so nighttime feedings should not be neglected if you want your baby to get the required amount of calories. 3
"It really depends on what you mean by 'sleep through the night,'" Cathy says. "And it's better than waking up every two hours anyway! I have met infants who, starting at six weeks old, fell asleep at 19:00 and woke up at 7:00, but most continue to wake up frequently at night after this age. All children are different."
In Wales, a study of more than 700 infants showed that almost 80% of children aged 6 to 12 months wake up at least once a night, and 25% of them wake up three times or more. And it did not depend on what type of feeding the child is on - breastfeeding or artificial. 10
And if nighttime awakenings are unavoidable anyway, breastfeeding is at least comfortable! Maina, a mother of two from Australia, agrees: “You can even take a nap while feeding in the middle of the night - both the body and the baby do their job on autopilot. No need to plan, measure, sterilize anything - ready-made food at the right temperature is right in your chest. I think it's ideal."
No need to plan, measure, sterilize anything - ready-made food at the right temperature is right in your chest. I think it's ideal."
My child wakes up more often. Perhaps he is hungry?
Around four months of age, a baby's sleep pattern changes as he, like an adult, develops deep and light sleep phases. Because of this, he may wake up more often at night. “At four months, sleep is more of a problem than feeding,” Cathy admits. “It can be exhausting, but try to adapt and be patient.”
Some people call this " a four-month sleep regression ", but "progress" is more appropriate here. From the outside it may look like a step back, but in fact the child is approaching an important stage of development. He learns quickly, begins to become aware of the world around him, his perception is sharpened and, perhaps, there is anxiety about being separated from his mother. Crying when waking up and being able to eat milk cuddled up to mommy’s chest is a way for a baby to calm down. 11–13
11–13
Resist the urge to “supplement” your baby with formula or start solid foods early
in an attempt to improve his sleep. Breast milk contains
hormones that make you sleepy and help you both relax
. Studies show that breastfeeding mothers actually sleep longer at night than mothers of formula-fed or mixed-fed babies
. 14
How does teething affect breastfeeding?
Teething usually begins around four months of age. When a baby has gum pain, he becomes restless, throws his chest and cries. All this, of course, is unpleasant.
However, breastfeeding can be an excellent sedative.
Studies have shown that babies who are breastfed
during the vaccination period cry less and forget pain more quickly. 15 Breastfeeding during teething can have the same calming effect.
An unpleasant side effect may be the child's attempts to try out his new teeth on the mother's breast. “Sometimes children flirt and bite their mother’s nipples. This can be felt in advance by how the behavior of the child changes when feeding: before biting, he removes his tongue, explains Cathy, “Usually this is not a problem and only happens a couple of times. It is enough to stop feeding, affectionately say that biting is not good, and the baby will soon leave this fun.
This can be felt in advance by how the behavior of the child changes when feeding: before biting, he removes his tongue, explains Cathy, “Usually this is not a problem and only happens a couple of times. It is enough to stop feeding, affectionately say that biting is not good, and the baby will soon leave this fun.
How to continue feeding if you have to be separated from the baby?
It happens that during the first six months, when the baby is still fully breastfed, the mother needs to be away for several hours - or even longer if she has to go to work or go away on business for a couple of days.
But this does not mean that you should stop breastfeeding. You can still feed your baby healthy breast milk - just express it and have someone give it to your baby when you're away. Here's Katie's advice:
“Start expressing milk a couple of days in advance, in small batches, 40-60 ml at a time. So you will have the necessary supply for the time of your absence, but at the same time the amount of milk produced will remain the same.
If you have to return to work, check with your employer about your daily schedule. Many mothers breastfeed their babies in the morning, evening and night, and pump milk at lunchtime to relieve discomfort and create a reserve for the next day.
This usually turns out to be much easier than one might think, and today many companies are well placed to do this, notes Cathy. “Breast pumps make it easy to solve this problem.”
Natalie, mother from the USA, shares her experience: “I feed Dylan as soon as he wakes up, and sometimes again before leaving for work, in order to maintain milk production and not lose contact with the child. At work, I pump twice the next day (in my absence, he eats two bottles of breast milk), and after work I rush home for the evening feed. I don't pump on the weekends - we resume regular breastfeeding."
Can breastfeeding continue after the introduction of solid foods?
When your baby begins to show interest in food and can sit up on his own - usually around six months of age - it's time to start solid foods. However, it is not necessary to stop breastfeeding, Cathy explains: “A baby’s iron stores during pregnancy are depleted by six months, so he needs additional sources of this element.
However, it is not necessary to stop breastfeeding, Cathy explains: “A baby’s iron stores during pregnancy are depleted by six months, so he needs additional sources of this element.
Start complementary foods with solid foods, but remember that breast milk remains a more important source of calories and nutrients until the baby is eight to nine months old. By this time, he will be eating much more solid food, but he will still need to breastfeed four to five times a day. By 12 months, the frequency of feeding may be two to six times a day. All babies are different, and many of them at this age are still getting half their daily calorie intake from breast milk.”
Don't forget that breast milk can be added to solid foods such as cereals and mashed potatoes so that the baby can taste the familiar taste. If possible, use milk expressed just before feeding (not thawed) and add just before serving to keep bacteria and nutrients alive. 16
You may be pressured by others to stop breastfeeding when your baby is six months old, but the longer you breastfeed or pump, the better for you and your baby.
How long can I continue breastfeeding?
“The World Health Organization recommends breastfeeding along with solid foods until at least two years of age because it plays an important role in supporting immunity,” says Cathy. feels bad".
At eight months, the baby sometimes breastfeeds four times a day, but by one year old, the frequency of feedings can be reduced to two times a day. You yourself will understand which feeding regimen is more suitable for you and your baby. For example, Jane, a mother of two from the US, breastfed until the age of two: “I breastfed when I was at home - in the evenings and on weekends, when the children wanted to be close to me,” says Jane, “It helped a lot when they were sick . Breastfeeding has become my favorite form of comfort."
“When my son got a little older and bolder, he still often asked me to breastfeed him - as if to calm down and gain strength,” recalls Amy, a mother of two children from Canada, “When he happened to hit or skin his knee , breastfeeding was a wonderful way to comfort him. ”
”
If your baby is over a year old and you are still breastfeeding, people around you will probably tell you that this way he will never wean. But if children are not pressured, they usually refuse to breastfeed themselves between the ages of two and four. 17
“I didn’t intend to breastfeed for so long, but as a result, I still breastfeed my four-year-old daughter and 22-month-old son,” says Suzanne, mother of two from the UK, “I breastfeed my youngest before and after work, and in I express milk on business trips. The eldest daughter likes to breastfeed a little before bed or when she is upset - this is a great way to make contact. When I get tired of it, I remind myself what great benefit and comfort it brings them. I now plan to pursue a baby-initiated end breastfeeding strategy — let them decide when to stop.”
For more information on what to expect and lots of tips and tricks, see our guide Breastfeeding Problems After the First Month.
Literature
1 Ballard O, Morrow AL. Human milk composition: nutrients and bioactive factors. Pediatr Clin North Am . 2013;60(1):49-74. - Ballard O., Morrow A.L., "Composition of breast milk: nutrients and biologically active factors." Pediatrician Clean North Am. 2013;60(1):49-74.
Human milk composition: nutrients and bioactive factors. Pediatr Clin North Am . 2013;60(1):49-74. - Ballard O., Morrow A.L., "Composition of breast milk: nutrients and biologically active factors." Pediatrician Clean North Am. 2013;60(1):49-74.
2 Kent JC et al. Principles for maintaining or increasing breast milk production. J Obstet , Gynecol , & Neonatal Nurs . 2012;41(1):114-21. - Kent J.S. et al., "Principles for Maintaining and Increasing Milk Production". J Obstet Ginecol and Neonatal Nurse. 2012;41(1):114-121.
3 Kent JC Volume and frequency of breastfeedings and fat content of breast milk throughout the day. Pediatrics. 2006;117(3): e 387-395. — Kent J.S. et al. , "Amount and frequency of breastfeeding and fat content of breast milk during the day." Pediatrix (Pediatrics). 2006;117(3):e387-95.
, "Amount and frequency of breastfeeding and fat content of breast milk during the day." Pediatrix (Pediatrics). 2006;117(3):e387-95.
4 Kent JC et al. Longitudinal changes in breastfeeding patterns from 1 to 6 months of lactation. Breast Med . 2013;8(4):401-407. - Kent J.S. et al., Longitudinal changes in breastfeeding patterns from 1 to 6 months of lactation. Brest Med. 2013;8(4):401-407.
5 Almroth S, Bidinger PD. No need for water supplementation for exclusively breast-fed infants under hot and arid conditions. Trans R Soc Trop Med 1990;84(4):602-604. - Elmroth S., Bidinger P.D., "No need for supplementation of exclusively breastfed infants in hot, dry conditions." Trans R Sots Trop Med Hyg. 1990;84(4):602-604.
6 Victora CG et al . Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet. 2016;387(10017):475-490. - Victor S.J. et al., Breastfeeding in the 21st century: epidemiology, mechanisms and long-term effects. Lancet 2016;387(10017):475-490.
Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet. 2016;387(10017):475-490. - Victor S.J. et al., Breastfeeding in the 21st century: epidemiology, mechanisms and long-term effects. Lancet 2016;387(10017):475-490.
7 Peres KG et al. Effect of breastfeeding on malocclusions: a systematic review and meta - analysis. Acta Paediatr. 2015;104( S 467):54-61. - Perez K.G. et al., "The impact of breastfeeding on malocclusion: a systematic review and meta-analysis". Akta Pediatr. 2015;104(S467):54-61.
8 Mennella JA, Beauchamp GK. Maternal diet alters the sensory qualities of human milk and the nursling's behavior. Pediatrics. 1991;88(4):737-744. - Mennella, JA, Beauchamp, GK, "Maternal nutrition influences the organoleptic properties of breast milk and infant behavior." Pediatrics (Pediatrics). 1991;88(4):737-744.
1991;88(4):737-744.
9 Hassiotou F et al. Maternal and infant infections stimulate a rapid leukocyte response in breastmilk. Clin Transl immunology. 2013;2(4). - Hassiot F. et al., "Infectious diseases of the mother and child stimulate a rapid leukocyte reaction in breast milk." Clean Transl Immunology. 2013;2(4).
10 Brown A, Harries V. Infant sleep and night feeding patterns during later infancy: Association with breastfeeding frequency, daytime complementary food intake, and infant weight. Breast Med . 2015;10(5):246-252. - Brown A., Harris W., "Night feedings and infant sleep in the first year of life and their association with feeding frequency, daytime supplementation, and infant weight." Brest Med (Breastfeeding Medicine). 2015;10(5):246-252.
11 Infant sleep information source. [Internet]. Normal Infant Sleep Development; December 2017 [cited 2018 Feb] - All about baby sleep. [Internet] "The development of normal sleep in a child", December 2017 [cited February 2018].
[Internet] "The development of normal sleep in a child", December 2017 [cited February 2018].
12 Baby sleep science. [Internet]. The-Four-Month-Sleep-Regression-What-is-it-and-What-can-be-Done-About-it. March 2014 [ cited 2018 Feb ] - The science of baby sleep. [Internet], "Four-month sleep regression: what it is and what to do about it." March 2014 [cited February 2018].
13 The Myth Of Baby Sleep Regressions – What’s Really Happening To Your Baby’s Sleep? [Internet]. Pinky Mckay ; December 2017 [ cited 2018 Feb ] - "The Myth of Baby Sleep Regression - What's Really Happening to Your Baby?" [Internet]. Pinky McKay, December 2017 [cited February 2018].
14 Kendall - Tackett K ET LA0128 .











