How to burp baby after feeding video
How and When to Burp a Newborn
NewbornPediatricsLactation Consultation
Reviewed By Melinda L. Winterscheid, M.D.
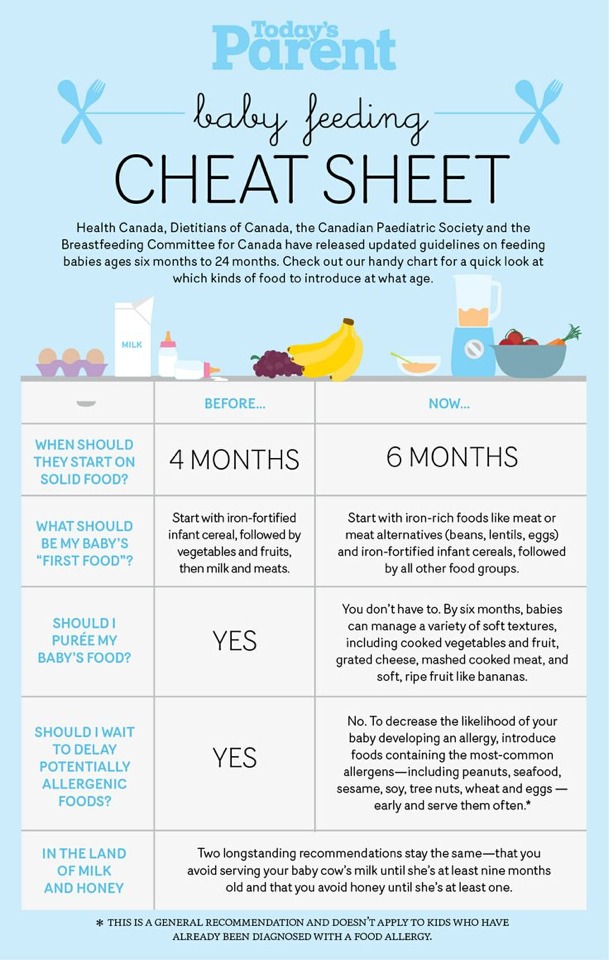
While it might not be the most glamorous of tasks, burping your baby is important for his or her comfort. When babies are feeding, they take in air, which can build up and make them uncomfortable, causing you to find yourself with a fussy, squirmy child.
When to Burp Your Baby
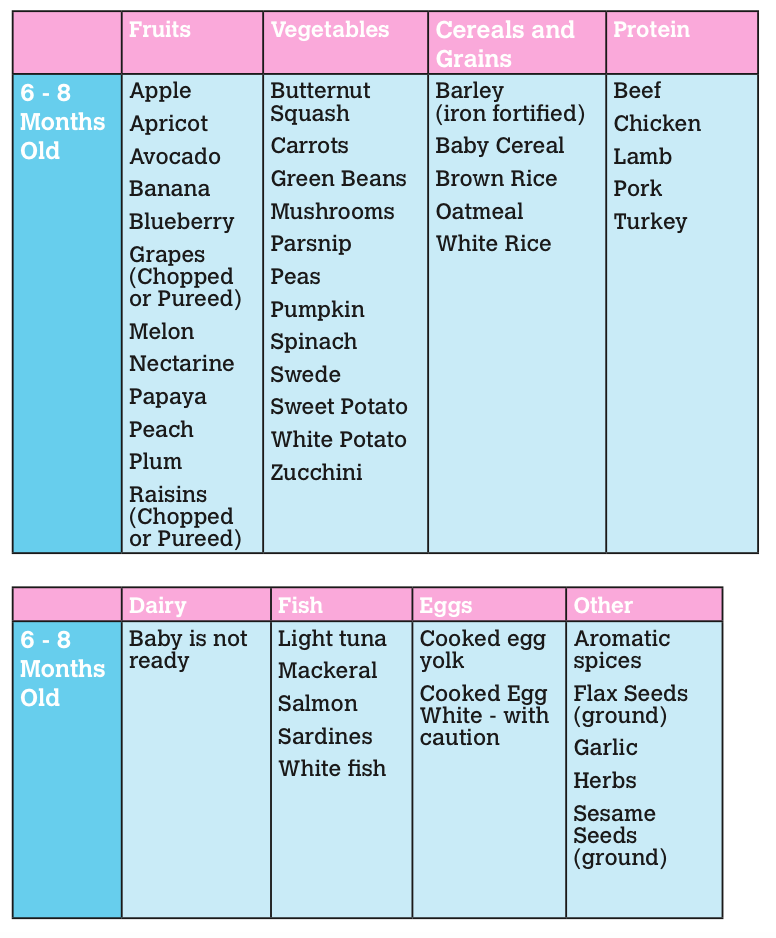
How much a baby needs to burp will vary from baby to baby. If you're burping a newborn after breastfeeding, the baby will typically burp less because they swallow less air. Most babies will outgrow the need to be burped by 4-6 months of age.
You can often tell that a baby needs to be burped if he or she is squirmy or pulling away while being fed. This being said, the American Academy of Pediatrics recommends that parents try to burp their baby:
- When a nursing mother switches breasts or
- Every 2-3 oz.
if being bottle-fed (60 – 90 mL)
Pausing to burp frequently slows feeding and reduces air intake. However, if your baby has not successfully burped after a few minutes of trying, switch methods or give up and continue with the feeding. It is possible that your baby doesn’t actually have to burp. The best method for burping will generally differ for babies and parents – use the method that works best for you.
Burping Methods
There are three popular methods for burping newborns and babies. All will require a burping cloth to protect from spit up or wet burps and a gentle patting motion across a baby’s back to coax out the burp. The main difference is how the baby is held. Take care to support the baby’s head and neck safely and move the baby slowly and gently.
- Leaning
- Place a burping cloth or towel on your shoulder and/or back.
- Rest your baby’s chin or belly on your shoulder. (If opting for the belly, make sure that your baby can breathe easily.
 Parents may benefit from trying this option after their baby has better head/neck control.)
Parents may benefit from trying this option after their baby has better head/neck control.) - Support and hold your baby in place with one hand, while using the other to gently pat your baby on the back.
- Sitting
- Place a burping cloth or towel across your lap and put a bib on your baby.
- Using your palm to support your baby’s chest and your fingers to support his or her jaw (not throat), place your baby sitting on your lap, facing away from you.
- With your free hand, gently pat your baby on the back.
- Laying
- Place a burping cloth or towel across your lap.
- Lay your baby across your knees, perpendicular to your body.
- Use one hand to support your baby’s head so that it is higher than the chest. This will prevent blood from rushing to the head.
- With your free hand, gently pat your baby on the back.
More information about feeding and burping your newborn:
When to be Concerned About Spit Up
Feeding Your Newborn
Is My Baby Eating Enough?
Newborn Pediatrics;Lactation Consultation
It looks like your browser does not have JavaScript enabled. Please turn on JavaScript and try again.
It looks like your browser does not have JavaScript enabled. Please turn on JavaScript and try again.
Please turn on JavaScript and try again.
How to Burp A Baby: A Step-By-Step Guide
Burps are not typically a pleasant sound – unless, of course, they’re coming from your new baby. Getting a good burp out of baby means they’re letting loose the air that’s trapped in their belly – which we all know feels pretty satisfying. And up until baby reaches a certain age, more often than not, they will need your help with burping; not necessarily because they can’t burp but because it’s difficult to expel air when you spend most of your time laying down.
How air gets in baby bellies varies; it can be caused by bottle feeding, breastfeeding moms who have an overactive letdown, or from a hefty crying session. If you’ve just switched over to Dr. Brown’s bottles from another bottle brand, you’ll notice baby doesn’t need as much burping as before. Still, it’s a good idea to incorporate the practice into your feeding regimen. Use this guide as to learn the ins and outs of burping baby.
Three Ways to Burp a Baby
So, what’s the best way to burp a baby? There are three popular techniques for burping – along with a plethora of other ways. For the sake of time, we’ll cover these three strategies and a few ways people tweak them.
- Over-the-Shoulder:
Simply put, it’s gently placing baby over your shoulder and patting or rubbing her back to expel trapped air. Of course, this is done with a protective layer via a burp cloth. Depending on who does this one, though, there can be a slight change in approach. Mom, lay baby in a way that positions her belly on your breast. This puts a padded layer of pressure into baby’s tummy that can facilitate release. Dad, bring baby a bit higher up so that her belly is resting closer to your shoulder for the same reason. Either way, don’t bounce her as you burp. - Face-Down on Lap:
Sit on a stable chair or couch with both feet on the ground. Lay baby tummy-down across your legs, one leg under his stomach and the other under his head, with his head turned sideways. Again with the burp cloth to avoid the dreaded “wet burp.” Use one hand to secure him and the other to gently pat or rub his back in a circular motion. When baby is a little older, some parents opt to lay on their side and place baby face-down over their hip to help burp them. - Sitting Up:
Sit baby in an upright position, lean her slightly forward, and use one hand to support her chest and head and the other hand to rub and pat her back. When baby has more head and neck control, consider what one mom did in a now-viral video. In the same position, she moved baby’s legs in, bent at the knee and lifted baby’s arms in a 90-degree angle out from baby’s body.
When to Burp Baby
Until you get to know signs baby needs a burp, there are some simple “rules-of-thumb” to follow.
Burping When Breastfeeding
For breastfeeding moms, a good time to burp baby is when you are switching breasts. If baby typically only feeds on one breast, burp during the usual “halfway point.” So, if you know baby’s usual feeding session lasts around 20 minutes, burp at the 10-minute mark.
Burping When Bottle Feeding
When to burp during bottle feeding largely depends on the bottle you’re using. With Dr. Brown’s bottles, it doesn’t need to be all that often. With non-vented bottles or bottles that can cause more air to build up, burping every 2-3 ounces consumed is a safe bet.
Whether you’re bottle or breastfeeding, after-feeding burping can be critical. Try not to wait until baby is practically asleep; jarring her awake with a burping session will not be appreciated. When baby starts to slow down, or is no longer actively sucking and swallowing, gently bring her to whichever burping position is desired.
How Long to Burp Baby
If baby doesn’t let one loose within a minute or so of trying, he probably doesn’t need any additional help. Sometimes air can take a little to work its way to the top of the stomach, though. If he is wriggling around making unhappy faces, give it another go. Unless he’s going down for a nap, consider keeping him upright for a while; sitting up helps nature take its own course.
When Can You Stop Burping Baby
The typical advice for when it’s OK to stop burping baby is anywhere between 4 – 9 months. Since that’s a huge range, we’ll offer this: If she hasn’t burped and she’s looking fussy, burp her. If she starts burping on her own, phase it out. When she can sit up for longer periods on her own, she should begin developing self-burping skills.
The Newborn that Won’t Burp
That’s ok! Whether or not baby has to burp can depend a lot on how much air they sucked in when they were feeding. With a bottle like Dr. Brown’s® Options+™, baby will burp less because they’re not taking in nearly as much air as other bottles. As long as baby is gaining weight appropriately and doesn’t seem uncomfortable, burping isn’t always necessary. Also – they may need to release it on the other end.
As long as baby is gaining weight appropriately and doesn’t seem uncomfortable, burping isn’t always necessary. Also – they may need to release it on the other end.
Burping baby doesn’t have to be a scientific endeavor; just go with your own gut and you’ll get the hang of it in no time. To learn more about the bottle that’s clinically proven to reduce colic, spit-up, and of course, burping and gas, check out our range of styles and Options+™!
How to help the baby when regulating
Support icon ofKeywords for searching
Home ›!! How to help a child in sprinkling
Home Home ›!! How to help a child in regurgitation
↑ Verki
Breastal feeding - completely special time for mom and her newborn baby. Together with the feeling of closeness and affection that feeding brings, understanding its nuances cannot but raise many questions, including the question of how to help an infant spit up. Regurgitation in a newborn is by no means always the result of a simple pat on his back.
In this article, we'll talk about the basics of helping a newborn spit up, as well as other questions you may have about spitting up.
Why do babies spit up?
Let's get it straight: why do newborns need to burp in the first place? During feeding, children usually swallow extra air - this is called aerophagia. Spitting up helps prevent this air from entering the intestines, as well as vomiting, gas, and crankiness in the baby. To avoid the return of milk after feeding, you should give the baby the opportunity to burp more often.
How to help a newborn spit up?
During the first six months, the baby should be kept upright in a column for 10-15 minutes after each feed. This will help keep the milk in his stomach, but if the baby occasionally burps anyway, parents need not worry. While carrying your baby in an upright position, you can put a baby diaper or wipes on your shoulder to keep your clothes clean.
We've already seen why spitting up is important, now let's find out how to help your baby spit up. Parents should gently pat the baby on the back with a hand folded in a handful until he burps. Folding your hand into a handful is important because clapping with a flat palm may be too strong for an infant.
Every baby is different and there is no one right position for spitting up. To get started, you can try the following options:
- Sitting position with the baby on the chest. In this position, the parent puts the baby's head with his chin on his shoulder and with one hand supports the baby under the back. With the other hand, you can gently pat the baby on the back. This method is most effective in a rocking chair or when the baby is gently rocking.
- Holding the child upright on your legs. With one hand, parents can hold the baby by the back and head, supporting his chin and placing his palm on the baby’s chest, with the other hand, you can gently pat him on the back.
 At the same time, it is important to be careful: do not press the child on the throat, but only gently support his chin.
At the same time, it is important to be careful: do not press the child on the throat, but only gently support his chin. - Holding a baby on your lap while lying on your tummy. Make sure his head is above his chest and gently pat your baby on the back until he burps.
Here are some tips on how best to help your newborn spit up:
- Let your baby spit up during feeding. If the baby is restless or has swallowed air, it is worth giving him the opportunity to burp during feeding, and not just after.
- When bottle feeding, let the newborn burp after every 50-60 ml.
- When breastfeeding, let the baby burp at every breast change.
It is important to let your baby spit up after eating, even if he spit up during feeding!
If your baby is gassy, spit up more often. Also, if he vomits frequently or suffers from gastroesophageal reflux disease (GERD), have him spit up after every 30 ml bottle-feeding or every five minutes while breastfeeding.
How long should a baby be held for it to burp? It's different for everyone, but generally keeping a newborn upright for 15 to 20 minutes after a feed helps the milk stay in the baby's stomach.
Minimize the amount of air you swallow. Gas production and regurgitation result from aerophagia during feeding. The baby will inevitably swallow air, but there are ways to prevent it from swallowing too much. Whether you bottle feed your baby or combine breastfeeding with bottle feeding, the Philips Avent anti-colic bottle with AirFree valve is designed so that the nipple is always filled with milk without excess air, even in a horizontal position, thus preventing the baby from swallowing excess air during feeding.
Reducing the amount of air your baby swallows can help reduce your baby's risk of colic, gas, and spitting up.
Breastfeeding is a wonderful time to strengthen the bond between parent and baby. Every mom and every baby is different, so learning to help your newborn burp properly can take time and practice.
Articles and tips from Philips Avent
Baby+ app
Download the app and track your child's development and growth with trackers, and keep those special moments forever.
Download app:
You are leaving the Philips Healthcare (“Philips”) official website. Any links to third party websites that may be included on this site are provided solely as a convenience to you. Philips makes no warranties regarding any third party websites or the information they contain.
I understand
You are about to visit a Philips global content page
Continue
You are about to visit the Philips USA website.
I understand
How to properly hold a newborn after a feed so that the baby burps
Why it is recommended to hold a newborn upright
Why modern pediatricians do not approve of this method
Why else can a baby spit up food
When wearing a upright is justified
How to hold a newborn after feeding
If a baby starts spitting up milk or adaptive infant formula, mothers turn to the Internet for help in fright. There you can find recommendations on how to hold a newborn after feeding, including a “column”.
There you can find recommendations on how to hold a newborn after feeding, including a “column”.
Babies are said to swallow excess air during feeding. The upright position and a pat on the back of the baby should help him release this air, which in turn reduces the frequency of colic and the amount of spitting up. The recommendation took place in the USSR, but even now some pediatricians continue to insist that after feeding the baby should be kept upright.
Do not miss
-
Don't miss
Regurgitation in newborns: what should alert parents (asked the doctor)
The famous American pediatrician Clay Jones and the popular doctor Komarovsky do not recommend carrying babies in a column after feeding. Doctors believe that this is a pointless exercise that does not eliminate the original cause of swallowing air. And it lies in the wrong attachment to the chest. It is because of him that excess air enters the esophagus to the baby.
And it lies in the wrong attachment to the chest. It is because of him that excess air enters the esophagus to the baby.
In addition, there are a number of studies that confirm that post-feeding anxiety and reflux in babies are not at all related to excess air in the stomach. There is no physiological reason why they cannot burp on their own. Therefore, they do not need help in this. And keeping a newborn in a column after feeding is completely optional.
Do not miss
-
Don't miss
Which diapers for newborns are better: rating 2020
Another study of 71 pairs of twins showed that a pat on the back had no effect on whether the baby had colic or not. In addition, this action increased the frequency of regurgitation. It turns out that patting a baby on the back, who has just eaten, leads to vomiting.
It is normal to spit up up to two tablespoons of milk or dairy food per day. If you are afraid that the child may burp during sleep and choke, then put him to sleep on his side. So that he does not accidentally roll over by himself, you can put a towel folded into a tube or a light diaper under his back. Or use a special sleep positioner.
The presence of air in the esophagus is not the only cause of regurgitation. There are at least three more.
- Too much dairy food;
- weakness of the lower esophageal sphincter;
- immaturity of the neuromuscular apparatus of the esophagus.
Carrying the baby upright after feeding may be useful in one case - if the baby has gastroesophageal reflux. This is a syndrome where the contents of the stomach rise up and regurgitate too often. The doctor establishes the diagnosis. If it is confirmed, then parents are given recommendations that indicate special positions for feeding and wearing after it.
The first three months of life are often referred to as the period of term or even the fourth trimester of pregnancy. If the baby did not fall asleep after feeding, then it is important for him to be with his mother: to feel her warmth, smell, hear her voice and heartbeat.
It does not matter at all what position to keep the newborn after feeding, if it is physiological. It can be a "cradle", "monkey on a branch", "soldier" with his head on his mother's shoulder. If feeding occurs before a night's sleep, then the baby can simply be put in the crib.
After three months of life, the situation may change. To establish a routine, the mother can start feeding the baby in the middle of waking hours so that he does not fall asleep immediately after eating. In this case, after feeding the child, it is better to lower it to the floor so that it can play a little and get tired before going to bed.
References
- Abaturov A. E. et al. Excess gas syndrome in children // Health of the child, 2012.