Power feeding baby
Can It Increase Your Milk Supply?
We’ve heard all the facts from the American Academy of Pediatrics (AAP), about how breastfeeding can protect babies against respiratory tract infections, ear infections, urinary tract infections, and even lower the risk of childhood obesity.
Learning about these benefits of breastfeeding likely influenced your decision to breastfeed your own baby. When you read all the benefits, it seems almost magical. But when it comes to nursing, everything doesn’t always feel magical. In fact, sometimes a drop in supply can feel like the worst kind of trick.
Some babies can’t latch on or refuse the breast, and if you’re like some mothers, you might experience a drop in milk supply at some point, making nursing or pumping difficult, if not impossible.
But while a sudden drop in milk supply can number your breastfeeding days, it doesn’t have to. Some mothers have been able to increase milk production with power pumping.
Power pumping is a technique that’s designed to mimic cluster feeding, and in turn, encourage your body to begin producing more breast milk.
With cluster feeding, your breastfed baby has shorter feedings more frequently than usual. So rather than one full feeding every 3 hours, your baby might have two or three short feeds over a few hours each day. Since your baby is feeding more often, your body responds to the demand by naturally increasing your milk supply.
Power pumping can produce similar results. The idea is to pump more frequently within a set time frame each day so that your body increases its milk supply naturally.
Other ways to increase milk supply can include taking supplements like fenugreek, oatmeal, or flaxseed, or asking your doctor to prescribe medication. But while these options are effective for some women, power pumping might provide a faster fix and increase your supply in as little as a few days.
Plus, when you’re able to increase your supply naturally, there’s no risk of unexpected side effects from supplements and medication, which might include restlessness, headache, sleep problems, or nausea.
But while power pumping is an excellent way to produce more milk, this technique is only recommended for women who need to increase their milk supply.
So if your body produces enough milk to keep up with your baby’s demands, this technique isn’t for you. Oversupply can actually be an issue, so if your supply is good, stick to what is working.
Keep in mind that milk supply can drop for various reasons. Some mothers experience a drop when they return to work and they’re not able to breastfeed as frequently.
Also, skipping breastfeeding sessions can cause a decline in supply. This might occur once your baby starts eating solid foods and doesn’t want to nurse as often, if your baby starts taking longer naps, or if their newfound skills make them too busy to stay interested through a feeding.
Your breastfeeding supply might also shift if you become ill or are menstruating, and some women see a drop in supply when taking hormonal contraceptives or medications containing pseudoephedrine.
Regardless of the reason behind a decrease in milk supply, power pumping can help naturally stimulate milk production and get your pumping routine back on track.
Related: 5 ways to increase breast milk production
To be clear, there are no hard or fast rules with regard to a power pumping schedule or duration. The general idea, though, is pumping more often during a span of time each day so that your body naturally responds to the extra demand.
For the best results, you’ll likely need to devote at least an hour a day over at least a week to power pumping, although some mothers power pump for up to 2 hours in a day.
Be mindful that it’s important to take breaks during your power pumping sessions to avoid nipple or breast soreness. One possible schedule is as follows:
- pump 20 minutes
- rest 10 minutes
- pump 10 minutes
- rest 10 minutes
- pump 10 minutes
You can repeat this schedule once or twice daily. Or try an alternative power pump schedule:
- pump 5 minutes
- rest 5 minutes
- pump 5 minutes
- rest 5 minutes
- pump 5 minutes
You can repeat this schedule up to five or six times daily.
The length of time you’ll need to power pump depends on your body. So while some mothers might have great results with single 1-hour sessions after a couple of days, other mothers may need to power pump for 2 hours a day for at least a week to see an increase in supply.
Although you can use a manual or an electric pump, an electric pump might work better given the frequency of pumping. With a manual pump, there’s the likelihood of your hands getting tired before you’re able to complete a session.
You might also try double pumping: using both breasts during each session. Alternatively, you may wish to feed your baby on one breast while pumping the other.
Related: Guide to choosing, using, and maintaining a breast pump
Before power pumping, consider the reasons why your supply may be dropping.
Investigate whether there’s a problem with your breast pump, such as broken parts or poor suction. Normal wear and tear can make a pump ineffective, producing little, if any breast milk.![]()
As a general rule of thumb, if you’ve been using your breast pump frequently and it’s older than a year, replace it to see if your milk supply increases.
You can also take the pump to a lactation store or service center to make sure it’s working properly. They can test the machine and recommend replacement parts.
Before power pumping, consider scheduling an appointment with a lactation consultant. It may be that you’re breastfeeding or pumping improperly and, as a result, your baby isn’t getting enough milk. Some simple adjustments to the baby’s latch or your pumping routine may be all you need.
Signs of poor milk supply include your baby not gaining weight or losing weight or not having enough wet and dirty diapers. Many typical baby behaviors, like frequent feedings or fussiness, may make parents think that milk supply is low, but as long as your baby is steadily gaining weight and producing wet and dirty diapers, they’re getting what they need.
If you’re not sure, or have any concerns about breastfeeding, speak with a lactation consultant for more information.
Again, women who don’t have a problem with milk supply should not power pump. This can cause an oversupply of breast milk where the breasts produce too much milk. This can cause breast engorgement and painful swelling that makes it difficult for a baby to breastfeed.
Also avoid power pumping if your baby already has a pattern of cluster feeding and you’re able to breastfeed during those times. This schedule in itself will naturally increase your breast milk supply. Plus, cluster feeding by your baby will be more efficient than pumping.
Along with power pumping, here are other general tips to maintain your milk supply.
Keep up with regular feedingsThe more your baby breastfeeds, the more milk your breasts will produce. The amount of time you’ll need to devote to breastfeeding depends on your baby’s age and their feeding habits.
For example, newborns may need to nurse 8 to 12 times a day for the first month, and then drop to 7 to 9 times a day by 1 or 2 months of age.
Keep an eye out for signs that your baby is hungry. This can include opening their mouth, placing their hands in their mouth, puckering their lips, and sticking out their tongue.
Focus on relaxingBeing relaxed and comfortable during feedings can stimulate letdown, which is a natural reflex that stimulates the flow of milk from breast to baby. During feedings, try to avoid distractions, clear your mind, and sit in a comfortable chair.
Switch breastsIt’s easy to get into a routine of breastfeeding in the same position, which might involve starting or ending each feed with the same breast. To keep your milk supply steady, switch breasts each feeding.
Massage your breastMassaging your breasts a few minutes before pumping or during pumping help release any clogged milk ducts, allowing your milk to flow more freely.
Use the correct pump flangeYour pumping sessions might be shorter if you have pain or discomfort.![]() This can happen if you’re using the wrong size flange (plastic piece that goes over your nipple). Find a flange that’s the correct fit for your nipple and breast to reduce friction and pain.
This can happen if you’re using the wrong size flange (plastic piece that goes over your nipple). Find a flange that’s the correct fit for your nipple and breast to reduce friction and pain.
A drop in milk supply can be frustrating and emotional, especially if you’re not ready to quit breastfeeding. Rather than give up, experiment with power pumping to trick your body into producing more milk. Be patient, though.
Some women notice an increase in as little as 1 to 2 days, but it might take a week or longer. If you have any concerns about milk supply, schedule an appointment with a lactation consultant.
What Are They and How Do I Do It?
Icon of phone 1-844-867-9890
Check Your Insurance Eligibility
Toggle Nav
Search
Menu
Account
- By Brianne Griffis
- Apr 13, 2021
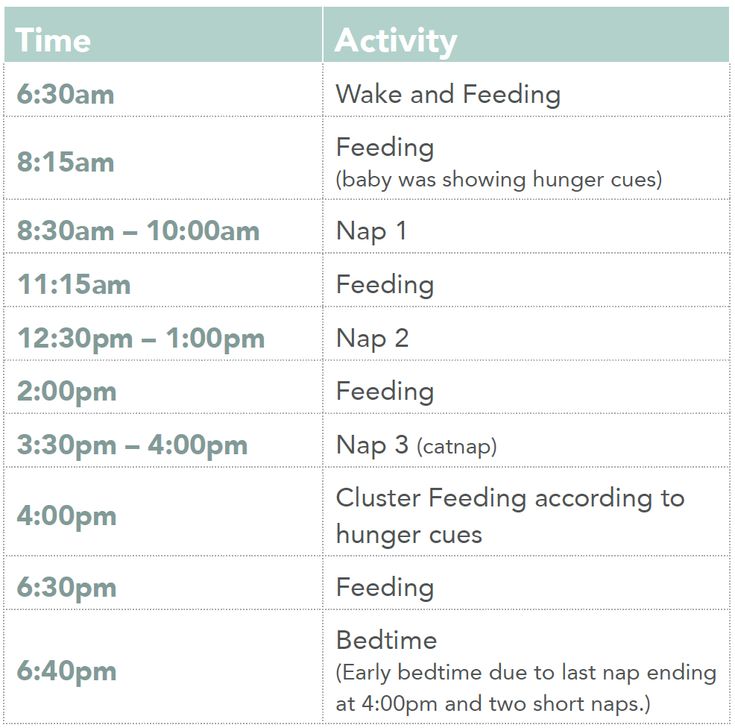
Newborn babies feed quite often throughout the day and night, generally with about 2 to 3 hours between each feeding. When your breastfed baby is suddenly fussing more and wanting feeding sessions much sooner than every 2 to 3 hours or is nursing for extended periods of time only to be ready to eat again less than an hour later, this is known as cluster feeding. Cluster feeding can be worrisome to breastfeeding moms because they are not sure their babies are getting enough to eat or that there is enough milk to satisfy their babies. Additionally, they may be tempted to supplement because they feel they have a low milk supply.
When your breastfed baby is suddenly fussing more and wanting feeding sessions much sooner than every 2 to 3 hours or is nursing for extended periods of time only to be ready to eat again less than an hour later, this is known as cluster feeding. Cluster feeding can be worrisome to breastfeeding moms because they are not sure their babies are getting enough to eat or that there is enough milk to satisfy their babies. Additionally, they may be tempted to supplement because they feel they have a low milk supply.
Why Do Babies Cluster Feed?
If your baby starts cluster feeding, this often goes hand-in-hand with fussiness and is generally linked to growth spurts. Babies will experience several growth spurts in the first few months of life; so many in fact that it sometimes feels like your baby is in a never-ending growth spurt! Growth spurts typically occur around 7-10 days after birth, between 2 and 3 weeks, again between 4 and 6 weeks, and around 12 weeks. Each time your baby goes through one of their growth spurts, they may temporarily start to breastfeed more or cluster feed as a way to boost your milk supply. Take comfort in knowing that growth spurts are temporary and will not last long.
Each time your baby goes through one of their growth spurts, they may temporarily start to breastfeed more or cluster feed as a way to boost your milk supply. Take comfort in knowing that growth spurts are temporary and will not last long.
How Long Does Cluster Feeding Last?
Periods of evenings filled with back-to-back feedings with a fussy baby are generally short-lived. Most growth spurts and episodes of cluster feeding will pass in just a few days. After a growth spurt, your baby’s feeding patterns will likely return to how they were prior to the growth spurt. Cluster feeding in the late afternoon may help your baby sleep better and for longer stretches!
What Can I Do to Increase My Milk Supply?
Cluster feeding is mother nature’s way of boosting milk production - as demand for breast milk goes up our bodies receive the signal to begin producing more milk to meet the baby’s increased consumption. During periods of cluster feeding and growth spurts, it is important to continue breastfeeding on-demand and allowing your little one to decide when they have had enough to eat. Be sure to continue drinking plenty of water and consider incorporating powering pumping into your routine. Additionally, we encourage you to reach out to a lactation consultant or IBCLC for personalized breastfeeding support and medical advice.
During periods of cluster feeding and growth spurts, it is important to continue breastfeeding on-demand and allowing your little one to decide when they have had enough to eat. Be sure to continue drinking plenty of water and consider incorporating powering pumping into your routine. Additionally, we encourage you to reach out to a lactation consultant or IBCLC for personalized breastfeeding support and medical advice.
What is Power Pumping?
Power pumping is like boot camp for your milk supply and mimics what it is like when your baby is going through a growth spurt or cluster feedings. When done properly, moms will begin to notice their milk supply increasing after about 3 days of a daily power pumping routine.
When is the Best Time to Power Pump?
To be most effective, power pumping should be done once a day for 5-7 days in a row at approximately the same time every day. Depending on your schedule, you may find it is easiest to power pump after your baby’s first time nursing for the day or just before you go to bed. Pumping in the morning is nice because moms generally have the most milk in the morning and you will not need to worry about there being enough milk available for your baby's needs at the next feeding. Pumping in the evening hours is especially helpful in boosting milk supply in the latter part of the day and is less stressful since babies will usually sleep the longest at the beginning of the night. After power pumping for 5-7 consecutive days, you should see the full effects and can stop power pumping. If you would like to further boost your milk supply, consider doing another 5-7 days of power pumping after taking a week off from power pumping.
Depending on your schedule, you may find it is easiest to power pump after your baby’s first time nursing for the day or just before you go to bed. Pumping in the morning is nice because moms generally have the most milk in the morning and you will not need to worry about there being enough milk available for your baby's needs at the next feeding. Pumping in the evening hours is especially helpful in boosting milk supply in the latter part of the day and is less stressful since babies will usually sleep the longest at the beginning of the night. After power pumping for 5-7 consecutive days, you should see the full effects and can stop power pumping. If you would like to further boost your milk supply, consider doing another 5-7 days of power pumping after taking a week off from power pumping.
Power Pumping Instructions
- Pump for 20 minutes
- Take a 10 minute break from pumping
- Pump for 10 minutes
- Take a 10 minute break from pumping
- Pump for 10 minutes
Need a Breast Pump?
Breast pumps come in handy so many times throughout a mother’s breastfeeding journey and are especially helpful when trying to increase milk production. Under the Affordable Care Act, many moms can get a free breast pump through insurance. Fill our Aeroflow Breastpumps' Qualify Through Insurance Form and they can quickly and easily help you find out if you qualify for a free pump.
Under the Affordable Care Act, many moms can get a free breast pump through insurance. Fill our Aeroflow Breastpumps' Qualify Through Insurance Form and they can quickly and easily help you find out if you qualify for a free pump.
About the Author
Brianne Griffis, Certified Lactation Counselor
Information provided in blogs should not be used as a substitute for medical care or consultation.
How To's Ask An Expert
Share:
Posted in Breastfeeding and Breast Pumping
Related Posts
Recent Posts
Feeding children with special needs
American Academy of Pediatrics and The American College of Obstetricians and Gynecologists. Breastfeeding Handbook for Physicians 2006). - American Academy of Pediatrics and American College of Obstetrics and Gynecology. "Medical Guide to Breastfeeding", 2006.
Lawrence , R . A . & Lawrence , R . M . Breastfeeding : a guide for the medical profession ( Elsevier Mosby , Maryland Heights , MO , 2011). - Lawrence R.A., Lawrence R.M., "Breastfeeding: A guide for healthcare professionals." (Publisher Maryland Heights , Missouri, USA: Elsevier Mosby; 2011.)
Prime, D.K.et al. Simultaneous breast expression in breastfeeding women is more efficacious than sequential breast expression. Breastfeed Med 7, 442-447 (2012). - Prime D. K. et al., “During the breastfeeding period, pumping both breasts simultaneously is more productive than sequential pumping.” Brest Med (Breastfeeding Medicine) 7, 442-447 (2012).
K. et al., “During the breastfeeding period, pumping both breasts simultaneously is more productive than sequential pumping.” Brest Med (Breastfeeding Medicine) 7, 442-447 (2012).
Morton, J., Hall, J.Y., Wong, R.J., Benitz, W.E. & Rhine, W.D. Combining hand techniques with electric pumping increases milk production in mothers of preterm infants. J Perinatol 29, 757–764 (2009). — Morton J., Hall J.I., Wong R.J., Benitz W.I. and Rhine, W.D., "Manual pumping combined with an electric breast pump increases breast milk production in mothers of preterm infants." J Perinatol (Journal of Perinatology) 29, 757-764 (2009)
Hill, P.D., Aldag, J.C., Chatterton RT. Initiation and frequency of pumping and milk production in mothers of non-nursing preterm infants. J Hum Lact . 2001;17(1):9–13 - Hill P.D., Aldag J.S. and Chatterton, R.T., "Onset and frequency of expression and milk production in mothers who have given birth to premature babies and have not breastfed them. " J Hum Lakt (Journal of the International Association of Lactation Consultants) 17, 9-13 (2001).
" J Hum Lakt (Journal of the International Association of Lactation Consultants) 17, 9-13 (2001).
Hill, P.D., Aldag, J.C., Chatterton RT, Zinaman M. Comparison of Milk Output Between Mothers of Preterm and Term Infants: The First 6 Weeks After Birth. J Hum Lact . 2005 February 1, 2005; 21(1):22–30. - Hill P.D., Aldag J.S., Chatterton R.T., Zinaman M., "Comparison of the amount of milk in mothers of full-term and premature babies in the first 6 weeks after birth." J Hum Lakt (Journal of the International Association of Lactation Consultants) 2005, 21(1): 22-30.
Parker, L.A., Sullivan, S., Krueger, C. & Mueller, M. Association of timing of initiation of breastmilk expression on milk volume and timing of lactogenesis stage II among mothers of very low-birth-weight infants. Breastfeed Med (2015). - Parker L.A., Sullivan S. , Kruger S., Kelechi T. and Muller M., "Association of the time of initiation of expression with the amount of milk and the timing of the second stage of lactogenesis in mothers of children who had extremely low birth weight" . Brestfeed Med (Breastfeeding Medicine) (2015)
, Kruger S., Kelechi T. and Muller M., "Association of the time of initiation of expression with the amount of milk and the timing of the second stage of lactogenesis in mothers of children who had extremely low birth weight" . Brestfeed Med (Breastfeeding Medicine) (2015)
Meier, P.P., Engstrom, J.L., Janes, J.E., Jegier, B.J. & Loera, F. Breast pump suction patterns that mimic the human infant during breastfeeding: Greater milk output in less time spent pumping for breast pump-dependent mothers with premature infants. J Perinatol 32, 103-110 (2012). - Meyer P.P., Engstrom J.L., Jaynes J.I., Jaegier B.J., Loera F. "Pumping patterns that mimic the behavior of a breastfeeding baby: more milk and less time for constant pumping mothers of premature babies". J Perinatol (Journal of Perinatology) 32, 103-110 (2012).
Torowicz, D.L., Seelhorst, A., Froh, E.B., Spatz, D.L. Human milk and breastfeeding outcomes in infants with congenital heart disease. Breastfeed Med 10, 31–37(2015). - Torowicz DL , Seelhorst , FroH EB , Spatz DL , "Breast milk and breastfeeding outcomes for children with congenital heart disease", Brestfeed Med (Breastfeeding Medicine) 10, 31-37 (2015).
Breastfeed Med 10, 31–37(2015). - Torowicz DL , Seelhorst , FroH EB , Spatz DL , "Breast milk and breastfeeding outcomes for children with congenital heart disease", Brestfeed Med (Breastfeeding Medicine) 10, 31-37 (2015).
Reilly, S. et al. ABM clinical protocol #18: Guidelines for breastfeeding infants with cleft lip, cleft palate, or cleft lip and palate, revised 2013. Breastfeed Med 8, 349–353 (2013) - Reilly S. et al., " AVM Clinical Protocol No. 18: Guidelines for breastfeeding children with cleft lip, cleft palate, or cleft lip and palate, 2013 edition. Brestfeed Med (Breastfeeding Medicine) 8, 349–353 (2013).
Thomas, J., Marinelli, K.A., & Hennessy, M. ABM clinical protocol #16: Breastfeeding the hypotonic infant. Breastfeed Med 2, 112–118 (2007). — Thomas J., Marinelli C.A. and Hennessy, M., "AVM Clinical Protocol #16: Breastfeeding a Baby with Reduced Muscle Tone." Brestfeed Med (Breastfeeding Medicine). 2, 112–118 (2007)
Breastfeed Med 2, 112–118 (2007). — Thomas J., Marinelli C.A. and Hennessy, M., "AVM Clinical Protocol #16: Breastfeeding a Baby with Reduced Muscle Tone." Brestfeed Med (Breastfeeding Medicine). 2, 112–118 (2007)
Helping children develop healthy eating habits
Maureen M. Black, PhD, Kristen M. Hurley, PhD
University of Maryland School of Medicine, USA
, 2nd rev. ed. (English language). Translation: August 2015
Introduction
The first year of a child's life is characterized by rapid age-related changes related to nutrition. As infants gain control of their own bodies, they move from the stage of sucking liquids in a recumbent or reclining position to the stage of eating solid foods in a sitting position. Oral motor skills are developed, moving from a basic "sucking-swallowing" mechanism based on breast milk or formula to a "chewing-swallowing" mechanism based on the consumption of semi-solid foods, gradually moving to more complex combined types of food. 1.2 When infants already regulate their movements well, they move from passive feeding, in which someone feeds them, to independent feeding, at least occasionally. The infant's diet is enriched: through the introduction of mashed potatoes and specially prepared foods, the transition is made from breast milk and formula for feeding to the family diet. By the end of the first year of life, children are already able to sit, chew and swallow on their own, consuming different types of food, learn to eat independently and move on to a diet and diet that is characteristic of the whole family.
Oral motor skills are developed, moving from a basic "sucking-swallowing" mechanism based on breast milk or formula to a "chewing-swallowing" mechanism based on the consumption of semi-solid foods, gradually moving to more complex combined types of food. 1.2 When infants already regulate their movements well, they move from passive feeding, in which someone feeds them, to independent feeding, at least occasionally. The infant's diet is enriched: through the introduction of mashed potatoes and specially prepared foods, the transition is made from breast milk and formula for feeding to the family diet. By the end of the first year of life, children are already able to sit, chew and swallow on their own, consuming different types of food, learn to eat independently and move on to a diet and diet that is characteristic of the whole family.
As children make the transition to a family diet, recommendations no longer apply only to food, but also to nutritional conditions. A variety of healthy foods improves the quality of the diet in the same way as early and regular recognition of new types of food by the child. Data on infants and young children aged 6 to 23 months, collected in 11 countries around the world, show a positive relationship between dietary diversity and nutritional status (nutritive status). 3 Teaching a child to consume fruits and vegetables during infancy and early childhood is associated with the adoption of these types of food at an older age. 4-6
A variety of healthy foods improves the quality of the diet in the same way as early and regular recognition of new types of food by the child. Data on infants and young children aged 6 to 23 months, collected in 11 countries around the world, show a positive relationship between dietary diversity and nutritional status (nutritive status). 3 Teaching a child to consume fruits and vegetables during infancy and early childhood is associated with the adoption of these types of food at an older age. 4-6
Eating habits and preferences are formed in children at an early age. If children forgo nutrient-dense foods such as fruits and vegetables, mealtimes can become stressful or wrestling. As a result, children may be deprived of both the nutrients they need and healthy, understanding relationships between them and caregivers. Adults who are inexperienced or stressed, and those who themselves have unhealthy eating habits, need help to establish healthy and fulfilling eating behaviors in children during the meal.
Item
Eating problems occur in 25% - 45% of all children, especially at a time when children are learning new skills, and new types of food or expectations associated with eating them become real for them test. 7 For example, the period of infancy and early childhood is characterized by a desire for independence - children try to do everything on their own. When these characteristics are also applied to eating behavior, it suggests that children may be neophobic (fear of trying new foods) and insist on a limited set of foods consumed, 8 which further leads to the perception of these children as picky eaters.
Most eating problems are temporary and easily resolved with little or no intervention. However, when such problems continue for a long time, their presence can slow down the child's growth, development and worsen relationships with people caring for him. This leads to long-term problems with the health and development of the child.![]() 9 Children with persistent eating problems may be at risk of developing growth and behavioral problems if caregivers do not seek help in a timely manner, allowing a critical situation to develop.
9 Children with persistent eating problems may be at risk of developing growth and behavioral problems if caregivers do not seek help in a timely manner, allowing a critical situation to develop.
Issues
Eating habits are influenced by age, family or environment. As they mature and are able to make the transition to a family diet, their internal regulatory signals for hunger and satiety may be suppressed by family and cultural patterns. In families where adults lead by example in healthy eating, children are more likely to eat more fruits and vegetables than children in families where they do not. At the same time, in a family where it is customary to eat less healthy food, snacks are abused, children are likely to have eating habits and taste preferences characterized by the consumption of excess amounts of fat and sugar. 10 In terms of environmental influences, children's exposure to fast food restaurants and similar establishments has resulted in increased consumption of high-fat foods, such as french fries, while not eating more nutrient-dense foods, such as fruits and vegetables. 11 What's more, adults may not realize that many commercial products advertised as products for children (such as sugary drinks) can satisfy hunger or thirst but provide minimal nutritional intake. 12
11 What's more, adults may not realize that many commercial products advertised as products for children (such as sugary drinks) can satisfy hunger or thirst but provide minimal nutritional intake. 12
A number of nationwide studies have documented excessive consumption of high-energy foods during early childhood, 13.14 while many children consume critically low amounts of fruits, vegetables and essential micronutrients. 15 By the time they enter primary school, many children get half their fluid intake from sugary drinks. 16 This eating habit is undoubtedly developed during early childhood and preschool age. The presence of these unhealthy eating habits (eating foods high in fat, sugar, and refined carbohydrates; sugary drinks; eating limited fruits and vegetables) increases the likelihood of micronutrient deficiencies (such as iron deficiency anemia) and overweight in young children. 17
Scientific context
The process of eating is often studied through observational data or adult reports of eating behavior. Some investigators rely on clinical study of groups of children with stunting or nutritional problems, others select children without any abnormalities for research.
Some investigators rely on clinical study of groups of children with stunting or nutritional problems, others select children without any abnormalities for research.
Key Questions
Key Questions explore the development of eating habits from infancy through early childhood, and the ways in which children report feeling hungry or full. In addition, this includes studying the reasons why some children (so-called "picky eaters") have selective food preferences. Key challenges for caregivers and families are to find ways to promote healthy eating habits in young children, encourage children to eat healthy foods, and prevent problems with feeding and growth.
Recent Research Findings
Attachment and Nutrition
Healthy eating habits develop in infancy as infants and their parents develop a partnership in which they recognize and interpret both verbal and non-verbal communication cues each other. This reciprocal process forms the basis for building an emotional bond or attachment in infants and caregivers that is an integral part of healthy social functioning. 18 If communication between a child and adults is disrupted, characterized by incoherent, unresponsive interactions, then bonds of attachment can be unreliable, resulting in the process of eating can turn into unproductive, exhausting quarrels over food.
18 If communication between a child and adults is disrupted, characterized by incoherent, unresponsive interactions, then bonds of attachment can be unreliable, resulting in the process of eating can turn into unproductive, exhausting quarrels over food.
Infants who do not communicate clearly about their needs, or who do not respond to caregivers' attempts to teach them regular and predictable habits related to eating, sleeping, and playing, are at risk of acquiring regulatory problems associated with eating as well. 9 Premature or sick babies may react more slowly than full-term babies, making it more difficult for these babies to express feelings of hunger or fullness. Adults who do not recognize signs of satiety in their children tend to overfeed them, causing infants to associate satiety with frustration and conflict.
Feeding in the context of the adult-child relationship
Variability in the context of the adult-child relationship during feeding is associated with feeding behavior and growth of the child.![]() 19 Aspects of parental behavior and guardianship, which include factors of perception and understanding of the child's behavior, are also applicable to the nature of feeding (Table 1). 20,21,22 Responsive feeding reflects an interaction-based behavioral pattern in which adults provide control and developmentally appropriate responses to a child's hunger or satiety signals. The unresponsive feeding process is marked by a lack of reciprocity between adults and the child. This is characterized by parents being overly in control of the feeding process (by forcing the child to eat or limiting the child's diet), or by the fact that the child controls the feeding process (for example, requires a limited menu, or eats only after much persuasion), or by the fact that an adult ignores the child's signals, or cannot organize the correct diet (isolated feeding). 23.24
19 Aspects of parental behavior and guardianship, which include factors of perception and understanding of the child's behavior, are also applicable to the nature of feeding (Table 1). 20,21,22 Responsive feeding reflects an interaction-based behavioral pattern in which adults provide control and developmentally appropriate responses to a child's hunger or satiety signals. The unresponsive feeding process is marked by a lack of reciprocity between adults and the child. This is characterized by parents being overly in control of the feeding process (by forcing the child to eat or limiting the child's diet), or by the fact that the child controls the feeding process (for example, requires a limited menu, or eats only after much persuasion), or by the fact that an adult ignores the child's signals, or cannot organize the correct diet (isolated feeding). 23.24
parents and child are in a relationship where requirements are clearly expressed and there is a mutual interpretation of signals for feeding. Responsive feeding is characterized by short-term interaction based on behavioral characteristics and consistent with a certain stage of development of the child. In the course of this interaction, both sides easily compromise. 22,25,26
Responsive feeding is characterized by short-term interaction based on behavioral characteristics and consistent with a certain stage of development of the child. In the course of this interaction, both sides easily compromise. 22,25,26
A controlling feeding style, well structured but low in caring, is typical of parents who use forceful or restrictive strategies to control the feeding process. A controlling feeding style is part of an authoritarian parenting model and may include overly assertive behaviors such as loud talking, force feeding, or other ways to get a child to do what they want. 27 Parents who control the feeding process can suppress the child's internal regulatory signals of hunger or satiety. 28 Infants' innate ability to self-regulate energy consumption disappears during early childhood due to the influence of family and cultural patterns. 29
An indulgent feeding style, characterized by a high level of nurturance and less structure, is an element of the indulgent parenting model. With this style of feeding, parents allow the child to decide for himself what to eat and when. 23 If the parents do not refer the child, the child is more likely to choose foods high in salt and sugar over a more balanced diet that includes vegetables. 23 Thus, an indulgent feeding style can be problematic given the genetic predisposition of infants to salty or sweet foods. 30 Babies whose parents practice indulgent feeding styles often weigh more than children of parents who use other feeding styles. 24
With this style of feeding, parents allow the child to decide for himself what to eat and when. 23 If the parents do not refer the child, the child is more likely to choose foods high in salt and sugar over a more balanced diet that includes vegetables. 23 Thus, an indulgent feeding style can be problematic given the genetic predisposition of infants to salty or sweet foods. 30 Babies whose parents practice indulgent feeding styles often weigh more than children of parents who use other feeding styles. 24
Detached feeding style, characterized by both low levels of nurturance and a less structured structure, is common among parents with a lack of knowledge and involvement in their child's eating behavior. 23 A detached feeding style may show signs such as lack of active assistance or verbalization during feeding, lack of communication between parent and child, negative feeding environment, and lack of an orderly structure or pattern of feeding. Indifferent parents often ignore both the feeding advice and the child's signals of hunger or satiety; they may not know what and when their child eats. Egeland and Sroufe 31 found that children of distant or psychologically unavailable parents were more likely to experience anxiety compared to children whose parents were actively involved in the process. Accordingly, a detached feeding style is an element of a detached parenting style. 23
Indifferent parents often ignore both the feeding advice and the child's signals of hunger or satiety; they may not know what and when their child eats. Egeland and Sroufe 31 found that children of distant or psychologically unavailable parents were more likely to experience anxiety compared to children whose parents were actively involved in the process. Accordingly, a detached feeding style is an element of a detached parenting style. 23
Several recent systematic reviews show an association between parental control of feeding and weight gain in infants and young children and/or weight class. 24,32,33 Control feeding is associated with weight gain (eg, children whose parents have a restrictive feeding style tend to overeat) 34 and weight loss (eg, children who are forced to eat more do not tend to overeat). 35 However, the cross-sectional nature of most studies, coupled with a tendency to rely solely on parental behavioral data without considering the importance of interactions during feeding, makes it difficult to understand parent-child interactions during feeding. A recent double-blind study of infants in Australia found that adherence to preventive infant feeding guidelines led to normal weight gain and improved mutual understanding during feeding, as judged by the respondents. 36 More research is needed to better understand strategies for promoting healthy relationships that are important for a child's feeding and healthy growth.
A recent double-blind study of infants in Australia found that adherence to preventive infant feeding guidelines led to normal weight gain and improved mutual understanding during feeding, as judged by the respondents. 36 More research is needed to better understand strategies for promoting healthy relationships that are important for a child's feeding and healthy growth.
Food preferences
Children who grow up in families where parents set an example of healthy eating behavior (for example, eat a diet rich in fruits and vegetables) develop similar food preferences. 4
Food preferences are also influenced by accompanying conditions. Children are more likely to avoid foods associated with unpleasant physical symptoms, such as nausea or pain. They may also avoid eating food associated with anxiety or distress caused by feeding disputes and confrontations.
Children also choose food based on qualities such as taste, texture, smell, temperature, or appearance, as well as environmental factors such as setting, presence of others, and perceived consequences of eating or not eating. For example, consequences of eating may include satiety, participation in a social function, or parental attention. Consequences of not eating can include things like extra play time, being the center of attention, or snacking instead of a normal meal.
For example, consequences of eating may include satiety, participation in a social function, or parental attention. Consequences of not eating can include things like extra play time, being the center of attention, or snacking instead of a normal meal.
The degree of familiarity with the taste of food increases the likelihood that the child will accept it. 37.38 Parents can make it easier to introduce new foods to their diet by regularly combining them with familiar foods until the food becomes familiar to the baby.
Conclusions
Eating habits are formed early in development in response to internal regulatory cues, parent-child relationships, dietary patterns, food offerings, and family patterns. Teaching children to eat fruits and vegetables early in their development develops a lifelong preference for these foods. It is necessary to conduct research on the factors that determine the context of the relationship between an adult and a child in a feeding situation, at an individual level, in an interaction situation and at the level of the external environment. The relationship between responsive/non-responsive feeding styles and children's feeding behavior in relation to weight gain should also be explored, and population-specific tools to measure responsive/non-responsive feeding characteristics should be developed. 24
The relationship between responsive/non-responsive feeding styles and children's feeding behavior in relation to weight gain should also be explored, and population-specific tools to measure responsive/non-responsive feeding characteristics should be developed. 24
Eating behavior in early childhood largely depends on parents and is developed through the acquisition of experience with food and its use. A system of education and support involving health professionals (i.e. health visitors, family doctors and pediatricians) and nutrition programs should be established so that parents always have the opportunity to seek help with their child's eating behavior.
Parents should combine their own meals with the feeding of the child in order to instill similar eating habits in him, and also to make the process of eating a pleasant experience for the child. Eating together allows children to watch their parents try new foods and helps them express feelings of hunger and satiety, as well as enjoyment of certain foods. 39
39
Parents control both the choice of food and the creation of a certain atmosphere in the process of feeding. Their "job" is to provide children with healthy food at fixed times and in pleasant surroundings. 39 By developing a certain diet, parents help children learn to consciously wait for the next meal. Children acquire the knowledge that the feeling of hunger will soon pass, and that they have no reason to be anxious or irritated. Children should not snack or eat throughout the day - this develops a sense of anticipation of a meal and the appearance of an appetite at a certain time. 39
Meals should be a pleasant family event, when all family members eat together and discuss the events of the day. When the duration of meals is shortened (less than 10 minutes), children may not have enough time to eat, especially during the period when they are learning to eat on their own, and the process of eating slows down. At the same time, it is difficult for a child to eat food that lasts more than 20 or 30 minutes, so such food can cause a feeling of disgust.
When feeding is accompanied by distractions like watching TV, family disputes, or other extraneous activities, it can be difficult for children to focus on food. Parents should separate meal times from play activities and avoid using toys, playing games, and not watching TV - all of these factors can distract the child from eating. Special equipment for children – high chairs, bibs and small utensils – encourages feeding and enables children to develop self-feeding skills.
Advice
Advice may be environmental, family or personal. In the environment, having healthy and tasty menus for young children at fast food restaurants can help avoid many of the problems associated with regularly eating high-fat foods (like french fries) instead of more nutritious foods like fruits and vegetables. Infant feeding recommendations should include the following information: information about the child's nutritional needs, methods to encourage healthy eating behaviors (including learning to recognize hunger or satiety signals and developing a specific type of interaction between parents and child during feeding), information on choosing the right time for about feeding, about ensuring regular feeding hours, about introducing new food into the diet through its modeling, data on ways to neutralize stressful and conflict situations during feeding. In terms of individual counseling, programs that help children develop healthy eating habits through nutrient-rich foods and develop the habit of eating to satisfy hunger rather than emotional needs can help prevent potential health and developmental problems. 40
In terms of individual counseling, programs that help children develop healthy eating habits through nutrient-rich foods and develop the habit of eating to satisfy hunger rather than emotional needs can help prevent potential health and developmental problems. 40
Literature
- Bosma J. Development and impairments of feeding in infancy and childhood. In: Groher M.E., ed. Dysphagia: Diagnosis and management . 3rd ed. Boston, MA: Butterworth-Heinemann; 1997:131-138.
- Morris SE. Development of oral motor skills in the neurologically impaired child receiving non-oral feedings Dysphagia 1989;3:135-154.
- Arimond M, Ruel MT. Dietary diversity is associated with child nutritional status: Evidence from 11 demographic and health surveys. The Journal of Nutrition 2004;134:2579-2585.
- Skinner JD, Carruth BR, Bounds W, Ziegler P, Reidy K. Do food-related experiences in the first 2 years of life predictary dietary variety in school-aged children? Journal of Nutrition Education and Behavior 2002;34(6):310-315.

- Schwartz C, Scholtens PA, Lalanne A, Weenen H, Nicklaus S. Development of healthy eating habits early in life. Review of recent evidence and selected guidelines. Appetite . 2011;57(3):796-807.
- Mennella JA, Nicklaus S, Jagolino AL, Yourshaw LM. Variety is the spice of life: strategies for promoting fruit and vegetable acceptance during infancy. Physiol Behav . 2008;22;94(1):29-38.
- Linscheid TR, Budd KS, Rasnake LK. Pediatric feeding disorders. In: Roberts MC, ed. Handbook of pediatric psychology . New York, NY: Guilford Press; 2003:481-498.
- Birch LL, McPhee L, Shoba BC, Pirok E, Steinberg L. What kind of exposure reduces children's food neophobia? Looking vs. tasting. Appetite 1987;9(3):171-178.
- Keren M, Feldman R, Tyano S. Diagnoses and interactive patterns of infants referred to a community-based infant mental health clinic. Journal of the American Academy of Child & Adolescent Psychiatry 2001;40(1):27-35.

- Palfreyman Z, Haycraft E, Meyer C. Development of the Parental Modeling of Eating Behaviours Scale (PARM): links with food intake among children and their mothers. Maternal and Child Nutrition . 2012 [Epub ahead of print].
- Zoumas-Morse C, Rock CL, Sobo EJ, Neuhouser ML. Children's patterns of macronutrient and intake associations with restaurant and home eating. Journal of the American Dietetic Association 2001;101(8):923-925.
- Smith MM, Lifshitz F. Excess fruit juice consumption as a contributing factor in nonorganic failure to thrive. Pediatrics 1994;93(3):438-443.
- Ponza M, Devaney B, Ziegler P, Reidy K, Squatrito C. Nutrient intakes and food choices of infants and toddlers participating in WIC. Journal of the American Dietetic Association 2004;104(1 Suppl 1):71-79.
- Devaney B, Kalb L, Briefel R, Zavitsky-Novak T, Clusen N, Ziegler P. Feeding infants and toddlers study: overview of the study design.
 Journal of the American Dietetic Association 2004;104(1 Suppl 1):8-13.
Journal of the American Dietetic Association 2004;104(1 Suppl 1):8-13. - Picciano MF, Smiciklas-Wright H, Birch LL, Mitchell DC, Murray-Kolb L, McConahy KL. Nutritional guidance is needed during the dietary transition in early childhood. Pediatrics 2000;106(1):109-114.
- Cullen KW, Ash DM, Warneke C, de Moor C. Intake of soft drinks, fruit-flavored beverages, and fruits and vegetables by children in grades 4 through 6. American Journal of Public Health 2002;92(9): 1475-1477.
- Brotanek JM, Gosz J, Weitzman M, Flores G. Secular trends in the prevalence of iron deficiency among US toddlers, 1976-2002. Archives of Pediatrics & Adolescent Medicine 2008;162:374-81.
- Ainsworth MDS, Blehar MC, Waters E, Wall S. Patterns of attachment: A psychological study of the strange situation . New York: Psychology Press, 1978.
- Rhee K. Childhood overweight and the relationship between parent behaviors, parenting style, and family functioning.
 The Annals of the American Academy of Political and Social Science 2008;615:11–37.
The Annals of the American Academy of Political and Social Science 2008;615:11–37. - Baumrind D. Rearing competent children In: Damon W, ed. Child development today and tomorrow. San-Francisco, CA: Jossey-Bass Publishers; 1989:349-378.
- Maccoby EE, Martin J. Socialization in the context of the family: parent-child interaction. In: Hetherington EM, ed. Handbook of child psychology: Socialization, personality, and social development. Vol 4 . New York, NY: John Wiley; 1983:1-101.
- Black MM & Aboud FE. Responsive feeding is embedded in a theoretical framework of responsive parenting. Journal of Nutrition 2011;141(3):490-4.
- Hughes SO, Power TG, Fisher JO, Mueller S, Nicklas TA. Revisiting a neglected construct: Parenting styles in a child-feeding context. Appetite 2005;44(1):83-92.
- Hurley KM, Cross MB, Hughes SO. A systematic review of responsive feeding and child obesity in high-income countries.
 Journal of Nutrition 2011;141:495-501.
Journal of Nutrition 2011;141:495-501. - Leyendecker B, Lamb ME, Scholmerich A, Fricke DM. Context as moderators of observed interactions: A study of Costa Rican mothers and infants from differing socioeconomic backgrounds. International Journal of Behavioral Development 1997;21(1):15-24.
- Kivijarvi M, Voeten MJM, Niemela P, Raiha H, Lertola K, Piha J. Maternal sensitivity behavior and infant behavior in early interaction. Infant Mental Health Journal 2001;22(6):627-640.
- Beebe B, Lachman F. Infant research and adult treatment: Co-constructing interactions . Hillsdale, NJ: The Analytic Press; 2002.
- Birch LL, Fisher JO. Mothers' child-feeding practices influence daughters' eating and weight. American Journal of Clinical Nutrition 2000;71(5):1054-1061
- Birch LL, Johnson SL, Andresen G, Peters JC, Schulte MC. The variability of young children's energy intake. New England Journal of Medicine 1991;324(4):232-235.

- Birch LL. Development of food preferences. Annual Review of Nutrition 1999;19:41-62.
- Egeland B, Sroufe LA. attachment and early maltreatment. Child Development 1981;52(1):44-52.
- DiSantis KI, Hodges EA, Johnson SL, Fisher JO. The role of responsive feeding in overweight during infancy and toddlerhood: a systematic review. International Journal of Obesity 2011;35:480-92.
- Faith MS, Scanlon KS, Birch LL, Francis LA, Sherry B. Parent-child feeding strategies and their relationships to child eating and weight status. Obesity Research 2004;12(11):1711-1722.
- Birch LL, Fisher JO, Davison KK. Learning to overeat: maternal use of restrictive feeding practices promotes girls' eating in the absence of hunger. American Journal of Clinical Nutrition 2003;78(2):215-220.
- Fisher JO, Mitchell DC, Smiciklas-Wright H, Birch LL. Parental influences on young girls' fruit and vegetable, micronutrient, and fat intakes.