Baby feeding teats
Cleft Lip & Palate Association
For babies unable to suck from standard bottles and teats, there are a number of options available. As each baby and their needs will differ, it is vital that you speak to your Cleft Nurse Specialist before purchasing or using any specialist feeding equipment.
While CLAPA does supply specialist bottles and teats, our staff are not medically trained and cannot give advice as to which items would be suitable for your baby.
Jump To:
- Welcome Packs
- MAM Bottles & Teats
- Dr. Brown’s
- Alternative Soft Bottles
- Haberman Feeder
Welcome Packs
CLAPA provides one free ‘Welcome Pack’ of bottles, teats and information for new parents in the UK. The Specialist Cleft Nurses will tell families about this service after meeting with them and assessing their baby’s feeding needs. They will advise families which bottles and teats they need. CLAPA Staff cannot give feeding advice or recommend particular bottles and teats.
Welcome Packs contain:
- Special bottles and teats – either two MAM 8oz soft bottles and two MAM teats OR two Dr Brown’s bottles (one large, one small) and four Dr Brown’s teats
- Medical information on caring for and feeding a baby with a cleft
- Copy of CLAPA News, our annual magazine
- ‘Join the CLAPA Community’ leaflet
- ‘One in 700’ leaflet about CLAPA and cleft
- ‘Callie and her Cleft’ picture book about cleft lip and palate (please let us know if you’d like this included)
- Feeding equipment catalogue
- Information from the Family Fund and the Cleft Collective
- Relevant leaflets or postcards about upcoming CLAPA events such as Awareness Week
Request your Welcome Pack
We need to know what kind of bottles and teats you need, your name, address and phone number. You can order extra bottles and teats at the same time and the postage will be free, but you will need a bank card to pay for the extra items. Prices can be found in our online shop.
You can order extra bottles and teats at the same time and the postage will be free, but you will need a bank card to pay for the extra items. Prices can be found in our online shop.
Please note, we can only supply one Welcome Pack per baby. If you are having serious issues paying for further feeding equipment, you can ask your Cleft Nurse Specialist to contact us on your behalf and we will send free-of-charge items at our discretion.
Due to our limited funding, we cannot supply free samples (e.g. to Health Visitors, students, etc). If you would like a pack for demonstration purposes, we ask that you make a donation of £20 to help us cover our costs.
Charlotte is being fed with a MAM soft bottle and orthodontic teatMAM Bottles and TeatsCLAPA is the only UK supplier of MAM’s range of specialist cleft feeding equipment, including their soft bottles and orthodontic teats. The soft bottles can be gently squeezed to help the milk flow regardless of the baby’s ability to suck.
Before using this bottle, parents and carers should be instructed in its safe use by a trained feeding specialist. This will reduce the risk of the baby aspirating or choking during feeds.
MAM teats have a small dimple in the side which may or may not have a slit in it. This is what is meant by the teats being either vented or non-vented. The slit helps to eliminate extra air.
Vented teats are either newborn or all ages sized. This isn’t necessarily to do with the age of your child, so it’s best to go with what the Cleft Nurse Specialist recommends.
Care Instructions
MAM Bottles
MAM Soft Bottles have a standard-sized neck which can be used with most teats.
They are BPA-free and comply with all international regulations and standards for baby feeding equipment.
They can be cleaned/sterilised by any normal method used in the home, including:
- All common dishwashing liquids
- Dishwasher (top rack only) 95 degrees C.
 It may discolour if strong food colourings are also in the washer.
It may discolour if strong food colourings are also in the washer. - Domestic steam or microwave steriliser, 100 degrees C MAX
- Boiling water for 5-10 minutes
- Cold water sterilisation (e.g. Milton fluid) – this is the recommended method as it may help your bottles to last longer.
MAM Teats
MAM teats come in three varieties: Non-Vented All Ages, Vented Newborn, and Vented All Ages. These teats are all considered ‘medium flow’. All teats have a small ‘dimple’ in the side, and in Vented teats there is a small slit in this dimple to help with the elimination of extra air during feeding. If you’re using vented teats, make sure to keep the vent on the top as these teats will badly leak otherwise. The difference between newborn and all ages sizes can be seen above.
MAM Teats are made of soft latex and will naturally swell up with use, as seen in the image below. They should be replaced at least every 4-6 weeks.
Using them for longer than this can lead to problems. Your baby may become used to the swollen size of the teats and find it difficult to use new teats, as they are not available in larger sizes. It can also be dangerous, as small tears will start to form in the delicate latex and make these teats harder to properly sterilise.
MAM recommends cold water sterilisation be used (e.g. Milton fluid, which is widely available) as this can help the teats to retain their shape for longer.
MAM Vented All Ages Teats brand new (left) and after 6 weeks of use (right).Direct sunlight or edible fats make latex age and become porous more quickly. When a latex teat becomes sticky, it is a natural sign that it should be replaced with a new one, usually after 1-2 months.
Dr. Brown’sThe Dr. Brown’s Specialty Feeding System was designed together with health professionals to help babies with feeding issues like those that often occur with a cleft lip and/or palate.
The system uses a special valve which babies can ‘work at’ with their tongues like they would when breastfeeding or using a regular bottle, but they don’t have to suck to get the milk to flow. This means that the person feeding the baby doesn’t have to squeeze the bottles, so they need much less training than with MAM bottles.
With this system, the baby is ‘feeding themselves’ as they control the flow of milk, so it teaches babies to self-regulate.
This system doesn’t work for everyone, however, so please do check with your Cleft Nurse Specialist before ordering.
Visit the Dr Browns website for more information about their Speciality Feeding System, including care instructions.
Cleaning Dr Browns bottles and preparing teats for first use.
Selecting the correct teat size.
Why Are My Dr. Brown Bottles Leaking? (Causes & Solutions)
How to sterilize your Dr Browns Bottles bottles
Note: If searching online or elsewhere for “Dr. Brown’s Bottles” be aware that Infant Paced Feeding Valves are only included with “Dr. Brown’s Specialty Feeding System bottles” and are not included with any other type of Dr. Brown’s bottle such as “Options” or “Anti-Colic” bottles
Brown’s Bottles” be aware that Infant Paced Feeding Valves are only included with “Dr. Brown’s Specialty Feeding System bottles” and are not included with any other type of Dr. Brown’s bottle such as “Options” or “Anti-Colic” bottles
The manufacturer does not supply spare valves so Clapa is also unable to supply them.
Note: If the markings on the side of your bottles are coming off, please contact our suppliers, Central Medical Supplies (CMS), directly on 0153 839 9541
Why is the ink coming off my bottles?
Note: Bottles should not be handled/ scrubbed (outside surface) or wiped with a cloth until they have fully cooled down (if using steam or microwave to sterilize) as it will lead to the ink coming off the bottles. With excessive sterilization and/or rough scrubbing of the exterior of the bottle, the ink on some Dr Brown’s bottles may peel or fade over time.
To prevent further issues, avoid over-sterilizing the bottle vessel for example leaving your bottle in a cold-water solution over night or all day, and do not aggressively wash the exterior.
CLAPA’s Stock
We are currently only able to get our stock of Dr Browns products through a third party at a significant cost. Because of how the bottle packs are packaged, we can’t control or alter their contents, we can only sell them as-is. We know this isn’t ideal for some parents, particularly those who use larger teats and need to buy these separately, and for this we sincerely apologise. Large bottle packs were originally supplied to us with Level 3 & 4 teats, but this has since changed, a decision that was beyond our control.
At present, the sealed bottle packs are the only financially viable way for CLAPA to supply Dr Browns products to parents in the UK, as the cost of stocking individual bottles is too high. We hope this will change in the future so we can provide parents with a more flexible service that suits their needs.
The bottles and teats provided for our Welcome Packs are generously donated by The Handi-Craft Company in the USA, and cannot be sold separately.
Alternative Soft Bottles
There are a number of alternative soft bottles available on the internet or high street. Brands include Vital and Nuby bottles. However, these are not designed specifically for babies with a cleft, so parents should always consult with their Cleft Nurse Specialists before purchasing or using any of these.
Some parents prefer these to the MAM bottles as they may be softer and easier to squeeze. While this can be a relief to parents struggling to keep squeezing the MAM bottles, it can also be dangerous, as too much milk squeezed into the baby’s mouth can cause them to choke, or ‘aspirate’. This is why it’s vital that parents are properly trained and follow all advice from their Cleft Nurse Specialist.
NUK Teats
NUK teats are very large, flat-headed teats which have been specially designed for babies with a cleft palate. However, the size and shape of the teat can make it dangerous to use for parents who have not been trained to use them, so again they should only be used if the Cleft Nurse Specialist has advised this.
Haberman Feeder
The Haberman Feeder is a specialised bottle that was designed by a mother of a child that was born with Pierre Robin. It is designed to help any baby that has a weak sucking reflex. It is much more expensive than other bottles but has been very successful for some babies.
These should be purchased directly from Athrodax Healthcare.
UK parents can get a reduced rate for this bottle as they can claim back the VAT. This exemption is because ‘your baby has a feeding difficulty’ and therefore this type of bottle has zero tax. On receipt of an order form, cheque and VAT form, Athrodax aim to send your order by return post. Credit card orders can be taken but they will be subject to VAT.
We hold a small emergency stock of complete Haberman bottles but we do not stock the replacement valves and teats, these will have to be purchased from Athrodax Healthcare at:
Athrodax Healthcare International Ltd
Hawthorne Business Park
Drybrook
Gloucestershire
GL17 9HP
Tel: 01594 544440
Minbie - award winning baby bottle nipples – Minbie US
PPSU Bottles Nipples Sterilizer & Dryer Breast PumpsWhy you need the Complete Package
1.
 avoid nipple confusion
avoid nipple confusionour award winning nipple encourages your baby to practice a proper latch and work for each feed using their instinctive breastfeeding technique, protecting your bond.
2. the freedom to pump & store
portable, comfortable pumping that mimics the breastfeeding experience gives you the freedom to pump on the go and hand over whilst protecting your breastfeeding relationship.
4. keep your baby healthy
time saving sterilization protects your whole family from harmful bacteria and viruses at the press of a button.
3. ‘me time’ for mum
secure the quiet moments you need and the relaxation you deserve whilst others safely feed your baby without risk to your breastfeeding bond.
Why you need the Complete Package
1. avoid nipple confusion+
2. the freedom to pump & store+
5. Keep your baby healthy+
4. ‘me time’ for mum+
Breast Pump & Bottle Bundle
$250. 00
00
PPSU 3 Month Kit
$20.90
Sterilizer & Dryer
$89.90
Save $7.90
ppsu 0-6 month bundle
$39.90
Breast Pump & Bottle Bundle
$250.00
PPSU 3 Month Kit
$20.90
Sterilizer & Dryer
$89.90
Save $7.90
ppsu 0-6 month bundle
$39.90
OUR MISSION
WE ARE HERE TO EMPOWER MOMS DURING THEIR BREASTFEEDING JOURNEY BY PROVIDING PRODUCTS THAT NURTURE AND PROTECT THAT INSTINCTIVE, SPECIAL BOND
read our story
functionally designed like nature intended
- - smart contours train baby to latch perfectly to the breast
- - protects your breastfeeding bond from nipple confusion
- - anti-colic vent floats air away from your baby's stomach
revolutionary nipple design
revolutionary nipple design
minbie
other nipples
Nurtures instinctive breastfeeding latch
-
Trains breastfeeding muscle-memory
-
prevents nipple confusion
-
Prevents lazy feeding
-
Supports good digestion
-
Anti reflux & colic
-
Gentle on palate & gums
-
SHOP BY AGE
months
NEWBORN RANGE
months
3+ MONTHS
months
6+ MONTHS
months
9+ MONTHS
SHOP BY AGE
months
NEWBORN RANGE
months
3+ MONTHS
months
6+ MONTHS
months
9+ MONTHS
READY SETS GO!
bundle them up and save + FREE shipping over $39. 90.
90.
shop all
clearly better
Premium PPSU Bottle
a higher heat resistance than regular bottles makes new PPSU the safest, most durable bottle you’ll find. our hypoallergenic nipples are made of premium-quality soft silicone. australian designed & owned.
shop all
-
Featured article
Everything you need to know about Baby Colic
read our story
HUMBLE BRAG
300k
parents and counting choose minbie
12k+
bottles and teats donated
15k+
five star reviews
follow us @minbie
Breastfeeding with pierced, flat or inverted nipples
The shape and size of nipples can vary greatly from woman to woman.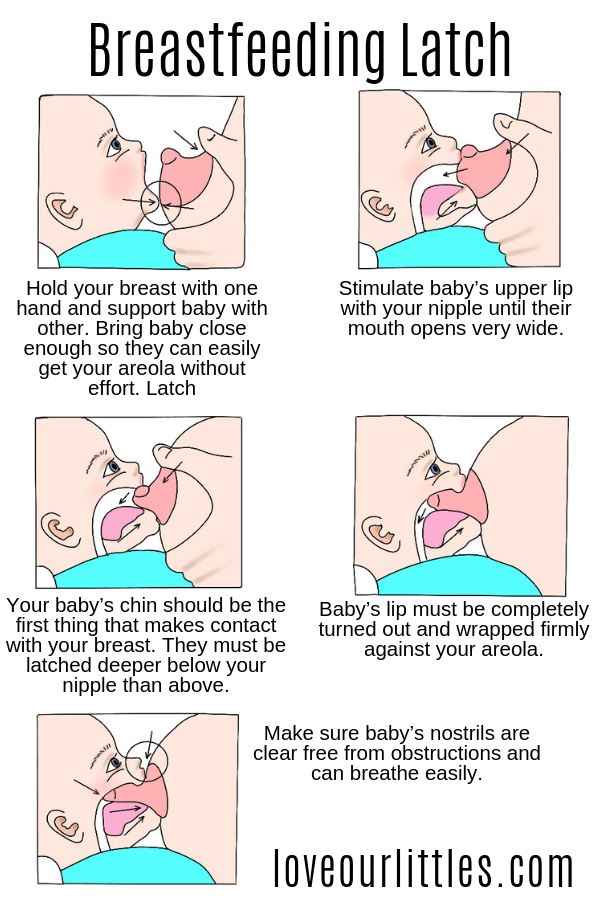 Our practical tips will help you make breastfeeding easier, no matter what your nipples are.
Our practical tips will help you make breastfeeding easier, no matter what your nipples are.
Share this information
Most women's nipples protrude, enlarge and swell when touched, but some have flat or even inward nipples. In addition, some women pierce one or both nipples. Usually flat, inverted or pierced nipples do not cause problems when breastfeeding, but in some cases additional help may be needed.
“Don't panic if you have flat or inverted nipples. As a rule, this does not interfere with breastfeeding in any way,” says Shawnad Hilton, a lactation consultant, health visitor and newborn care specialist who has worked with Medela in the UK for more than a decade. “Remember that your baby takes into his mouth not only the nipple, but also part of the breast.”
However, in the early days, when the baby's mouth is still very small and suckling skills have not developed, inverted or flat nipples can make feeding difficult, especially if the baby is unwell or born prematurely.
“Flat or inverted nipples may not reach the baby's palate and therefore not trigger the sucking reflex,” Schoned explains. “That is, the baby may have trouble grasping and holding the breast in the mouth, and the baby will not get enough milk.”
How to tell if you have flat or inverted nipples
Flat nipples 1 do not protrude much from the areola (the darker
area surrounding the nipple) even when stimulated.
Inverted nipples seem to be recessed in the center. They may look like this all the time or only if they are stimulated. Sometimes inverted nipples are on the same level with the areola, and sometimes even sink deep into the breast tissue.
This feature may occur on one or both nipples. It is estimated that approximately 10% of nulliparous women have at least one retracted nipple. 2 If you're not sure what type of nipples you have, try a simple pinch test: Gently squeeze your breast with your thumb and forefinger on both sides of the areola. The nipple should come forward. If your nipple hides inside, creating a depression, then it is retracted.
The nipple should come forward. If your nipple hides inside, creating a depression, then it is retracted.
Preparing inverted and flat nipples during pregnancy
You may have noticed that during pregnancy your breasts have changed and your nipples have become more protruding. If this does not happen and you are worried that the shape of your nipples will make breastfeeding difficult, try using nipple formers* in consultation with your doctor. These are soft and flexible silicone discs that are discreetly placed in the bra and slightly squeeze the nipples, helping to pull them out.
“In a normal pregnancy, nipple formers can be worn from 32 weeks,” advises Schoned. - Start wearing them for an hour a day, gradually increasing the time to eight hours. If you have an incompetent (weakened) cervix or are at risk of preterm labor, check with your healthcare provider about when you can start using shapers, as nipple stimulation can trigger contractions.”
“Nipple formers can continue to be worn after childbirth,” adds Schoned. “Try to put them in a bra 30 to 60 minutes before feeding.”
“Try to put them in a bra 30 to 60 minutes before feeding.”
“I have inverted nipples, and after two or three weeks of constantly trying to latch on, I almost switched to formula,” recalls Nina, a mother from Germany. “I turned to La Leche Liga for help, and one nice woman came to me and supported me to continue to feed. She suggested trying nipple shapers and they really helped me. Somehow my baby began to understand what to do! Breastfeeding went well and I nursed him until he was 21 months old.”
How to help your baby latch on to flat or inverted nipples
If your baby enjoys sucking on your thumb but isn't as interested in your breast, chances are your nipple isn't reaching the palate. The baby may become nervous, push off the breast and cry or even fall asleep on your chest. If this happens, ask a lactation consultant or healthcare professional to check the grip.
There are several tricks you can use before every feed to make your nipples more comfortable to latch on to. Schoned recommends the following:
Schoned recommends the following:
- twist the nipple between thumb and forefinger so that it protrudes better;
- place fingers in a "V" or "C" shape and squeeze the breast just behind the areola to push out the nipple;
- apply a cold compress or ice cube to the nipple to push it forward;
- Express milk manually or with a breast pump for a couple of minutes before feeding so that the nipple comes out more.
“I had a flat nipple, but I only found out about it when I noticed Austin was having trouble suckling on that side,” says Jennifer, mother of two in the UK. “From an anatomical point of view, there is nothing abnormal in this, it’s just that my nipple does not protrude so much, and this requires some skill when feeding. Before giving this breast, I always pinched and squeezed the nipple a little and tried to put it into the baby's mouth. It was a little difficult at first, but over time I learned.”
Using nursing pads
If none of the above work and your baby still has difficulty latch-on, your lactation consultant or healthcare professional may recommend that you breastfeed with a nursing pad*. They are thin and flexible nipple-shaped silicone funnels with holes at the tip through which milk will flow.
They are thin and flexible nipple-shaped silicone funnels with holes at the tip through which milk will flow.
It is easier for the baby to put the feeding pad in his mouth, as it is larger and more rigid. In addition, such an overlay will reach him to the sky, causing a sucking reflex. Do not use nursing pads for a long time. If you experience pain or other problems, contact your lactation consultant or healthcare professional to check that your baby is latching on properly with a breastfeeding pad. You will also need to monitor your baby's weight gain to ensure that milk production is meeting his needs. 3
Over time, as your baby learns to suckle properly and your nipples get used to breastfeeding, you will be able to breastfeed without breast pads.
“My nipples are rather flat. The doctor advised me nursing pads, and I was successfully able to feed my two babies,” says Ann-Sophie, mother of two from Sweden. “My secret is to make them adhere better to the skin, I lightly wet the edges before use. ”
”
Breastfeeding with pierced nipples
Many women with pierced nipples find it does not affect their ability to breastfeed. However, jewelry must be removed before feeding, as the child may choke on them or injure their tongue, gums or palate.
“I had a nipple piercing, but I got it off a year later when I got pregnant because my breasts were very sensitive,” says Kelly, mother of three from the UK. “I breastfed my daughter exclusively, and then her two younger brothers, and never had any problems. And the pierced nipple was my favorite!”
Some women report that milk can leak from piercings, while others believe that piercing scars reduce milk production 4 - but this has not been well researched.
“You can't predict how a piercing will affect breastfeeding until milk production begins,” Schoned explains. - If you are concerned, talk to a lactation consultant or healthcare professional. And remember that one breast may be enough for babies to get the nutrition they need if there are problems with the second. ”
”
What to do if you can't breastfeed with flat or inverted nipples
If you've tried all the options and still can't breastfeed, you still shouldn't deprive your baby of breastmilk.
“Mom and baby's health is the most important thing,” says Schoned. “Maybe you should switch to full pumping and feed your baby only expressed milk. You can also try the supplementary feeding system** where the baby continues to feed at the breast while receiving additional expressed milk through a tube. That is, the baby will still suck on the breast and stimulate the production of milk, which, in turn, will help you pump even more.
“I have inverted nipples. After the disastrous experience of breastfeeding my first son with my second, I decided to get my way after all,” says Babettli, mother-of-two from Italy. - On the advice of experts, I tried nipple formers and nursing pads, but everything was unsuccessful. In the end, pumping with the Medela Symphony*** Double Electronic Clinical Breast Pump proved to be the best solution for us. I fed exclusively on expressed milk for up to four months.”
I fed exclusively on expressed milk for up to four months.”
Care for different types of nipples
Flat or inverted nipples may require extra care as the baby may squeeze them harder and they may become inflamed at first. Tips on how to care for sore nipples can be found in Nursing Nipple Care.
If your nipples become inverted after a feed, any moisture can lead to inflammation and increase the risk of infections, including thrush. Blot your nipples dry after each feed before they have time to hide inside.
With swelling of the mammary glands, when even protruding nipples can become flat, flat or inverted nipples can be difficult. Read the helpful tips in the article on breast swelling.
The good news is that continuous breastfeeding or pumping can change the shape of your nipples and breastfeeding will become easier over time. With the arrival of the next child, you may not have to face this problem at all, as happened with Leanne, a mother of two from the UK.
“The second feeding was like a fairy tale,” she says. “After almost four months of pumping for my first son, my flat nipples were so extended that with my second son I no longer had to use breast pads - he was able to suck directly from the breast. The youngest is now nine months old and I still breastfeed him.”
Literature
1 Pluchinotta AM. The Outpatient Breast Clinic. Springer International Publishing ; 2015. - Pluchinotta A.M., "Treatment of breast diseases on an outpatient basis". Springer International Publishing. 2015.
2 Alexander JM, Campbell MJ. Prevalence of inverted and non-protractile nipples in antenatal women who intend to breast-feed. The Breast . 1997;6(2):72-78. — Alexander JM, Campbell MJ, "Prevalence of inverted and intractable nipples in pregnant women who intend to breastfeed." Ze Brest (Chest). 1997;6(2):72-78.
3 McKechnie AC, Eglash A. Nipple shields: a review of the literature.Breastfeeding Medicine. 2010;5(6):309-314. — McKechnie A.S., Eglash A., "Nipple Covers: A Review of the Literature". Brestfeeding Medicine (Breastfeeding Medicine). 2010;5(6):309-314.
Nipple shields: a review of the literature.Breastfeeding Medicine. 2010;5(6):309-314. — McKechnie A.S., Eglash A., "Nipple Covers: A Review of the Literature". Brestfeeding Medicine (Breastfeeding Medicine). 2010;5(6):309-314.
4 Garbin CP0106 , Rowan MK , Hartmann PE , Geddes DT . Association of nipple piercing with abnormal milk production and breastfeeding. JAMA, Journal of the American Medical Association. 2009;301(24):2550-2551. - Garbin S.P., Deacon J.P., Rowan M.C., Hartmann P.I., Geddes D.T., "Nipple piercing and its impact on abnormal milk production and breastfeeding", JAMA (Journal of the American medical association). 2009;301(24):2550-2551.
Read instructions before use. Consult a specialist about possible contraindications.

* RC No. FSZ 2010/07352 dated 07/19/10
** RC No. FSZ 2010/07353 dated 07/19/10
*** RC No. FSZ 2010/06525 dated 17/03/2021 nursing mothers | Breast Care
Breastfeeding is good for you and your baby, but it can be a real challenge for the nipples. Check out our tips and tricks to help reduce the pain.
Share this information
Sioned Hilton, health visitor, neonatal nurse and lactation consultant:
A mother of three, Sioned Hilton has been supporting families with newborns and young children for over 30 years. She provides advice on breastfeeding and pumping, both in clinics and at home. In addition, Schoned writes articles for parenting magazines, attends conferences, and conducts seminars for attending physicians.
New mothers often hear: "Breastfeeding doesn't have to be painful." However, in the early days, many are faced with the opposite.
In most women during pregnancy, the nipples enlarge and become more sensitive. When a newborn baby begins to suckle, it creates a certain pressure, and this is a completely new and unfamiliar sensation for a woman (at least for a first-time mother).
When a newborn baby begins to suckle, it creates a certain pressure, and this is a completely new and unfamiliar sensation for a woman (at least for a first-time mother).
Feedings can be prolonged for a long time, sometimes up to an hour, and the child may ask to be breastfed up to 13 times a day. 1 This sucking, pressure and saliva of the baby can cause sore nipples.
Remember how your lips crack in the wind and sun. The more often you lick them, the more they will dry and become inflamed. Therefore, lips require good hydration to soften, protect and speed up the healing of cracks. The same thing happens with nipples.
However, sore nipples usually don't last more than a couple of weeks and go away as your baby and your breasts get used to breastfeeding. It is important to start nipple care as early as possible to prevent the situation from worsening. Therefore, if your nipples become very inflamed, crack or bleed, contact your doctor as soon as possible. 2
Prevention is better than cure, so check out our tips.
Check your baby's latch on
Correct latch is the key to pain-free breastfeeding. When putting the baby to the breast, point the nipple towards his palate. This will allow him to grab the nipple and the part of the areola (the darker skin around the nipple) underneath. When the nipple and part of the breast is in the baby's mouth, feeding is taking place correctly. 3
For the first few days, see a lactation consultant or specialist to check for proper latch. He will be able to give you advice on how to solve problems and recommend other feeding positions that will make it less painful for you to feed your baby.
Check tongue frenulum
Tongue frenulum (ankyloglossia) occurs in 4-11% of
newborns. 4 At the same time, the strip of skin that attaches the tongue to the bottom of the mouth - the so-called frenulum - is too short. A child with a shortened frenulum will not be able to open his mouth wide enough to latch onto the breast well, and his tongue will not cover the lower gum when sucking. As a result, the baby will be nervous, and your nipples may become inflamed.
As a result, the baby will be nervous, and your nipples may become inflamed.
The doctor or lactation consultant must examine the baby to make this diagnosis. The problem of a shortened bridle is solved by a simple undercutting procedure. It is performed by a doctor, and is usually done without blood and does not require anesthesia. Cutting the bridle allows you to restore the normal feeding mechanism almost instantly. 5
Less common in children is a short frenulum of the upper lip. In this case, it is necessary to dissect the skin that connects the upper lip to the gum. A shortened frenum of the tongue or upper lip in a newborn is not always detected during the examination conducted immediately after birth, so if you think that this is what is causing your nipples pain, seek medical advice as soon as possible. 4
Breastfeeding tips for nipples
- Wash your breasts with water only when you shower or bathe. Small bumps on the areola (Montgomery's glands) secrete oil that moisturizes and protects your nipples.
 Soaps and shower gels can strip away this natural defense, causing dryness and irritation. 6
Soaps and shower gels can strip away this natural defense, causing dryness and irritation. 6 - Pat the nipples gently with a soft towel or simply let them air dry. In the past, women were often advised to rub their nipples to make them stiffer, but thankfully, such advice is a thing of the past!
- Do not wash breasts or nipples before feeding. The bacteria found on the surface of the breast actually help the baby's intestinal microflora to develop. 7
- Fresh breast milk helps to heal cracked nipples, 8 so rub a few drops of milk into them before and after feeding.
- Change your bra pads often if they get wet. This will reduce the risk of bacterial and fungal infections, including thrush. 6
- It is not necessary to increase the intervals between feedings to give the nipples a "rest". For a baby to be healthy and grow well, it needs to be fed on demand. Remember, frequent feeding stimulates and maintains milk production, so keep feeding despite the pain.
 9
9
Healthy teat care products
- Pure lanolin teat cleaner, a natural product derived from sheep's wool. It moisturizes and promotes healing of the nipples. This cream is safe for the baby, so it does not need to be washed off before feeding.
- Hydrogel Pads* can be applied to sore nipples to relieve pain while feeding and help promote healing. They can even be stored in the refrigerator to enhance the soothing cooling effect.
- Breast pads* fit inside a bra. They help prevent nipple irritation from clothing and have air holes to help nipples heal.
- Nursing Bras** are made from breathable material such as cotton or a special fabric that dries quickly and wicks moisture away from sore nipples.
- Nursing pads* are special silicone pads that are worn over the nipples. They have small holes through which milk flows when you are breastfeeding. The pads help to protect the skin underneath and help the baby to better latch on to the nipple by making the nipple stiffer.
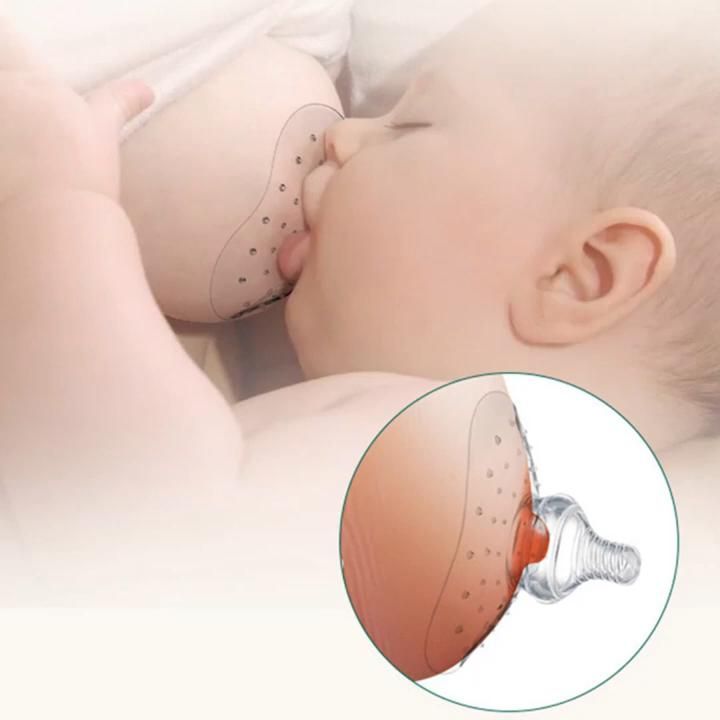 Do not use nursing pads for a long time. If you have problems or pain, contact your healthcare professional or lactation consultant.
Do not use nursing pads for a long time. If you have problems or pain, contact your healthcare professional or lactation consultant.
When to Seek Medical Care
The soreness should go away as your nipples and baby get used to breastfeeding. It is worth repeating that the main cause of sore nipples is improper grip. If your lactation consultant has not been able to resolve your pain while feeding, see another specialist and a third if necessary.
If nipple pain persists or if you notice unusual symptoms, talk to your doctor. The appearance of white spots or flakes on the nipples may be a sign of thrush, whitish or bluish nipples may indicate a circulation disorder such as Raynaud's disease (vasospasm), and pus and redness indicate an infection. 2
Literature
1 Kent JC et al. Volume and frequency of breastfeedings and fat content of breast milk throughout the day. Pediatrics. 2006;117(3): e 387-395. - Kent J.S. et al., "Amount and frequency of breastfeeding and fat content of breast milk during the day." Pediatrix (Pediatrics). 2006;117(3):e387-95.
- Kent J.S. et al., "Amount and frequency of breastfeeding and fat content of breast milk during the day." Pediatrix (Pediatrics). 2006;117(3):e387-95.
2 Berens P et al. Academy of Breastfeeding Medicine. ABM Clinical Protocol#26: Persistent pain with breastfeeding. Breastfeeding Medicine. 2016;11(2):46-53. - Behrens, P. et al., Academy of Breastfeeding Medicine, AVM Clinical Protocol #26: Persistence of Breastfeeding Pain. Brestfeed Med (Breastfeeding Medicine). 2016;11(2):46-53.
3 Cadwell K. Latching - On and Suckling of the Healthy Term Neonate: Breastfeeding Assessment. J Midwifery & Women's Health. 2007;52(6):638-42. — Cadwell, K., "Latching and sucking in healthy newborns: evaluation of breastfeeding." F Midwifery Women Health. 2007;52(6):638-642.
4 Segal LM et al. Prevalence, diagnosis, and treatment of ankyloglossia: methodological review. Canadian Family Physician. 2007;53(6):1027-1033. - Segal L.M. et al., Incidence, Diagnosis, and Treatment of Ankyloglossia: A Methodological Review. Canadian Family Physic. 2007;53(6):1027-1033.
Canadian Family Physician. 2007;53(6):1027-1033. - Segal L.M. et al., Incidence, Diagnosis, and Treatment of Ankyloglossia: A Methodological Review. Canadian Family Physic. 2007;53(6):1027-1033.
5 O'Shea JE et al. Frenotomy for tongue - tie in newborn infants. The Cochrane Library. 2017. - O'Shea J.I. et al., "Dissection of the frenulum in the newborn", The Cochrane Labrery (Cochrane Library), 2017.
6 Jacobs A et al. S3-guidelines for the treatment of inflammatory breast disease during the lactation period. Geburtshilfe und Frauenheilkunde. 2013;73(12):1202-1208. - Jacobs A. et al., "Recommendations S -3 for the treatment of inflammatory diseases of the breast during breastfeeding. Geburtskhilfe und Frauenheilkünde. milk bacterial communities and establishment and development of the infant gut microbiome JAMA pediatrics 2017;171(7):647-654 - P. S. Pannaraj et al., "Bacterial communities in breast milk and their association with the occurrence and development of the neonatal gut microbiome." JAMA pediatric. 2017;171(7):647-654.
S. Pannaraj et al., "Bacterial communities in breast milk and their association with the occurrence and development of the neonatal gut microbiome." JAMA pediatric. 2017;171(7):647-654.
8 Mohammadzadeh A et al. The effect of breast milk and lanolin on sore nipples. Saudi medical journal. 2005;26(8):1231-1234. — Mohammedzade A. et al., "Effects of breast milk and lanolin on sore nipples." Saudi Medical Journal. 2005;26(8):1231-1234.
9 Kent JC et al. Principles for maintaining or increasing breast milk production. J Obstet , Gynecol , & Neonatal Nurs . 2012;41(1):114-121. - Kent J.S. et al., "Principles for Maintaining and Increasing Milk Production". J Obstet Ginecol Neoneutal Nurs. 2012;41(1):114-121.
Read instructions before use. Consult a specialist about possible contraindications.