Bottle feeding breastfed baby amount
How much expressed milk will my baby need? • KellyMom.com
By Kelly Bonyata, BS, IBCLC
- How much milk do babies need?
- What if baby is eating solid foods?
- Is baby drinking too much or too little expressed milk?
- Other ways of estimating milk intake
- References
Image credit: Jerry Bunkers on flickr
How much milk do babies need?
Many mothers wonder how much expressed breastmilk they need to have available if they are away from baby.
.
In exclusively breastfed babies, milk intake increases quickly during the first few weeks of life, then stays about the same between one and six months (though it likely increases short term during growth spurts). Current breastfeeding research does not indicate that breastmilk intake changes with baby’s age or weight between one and six months. After six months, breastmilk intake will continue at this same level until — sometime after six months, depending in baby’s intake from other foods — baby’s milk intake begins to decrease gradually (see below).
The research tells us that exclusively breastfed babies take in an average of 25 oz (750 mL) per day between the ages of 1 month and 6 months. Different babies take in different amounts of milk; a typical range of milk intakes is 19-30 oz per day (570-900 mL per day).
We can use this information to estimate the average amount of milk baby will need at a feeding:
- Estimate the number of times that baby nurses per day (24 hours).
- Then divide 25 oz by the number of nursings.
- This gives you a “ballpark” figure for the amount of expressed milk your exclusively breastfed baby will need at one feeding.
Example: If baby usually nurses around 8 times per day, you can guess that baby might need around 3 ounces per feeding when mom is away. (25/8=3.1).
What if baby is eating solid foods?
Sometime between six months and a year (as solids are introduced and slowly increased) baby’s milk intake may begin to decrease, but breastmilk should provide the majority of baby’s nutrition through the first year. Because of the great variability in the amount of solids that babies take during the second six months, the amount of milk will vary, too. One study found average breastmilk intake to be 30 oz per day (875 ml/day; 93% of total intake) at 7 months and 19 oz (550 ml/day; 50% of total energy intake) at 11-16 months.
Because of the great variability in the amount of solids that babies take during the second six months, the amount of milk will vary, too. One study found average breastmilk intake to be 30 oz per day (875 ml/day; 93% of total intake) at 7 months and 19 oz (550 ml/day; 50% of total energy intake) at 11-16 months.
Several studies have measured breastmilk intake for babies between 12 and 24 months and found typical amounts to be 14-19 oz per day (400-550 mL per day). Studies looking at breastmilk intake between 24 and 36 months have found typical amounts to be 10-12 oz per day (300-360 mL per day).
Is baby drinking too much or too little expressed milk?
Keep in mind that the amount of milk that baby takes at a particular feeding will vary, just as the amount of food and drink that an adult takes throughout the day will vary. Baby will probably not drink the same amount of milk at each feeding. Watch baby’s cues instead of simply encouraging baby to finish the bottle.
If your baby is taking substantially more than the average amounts, consider the possibility that baby is being given too much milk while you are away. Things that can contribute to overfeeding include:
Things that can contribute to overfeeding include:
- Fast flow bottles. Always use the lowest flow bottle nipple that baby will tolerate. Even with a slower flowing nipple, it is important to pace the bottle feed to allow baby to better control his intake.
- Using bottle feeding as the primary way to comfort baby. Some well-meaning caregivers feed baby the bottle every time he makes a sound. Use the calculator above to estimate the amount of milk that baby needs, and start with that amount. If baby still seems to be hungry, have your caregiver first check to see whether baby will settle with walking, rocking, holding, etc. before offering another ounce or two.
- Baby’s need to suck. Babies have a very strong need to suck, and the need may be greater while mom is away (sucking is comforting to baby). A baby can control the flow of milk at the breast and will get minimal milk when he mainly needs to suck. When drinking from a bottle, baby gets a larger constant flow of milk as long as he is sucking.
 If baby is taking large amounts of expressed milk while you are away, you might consider encouraging baby to suck fingers or thumb, or consider using a pacifier for the times when mom is not available, to give baby something besides the bottle to satisfy his sucking needs.
If baby is taking large amounts of expressed milk while you are away, you might consider encouraging baby to suck fingers or thumb, or consider using a pacifier for the times when mom is not available, to give baby something besides the bottle to satisfy his sucking needs. - If, after trying these suggestions, you’re still having a hard time pumping enough milk, see I’m not pumping enough milk. What can I do?
If baby is taking significantly less expressed milk than the average, it could be that baby is reverse-cycling, where baby takes just enough milk to “take the edge off” his hunger, then waits for mom to return to get the bulk of his calories. Baby will typically nurse more often and/or longer than usual once mom returns. Some mothers encourage reverse cycling so they won’t need to pump as much milk. Reverse cycling is common for breastfed babies, especially those just starting out with the bottle.
If your baby is reverse cycling, here are a few tips:
- Be patient.
 Try not to stress about it. Consider it a compliment – baby prefers you!
Try not to stress about it. Consider it a compliment – baby prefers you! - Use small amounts of expressed milk per bottle so there is less waste.
- If you’re worrying that baby can’t go that long without more milk, keep in mind that some babies sleep through the night for 8 hours or so without mom needing to worry that baby is not eating during that time period. Keep an eye on wet diapers and weight gain to assure yourself that baby is getting enough milk.
- Ensure that baby has ample chance to nurse when you’re together.
Other ways of estimating milk intake
There are various ways of estimating the amount of milk intake related to the weight of the baby and the age of the baby, based upon formula intake – research has shown that after the early weeks these methods overestimate the amount of milk that baby actually needs. These are the estimates that we used for breastfed babies for years, with the caveat that most breastfed babies don’t take as much expressed milk as estimated by these methods. Current research tells us that breastmilk intake is quite constant after the first month and does not appreciably increase with age or weight, so the current findings are validating what moms and lactation counselors have observed all along.
Current research tells us that breastmilk intake is quite constant after the first month and does not appreciably increase with age or weight, so the current findings are validating what moms and lactation counselors have observed all along.
More:
- Breast Versus Bottle: How much milk should baby take? By Nancy Mohrbacher, IBCLC, FILCA
- Supplementation Guidelines from LowMilkSupply.org
References
Onyango, Adelheid W., Receveur, Olivier and Esrey, Steven A. The contribution of breast milk to toddler diets in western Kenya. Bull World Health Organ, 2002, vol.80 no.4. ISSN 0042-9686.
Salazar G, Vio F, Garcia C, Aguirre E, Coward WA. Energy requirements in Chilean infants. Arch Dis Child Fetal Neonatal Ed. 2000 Sep;83(2):F120-3.
Kent JC, Mitoulas L, Cox DB, Owens RA, Hartmann PE. Breast volume and milk production during extended lactation in women. Exp Physiol. 1999 Mar;84(2):435-47.
Persson V, Greiner T, Islam S, and Gebre-Medhin M. The Helen Keller international food-frequency method underestimates vitamin A intake where sustained breastfeeding is common. Food and Nutrition Bulletin, vol.19 no.4. Tokyo, Japan: United Nations University Press, 1998.
The Helen Keller international food-frequency method underestimates vitamin A intake where sustained breastfeeding is common. Food and Nutrition Bulletin, vol.19 no.4. Tokyo, Japan: United Nations University Press, 1998.
Cox DB, Owens RA, Hartmann PE. Blood and milk prolactin and the rate of milk synthesis in women. Exp Physiol. 1996 Nov;81(6):1007-20.
Dewey KG, Heinig MJ, Nommsen LA, Lonnerdal B. Maternal versus infant factors related to breast milk intake and residual milk volume: the DARLING study. Pediatrics. 1991 Jun;87(6):829-37.
Neville MC, et al. Studies in human lactation: milk volumes in lactating women during the onset of lactation and full lactation. Am J Clin Nutr. 1988 Dec;48(6):1375-86.
Dewey KG, Finley DA, Lonnerdal B. Breast milk volume and composition during late lactation (7-20 months). J Pediatr Gastroenterol Nutr. 1984 Nov;3(5):713-20.
Butte NF, Garza C, Smith EO, Nichols BL. Human milk intake and growth in exclusively breast-fed infants. J Pediatr. 1984 Feb;104(2):187-95.
J Pediatr. 1984 Feb;104(2):187-95.
Dewey KG, Lonnerdal B. Milk and nutrient intake of breast-fed infants from 1 to 6 months: relation to growth and fatness. J Pediatr Gastroenterol Nutr. 1983;2(3):497-506.
Brown K, Black R, Robertson A, Akhtar N, Ahmed G, Becker S. Clinical and field studies of human lactation: methodological considerations. Am J Clin Nutr 1982;35:745-56.
Jelliffe D, Jelliffe E. The volume and composition of human milk in poorly nourished communities: a review. Am J Clin Nutr 1978;31:492-515.
| Summary of Research Data | ||||
| Baby’s Age | Average Milk Intake per 24 hours | Reference | ||
| g | ml | oz | ||
| 5 days | 498 +/- 129 g | 483 ml | 16 oz | Neville 1988 |
| 1 mo | 728 g | 706 ml | 24 oz | Salazar 2000 |
| 1 mo | — | 673 ml | 23 oz | Dewey 1983 |
| 1 mo | 708 +/- 54. 7 g 7 g | 687 ml | 23 oz | Cox 1996 |
| 1-6 mo | 453.6+/-201 g per breast | 440 ml x2 = 880 ml | 30 oz | Kent 1999 |
| 3 mo | 818 g | 793 ml | 27 oz | Dewey 1991 |
| 3-5 mo | 753 +/- 89 g | 730 ml | 25 oz | Neville 1988 |
| 6 mo | — | 896 ml | 30 oz | Dewey 1983 |
| 6 mo | 742 +/- 79.4 g | 720 ml | 24 oz | Cox 1996 |
| 7 mo | — | 875 ml (93% of total energy intake) | 30 oz | Dewey 1984 |
| 11-16 mo | — | 550 ml (50% of total energy intake) | 19 oz | Dewey 1984 |
| 11-16 mo | 502 +/- 34 g | 487 ml (32% of total energy intake) | 16. | Onyango 2002 |
| 12-17 mo | 563 g | 546 ml | 18 oz | Brown 1982 |
| 12-23 mo | 548 g | 532 ml | 18 oz | Persson 1998 |
| 15 mo | 208.0+/-56.7 g per breast | 202 ml x2 = 404 ml | 14 oz | Kent 1999 |
| 18-23 mo | 501 g | 486 ml | 16 oz | Brown 1982 |
| >24 mo | 368 g | 357 ml | 12 oz | Brown 1982 |
| 24-36 mo | 312 g | 303 ml | 10 oz | Persson 1998 |
| Specific Gravity of Mature Human Milk = 1.031, so Density of Mature Human Milk ~ 1.031 g/ml;1 oz = 29.6 ml;Numbers in gray were derived using the above conversion factors. | ||||
Feeding expressed milk | introducing bottle
When can you start feeding your baby expressed breast milk? What’s the best way to do it? And should you be concerned about ‘nipple confusion’? We answer your questions about expressed milk feeding
Share this content
When should I start giving my baby expressed milk?
If your baby is healthy and breastfeeding is going well, there’s no need to rush into giving her expressed milk. For the first four weeks, you’re working together to initiate and build your breast milk supply while she learns to breastfeed efficiently. While there is limited data,1 it is thought that unnecessarily introducing bottles during this crucial first month could interfere with these processes.
But if your newborn struggles to latch or suck for any reason, then start expressing milk as soon as possible after the birth. Read our articles on overcoming problems in the first week and feeding breast milk to your premature baby or infant with special needs for more advice, as well as getting support from your healthcare professionals.
How can I feed expressed milk to my baby?
There is a range of expertly designed feeding solutions that can help you give expressed milk to your baby, depending on your and her needs.
For example, Medela’s innovative Calma teat will only allow milk to flow when babies create a vacuum by sucking. This means they can feed from a bottle using the same technique, tongue motion and jaw movement they would at the breast. 2,3 Developed with breastfeeding experts from the University of Western Australia, Calma allows your baby to suck, swallow, pause and breathe just as she does when breastfeeding.4 By maintaining babies’ natural sucking behaviour, Calma is designed to make it easy to switch from breast to bottle-feeding and back again.
Medela also makes conventional bottle teats in two flow versions. And all our teats can be attached directly to the bottles you express milk into, minimising the risk of spillages.
If your newborn needs expressed milk, but you don’t want to offer her a bottle until she’s become used to breastfeeding, you could use a baby cup designed for short-term feeding. This allows your baby to sip or lap your expressed milk – be careful to avoid spills! It’s advisable to have a healthcare professional on hand the first time you use the baby cup, to make sure you’re both getting the hang of it.
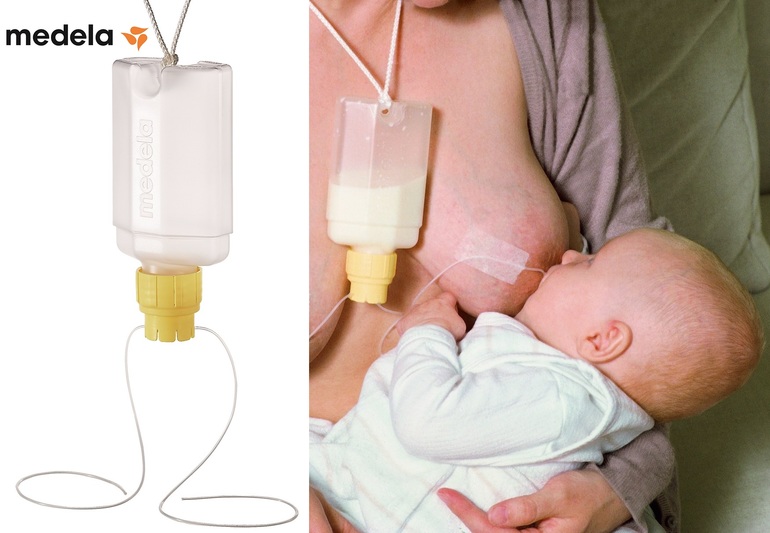
For babies who need expressed milk supplements in addition to regular breastfeeding, a supplemental nursing system (SNS) can be helpful. This has a thin, flexible feeding tube that can be fixed alongside your nipple to give your baby expressed milk while you’re breastfeeding her. This allows your baby to stay at your breast longer, which further stimulates your breasts to help maintain your milk supply, and also helps improve her breastfeeding skills. It can be useful for mums with low milk supply or with adopted or surrogate babies.
If your baby can’t create the suction needed to breastfeed – perhaps because of a disability, congenital condition or weakness – you could try a feeder designed for babies with special needs. These allow infants who can’t suck to feed using gentle compression instead.
What’s the best way to introduce a bottle?
If breastfeeding is going well and you’ve decided it’s the right time to give your baby a bottle of expressed milk, follow these tips:
Take your time
Don’t wait until your big night out or first day back at work to introduce your baby to the bottle. Start trying with a small amount of expressed milk, in a relaxed and unhurried way, a couple of weeks beforehand. Gradually build up to giving a full feed of expressed breast milk from a bottle.
Pick your moment
Ideally your breastfed baby should be alert, but not too hungry, the first time she has a bottle of expressed milk, so that she is as relaxed as possible.
Delegate feeding duties
Your baby may be confused or frustrated when you offer a bottle, as she’s used to your breast. It might be easier if someone else gives the first bottle, and you stay out of the room so your baby can’t see or smell you.
Not too hot, not too cold
Your baby may be more likely to take the expressed milk if it’s around body temperature, 37 °C (98.6 °F).
Dip and sip
Try dipping the bottle teat into some expressed milk before offering it, so it tastes and smells of your breast milk. Then gently stimulate your baby’s top lip with the teat to encourage her to open her mouth.
Positioning for bottle-feeding
Feed your baby on demand and cuddle her in a semi-upright position. Never bottle-feed her while she’s lying flat or prop her up with the bottle, in case of choking. Go at her pace, with as many pauses as she needs – you can even try switching sides during the feed.
Be patient
Don’t worry if she doesn’t take to the bottle straight away – it may take several tries. If she pushes the bottle away or becomes upset, comfort her and wait a few minutes before trying again. If she still won’t drink from the bottle, wait a few more minutes and then breastfeed her as normal. Try again with the bottle at a different time of day.
How much expressed milk should I give my baby?
Every baby is different. Research shows that in babies aged one to six months, one baby may take as little as 50 ml during a feed while another may take as much as 230 ml. Start by preparing a bottle with around 60 ml, and see if your baby needs more or less. You'll soon learn how much she typically takes – but don’t ever pressure her to finish the bottle.
How can I ensure bottle-feeding is safe for my baby?
Always clean and sanitise your breast pump set and bottles according to the instructions, and wash your hands before pumping, handling milk or feeding your baby. Follow our guidelines for storing and thawing your expressed milk safely.
If warming your breast milk, place the milk bottle or bag into a bowl of warm water or a warmer, or run it under a warm tap (max 37 °C or 98.6 °F). Never warm breast milk in the microwave or on the stove top.
Will my baby cope with switching from breast to bottle?
Mums sometimes worry that if they introduce a bottle too soon, their baby will get accustomed to the artificial teat and struggle to return to breastfeeding. Others are concerned about the opposite problem – if they don’t get their baby used to a bottle early she may never accept one later. Both of these problems are commonly referred to as ‘nipple confusion’.
Experts disagree on whether nipple confusion is really an issue.1 Certainly sucking from a conventional bottle teat that doesn’t require a vacuum to be created is less effort for a baby than sucking from mum’s nipple, as the milk flows more freely and gravity lends a hand. And some babies do seem to have a preference for breast or bottle, and never take to the other. But many babies switch happily between the two.
If you’re still struggling to feed your baby expressed breast milk, speak to a lactation consultant or breastfeeding specialist.
References
1 Zimmerman E, Thompson K. Clarifying nipple confusion. J Perinatol. 2015;35(11):895-899.
2 Geddes DT et al. Tongue movement and intra-oral vacuum of term infants during breastfeeding and feeding from an experimental teat that released milk under vacuum only. Early Hum Dev. 2012;88(6):443-449.
3 Segami Y et al. Perioral movements and sucking pattern during bottle feeding with a novel, experimental teat are similar to breastfeeding. J Perinatol. 2013;33(4):319-323.
J Perinatol. 2013;33(4):319-323.
4 Sakalidis VS et al. Oxygen saturation and suck-swallow-breathe coordination of term infants during breastfeeding and feeding from a teat releasing milk only with vacuum. Int J Pediatr. 2012;2012:130769.
Bottle feeding - how much milk a newborn needs
search support iconSearch Keywords
Shopping Cart
There are currently no items in your shopping cart.
{{#if isPersonalizedBundle}}
{{#if curatedBundle.price}}
{{curatedBundle.price}}
{{curatedBundle.discountPrice}}
{0{/if}}
{0{/if}} {{/if}} {{#if isSubscriptionBundle}}
{{#if curatedBundle.displayPrice}}
{{curatedBundle.displayPrice}}
+{{curatedBundle.displayRecurringCharge.totalFormattedValue}} / {{curatedBundle. ratePlanDuration}}
ratePlanDuration}}
{{/if }}
{{/if}} {{/if}} {{#if isBundle}} {{#each bundle}}{{#if bundle.label}}{{bundle.label}}{{else}}Bundled Item{{/if}}
{{#if totalPrice}} {{#if formerPrice}}
{{formerPrice}}
{{/if}}
{{totalPrice}}
{{/if}}
{{/each}} {{/if}} {{#if isSingleItem}}
-{{discountValue}}
{{/if}}{{#if miniCartProductpath}}
{{/if}}{{#iff quantity 'gt' '1'}} {{quantity}} x {{/iff}} {{#if familyName}} {{familyName}} {{/if}} {{#if descriptor}} {{descriptor}} {{/if}}
{{#if miniCartProductpath}}{{/if}} {{#if sellerName}} {{soldBySiteText}} {{sellerName}} {{/if}}
{{#if totalPrice. formattedValue}} {{#if formerPrice.formattedValue}}
formattedValue}} {{#if formerPrice.formattedValue}}
{{formerPrice.formattedValue}}
{{/if}}
{{totalPrice.formattedValue}}
{{/if}}
an error occurred from the cart. Try again
{{/if}} {{/each}}
{{#iff cart.attributes.pricing.orderDiscountNoDelivery.value 'gt' 0}}
Discount: - {{cart.attributes.pricing.orderDiscountNoDelivery.formattedValue}}
{{/ iff}}
Shipping cost: {{#iff cart.attributes.pricing.totalDelivery.value 'gt' 0}} {{cart.attributes.pricing.totalDelivery.formattedValue}} {{else}} FREE {{/iff }}
Subtotal: {{cart.attributes.pricing.total.formattedValue}}
{{/if}} {{#if price.formattedValue}}
{{price.formattedValue}}
{{/if}}
Like any new mom, of course you want to know how much a newborn should eat and how many milliliters he drinks milk in one feeding session. In creating your body, nature made sure that you can give your baby all the necessary nutrients. And yet, each of us needs practical advice and authoritative opinion from the outside when it comes to such an important issue as feeding. So how much milk does your baby need?
Whether you are breastfeeding or formula feeding your baby (or a combination of both), our page will tell you how much milk a newborn needs for healthy growth and development.
How do you know if a child is hungry?
All mothers have well-developed instincts, but at first not everyone can read their baby's mind! Over time, you will learn to understand your baby's body language well and to recognize the signs that indicate that he is hungry. In the meantime, you are just learning, we will tell you how to understand what the baby is asking to eat. Here are the most typical signs:
- Reaches head towards breast or bottle.
- Clenches her fists.
- Brings pens to mouth.
- Wrinkles, smacks or licks lips.
If you notice even one of these signs, then your baby is trying to tell you that it's time to eat. Ideally, the baby should only be breastfed when he is hungry and asks for food. If you are breastfeeding, this approach will allow you to maintain the required supply of milk, as the body naturally responds to the baby's need and produces the optimal amount of milk. On-demand formula feeding can also be beneficial for the baby, as newborns are able to self-regulate their feeding needs.
How much breast milk does a newborn need?
So, how much do newborns eat? The beauty is that each child is unique, so no kid will ever eat according to the textbook. Don't be discouraged if your feeding schedule is slightly different from what is described in this article. However, if something causes you serious concerns, be sure to consult your doctor or the pediatrician who is treating your baby.
Newborns typically eat every two to three hours, eight to twelve times a day. How many milliliters of milk does a newborn drink in one feeding session? In the first days after giving birth, your milk is yellowish in color and has a thick consistency. Colostrum - the name of the first breast milk - has unique immunological properties and is an ideal source of nutrients needed by the newborn 1 .
How much milk does a baby need to be full? In the first days of life, newborns drink from 30 to 60 ml of milk per feeding, after two weeks this amount increases to 60-90 ml. So don't worry if you feel like you don't have enough milk in the first days after giving birth! The duration of feeding also changes: in the first days it ranges from 10 to 30 minutes, then it gradually increases as the baby grows.
How much breast milk do you need if you want to bottle feed your baby?
If you decide to bottle feed your baby from time to time, the duration of the feeding session should be no less than the duration of breastfeeding. Periodic pumping allows the nipples to rest, while your baby continues to receive healthy breast milk, and you can plan and control the feeding process more effectively.
It's important to choose a bottle that will help you and your baby feel comfortable formula feeding, such as the Natural bottles. The comfortable bottle shape and special soft petals on the nipple provide a natural latch and feel like a real mother's breast - so realistic that the baby will hardly notice the difference.
How do you know when your baby is no longer hungry? Whether you're breastfeeding or bottle feeding, the following signs will tell you when your baby is full:
If you see that the baby is full, stop feeding, even if there is milk left in the breast or bottle 2 .
The right choice for you and your baby
Remember, every child is different and your relationship with your baby is unlike anyone else's. Choose the feeding method that works best for you and your baby, whether it's breastfeeding, bottle feeding, or a combination of both.
1. https://medlineplus.gov/ency/patientinstructions/000712.htm
You are leaving the Philips Healthcare (“Philips”) official website. Any links to third party websites that may be included on this site are provided solely as a convenience to you. Philips makes no warranties regarding any third party websites or the information they contain.
I understand
You are about to visit a Philips global content page
Continue
You are about to visit the Philips USA website.
I understand
Feeding expressed milk | breastfeeding
When can I start breastfeeding my baby with expressed breast milk? How to do it right? Is it worth worrying that the child will confuse the pacifier with the breast? In this article we will answer your questions.
Share this information
When can I start breastfeeding my baby?
If your baby is healthy and breastfeeding well, there is no need to give him expressed milk. For the first four weeks, you work together to start and increase milk production, and your baby also learns to suckle properly at the breast. There is not enough scientific data on this yet, 1 but there is an opinion that bottle feeding in the first month may adversely affect the process of establishing breastfeeding.
However, if the newborn is unable to latch on or suckle for some reason, start expressing milk as soon as possible after delivery. Read more about this in our articles on coping with problems in the first week, breastfeeding premature babies and babies with special needs, and seeking help from your healthcare provider.
How can I feed my baby with expressed breast milk?
There are many expert feeding solutions that allow you to give your baby expressed milk in a variety of ways, depending on your and your baby's needs.
For example, the innovative Calma smart pacifier only lets milk through when the baby creates a vacuum by suckling. This means that when feeding from a bottle, he will make the same movements with his tongue and jaws as when sucking at the breast. 2.3 Calma was developed with the help of breastfeeding experts from the University of Western Australia. When using this pacifier, the baby can suck, swallow, pause and breathe in the same way as when breastfeeding. 4 Maintaining natural sucking habits allows baby to transition easily from breast to bottle and back.
In addition, Medela also offers regular bottle teats* in two versions that produce milk at different rates. All Medela* nipples can be placed directly on bottles used for expressing milk, minimizing the risk of spillage.
If you need to feed your baby with expressed milk, but you do not want to bottle feed him until he is learning to breastfeed, you can use a sippy cup* for temporary feeding. The baby will be able to drink milk from such a mug, but you should be careful not to spill the milk. For the first time, it is advisable to feed the child from a drinking cup under the supervision of the attending physician in order to learn how to do it correctly.
If your baby needs to be supplemented with expressed milk in addition to regular breastfeeding, the Supplementary Feeding System (SNS)* can be used. It is equipped with a thin, flexible capillary that can be clipped close to the nipple to give your baby expressed milk while breastfeeding. Thanks to this, the baby suckles the breast for longer, thereby developing sucking skills and stimulating the production of milk from the mother. This can be helpful when there is a shortage of breast milk, as well as when feeding adopted or surrogate children.
If the baby is unable to breastfeed because he is too weak or has a congenital disease, you can use the Special Needs Cup*, which releases milk with gentle pressure, making it suitable for feeding these babies.
How to teach a child to bottle feed?
If breastfeeding is going well and you decide to start bottle feeding your baby with expressed breast milk, follow these guidelines.
Start early and take your time
Don't wait until the first day of work or the first time you leave the house to bottle feed your baby. Start accustoming your baby to small portions of expressed milk a couple of weeks before the desired date, calmly and without haste. Gradually build up to one full serving of pumped milk from a bottle.
Choose a time
Ideally, at the first bottle feeding, the baby should be hungry, but not too hungry - in this state, he is as relaxed as possible.
Let others feed
Your baby is used to feeding from your breast, so when you offer him a bottle it can be confusing. The process can go faster if the first time the baby is bottle-fed by someone else while you are not in the room, so that your sight and smell do not embarrass the baby.
Maintain optimal temperature
Your baby will be more willing to eat expressed milk if the temperature is around 37°C, close to body temperature.
Dip a nipple in milk
Try dipping a nipple in expressed milk before offering it to your baby. This way it will taste and smell like your breast milk. Lightly touch the baby's upper lip with the nipple to open the mouth.
Choose the right position for bottle feeding
Feed your baby on demand and keep him reclining during feeding. Never bottle feed your baby when he is lying or sitting, otherwise he may choke. Listen to the wishes of the child - take as many pauses as he needs. You can even try to shift it from one hand to another during feeding.
Be patient
Don't worry if your baby doesn't take the bottle right away - it may take several tries. If he pushes the bottle away or starts crying, calm him down, wait a few minutes and try again. If he still doesn't want to bottle feed, wait a few more minutes and breastfeed him as usual. Repeat the bottle experiment at a different time of day.
How much expressed milk should I give my baby?
All children are different. Research shows that between the ages of one and six months, a baby can consume between 50 and 230 ml of milk per feeding. To start, prepare about 60 ml and observe how much your baby needs - more or less. You will soon realize how much milk he usually eats. Just never force him to finish the cooked portion.
How can I keep my baby safe when bottle feeding?
Always clean and sterilize your pump and bottles according to the manufacturer's instructions. Wash your hands before expressing, pouring milk, and feeding your baby. Follow our instructions for safely storing and thawing your expressed milk.
If breastmilk needs to be warmed, place the bottle or bag in a bowl of warm water or a heater or under running water at a maximum of 37°C. Never heat breast milk in the microwave or on the stove.
Will the baby be able to transition from breast to bottle?
Some mothers worry that if they start bottle feeding too early, they will get used to the artificial nipple and not want to breastfeed. Others, on the contrary, are worried that if the child is not immediately accustomed to the bottle, then he will no longer eat from it. In general, in these cases, they say that the child confuses the nipple with the breast.
Experts disagree on whether such confusion is a problem. 1 Without a doubt, it is easier for a baby to suckle milk from a regular bottle with a nipple, which does not require a vacuum, than from the breast, since the milk flows faster, also under the influence of gravity. And some babies really have clear preferences: only the breast or only the nipple. However, many babies are comfortable suckling both the breast and the pacifier.
If you are unable to feed your baby with expressed breast milk, seek help from a lactation consultant or specialist.
Literature
1 Zimmerman E, Thompson K. Clarifying nipple confusion. J. Perinatol. 2015;35(11):895-899. - Zimmerman I., Thompson K., "On the issue of breastfeeding." J Perinatol (Journal of Perinatology). 2015;35(11):895-899.
2 Geddes DT et al. Tongue movement and intra-oral vacuum of term infants during breastfeeding and feeding from an experimental teat that released milk under vacuum only. Early Hum Dev . 2012;88(6):443-449. - Geddes D.T. et al., "Language Movements and Oral Vacuum Generation in Term Infants During Breastfeeding and Feeding from an Experimental Vacuum-Delivery Teat". Airlie Hume Dev. 2012;88(6):443-449.
3 Segami Y et al. Perioral movements and sucking pattern during bottle feeding with a novel, experimental teat are similar to breastfeeding. J. Perinatol. 2013;33(4):319-323. - Segami I. et al.