Bottle feeding down syndrome baby
Bottle Feeding a Baby - Central Mississippi Down Syndrome Society
Most babies with Down syndrome grow properly and do just fine in the eating department. But some young babies with Down syndrome have a harder time sucking efficiently, due to their low muscle tone. Their mouths may be less “alert” or ready for feeding, and the extra effort they have to put out to eat gives them less endurance for getting through the whole meal.
Babies with Down syndrome and their parents usually find a few tricks that make feedings easier for everybody.
Breastfed babies with low muscle tone can lose interest while waiting for the milk to let-down. Some babies with Down syndrome find it harder to latch on to the breast or bottle nipple and maintain a good hold throughout the meal. These babies take many more breaks and end up eating less per feeding than you would expect for the amount of time spent. Swallowing excess air is common because the baby has a less efficient hold on the nipple.
Despite these concerns, babies with Down syndrome and their parents usually find a few tricks that make feedings easier for everybody. Below are some of the techniques that often work.
What Can Be Done?
Babies with low tone may need help using the muscle strength and control they have. They often prefer to be fed in a way that requires the least effort, rather than using their muscle control. To help encourage muscle strength, you need to “wake them up” or alert them before and during each feeding. Here are a few wake-up strategies; contact your baby’s doctor to review the appropriateness of these activities for your child.
Preparation
Start the feeding when your baby is most awake or alert.
See if playing with your baby just before feeding helps increase attention for the meal. Play gentle tickle games with fingers, toys, or kissing around the face and neck. While supporting your baby’s head, dance with your baby so head and upper body control is stimulated. Bounce your baby gently in your lap. Of course, the dancing and bouncing should be done only if your baby can handle that much stimulation and has the head control necessary to participate without getting hurt.
Bounce your baby gently in your lap. Of course, the dancing and bouncing should be done only if your baby can handle that much stimulation and has the head control necessary to participate without getting hurt.
Some parents find that a cool or tepid bath wakes up their baby before feedings. Others find that a brisk towel rub helps.
After waking up your baby’s body, focus the alerting on the face and mouth area. A cool washcloth on the face or gentle tapping around face and mouth may increase readiness for the bottle.
Some parents find that gently tickling or stretching the muscles around the lips and cheeks helps wake up the mouth. You can use fingers and washcloths.
Position
Feed your baby in as upright a position as possible. The more your baby is up against gravity, the more active the muscles become. In addition, babies with Down syndrome seem to be more prone to ear infections. Upright feedings decrease the chance of liquid backing up in the ear canals, reducing the risk of infection.
Be sure that your baby is being fed in a chin tuck position. This position, with the head not too far back and not too far forward, seems to set up the neck and mouth muscles for the strongest sucking response. Try to rest your baby’s head – not neck – on your arm when holding during feedings, which automatically tucks the chin slightly. This position also can be achieved with pillows or arm rests.
An angled bottle, available commercially, may be used to keep the baby’s head at this angle until the end of the feeding. With a regular bottle, children must tip their heads back to get the last few drops. An angled bottle solves this problem. Cool the liquid.
Temperature may affect the efficiency and speed of your baby’s sucking and swallowing. After checking with your doctor, consider starting the baby at room-temperature formula and gradually chilling the formula until your baby can handle it straight from the refrigerator. This can increase not only the baby’s interest in sucking but also the amount that is sucked during the meal.
Cheek and Tongue Involvement
Some babies need to be reminded to suck during the meal by having a little attention drawn to their tongues. To increase tongue involvement, try tapping the nipple on the tongue or pressing up and down on the tongue regularly throughout the meal. This may serve to wake up the tongue, but should be discontinued or decreased if it disrupts the meal too much. Cheeks can be tickled, squeezed slightly, or tapped to keep them active during a feeding.
Ask for Help
Babies with Down syndrome have all the basic skills necessary for taking a breast or bottle. The suggestions in this article are intended to increase babies’ efficiency and control, so they can progress to more difficult food textures and consistencies.
Some babies with Down syndrome have further medical complications that interfere with good sucking or good nutritional intake. These conditions may require extra assistance. Ask your pediatrician, feeding specialist, or developmental team if you have questions or need more help. If you do not have a team in place, please see our list of suggested professionals.
If you do not have a team in place, please see our list of suggested professionals.
Food for Thought: Addressing Feeding and Swallowing Challenges
From Down Syndrome World Summer 2016
By Arwen Jackson, M.A., CCC-SLP; Bridget Harrington, M.A., CCC-SLP; and Carol Spicer, OTR/L, Anna and John J. Sie Center for Down Syndrome, Children’s Hospital Colorado
It’s important to identify and treat feeding and swallowing issues early to ensure your child with Down syndrome gets the most out of every healthy meal.
Children with Down Syndrome can encounter problems with feeding or swallowing due to physical, medical, or behavioral issues associated with their condition. Low muscle tone , sensory problems, food refusal, low endurance, or issues with oral motor skill development can all lead to problems that make eating difficult. This creates stress for children and their parents and can ultimately interfere with a child’s ability to grow and thrive.
A safe and enjoyable meal begins with attending to your child’s cues and supporting where he or she is developmentally.
BUILDING UP BABY
Both breast- and bottle-feeding help babies grow and develop oral motor skills. Beyond looking at your baby’s mouth, it is critical to observe the coordination of breathing and swallowing, the level of alertness, and beginning postural control. Babies do best with latching when they are in an awake, alert state. To help babies stay awake, talk to them, stroke their feet, or change their diapers.
This article was published in the award-winning Down Syndrome World™ magazine. Become a member to read all the articles and get future issues delivered to your door!
A pediatrician may suggest working with specialists, such as those at the Feeding Clinic at the Anna and John J. Sie Center for Down Syndrome at Children’s Hospital Colorado, to develop a safe and effective feeding plan that can be adapted to babies who breast-feed, bottle-feed, or both.
CAREFUL OBSERVATION
A parent’s power of observation is crucial in detecting issues with feeding and swallowing. Look for signs of swallowing difficulties, such as red watery eyes, coughing, choking, congestion, and chronic pulmonary or respiratory illness. Any of these could indicate dysphagia, or difficulty swallowing, which requires further medical investigation.
During meals, feeding difficulties may appear as prolonged or no chewing, overstuffing the mouth, and pocketing food. Behavioral signs related to feeding issues can include, but are not limited to, food refusal, inability to sit at the table, unwillingness to try new foods, or willful gagging and vomiting.
If your child is overstuffing his or her mouth, place two or three bites of food on a plate at a time and continue offering small servings. Children often have difficulty controlling the impulse to stuff their mouths when offered a full plate of food.
Poor postural stability also affects children’s ability to sit and actively participate in feeding themselves. If they cannot hold their heads up independently or have difficulty sitting, eating safely is more challenging. To improve posture, try holding your child in a more upright position on your lap or placing small towel rolls on either side of the trunk while in a high chair. This may offer enough support to free up the child’s hands for food exploration and self-feeding.
If they cannot hold their heads up independently or have difficulty sitting, eating safely is more challenging. To improve posture, try holding your child in a more upright position on your lap or placing small towel rolls on either side of the trunk while in a high chair. This may offer enough support to free up the child’s hands for food exploration and self-feeding.
SETTING THE TABLE
If your child appears to have behavioral or sensory issues with food, try these tips to set him or her up for success:
- Lay the groundwork for fun and exploration before mealtime. Let children have a voice in what they want to eat and allow them to help with meal preparation — make a smoothie together, for example. Allow them to experience the sensory side of preparing food by touching, smelling, and of course, tasting the ingredients.
- Eat at their eye level. Children learn eating skills by watching you, so it’s important that you model these skills at their eye level.
- Listen — even when your child isn’t saying anything. Young children with Down syndrome may take longer to chew and swallow food than typical children. Don’t rush them. Understand that nonverbal cues, such as pushing a spoon away or turning the head to the side, are your child’s way of saying, “I’m not ready for another bite yet.” Respecting these signs builds trust, which is the foundation of a successful feeding relationship.
Finally, remember that every child is different and a one-size-fits-all approach to treating feeding and swallowing challenges may not work. Pediatricians and specialists can be invaluable resources, assisting parents in developing evidence-based, individualized feeding plans to help children find mealtime success.
PERSISTENT PROBLEMS
Feeding and swallowing challenges can follow individuals with Down syndrome into adulthood. If this happens, it’s important for friends, family, and caregivers to encourage or provide consistent, structured mealtimes.
Being attentive to adults’ feeding behaviors is important, as some people may not be able to verbalize that a problem, such as a cavity or pain when swallowing, is present. Refusal to eat, sudden shifts in food choices and nutrition level, and changes in normal feeding behavior may be clues that something is amiss.
READ MORE
The following resources provide additional information for parents whose children with Down syndrome have feeding and swallowing issues:
- Child of Mine: Feeding with Love and Good Sense by Ellyn Satter (Third Edition, Bull Publishing Company, 2000)
- Gross Motor Skills in Children with Down Syndrome: A Guide for Parents and Professionals by Patricia C. Winders (Woodbine House, 2007)
- Feeding Matters: feedingmatters.org
- “Healthy Eating Habits in Children with Down Syndrome,” National Down Syndrome Society: www.ndss.org/resources/nutrition/
Find a medical care center near you that specializes in treating patients with Down syndrome at www. globaldownsyndrome.org/research-medical-care/medical-care-providers.
globaldownsyndrome.org/research-medical-care/medical-care-providers.
Like this article? Join Global Down Syndrome Foundation’s Membership program today to receive 4 issues of the quarterly award-winning publication, plus access to 4 seasonal educational Webinar Series, and eligibility to apply for Global’s Employment and Educational Grants.
Register today at downsyndromeworld.org!
Feeding children with special needs
American Academy of Pediatrics and The American College of Obstetricians and Gynecologists. Breastfeeding Handbook for Physicians 2006). - American Academy of Pediatrics and American College of Obstetrics and Gynecology. "Medical Guide to Breastfeeding", 2006.
Lawrence , R . A . & Lawrence , R . M . Breastfeeding : a guide for the medical profession ( Elsevier Mosby , Maryland Heights , MO , 2011). - Lawrence R.A., Lawrence R.M., "Breastfeeding: A guide for healthcare professionals." (Publisher Maryland Heights , Missouri, USA: Elsevier Mosby; 2011.)
Breastfeeding : a guide for the medical profession ( Elsevier Mosby , Maryland Heights , MO , 2011). - Lawrence R.A., Lawrence R.M., "Breastfeeding: A guide for healthcare professionals." (Publisher Maryland Heights , Missouri, USA: Elsevier Mosby; 2011.)
Prime, D.K.et al. Simultaneous breast expression in breastfeeding women is more efficacious than sequential breast expression. Breastfeed Med 7, 442-447 (2012). - Prime D.K. et al., “During the breastfeeding period, pumping both breasts simultaneously is more productive than sequential pumping.” Brest Med (Breastfeeding Medicine) 7, 442-447 (2012).
Morton, J., Hall, J.Y., Wong, R.J., Benitz, W.E. & Rhine, W.D. Combining hand techniques with electric pumping increases milk production in mothers of preterm infants. J Perinatol 29, 757–764 (2009). — Morton J., Hall J.I., Wong R.J., Benitz W.I. and Rhine, W.D., "Manual pumping combined with an electric breast pump increases breast milk production in mothers of preterm infants." J Perinatol (Journal of Perinatology) 29, 757-764 (2009)
Hill, P.D., Aldag, J.C., Chatterton RT. Initiation and frequency of pumping and milk production in mothers of non-nursing preterm infants. J Hum Lact . 2001;17(1):9–13 - Hill P.D., Aldag J.S. and Chatterton, R.T., "Onset and frequency of expression and milk production in mothers who have given birth to premature babies and have not breastfed them." J Hum Lakt (Journal of the International Association of Lactation Consultants) 17, 9-13 (2001).
Hill, P.D., Aldag, J.C., Chatterton RT, Zinaman M. Comparison of Milk Output Between Mothers of Preterm and Term Infants: The First 6 Weeks After Birth. J Hum Lact . 2005 February 1, 2005; 21(1):22–30. - Hill P.D., Aldag J.S., Chatterton R.T., Zinaman M., "Comparison of the amount of milk in mothers of full-term and premature babies in the first 6 weeks after birth." J Hum Lakt (Journal of the International Association of Lactation Consultants) 2005, 21(1): 22-30.
Parker, L.A., Sullivan, S., Krueger, C. & Mueller, M. Association of timing of initiation of breastmilk expression on milk volume and timing of lactogenesis stage II among mothers of very low-birth-weight infants. Breastfeed Med (2015). - Parker L.A., Sullivan S., Kruger S., Kelechi T. and Muller M., "Association of the time of initiation of expression with the amount of milk and the timing of the second stage of lactogenesis in mothers of children who had extremely low birth weight" . Brestfeed Med (Breastfeeding Medicine) (2015)
Brestfeed Med (Breastfeeding Medicine) (2015)
Meier, P.P., Engstrom, J.L., Janes, J.E., Jegier, B.J. & Loera, F. Breast pump suction patterns that mimic the human infant during breastfeeding: Greater milk output in less time spent pumping for breast pump-dependent mothers with premature infants. J Perinatol 32, 103-110 (2012). - Meyer P.P., Engstrom J.L., Jaynes J.I., Jaegier B.J., Loera F. "Pumping patterns that mimic the behavior of a breastfeeding baby: more milk and less time for constant pumping mothers of premature babies". J Perinatol (Journal of Perinatology) 32, 103-110 (2012).
Torowicz, D.L., Seelhorst, A., Froh, E.B., Spatz, D.L. Human milk and breastfeeding outcomes in infants with congenital heart disease. Breastfeed Med 10, 31–37(2015). - Torowicz DL , Seelhorst , FroH EB , Spatz DL , "Breast milk and breastfeeding outcomes for children with congenital heart disease", Brestfeed Med (Breastfeeding Medicine) 10, 31-37 (2015).
Reilly, S. et al. ABM clinical protocol #18: Guidelines for breastfeeding infants with cleft lip, cleft palate, or cleft lip and palate, revised 2013. Breastfeed Med 8, 349–353 (2013) - Reilly S. et al., " AVM Clinical Protocol No. 18: Guidelines for breastfeeding children with cleft lip, cleft palate, or cleft lip and palate, 2013 edition. Brestfeed Med (Breastfeeding Medicine) 8, 349–353 (2013).
Thomas, J., Marinelli, K.A., & Hennessy, M. ABM clinical protocol #16: Breastfeeding the hypotonic infant. Breastfeed Med 2, 112–118 (2007). — Thomas J., Marinelli C.A. and Hennessy, M., "AVM Clinical Protocol #16: Breastfeeding a Baby with Reduced Muscle Tone." Brestfeed Med (Breastfeeding Medicine). 2, 112–118 (2007)
My newborn was born with special needs. Can I breastfeed?
Translation: Tatyana Tutatchikova
Editor: Evgenia Champalova, Maria Sorokina
Proofreader: Tatyana Romanova
So, congratulations on the birth of your unique baby! And also because you decide to breastfeed him, because children with special needs receive special benefits from breast milk. Right now you are probably having conflicting feelings. Like most parents, you are excited to meet your newborn. At the same time, you may feel frustrated, angry, helpless, and even guilty. Give yourself time to accept these and other unfortunate feelings. Remember that your child is first and foremost just a baby, and only then a child with special needs.
Right now you are probably having conflicting feelings. Like most parents, you are excited to meet your newborn. At the same time, you may feel frustrated, angry, helpless, and even guilty. Give yourself time to accept these and other unfortunate feelings. Remember that your child is first and foremost just a baby, and only then a child with special needs.
Babies born with Down syndrome, cleft lip or palate (“cleft palate”), heart problems, cystic fibrosis, neurological problems, or other special needs need even more breast milk than other babies. Breast milk strengthens the baby's immunity and is easier to digest in the body. It is also optimal nutrition to support his health. This is especially important because your baby may need surgery or long-term care. The special bond between mother and baby and breast milk hormones help keep you calm and in touch with your baby.
Often a child with special needs is reluctant to breastfeed; in this case, you and your baby will need additional support during feeding. Let your health care provider know that you are determined to breastfeed. Your partner, other family members and friends, your lactation consultant or your LLL volunteer consultant can support you. Try to start breastfeeding right now. Be patient, it may take a few weeks for your baby to learn how to latch on properly. If your baby is still having difficulty sucking milk out of the breast, start expressing with a breast pump as soon as possible after birth. You should express milk as often as a baby would suck, that is, every two to three hours during the day; the alarm clock will help you keep a schedule of pumping and feeding. Expressed milk is best given to a child from non-sucking objects (spoon, cup or syringe). It is best to avoid bottles and pacifiers because breastfeeding is different from bottle sucking and nipple confusion can occur.
Let your health care provider know that you are determined to breastfeed. Your partner, other family members and friends, your lactation consultant or your LLL volunteer consultant can support you. Try to start breastfeeding right now. Be patient, it may take a few weeks for your baby to learn how to latch on properly. If your baby is still having difficulty sucking milk out of the breast, start expressing with a breast pump as soon as possible after birth. You should express milk as often as a baby would suck, that is, every two to three hours during the day; the alarm clock will help you keep a schedule of pumping and feeding. Expressed milk is best given to a child from non-sucking objects (spoon, cup or syringe). It is best to avoid bottles and pacifiers because breastfeeding is different from bottle sucking and nipple confusion can occur.
Ask your LLL Volunteer Consultant or Lactation Consultant about the possibility of using a breastfeeding system. Such a system is a container for breast milk with thin tubes.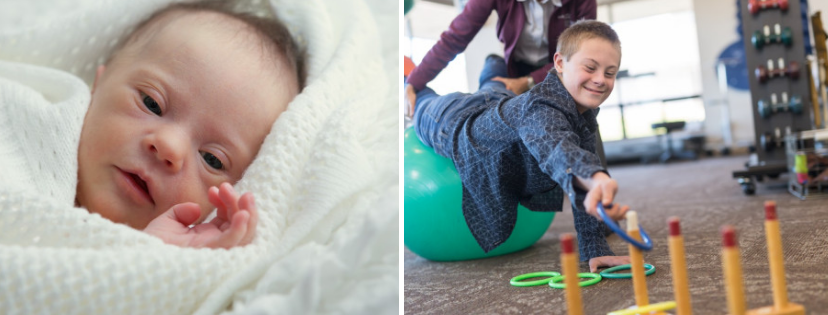 The tube is attached to your breast so your baby can get extra milk while he or she learns to suckle. Or you can attach a straw to your finger, allowing your baby to suck on it and get breast milk at the same time. (An adult's finger looks more like your nipple than a bottle nipple.) Some healthcare professionals may not be familiar with this method. Explain why this is important to you and your baby. Continue breastfeeding if possible. Studies show that breastfeeding is less stressful for the baby than bottle feeding; your doctor may not think about it. When you breastfeed, you hug your baby and touch him “skin to skin”, and this helps him develop his abilities and his potential to the fullest!
The tube is attached to your breast so your baby can get extra milk while he or she learns to suckle. Or you can attach a straw to your finger, allowing your baby to suck on it and get breast milk at the same time. (An adult's finger looks more like your nipple than a bottle nipple.) Some healthcare professionals may not be familiar with this method. Explain why this is important to you and your baby. Continue breastfeeding if possible. Studies show that breastfeeding is less stressful for the baby than bottle feeding; your doctor may not think about it. When you breastfeed, you hug your baby and touch him “skin to skin”, and this helps him develop his abilities and his potential to the fullest!
In many cases, the doctor may recommend that a child who is slowly gaining weight should be supplemented. If your expressed milk is suitable for this, you can express it with a breast pump or manually, and supplement your baby with a spoon, cup or syringe if your baby is not suckling well.
In some cases, your child with special needs may not be exclusively breastfed, and that's okay. Rest assured that any amount of your milk, whether breastfed, bottled or otherwise (breastfeeding, syringe, spoon, cup, Habermann cup) will greatly enhance your baby's health and development. Breast milk is exactly what you can give your baby and it's important for your morale!
Breastfeeding your baby with Down syndrome:
Benefits of breastfeeding for a baby with Down syndrome:
- Breast milk provides your baby with additional protection against infections and digestive problems that are more common in babies with Down syndrome.
- Breast sucking stimulates and strengthens the muscles of the lips, tongue and jaw of the baby, creating the basis for the development of speech. Mouth-tongue coordination also develops, giving your baby a real developmental advantage.
- Breastfeeding promotes closeness between mother and baby, creating a special bond. This helps the mother process the grief she may feel when she learns about Down's syndrome in a baby.
This helps the mother process the grief she may feel when she learns about Down's syndrome in a baby.
- Human milk is easier to digest in the body than formula baby food, which is especially important for digestive problems that are common in children with Down syndrome.
Recommendations for breastfeeding a baby with Down syndrome:
A mother's patience and adequate expectations are critical when breastfeeding a baby with Down syndrome. Low muscle tone, uneven tongue movements, and poor suckling can all affect a baby's ability to suckle at the breast.
Children with Down syndrome are often more sleepy and calm. Make sure your baby is getting enough nutrition and milk production is on track. This may require waking up every two hours for frequent feedings (at least 8-12 times a day).
Make sure your baby is fully awake before feeding. You can further stimulate him with touch throughout the feeding process.
Subdued light in the room will help the baby not close his eyes. You can try undressing your baby for skin-to-skin contact while feeding.
You can try undressing your baby for skin-to-skin contact while feeding.
Breast rotation during feeding is very helpful if your baby falls asleep on the breast. If this happens, immediately offer another breast. Keep repeating until the child is satisfied.
Pay attention to your baby's posture while breastfeeding. Place the baby on you belly to belly, make sure that his chin rests on your chest, and the baby's ear, shoulder and hip are in a straight line. Use extra pillows for support. See the Positioning section for more details.
If there is difficulty swallowing, the baby is choking, try to position the child so that his head is higher than his legs. Under-arm and relaxed feeding positions may be helpful. See the Positioning section for more information.
Low muscle tone can lead to sucking difficulties, including weakness of the tongue and lips. It is also important to have a stable head position when the baby is suckling. There are many effective ways to support your head, neck, and back. For example, the dancer's hand support (Dan-Cher position) is especially important for children with low muscle tone. Hold your hand in front of the breast you will be offering. Using the hand on the same side as the breast you are offering, grasp the breast with your thumb on one side of the chest, palm down, index finger out, and the other three fingers on the other side of the chest. Use your index finger to support your baby's lower jaw while feeding. As your baby's muscle tone improves through breastfeeding and maturity, he will be able to maintain his posture and breastfeed more effectively.
For example, the dancer's hand support (Dan-Cher position) is especially important for children with low muscle tone. Hold your hand in front of the breast you will be offering. Using the hand on the same side as the breast you are offering, grasp the breast with your thumb on one side of the chest, palm down, index finger out, and the other three fingers on the other side of the chest. Use your index finger to support your baby's lower jaw while feeding. As your baby's muscle tone improves through breastfeeding and maturity, he will be able to maintain his posture and breastfeed more effectively.
Babies with Down Syndrome may have a very large tongue that puts pressure on your nipple. This sometimes makes it difficult for the baby to latch onto the breast, as the nipple may be pushed out of the mouth.
If your baby is properly attached, you will be able to see his tongue engulfing the chest from below and resting on the lower gum. When you put the baby to the chest, make sure that his mouth is open wide and his tongue is sticking out forward and down.