Breast feeding a baby with down syndrome
Special Needs - La Leche League International
My new baby was born with special needs. Can I still breastfeed?First, congratulations on the birth of your new special baby. Second, congratulations on making the choice to breastfeed your new baby. How wonderful that you want to give your baby the gift of your milk. Babies with special needs experience special benefits from breastfeeding beyond the many advantages to typical newborns. Right now, you are probably struggling with conflicting feelings. Like most parents, you are joyful and excited to meet your new baby. At the same time, you may have feelings of disappointment, anger, helplessness, even guilt. Allow yourself time to process these feelings of grief, remember that your baby is a baby first and a baby with special needs second.
Babies born with Down syndrome, cleft lip or palate, cardiac problems, cystic fibrosis, a neurological impairment or other special needs will benefit from human milk even more than other babies. Human milk will boost your baby’s immune system, and is more easily digestible. It offers the perfect nutrition to keep your baby as healthy as possible, and be strong for any surgeries or treatments they may need. The special bond and breastfeeding hormones produced will help to keep you calmer and more in touch with your baby as well.
Often a baby with special needs is reluctant to take the breast; you and baby will need extra kinds of support while nursing. Let your medical team know that you are determined to breastfeed. Your partner, other family members and friends, your lactation consultant and your LLL Leader can back you up. If you want to give your milk to your baby, try to breastfeed right away. Be prepared to be patient, it may take a few weeks for your baby to learn how to properly latch on. If this isn’t working, start pumping as soon as possible after birth. You should pump as often as a baby would breastfeed, every two to three hours during each 24-hour period; setting an alarm will help keep you on schedule. The pumped milk can be given by other feeding methods. It’s best to avoid bottles and pacifiers if possible, because suckling at the breast is different than sucking on a bottle and will help to avoid nipple confusion.
The pumped milk can be given by other feeding methods. It’s best to avoid bottles and pacifiers if possible, because suckling at the breast is different than sucking on a bottle and will help to avoid nipple confusion.
Ask your Leader or board-certified lactation consultant about getting an at-breast nursing supplementer system. These systems hold your milk in a small bottle or bag with a thin tube attached to carry the milk to your baby. The tube may be taped to your breast, so your baby can get extra milk while learning to breastfeed. Or you may tape the tube to a finger and let the baby suck on your finger to get milk. (Your finger is more similar to your nipple than a bottle nipple.) Some health care providers may be unfamiliar with this method. Tell them about why it is important to you and your baby. Keep trying to breastfeed, if at all possible. It’s been proven by research that breastfeeding is less stressful for babies than bottle feeding, but your health care team may not know this. Also, the cuddling and skin-to-skin contact involved in breastfeeding provides the stimulation your baby needs to fully develop his capabilities.
Also, the cuddling and skin-to-skin contact involved in breastfeeding provides the stimulation your baby needs to fully develop his capabilities.
Oftentimes your doctor will want you to supplement a slow-gaining baby. See if your doctor will agree to have you use your own expressed breastmilk – you can pump or hand express your milk and give it by another feeding method if your baby is not sucking effectively.
In some cases, your baby with special needs may not become exclusively breastfed, and that’s okay. Rest assured that any amount of your milk received, by breast, pumped and given by bottle, or provided by another method (SNS, syringe, spoon, g-tube, Habermann Feeder) will greatly benefit your baby’s health and development. It’s something you alone can provide, which is good for your morale!
Breastfeeding your baby with Down syndrome:Benefits to breastfeeding your baby with Down syndrome:
- Breastmilk provides extra protection against infections and bowel problems, which are more common in babies with Down syndrome.

- The repetitive action during breastfeeding provides stimulation to strengthen your baby’s lips, tongue, and facial muscles; creating a building block for speech development. It will also improve mouth and tongue coordination giving your child a real developmental advantage.
- Breastfeeding promotes closeness between mom and baby, creating a special bond. This will especially help in the grieving process that can be associated with a Down syndrome diagnosis.
- Human milk is more easily digestible than formula and can help if your baby has digestive issues which is common in babies born with Down syndrome.
Extra patience and reasonable expectations are critical when breastfeeding a baby with Down syndrome. Low muscle tone, tongue thrusts, and a weak suck can affect the baby’s ability to breastfeed.
- Babies born with Down syndrome are often more sleepy and placid. To make sure your baby gets the nutrients that she needs and establish your milk supply, it may be necessary to wake her every two hours for frequent feedings (at least 8-12 times per day).
 Make sure your baby is fully awake before feeding, you can do this with extra touch and stimulation throughout the feeding session. Also dimming the lights in the room helps to keep your baby’s eyes open, or you can try undressing your baby and using skin to skin contact to keep your baby alert and aware.
Make sure your baby is fully awake before feeding, you can do this with extra touch and stimulation throughout the feeding session. Also dimming the lights in the room helps to keep your baby’s eyes open, or you can try undressing your baby and using skin to skin contact to keep your baby alert and aware. - Switch nursing is very beneficial if your baby falls asleep at the breast. If your baby starts to lose interest in the breast, break the latch and offer the other breast. Keep repeating until he seems satisfied.
- Pay extra attention to positioning your baby at your breast. Try to keep your baby’s body close to your body with chin and chest at breast level with his ear, shoulder and hip in a straight line and use extra pillows for support. See Positioning for more information.
- If gulping and choking are a problem, try positioning your baby so that his head is higher than his bottom. The football and laid-back position can be helpful. See Positioning for more information.

- Poor muscle tone may make it difficult for your baby to latch on well, including reduced muscle strength in their tongue and lips. It is very important to offer good head support during breast feeding. There are a variety of ways you can hold your baby to support his head, neck, and back. The Dancer hand position is especially beneficial to babies with low muscle tone. Hold your arm opposite the breast you’ll be offering. Using the hand on the same side as the breast you are offering, cup your breast with your thumb on one side of the breast, palm beneath, index finger pointing outward, and the other three fingers on the other side of the breast. Use your index finger to support your baby’s lower jaw while nursing. As your baby’s muscle tone improves through breastfeeding and maturity, he will become able to support himself and breastfeed more effectively.
- Babies with Down syndrome may have a protruding tongue that can push against your nipple. This may pose a challenge for your baby when latching on, as he may push the nipple out of his mouth.

- If your baby is latched on properly, you should be able to see his tongue cupped under the breast, resting on his lower gum. When you are latching your baby onto the breast, watch for his mouth to open wide, with his tongue forward and down. To encourage your baby to bring his tongue forward: use your index finger to press down softly on the baby’s chin while he latches on. This opening of the jaw will cause the tongue to protrude further out of his mouth. Don’t be disheartened if your baby needs some initial encouragement to keep his tongue down while latching on. Here is an exercise you can try to promote cupping of the tongue; 1) Place your index finger on the center of your baby’s tongue, encouraging the tongue to form the shape of a trough. 2) Push down on his tongue while gradually pulling your finger out of his mouth. 3) Repeat this exercise several times before latching your baby onto the breast.
Find an LLL Leader or Group Near You
Feeding Breastmilk From A Bottle
Pumping
Hand Expressing
Working With Your Child’s Doctor
Published January 2018, revised October 2020.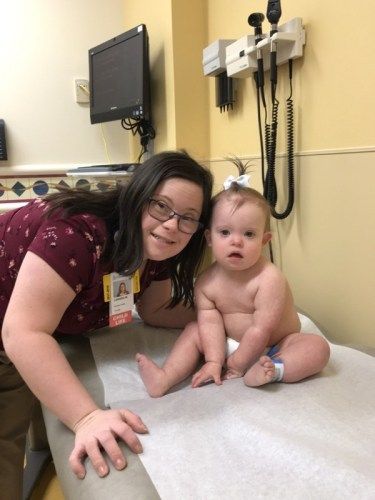
Breastfeeding an infant with Down syndrome
How does breastfeeding help my baby?
Breast milk:
- is more nutritious and easier to digest than formula
- gives immune protection not found in formula
- lowers risk of infections
- helps minimize allergies
- helps the digestive system mature; protects against some bowel problems
- lowers risk of Sudden Infant Death Syndrome (SIDS)
- promotes eye and brain development
- is more economical than formula
When you breastfeed:
- you crate a special bond with your baby
- your baby's mouth and tongue coordination improves, which will help speech skills
- you burn more calories than usual
- your uterus may shrink toward its pre-pregnancy size more quickly
For more details, see the education sheet "Breastfeeding."
Are there special benefits for babies with Down syndrome?
Babies with Down syndrome have a higher risk of infection—and breast milk helps protect again infection more than formula does. Whenever a mother is exposed to a virus, her body makes antibodies that protect her from getting that infection again. She passes these antibodies on to her baby in her breast milk.
Whenever a mother is exposed to a virus, her body makes antibodies that protect her from getting that infection again. She passes these antibodies on to her baby in her breast milk.
Because breast milk is easy to digest, stools are very soft and easy to pass. This may be helpful for infants who have bowel problems related to Down syndrome.
Infants with Down syndrome usually have low muscle tone. Breastfeeding offers extra stimulation through skin-to-skin contact.
What challenges could my baby have with breastfeeding?
- low muscle tone
- non-rhythmic suck
- arching of the body
- over-sensitive to stimulation
- weak reflexes for sucking, swallowing, and gagging
- may tire more easily and not nurse long enough to get the hind milk (which has the most calories)
How can I help my baby breastfeed?
Feed often: 8 or more times in 24 hours. You may need to wake your baby to feed. Look for mouth or hand movement even if the baby's eyes are closed. This usually means the infant is in a lighter sleep and can wake up more easily. Other ways to wake the baby: undress for diaper change, or make skin-to-skin contact.
This usually means the infant is in a lighter sleep and can wake up more easily. Other ways to wake the baby: undress for diaper change, or make skin-to-skin contact.
A baby with low muscle tone usually sucks better when the head and bottom are level, or close to it. Support your baby using pillows on your lap.
If the baby tends to arch the body, try to hold the body flexed, with knees bent and spine rounded. Swaddling in a blanket in a flexed position can help.
If your baby does not start sucking, express some breast milk onto the nipple by hand, or use a pump to get "let-down" started. This can encourage the infant to suck.
Once baby starts sucking, look for jaw, ear, and temple movement. If not seen, the infant's suck is probably not as strong as it needs to be.
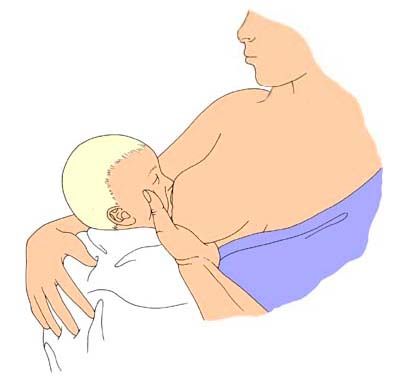
Sometimes the dancer-hand position (see picture below) can be used to support the infant's chin.
Slide the hand under your breast forward, so you are supporting the breast with 3 fingers rather than 4. Form a U-shape with your thumb and forefinger to cradle your baby's chin. This will help your baby press the nipple and areola between the gums.
Form a U-shape with your thumb and forefinger to cradle your baby's chin. This will help your baby press the nipple and areola between the gums.
If the infant has a non-rhythmic suck, try using a rocking chair, and offer extra chin support while breastfeeding.
Breastfeeding in calm surroundings with few distractions can help the infant who easily overreacts to stimulation.
A breast pump can boost your milk supply while you get started. Feel free to ask your health care provider or lactation specialist.
How will I know if my baby is getting enough milk?
Your baby should nurse every 2 or 3 hours (8 to 12 times in 24 hours), including some feedings during the night. Here are some things to watch for:
Watch for this pattern in your baby's urine and stools during the first week after birth:
| Days after birth | Wet diapers (at least this many in 24 hrs) | Stool color | Number of stools (at least this many in 24 hrs) |
| 1st day | 1 | greenish-black | possible stool smears in first 24 hours |
| 2nd day | 2 | 1 to 2 stools | |
| 3rd day | 3 | stool turns yellower, softer, and seedier | 2 to 4 stools |
| 4th day | 4 | 3 to 5 stools | |
| 5th day | 5 | yellow, soft, seedy | 3 to 5 stools |
What else do I need to know?
Take care of yourself. You will be spending a lot of time each day feeding your baby. Patience is important.
You will be spending a lot of time each day feeding your baby. Patience is important.
Get comfortable before starting a feeding. Find a special place—perhaps where you can look out of a window. Cuddle and chat with your baby while feeding.
Keep what you need at hand—maybe the phone and something to drink. You may want to listen to music or a relaxing program. If you are comfortable and well supported physically and emotionally, you will have more energy to support your baby.
Questions?
This sheet is not specific to you and your baby, but provides general information. If you have any questions, please talk to the nurse or lactation specialist.
At home, if you cannot tell if your baby is getting enough milk, or if you have other concerns, please call the clinic. If you need a pump or a lactation specialist, call:
Hollister at 1-800-323-4060, or
Medela at 1-800-835-5968.
La Leche League, International provides help and support to breastfeeding mothers over the phone and in support groups. For information, call 1-800-525-3243.
For information, call 1-800-525-3243.
Children's Minnesota
Last reviewed 8/2015
Back To Top
My newborn was born with special needs. Can I breastfeed?
Translation: Tatyana Tutatchikova
Editor: Evgeniya Champalova, Maria Sorokina
Proofreader: Tatyana Romanova
So, congratulations on your unique birth to your babies! And also because you decide to breastfeed him, because children with special needs receive special benefits from breast milk. Right now you are probably having conflicting feelings. Like most parents, you are excited to meet your newborn. At the same time, you may feel frustrated, angry, helpless, and even guilty. Give yourself time to accept these and other unfortunate feelings. Remember that your child is first and foremost just a baby, and only then a child with special needs.
Babies born with Down syndrome, cleft lip or palate (“cleft palate”), heart problems, cystic fibrosis, neurological problems, or other special needs need even more breast milk than other babies. Breast milk strengthens the baby's immunity and is easier to digest in the body. It is also optimal nutrition to support his health. This is especially important because your baby may need surgery or long-term care. The special bond between mother and baby and breast milk hormones help keep you calm and in touch with your baby.
Breast milk strengthens the baby's immunity and is easier to digest in the body. It is also optimal nutrition to support his health. This is especially important because your baby may need surgery or long-term care. The special bond between mother and baby and breast milk hormones help keep you calm and in touch with your baby.
Often a child with special needs is reluctant to latch on; in this case, you and your baby will need additional support during feeding. Let your health care provider know that you are determined to breastfeed. Your partner, other family members and friends, your lactation consultant or your LLL volunteer consultant can support you. Try to start breastfeeding right now. Be patient, it may take a few weeks for your baby to learn how to latch on properly. If your baby is still having difficulty sucking milk out of the breast, start expressing with a breast pump as soon as possible after birth. You should express milk as often as a baby would suck, that is, every two to three hours during the day; the alarm clock will help you keep a schedule of pumping and feeding. Expressed milk is best given to a child from non-sucking objects (spoon, cup or syringe). It is best to avoid bottles and pacifiers because breastfeeding is different from bottle sucking and nipple confusion can occur.
Expressed milk is best given to a child from non-sucking objects (spoon, cup or syringe). It is best to avoid bottles and pacifiers because breastfeeding is different from bottle sucking and nipple confusion can occur.
Ask your LLL Volunteer Consultant or Lactation Consultant about the possibility of using a breastfeeding system. Such a system is a container for breast milk with thin tubes. The tube is attached to your breast so your baby can get extra milk while he or she learns to suckle. Or you can attach a straw to your finger, allowing your baby to suck on it and get breast milk at the same time. (An adult's finger looks more like your nipple than a bottle nipple.) Some healthcare professionals may not be familiar with this method. Explain why this is important to you and your baby. Continue breastfeeding if possible. Studies show that breastfeeding is less stressful for the baby than bottle feeding; your doctor may not think about it. When you breastfeed, you hug your baby and touch him “skin to skin”, and this helps him develop his abilities and his potential to the fullest!
In many cases, a doctor may recommend supplementary feeding to a child who is slowly gaining weight. If your expressed milk is suitable for this, you can express it with a breast pump or manually, and supplement your baby with a spoon, cup or syringe if your baby is not suckling well.
If your expressed milk is suitable for this, you can express it with a breast pump or manually, and supplement your baby with a spoon, cup or syringe if your baby is not suckling well.
In some cases, your baby with special needs may not be exclusively breastfed, and that's okay. Rest assured that any amount of your milk, whether breastfed, bottled or otherwise (breastfeeding, syringe, spoon, cup, Habermann cup) will greatly enhance your baby's health and development. Breast milk is exactly what you can give your baby and it's important for your morale!
Breastfeeding your baby with Down syndrome:
Benefits of breastfeeding for a baby with Down syndrome:
- Breast milk provides your baby with additional protection against infections and digestive problems that are more common in babies with Down syndrome.
- Breast sucking stimulates and strengthens the muscles of the lips, tongue and jaw of the baby, creating the basis for the development of speech. Mouth-tongue coordination also develops, giving your baby a real developmental advantage.
Mouth-tongue coordination also develops, giving your baby a real developmental advantage.
- Breastfeeding promotes closeness between mother and baby, creating a special bond. This helps the mother process the grief she may feel when she learns about Down's syndrome in a baby.
- Human milk is easier to digest in the body than formula baby food, which is particularly important in the presence of digestive problems that are common in children with Down's syndrome.
Recommendations for breastfeeding a baby with Down syndrome:
A mother's patience and adequate expectations are critical when breastfeeding a baby with Down syndrome. Low muscle tone, uneven tongue movements, and poor suckling can all affect a baby's ability to suckle at the breast.
Children with Down syndrome are often more sleepy and calm. Make sure your baby is getting enough nutrition and milk production is on track. This may require waking up every two hours for frequent feedings (at least 8-12 times a day).
Make sure your baby is fully awake before feeding. You can further stimulate him with touch throughout the feeding process.
Subdued light in the room will help the baby not to close his eyes. You can try undressing your baby for skin-to-skin contact while feeding.
Breast rotation during feeding is very helpful if your baby falls asleep on the breast. If this happens, immediately offer another breast. Keep repeating until the child is satisfied.
Pay attention to your baby's posture while breastfeeding. Place the baby on you belly to belly, make sure that his chin rests on your chest, and the baby's ear, shoulder and hip are in a straight line. Use extra pillows for support. See the Positioning section for more details.
If there are problems with swallowing, the baby is choking, try to position the child so that his head is higher than his legs. Under-arm and relaxed feeding positions may be helpful. See the Positioning section for more information.
Low muscle tone can lead to sucking difficulties, including weakness of the tongue and lips. It is also important to have a stable head position when the baby is suckling. There are many effective ways to support your head, neck, and back. For example, the dancer's hand support (Dan-Cher position) is especially important for children with low muscle tone. Hold your hand in front of the breast you will be offering. Using the hand on the same side as the breast you are offering, grasp the breast with your thumb on one side of the chest, palm down, index finger out, and the other three fingers on the other side of the chest. Use your index finger to support your baby's lower jaw while feeding. As your baby's muscle tone improves through breastfeeding and maturity, he will be able to maintain his posture and breastfeed more effectively.
Image from https://www.lllc.ca Babies with Down Syndrome may have a very large tongue that puts pressure on your nipple. This sometimes makes it difficult for the baby to latch onto the breast, as the nipple may be pushed out of the mouth.
If your baby is properly attached, you will be able to see his tongue engulfing the breast from below and resting on the lower gum. When you put the baby to the chest, make sure that his mouth is open wide and his tongue is sticking out forward and down. To encourage your baby to move their tongue forward, use your index finger to gently press down on your baby's chin as he applies. This opening of the jaw will cause the tongue to protrude even more out of the mouth. Don't be discouraged if your baby needs some initial help to keep his tongue over his teeth during latch on.
Here is an exercise that can help your baby's tongue move effectively:
1) Place your index finger in the center of your baby's tongue.
2) Press on his tongue, gradually pulling your finger out of his mouth.
3) Repeat this exercise several times before bringing the baby to the breast.
Breastfeeding and Down syndrome
donate milk
Find milk
Down syndrome is the most common hereditary disease. The birth rate of children with Down syndrome ranges from 1:600 to 1:900.
The birth rate of children with Down syndrome ranges from 1:600 to 1:900.
Caring for a baby with Down's syndrome can be challenging, but the patience and perseverance of parents in achieving goals, as well as the growth and development of the child, the formation of muscle tone, makes it possible to establish breastfeeding. You and your baby can experience all the benefits of breastfeeding.
Some of these benefits are:
-
Protection against infections. Children with Down syndrome are particularly susceptible to respiratory tract infections, ear infections, thyroid disease, and cancer. Unlike artificial infant formula, breast milk, which contains living cells and antibodies, has a protective effect against all infections. When a breastfeeding mother encounters a virus, her body produces antibodies that help prevent re-infection with this infection. These specific antibodies, together with breast milk, enter the body of the child, thereby protecting him as well.

-
Improving the functioning of the child's digestive system. Children with diabetes often have digestive problems due to weak gastrointestinal muscle tone. Unlike formula, breast milk is easier to digest and helps relieve digestive problems like constipation.
-
Reducing the risk of allergies and skin problems. Children with Down syndrome often have more skin problems than healthy children, such as dry skin, eczema, seborrhea, and cheilitis (a benign inflammatory disease of the lips). They are also more prone to food allergies. Breast milk reduces the incidence of all these diseases.
-
Development of the speech apparatus. Children with Down syndrome have various anatomical features of oral development, such as an open bite and a relatively large tongue that may not fit well in the mouth. This can affect proper attachment to the breast and lead to problems with breastfeeding. However, the sucking movements necessary for feeding, training and thereby strengthening the muscles of the speech apparatus and tongue, further contribute to the proper development of speech.
-
Psycho-emotional development. Breast milk contains docosahexaenoic acid (DHA), an omega-3 fatty acid not found in cow's milk. This fatty acid DHA plays an important role in the development of the brain and eyes. Several studies have shown that breastfed babies tend to have 8 IQ points higher than their formula-fed peers. This increased brain stimulation is especially beneficial for children with Down syndrome.
-
Additional stimulation. The extra skin-to-skin contact that goes hand in hand with breastfeeding babies provides extra stimulation to reach their full potential.
-
Proximity of the child's matter. Feeding a child with Down syndrome is not only an opportunity to provide skin-to-skin contact, but also a way to spend more time with the child, hug him. Mothers of special children often feel helpless in caring for such babies, so breastfeeding and breastfeeding can help a mother feel more confident because they are doing something meaningful, important for their child to ensure their health and development.
 If, for some reason, the mother has not been able to breastfeed, it is necessary to provide additional bodily contact between the child and the mother - an intimacy that helps both mother and child develop.
If, for some reason, the mother has not been able to breastfeed, it is necessary to provide additional bodily contact between the child and the mother - an intimacy that helps both mother and child develop. -
Acquisition of maternal childcare skills. The doctor will tell you about the ways of caring for the child in the first days after childbirth - these are skills that will be useful to you in raising a child for many years. However, the mother needs to learn to understand her child correctly on her own. In this, she is helped by the “mother hormone” - oxytocin, which is released during breastfeeding. Mom rests during feeding and is able to care for and understand the needs of the baby better.
-
Feeding during sickness and comfort. Children with Down syndrome are prone to diseases such as heart defects, oncology, vision problems. Therefore, a medical examination, which includes various procedures or operations, is carried out more often in children with DM.
 Breastfeeding helps the baby survive stress during painful procedures, calm down during illness, and it is easier to endure it.
Breastfeeding helps the baby survive stress during painful procedures, calm down during illness, and it is easier to endure it.
Babies with Down syndrome have difficulty breastfeeding due to anatomical and medical conditions such as inability to suckle and control swallowing, reduced muscle tone, and various diseases. Children with diabetes who have a number of diseases need additional medical procedures and surgical interventions that involve the separation of mother and child for some time.
Down's syndrome can cause hypertonicity (excessive tension in a specific muscle group) or hypotonicity (weakened muscle condition), leading to problems with breastfeeding.
If the baby does not suckle effectively, he will quickly tire, as a result of which he cannot be at the breast long enough to suck out the richer hindmilk necessary for weight gain. "Lazy suckers" need more help from the nursing staff or a lactation consultant to solve this problem.
Muscle tone in children with Down syndrome leads to a number of problems with breastfeeding. You can experiment with different positions to find the best position for both mom and baby. A rocking chair helps many mothers during breastfeeding, the motion sickness process helps mother and baby relax during feeding.
You can experiment with different positions to find the best position for both mom and baby. A rocking chair helps many mothers during breastfeeding, the motion sickness process helps mother and baby relax during feeding.
Even if you can find a comfortable position for feeding your baby, you may have problems with the correct attachment of the baby to the breast, due to the characteristics of the bite and large tongue. Children with hypotension are recommended to be fed by laying them on a pillow so that the body and head are at the same level. It is important to keep an eye on the baby's chin so that the grip is not lost and there are no gaps between the baby's chest and mouth.
Children with hypertonicity should be helped to relax, try to position them so that the back is rounded, the knees are bent and brought to the stomach. Sometimes loose swaddling is necessary to maintain this body position.
You can check whether the baby has received enough breast milk by counting the number of urination and the frequency of the baby's stools. A child's weight is the best indicator of a child's adequate nutrition and should be closely monitored.
A child's weight is the best indicator of a child's adequate nutrition and should be closely monitored.
It is important to remember that even if breastfeeding has not been arranged, it is possible to feed the baby with bottled expressed breast milk or alternative feeding devices (eg breastfeeding system). Breastmilk offers many advantages over formula and solves many problems with feeding and caring for special babies. Even if your baby is mixed-fed (formula and breast milk), he receives the nutrition and benefits that are important for his growth and development from breast milk.
Lactation support with a breast pump allows you to consider different options for feeding your baby. Some children with Down's syndrome are unable to breastfeed, so mothers maintain the proper level of lactation exclusively by pumping.
All breast pumps are different. Moms who need to pump often will benefit from a double electric breast pump. Some of them may be provided by medical organizations and included in the cost of medical insurance (not included in Russia - ed.











