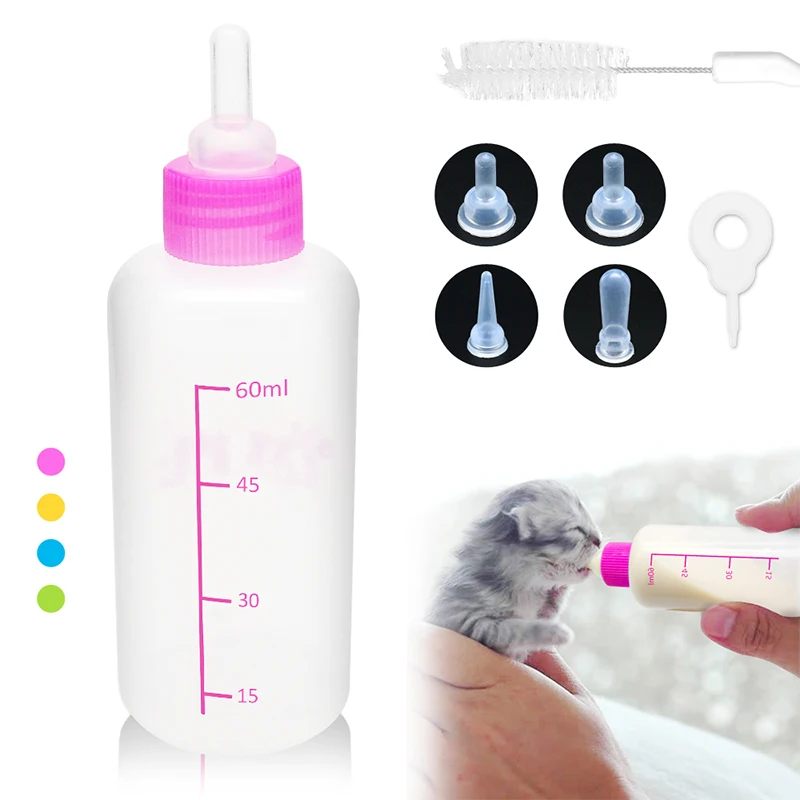
Burping of baby after feeding
Burping Your Baby (for Parents)
Reviewed by: Madhu Desiraju, MD
Primary Care Pediatrics at Nemours Children's Health
en español Hacer eructar a su bebé
An important part of feeding a baby is burping. Burping helps to get rid of some of the air that babies tend to swallow during feeding. Not being burped often and swallowing too much air can make a baby spit up, or seem cranky or gassy.
How to Burp Your Baby
When burping your baby, repeated gentle patting on your baby's back should do the trick. Cup your hand while patting — this is gentler on the baby than a flat palm.
To prevent messy cleanups when your baby spits up or has a "wet burp," you might want to place a towel or bib under your baby's chin or on your shoulder.
Try different positions for burping that are comfortable for you and your baby. Many parents use one of these three methods:
- Sit upright and hold your baby against your chest. Your baby's chin should rest on your shoulder as you support the baby with one hand.
With the other hand, gently pat your baby's back. Sitting in a rocking chair and gently rocking with your baby while you do this may also help.
- Hold your baby sitting up, in your lap or across your knee. Support your baby's chest and head with one hand by cradling your baby's chin in the palm of your hand. Rest the heel of your hand on your baby's chest, but be careful to grip your baby's chin, not the throat. Use the other hand to pat your baby's back.
- Lay your baby on your lap on his or her belly. Support your baby's head and make sure it's higher than their chest. Gently pat your baby's back.
If your baby seems fussy while feeding, stop the session, burp your baby, and then begin feeding again. Try burping your baby every 2 to 3 ounces (60 to 90 milliliters) if you bottle-feed and each time you switch breasts if you breastfeed.
Try burping your baby every ounce during bottle-feeding or every 5 minutes during breastfeeding if your baby:
- tends to be gassy
- spits a lot
- has gastroesophageal reflux (GER)
- seems fussy during feeding
If your baby doesn't burp after a few minutes, change the baby's position and try burping for another few minutes before feeding again. Always burp your baby when feeding time is over.
Always burp your baby when feeding time is over.
To help prevent the milk from coming back up, keep your baby upright after feeding for 10 to 15 minutes, or longer if your baby spits up or has GERD. But don't worry if your baby spits sometimes. It's probably more unpleasant for you than it is for your baby.
Sometimes your baby may awaken because of gas. Picking your little one up to burp might put them back to sleep. As your baby gets older, don't worry if your child doesn't burp during or after every feeding. Usually, it means that your baby has learned to eat without swallowing too much air.
Babies with colic (3 or more hours a day of continued crying) might have gas from swallowing too much air during crying spells, which can make the baby even more uncomfortable. Check with your pediatrician before giving your baby anti-gas drops.
Reviewed by: Madhu Desiraju, MD
Date reviewed: June 2022
How and When to Burp Your Baby
A key part of your baby's feeding routine is burping him. Your baby may swallow lots of air while feeding, and burping can help remove some of that gassiness and ease his fussiness. It may also help prevent him from spitting up.
Your baby may swallow lots of air while feeding, and burping can help remove some of that gassiness and ease his fussiness. It may also help prevent him from spitting up.
Find out how to burp your baby, and pick up some tips on making burping more effective.
How to Burp Your Baby: Positions to Try
Here are three burping techniques that have stood the test of time. After trying each of them out, you’ll probably settle on one that works best for you and your baby:
Hold your baby upright against your chest with his chin on your shoulder, all the while supporting him with one hand as you gently pat his back with your other hand.
Place your baby on your lap with him sitting up, all the while supporting his head and chest with one hand while you softly pat his back with your other hand.
Lay your baby on your lap with his belly faced down, all the while supporting his head so it’s higher than his chest, and pat his back.

Tips for Burping Your Baby
Try these tips the next time you need to burp your baby:
Use repeated, gentle pats on her back.
Cup your hand slightly as you pat her, as this is gentler than using a flattened palm.
Drape a towel or bib over your lap or shoulder to protect your clothing as you burp your baby, in case your baby spits up (sometimes called “wet burps”).
Now that you know how to burp your baby, and these tips help you do so effectively, here’s a helpful visual guide:
How Long Should You Burp Your Baby?
There is no specific length of time needed for burping your baby. The more important factor is how often you burp him. With that in mind, burp your baby frequently throughout feeds, even when it looks like he doesn’t need to be burped.
Waiting until after a feeding to burp your baby may mean your little one has swallowed too much air and may be fussier, so it’s better to stop feeding every so often and try to burp your little one. You could also try paced bottle feeding, which slows the flow of breast milk or formula from the bottle, which could help prevent gas.
You could also try paced bottle feeding, which slows the flow of breast milk or formula from the bottle, which could help prevent gas.
Here are some tips for burping your baby during a feeding:
If you’re bottle feeding (which can include formula feeding or offering expressed breast milk), you’ll want to burp him after every two to three ounces of milk.
If you’re breastfeeding, burp your baby each time he switches breasts. Some breastfed babies may not need to burp as often, as they may not swallow as much air.
If your baby hasn’t burped after some time, go back to feeding. Not every baby burps every time you want him to burp.
If your baby shows any of the following signs, you may want to burp him more regularly — for example, after every ounce of milk during bottle feeding or every five minutes during breastfeeding:
He is gassy
He spits up frequently
He has Gastroesophageal Reflux Disease (GERD)
He seems very fussy.

After a feeding is over, keep your baby in an upright position for 10 to 15 minutes. This can help prevent him from spitting up. You may need to burp him longer if he does spit up or has been diagnosed with GERD.
Other Instances When Burping Your Baby Might Be Beneficial
If your sleeping baby wakes suddenly and you suspect it may be because of gas, burping her might help relieve the pressure and help her fall back asleep.
A colicky baby, who may cry for three or more hours per day, might have gas from all the air she’s swallowed during one of these crying spells. You may consider burping her to see if it helps comfort her.
We hope these tips can help you burp your baby during feeding time to ensure she’s more comfortable.
Don’t forget to stock up on plenty of diapers, which you will surely need after all these feedings and burpings. Get rewarded for your Pampers purchases by using the Pampers Club app to earn rewards like coupons, gifts, and gift cards.
Why does the baby spit up after feeding?
search support iconSearch Keywords
Regurgitation is a common condition in newborns and infants and is most often a normal variant. However, it is not uncommon for parents to worry if their baby is spitting up frequently, believing that it is due to nutritional or health problems in general. Sometimes these fears are not unfounded, and regurgitation really has a pathological origin. What is its cause and when should you really consult a doctor about this?
Regurgitation - Return of a small amount of food (uncurdled or partially curdled milk) from the stomach up the digestive tract: into the esophagus and further into the oral cavity. According to statistics, at least 1 time during the day, at least 50% of babies from 0 to 3 months old can spit up, more than 60% of children 3-4 months old, and in 5% of children spit up continues up to the year 1 .
Regurgitation in newborns is considered a physiological process. It is caused by a number of factors, including:
It is caused by a number of factors, including:
- Features of the structure of the upper digestive tract in babies
- In newborns and infants up to a year of life, the stomach has a spherical shape. It holds a small amount of food, besides, the release from it into the duodenum is slower in comparison with children after the year 2 .
- Weakness of the lower esophageal sphincter that separates the esophagus from the stomach
- Normally, the lower esophageal sphincter should tightly "close" the esophagus, allowing food to pass into the stomach and not allowing it to enter back into the upper digestive tract. However, in young children (up to a year), the muscles of the esophageal sphincter are poorly developed, and it does not do its job very well 2 .
- Slow movement of food through the gastrointestinal tract
- The neuromuscular system of newborns is immature. It does not ensure the proper movement of food through the esophagus, causing regurgitation.
One of the important risk factors contributing to regurgitation in newborns is aerophagia. This is the swallowing of large amounts of air during feedings. This happens when the baby is not properly attached to the breast, the mother has a lack of breast milk, or the bottle is in the wrong position in the child who receives the mixture. The size of the opening in the nipple also matters - if it is too large, the newborn swallows a lot of air 3 .
With aerophagia, the baby becomes capricious, restless immediately after feeding. Noticeable bloating. If the baby spits up immediately after a feed, the milk (or formula) remains practically fresh, uncurdled 3 .
Promotes regurgitation after feeding and a predominantly horizontal position of the baby during the day, combined with relatively high intra-abdominal pressure 4 . Therefore, the correct position of the baby after feeding is so important. To avoid regurgitation of an excessive amount of stomach contents, after feeding, it is necessary to hold the baby in an upright “column” position for some time (10-20 minutes), lightly patting on the back and allowing excess air to “exit”.
Regurgitation in many newborns can be provoked by other situations in which pressure in the abdominal cavity increases and stomach contents are thrown into the esophagus, in particular 3 :
- tight swaddling;
- stool disorders, in particular constipation;
- long, forced cry and some others.
Want to avoid common feeding problems?
Start with a baby bottle with an anti-colic system that helps you avoid common feeding problems such as colic, gas and spitting up*
How can you tell the difference between normal spitting up and vomiting?
Sometimes regurgitation is considered a manifestation of disorders in the digestive tract of children. Due to the constant reflux of acidic stomach contents into the upper sections, inflammation and other complications may develop, including growth retardation, a decrease in hemoglobin levels, and others. Therefore, it is important for parents to understand where the line is between physiological and pathological regurgitation 1 .
Therefore, it is important for parents to understand where the line is between physiological and pathological regurgitation 1 .
If the mother is worried that her baby is spitting up, keep track of when this happens and count the total number of spit ups per day. Normally, regurgitation usually occurs after eating (the child burps after each feeding), lasts no more than 20 seconds and repeats no more than 20-30 times a day. With pathology, the problem manifests itself at any time of the day, regardless of when the baby was fed. Their number can reach 50 per day, and sometimes more 1 .
The amount of discharge during regurgitation also matters. With normal, physiological regurgitation, it is approximately 5 - 30 ml. If this volume fluctuates between 50 and 100 ml, it is already defined as profuse vomiting. When the range of the jet of vomit is up to 50 cm, doctors talk about "vomiting a fountain." A variant of atonic vomiting is possible, when the contents of the stomach flow "sluggishly". It occurs with atony of the stomach (decrease in muscle tone of the stomach wall) and disruption of the esophagus 1 .
It occurs with atony of the stomach (decrease in muscle tone of the stomach wall) and disruption of the esophagus 1 .
Vomiting in babies is a warning sign. Doctors are especially alarmed by repeated vomiting, a fountain, with an admixture of bile, in combination with constipation. Vomiting can lead to the development of dehydration, acid-base imbalance and other consequences, therefore, if it occurs, you should urgently contact a pediatrician to find out the cause and begin treatment. A doctor's consultation is necessary if the child is spitting up a lot (more than 15-30 ml at a time), with a frequency of more than 50 episodes per day 1.3 .
Physiological regurgitation: symptoms
Regurgitation in newborns, which is considered a normal variant and does not cause concern to pediatricians 3 :
- usually continues for a certain period of time;
- is characterized by slow, "passive" leakage; if the baby spits up a fountain, it is better to consult a doctor;
- has a sour smell of curdled milk;
- occurs without the participation of muscles - the baby does not strain during regurgitation;
- does not affect the general well-being of the baby.

How to help a newborn who spit up often?
If the baby is healthy, no medication is prescribed for spitting up. To help the child allow simple measures based on lifestyle changes and feeding.
- Frequent feeding of the baby
It is known that the baby is more prone to spit up if his stomach is full. To improve the situation, it is recommended to feed the baby more often, avoiding oversaturation, best of all - on demand 5 .
- Correct feeding technique
Every feeding, the mother must ensure that the baby does not swallow too much air during suckling. When sucking, there should be no loud, smacking, clicking sounds. You also need to control that the baby captures the nipple along with the areola.
- Choosing the right bottle and nipple
If the newborn is bottle-fed and receiving formula, it is important to choose the right bottle and nipple. The hole in it should be such that the milk flows out in drops, and not in a stream. The nipple must not be filled with air
The hole in it should be such that the milk flows out in drops, and not in a stream. The nipple must not be filled with air New Anti-colic bottle with AirFree valve
The AirFree valve prevents air from entering the baby's stomach.
- Baby standing upright after eating
To allow air that has entered the digestive tract during meals to escape, it is important to keep the newborn upright for 10-20 minutes after feeding 4 .
- Ensure the correct position of the baby during sleep
To reduce the negative impact of the acidic contents of the stomach on the esophagus, it is necessary to put the baby to sleep in the supine position. The side or prone position, which many pediatricians used to recommend, is no longer recommended. It was found to be associated with an increased risk of sudden infant death syndrome 5 .
If parents notice alarming symptoms, such as spitting up too often or large volume, etc.
 , it is important to consult a pediatrician without delay. This will allow you to identify the real problem in time and help the baby grow up healthy and happy.
, it is important to consult a pediatrician without delay. This will allow you to identify the real problem in time and help the baby grow up healthy and happy.
References1 Zakharova I. N., Andryukhina E. N. Regurgitation and vomiting syndrome in young children // Pediatric pharmacology, 2010. V. 7. No. 4.
Nagornaya 2900 V., Limarenko M. P., Logvinenko N. G. Experience with the use of domperidone in suspension in young children with regurgitation syndrome // Child Health, 2013. No. 5 (48).
3 Zakharova IN Regurgitation and vomiting in children: what to do? //Pediatrics. Supplement to Consilium Medicum, 2009. No. 3. S. 58-67.
4 Zakharova I. N., Sugyan N. G., Pykov M. I. Regurgitation syndrome in young children: diagnosis and correction // Effective pharmacotherapy, 2014. No. 3. P. 18-28.
5 Vandenplas Y. et al. Pediatric gastroesophageal reflux clinical practice guidelines: joint recommendations of the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN) and the European Society for Pediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN) //Journal of pediatric gastroenterology and nutrition.
 2009; 49(4): 498-547.
2009; 49(4): 498-547. You are leaving the Philips Healthcare (“Philips”) official website. Any links to third party websites that may be included on this site are provided solely as a convenience to you. Philips makes no warranties regarding any third party websites or the information they contain.
I understand
You are about to visit a Philips global content page
Continue
You are about to visit the Philips USA website.
I understand
How to help the baby when regulating
Support Support iconKeywords for searching
Home Home ›!! How to help a child in sprinkling
Home Home ›!!
Breastfeeding is a very special time for a mother and her newborn baby. Together with the feeling of closeness and affection that feeding brings, understanding its nuances cannot but raise many questions, including the question of how to help an infant spit up. Regurgitation in a newborn is by no means always the result of a simple pat on his back.
Regurgitation in a newborn is by no means always the result of a simple pat on his back.
In this article, we'll talk about the basics of helping a newborn spit up, as well as other questions you may have about spitting up.
Why do babies spit up?Let's get this straight: Why do newborns need to burp in the first place? During feeding, children usually swallow extra air - this is called aerophagia. Spitting up helps prevent this air from entering the intestines, as well as vomiting, gas, and crankiness in the baby. To avoid the return of milk after feeding, you should give the baby the opportunity to burp more often.
How to help a newborn spit up?
During the first six months, the baby should be kept upright in a column for 10-15 minutes after each feed. This will help keep the milk in his stomach, but if the baby occasionally burps anyway, parents need not worry. While carrying your baby in an upright position, you can put a baby diaper or wipes on your shoulder to keep your clothes clean.
We've already seen why spitting up is important, now let's find out how to help your baby spit up. Parents should gently pat the baby on the back with a hand folded in a handful until he burps. Folding your hand into a handful is important because clapping with a flat palm may be too strong for an infant.
Every baby is different and there is no one right position for spitting up. To get started, you can try the following options:
- Sitting position with the baby on the chest. In this position, the parent puts the baby's head with his chin on his shoulder and with one hand supports the baby under the back. With the other hand, you can gently pat the baby on the back. This method is most effective in a rocking chair or when the baby is gently rocking.
- Holding a child upright on one's legs. With one hand, parents can hold the baby by the back and head, supporting his chin and placing his palm on the baby’s chest, with the other hand, you can gently pat him on the back.
 At the same time, it is important to be careful: do not press the child on the throat, but only gently support his chin.
At the same time, it is important to be careful: do not press the child on the throat, but only gently support his chin. - Holding a baby lying on his tummy in his lap. Make sure his head is above his chest and gently pat your baby on the back until he burps.
Here are some tips on how best to help your newborn spit up:
- Let your baby spit up while feeding. If the baby is restless or has swallowed air, it is worth giving him the opportunity to burp during feeding, and not just after.
- When bottle feeding, let the newborn burp after every 50-60 ml.
- When breastfeeding, let the baby burp at every breast change.
It is important to let your baby spit up after eating, even if he spit up during feeding!
If your baby is gassy, spit up more often. Also, if he vomits frequently or suffers from gastroesophageal reflux disease (GERD), have him spit up after every 30 ml bottle-feeding or every five minutes while breastfeeding.

How long should a baby be held for it to burp? It's different for everyone, but generally keeping a newborn upright for 15 to 20 minutes after a feed helps the milk stay in the baby's stomach.
Minimize the amount of air you swallow. Gas production and regurgitation result from aerophagia during feeding. The baby will inevitably swallow air, but there are ways to prevent it from swallowing too much. Whether you bottle feed your baby or combine breastfeeding with bottle feeding, the Philips Avent anti-colic bottle with AirFree valve is designed so that the nipple is always filled with milk without excess air, even in a horizontal position, thus preventing the baby from swallowing excess air during feeding.
Reducing the amount of air your baby swallows can help reduce your baby's risk of colic, gas, and spitting up.
Breastfeeding is a wonderful time to strengthen the bond between parent and baby. Every mom and every baby is different, so learning to help your newborn burp properly can take time and practice.