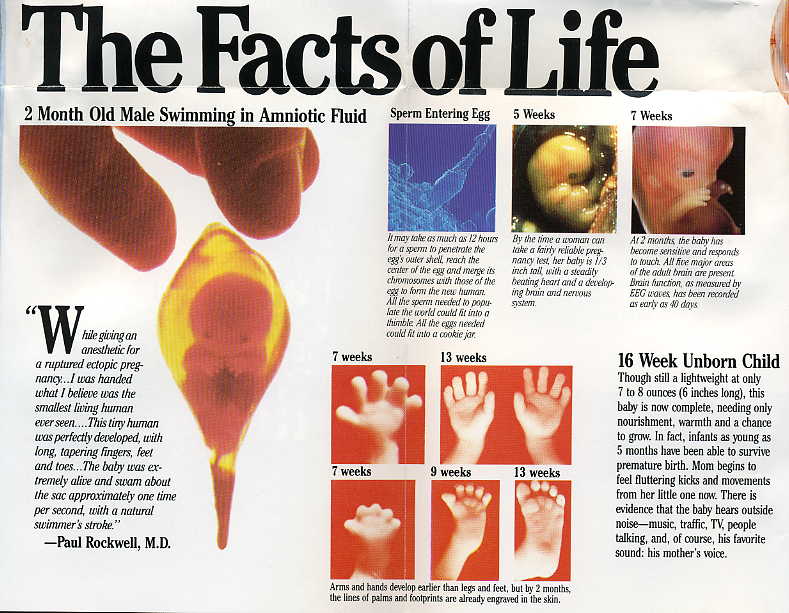
Can food poisoning kill your unborn baby
Symptoms, treatment, dangers, and more
Pregnancy brings a greater chance of getting food poisoning. It can be a scary experience for expecting parents. There are many risks that come with food poisoning during pregnancy.
Hormonal changes that occur during pregnancy can alter a person’s immune system, leading them to be more susceptible to food poisoning.
Food poisoning can happen after a person eats or drinks something containing bacteria, a virus, parasites, or other contaminants.
Food poisoning in pregnancy can result in harm to the baby, early labor, pregnancy loss, or stillbirth. However, there are many ways to prevent it or treat it.
This article will explain what the symptoms of food poisoning during pregnancy are, explore its possible dangers, and discuss treatment and prevention methods.
General symptoms of food poisoning may include:
- upset stomach
- abdominal cramps
- nausea
- vomiting
- diarrhea
- fever
The timing of symptoms may vary depending on when a person has eaten the contaminated food and what type of food poisoning a person has.
The type of food poisoning may also produce varying symptoms. According to the CDC, the following types of food poisoning have the following symptoms:
Listeria
Pregnant women are 10 times more likely to get a Listeria infection than the general population. Symptoms can take between a week to a month to develop. They may include:
- fever
- muscle ache
- headache
- fatigue
Salmonella
Salmonella symptoms can begin between 6 hours and 6 days after exposure to the contaminated food and may include:
- stomach pain
- vomiting
- diarrhea
- nausea
Norovirus
Norovirus symptoms usually start 12–48 hours after a person has consumed the contaminated food or drink. Norovirus symptoms include:
- stomach cramps
- diarrhea
- vomiting
- nausea
A person may start to experience E. coli symptoms 3–4 days after consuming the contaminated food or drink. These symptoms may include:
These symptoms may include:
- stomach cramps
- vomiting
- diarrhea
Staph (Staphylococcus aureus)
Staph symptoms may occur quickly, between 30 minutes and 8 hours after a person consumes the affected food. They can include:
- nausea
- vomiting
- stomach cramps
- diarrhea
There are some other conditions that can give a person similar symptoms to food poisoning.
Food poisoning or a stomach bug?
Gastroenteritis, or a stomach bug, is highly contagious and can spread easily from person to person. It is an inflammation of the intestines. Contaminated food or drink can cause gastroenteritis, but the main cause is usually a bacterial or viral infection.
Food poisoning is usually not contagious. People will only get it at the same time as someone else if they eat the same contaminated food.
Find out more about gastroenteritis here.
Food poisoning or morning sickness?
Morning sickness also presents similar symptoms to food poisoning. A person with morning sickness may experience symptoms during the first 12 weeks of pregnancy, though they can occur at any time.
A person with morning sickness may experience symptoms during the first 12 weeks of pregnancy, though they can occur at any time.
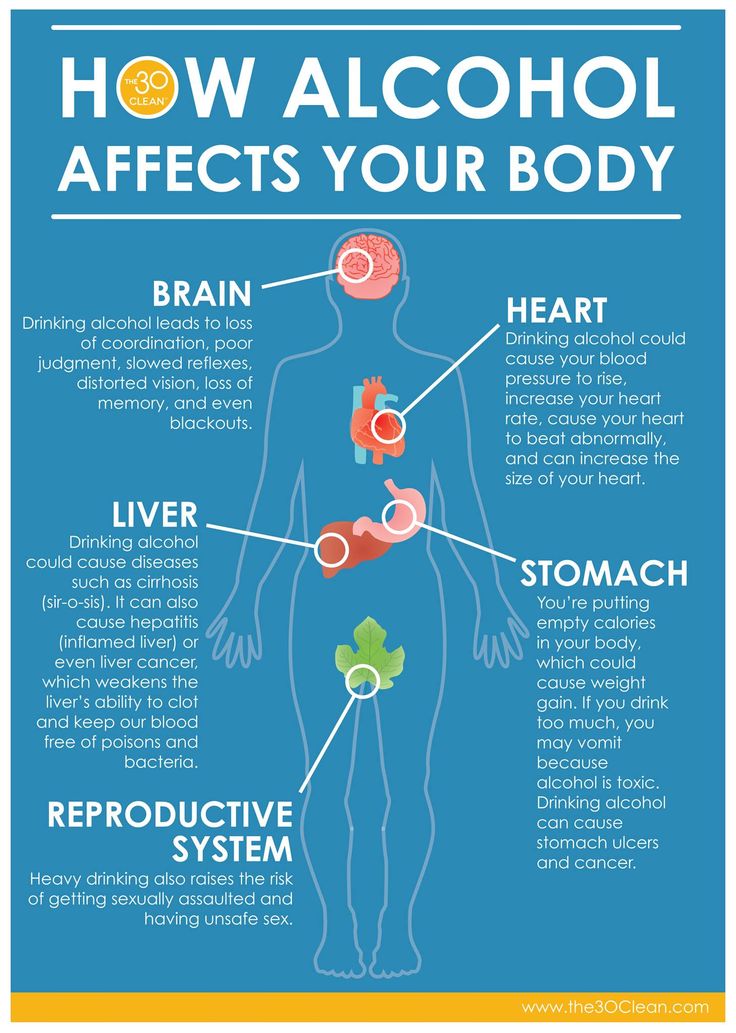
Food poisoning can be dangerous to the unborn child as well as the parent. It can cause serious health problems for the child, pregnancy loss, premature delivery, stillbirth, or even the death of the person carrying the child.
Developing fetuses need to get as many nutrients as possible from their parent carrying them. If the parent is unable to keep food in their body for long enough for their body to absorb the nutrients, the fetus may not grow appropriately.
A person with mild symptoms can pass an infection to their unborn child during pregnancy without the parent even knowing that they have food poisoning.
Newborns can also experience health issues, and can even be born with food poisoning if the person carrying the child has an infection.
While pregnant people should always visit a doctor if they have symptoms of food poisoning, there are some things that they can do at home to help too.
Foods
It can be difficult for a person to feel like eating anything when they have food poisoning. However, a pregnant person needs to eat to keep their strength up and ensure they are eating enough for themselves and the unborn child. It is best to eat bland, low-fat foods that will help keep the stomach as calm as possible.
Foods they can eat include:
- saltine crackers
- toast
- applesauce
- mashed potatoes
- boiled rice
Drinks
A person with food poisoning has a high risk of developing dehydration. Therefore, ensuring that they consume enough fluids is very important. Easy ways of replacing lost fluids include drinking:
- plain water
- fruit juices diluted with water
- sports drinks containing electrolytes
- broths
Oral rehydration solutions or salts can also help replace glucose and electrolytes. They are made up of water with extra salt and glucose that help the body rehydrate.
Natural remedies
Ginger has properties that ease nausea and vomiting. Ginger tea may help a person if they are experiencing these symptoms.
Find out more about the benefits of ginger tea here.
A person should contact a doctor if they are pregnant and suspect they have food poisoning. Even though most people will recover from food poisoning without needing to seek medical attention, a pregnant person must also consider the health of the unborn child.
A pregnant person should contact a doctor immediately if they have any of the following symptoms:
- a temperature of over 102°F
- blood in the stool
- diarrhea lasting longer than 3 days
- dizziness
- a dry mouth or throat
- frequent vomiting
Although the risks of food poisoning in pregnancy can be scary, there are ways to prevent it.
Food types to avoid
Food poisoning can come from a variety of different food products, but there are steps people can take to reduce their risk. For example:
For example:
Meat and poultry
Always make sure that these are cooked through. This will lower the risk of developing food poisoning. A meat thermometer can help a person check that their meat has reached a safe minimum internal temperature. For example, a person should cook beef, pork, steaks, and chops to at least 145°F (63°C), giving the meat a 3 minute rest time after cooking.
Vegetables
Unwashed vegetables and raw vegetables can cause a person to develop food poisoning. Make sure to carefully wash all vegetables.
Eggs
Consuming raw or undercooked eggs increases a person’s risk of foodborne illnesses. Pasteurized eggs carry a lower risk.
Milk
Unpasteurized milk can increase a pregnant person’s risk of food poisoning. This includes cheeses made with unpasteurized milk.
Seafood
Pregnant people should avoid raw or undercooked fish, like sushi. Cooked seafood and canned fish and seafood carry a lower risk of causing foodborne illnesses.
Other foods pregnant people should avoid include:
- raw sprouts
- deli salads
- pâtés
A pregnant person should also avoid deli meats and hot dogs unless cooked to a temperature of 165ºF (74ºC) or above.
Food safety tips
The Centers for Disease Control and Prevention (CDC) recommend four food safety tips to try to avoid food poisoning:
Clean
Make sure that everything is clean before preparing food. This includes washing hands and working with clean utensils and cutting boards on freshly cleaned countertops. This lowers the risk of contamination.
Rinsing fresh fruits and vegetables under running water can remove the germs that may cause food poisoning.
Separate
Avoid cross-contamination by ensuring that all utensils that come into contact with raw foods do not then touch cooked or ready-to-eat foods.
Keep raw meat, poultry, seafood, and eggs separate from other foods when grocery shopping and after returning home, from storing them in the fridge to the preparation of meals.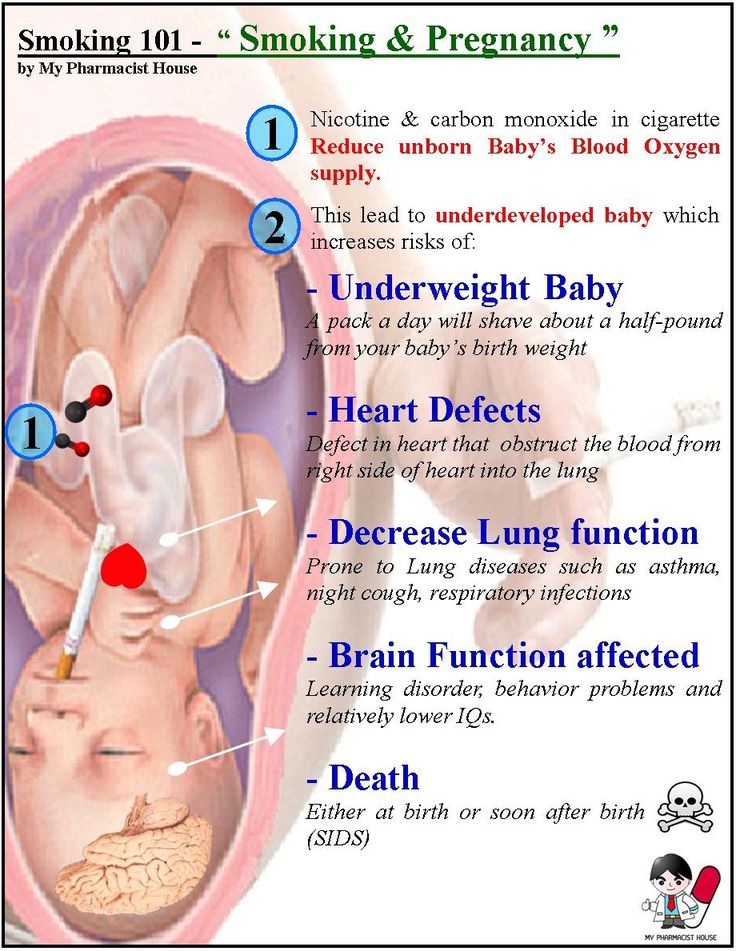
Cook
Use a thermometer to determine if the internal temperature of their food is high enough to kill off germs that could cause food poisoning.
Chill
Chill perishable food as soon as possible, making sure the fridge stays at a temperature of 40°F (4°C) or below. Thaw frozen food in the refrigerator, in cold water, or in the microwave. When food is thawed on the counter, bacteria can multiply quickly in any parts of the food that reach room temperature.
According to the Centers for Disease Control and Prevention (CDC), 48 million people get sick from a foodborne illness each year. 128,000 of those people require hospitalization, and 3,000 of them pass away.
Pregnant people are more susceptible to food poisoning.
Food poisoning usually resolves itself after a few days, but in a pregnant person, it can be a serious and even fatal illness. Following food safety protocols can help pregnant people avoid food poisoning, have a safe and healthy pregnancy, and avoid any related issues for them and their child.
Food poisoning during pregnancy | March of Dimes
Food poisoning happens when you eat or drink something with harmful bacteria (germs) in it.
Normal changes in your body during pregnancy may make you more likely to get food poisoning.
During pregnancy, food poisoning can cause serious problems for you and your baby, including premature birth, miscarriage and stillbirth.
Wash your hands before handling food and learn how to handle food safely. Don’t eat foods that commonly cause food poisoning.
If you think you have food poisoning, call your health care provider right away.
What is listeriosis and how can it affect pregnancy?
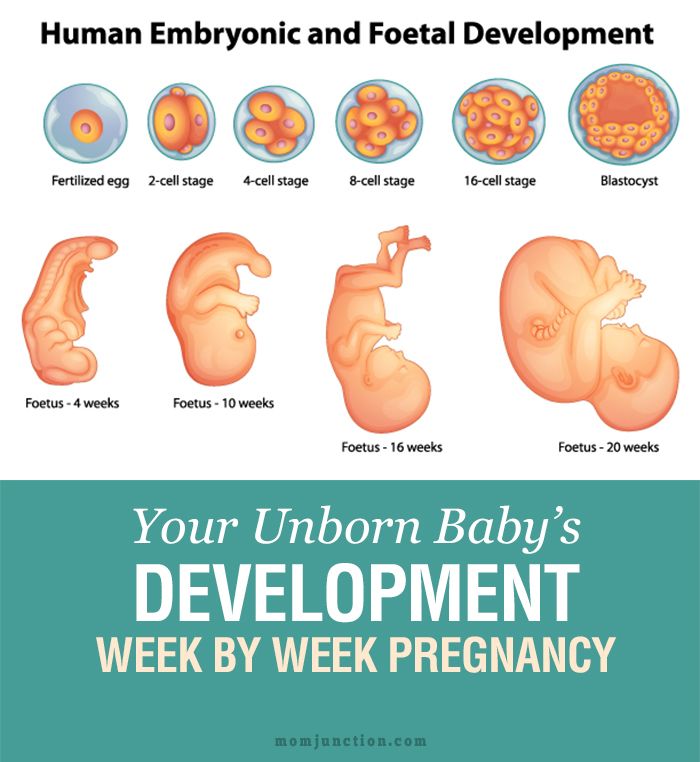
Listeriosis is a kind of food poisoning caused by Listeria bacteria. During pregnancy, you can pass the bacteria to your baby. This can cause problems, including:
- Miscarriage. This is when a baby dies in the womb before 20 weeks of pregnancy.
- Stillbirth.
 This is when a baby dies in the womb after 20 weeks of pregnancy.
This is when a baby dies in the womb after 20 weeks of pregnancy. - Preterm labor and premature birth. These are labor and birth that happen too early, before 37 weeks of pregnancy. Babies born prematurely may have health problems and birth and later in life.
- Low birthweight. This is when a baby is born weighing less than 5 pounds, 8 ounces.
- Life-threatening infections in your baby, including bacteria in the blood (called bacteremia) and meningitis. Meningitis is an infection that causes swelling in the brain and spinal cord. Infected babies may have health problems after birth, including seizures, blindness and problems with the brain, heart and kidneys.
Listeria may be in the soil, water, on animals and in animal waste. The most common cause of listeriosis is eating food with Listeria in it. Foods that are most likely to have Listeria include:
- Unpasteurized milk and foods made with it. If milk is pasteurized, it’s been heated to kill germs.
 Look for the word “pasteurized” on the label.
Look for the word “pasteurized” on the label. - Soft cheeses, like feta, Brie, Camembert, Roquefort and Mexican-style cheeses, like queso fresco, queso blanco, Panela and Asadero
- Deli meat, hot dogs, juice from hot dogs and dry sausages that are chilled or at room temperature
- Unwashed fruits, vegetables or sprouts
- Cold salads from delis or salad bars
- Refrigerated patés or meat spreads (Canned meat spreads are safe.)
- Refrigerated smoked seafood, including nova-style, lox, kippered, smoked and jerky
How do you know if you have listeriosis?
Signs and symptoms of listeriosis usually start a few days after eating food contaminated by Listeria, but they may not happen for up to 2 months. They’re usually mild and flu-like. Your health care provider can test your blood to see if you have listeriosis.
Call your provider right away if you have:
- Being confused or having trouble with balance
- Fever or chills
- Headache
- Muscle aches
- Nausea (feeling sick to your stomach) or diarrhea
- Seizures
- Stiff neck
What is salmonellosis and how can it affect pregnancy?
Salmonellosis is a kind of food poisoning caused by Salmonella bacteria. Salmonellosis can cause problems during pregnancy, including:
Salmonellosis can cause problems during pregnancy, including:
- Dehydration. This is when you don’t have enough water in your body. Signs and symptoms of dehydration include feeling dizzy or lightheaded, having a fast heartbeat, having dark-colored urine and having a dry mouth and lips.
- Bacteremia
- Meningitis
- Reactive arthritis (also called Reiter’s syndrome). This condition can cause swelling or pain in joints, like the knees, ankles and toes.
You can pass salmonellosis to your baby during pregnancy. If your baby is born with salmonellosis, she may have diarrhea and fever after birth. She also may develop meningitis.
You can get infected with Salmonella in two ways:
- By touching an infected animal. Salmonella can be found in poop, soil, water (including fish tank water), food and bedding of infected animals, including pets. Salmonella germs can spread easily to an animal’s fur, feathers and scales. Animals that are most likely to carry Salmonella include reptiles (turtles, lizards, snakes) and poultry (chickens, ducks, geese).

- By eating foods that are contaminated with Salmonella. These foods may look and smell normal, even if they’re contaminated.
Foods that often have Salmonella include:
- Raw or undercooked poultry, meat or fish. Cooking these items fully kills Salmonella.
- Raw or undercooked eggs and foods made with them. Salmonella can pass from chickens to their eggs. Even eggs that look normal can have Salmonella. Don’t eat food made with raw eggs, including homemade mayonnaise, hollandaise sauce, Caesar salad dressing, cookie dough, frostings and homemade ice cream.
- Unpasteurized milk, milk products and juice, or foods made from them. Milk and juice often are pasteurized. Look for the word “pasteurized” on the product label.
- Foods that come in contact with animal poop in the soil or water where they grow. These include mushrooms, fruits, vegetables and vegetable sprouts, like alfalfa, clover, radish and mung beans.
- Food that comes into contact with Salmonella while you’re making or serving it.
 For example, if you’re infected and don’t wash your hands after using the bathroom, you can spread the infection to food. Or if you use the same knife to cut raw chicken and tomatoes and don’t wash the knife in between, the knife can pass Salmonella from the chicken to the tomatoes.
For example, if you’re infected and don’t wash your hands after using the bathroom, you can spread the infection to food. Or if you use the same knife to cut raw chicken and tomatoes and don’t wash the knife in between, the knife can pass Salmonella from the chicken to the tomatoes.
How do you know if you have salmonellosis?
You may be at increased risk of getting salmonellosis if you:
- Have reduced stomach acid from using medicines for heartburn (called antacids), like Tums®.
- Have recently used antibiotics. Antibiotics are medicines that kill infections caused by bacteria.
- Have a digestive condition called inflammatory bowel disease (also called IBD). Digestion is the process of how your body breaks down food after you eat.
- Have a weak immune system or an illness like HIV, sickle cell disease or malaria
- Travel to places that don’t have good sanitation systems. This means they don’t have toilets and clean water for cooking and washing.

- Have a pet bird or reptile
- Live and eat in group housing, like a dormitory
Signs of salmonellosis usually start a half day to 3 days after contact and last for 4 to 7 days. To test for salmonellosis, your health care provider takes a stool sample (a sample of your poop) and sends it to a lab for testing.
Call your provider right away if you have any signs or symptoms of salmonellosis, including:
- Belly pain
- Blood in your poop or dark or amber-colored urine (pee)
- Dehydration
- Fever or chills
- Headache
- Muscle pains
- Nausea, diarrhea or throwing up
How is food poisoning treated?
Treatment depends on how sick you are. You may not need any treatment, or your provider may treat you with antibiotics to help keep you and your baby safe. If you have food poisoning, drink lots of water to help you stay hydrated (have water in your body). If you’re severely dehydrated (don’t have enough water in your body), you may need to go to the hospital for treatment.
How can you protect yourself and your baby from food poisoning during pregnancy?
Here’s what you can do:
- Wash your hands right before handling food. Wash your hands well with soap and water after using the bathroom.
- Wash your hands well with soap and water after touching animals or their food, bedding, tanks or waste.
- Don’t eat foods that are likely to be contaminated with Listeria or Salmonella.
- Handle foods safely whenever you wash, prepare, cook and store them. Wash knives, cutting boards and dishes used to prepare raw meat, fish or poultry before using them for other foods.
More information
Centers for Disease Control and Prevention
Food and Drug Administration
Last reviewed: May, 2016
Food poisoning in a child - rules for prevention and treatment There are frequent cases when, even in the treatment of children, parents do not resort to the help of doctors, but manage with a “standard” set of funds from grandmother's recipes or advertising on TV.
 Gastric lavage with potassium permanganate, taking activated charcoal or some other absorbent, this is the usual set in the hands of an “experienced” parent. However, not everyone clearly understands the essence of intoxication of the body, not everyone can correctly determine its nature and predict the consequences. Not everyone knows that in some cases, poisoning can cause deadly bacteria, such as botulism, and sometimes it happens that a completely different disease is hidden under the symptoms of intoxication of the body, for example, heat stroke. And while parents are trying to overcome the false poisoning of the child, they lose precious time, which can lead to a sharp deterioration in the condition and serious consequences.
Gastric lavage with potassium permanganate, taking activated charcoal or some other absorbent, this is the usual set in the hands of an “experienced” parent. However, not everyone clearly understands the essence of intoxication of the body, not everyone can correctly determine its nature and predict the consequences. Not everyone knows that in some cases, poisoning can cause deadly bacteria, such as botulism, and sometimes it happens that a completely different disease is hidden under the symptoms of intoxication of the body, for example, heat stroke. And while parents are trying to overcome the false poisoning of the child, they lose precious time, which can lead to a sharp deterioration in the condition and serious consequences. Given all of the above, it should be noted that parents should not self-medicate, even if it seems to them that it is food poisoning in a child and that they themselves will quickly cope. We recommend that you always seek medical attention, although if possible, take some steps to alleviate the child's condition.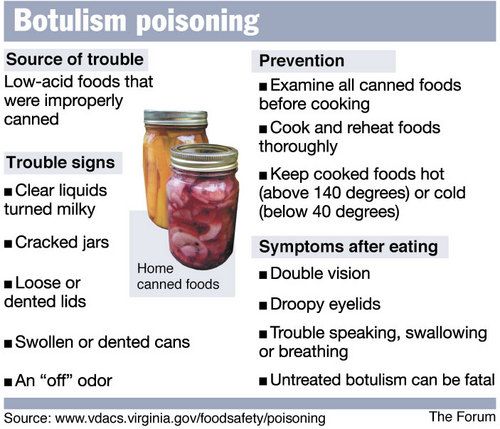 We will describe how to prevent food intoxication and what to do if it occurs.
We will describe how to prevent food intoxication and what to do if it occurs.
We also recommend reading the resource "Protecting children from the sun", where you will learn about the dangers of the scorching summer sun, about common myths about this and about the correct methods of protection. If you are raising a teenager and have begun to notice oddities in their behavior, then we recommend reading an important article about common signs of drug addiction in teenagers.
Children will not get food poisoning if adults follow simple rules
Food poisoning in children - possible routes of intoxication and their symptoms
Their immune systems are still not strong enough. Food poisoning in children, as well as in adults, most often occurs when eating food that is contaminated with microbes. Separate manifestations in two forms - toxic infection, as well as intoxication.
Usually, toxic infection is caused by microbes belonging to the Salmonella group, as well as para-Escherichia and Escherichia coli. Be aware that salmonella is very common and often infects the intestines of birds and animals. And when the animal's body weakens and, accordingly, its protective functions, too, salmonella infect all internal organs. Such meat, having got on the table to people after a weak heat treatment, causes poisoning. Salmonella can also infect eggs, pies, milk, cheese, fish and cottage cheese. Symptoms of poisoning usually occur after a few hours or later, depending on the dose, the organism and the nature of the poisoning. The child begins to feel nausea, vomiting, headache, stools are frequent and liquid, body temperature rises. The disease lasts from two days to a week and in most cases ends in recovery.
Be aware that salmonella is very common and often infects the intestines of birds and animals. And when the animal's body weakens and, accordingly, its protective functions, too, salmonella infect all internal organs. Such meat, having got on the table to people after a weak heat treatment, causes poisoning. Salmonella can also infect eggs, pies, milk, cheese, fish and cottage cheese. Symptoms of poisoning usually occur after a few hours or later, depending on the dose, the organism and the nature of the poisoning. The child begins to feel nausea, vomiting, headache, stools are frequent and liquid, body temperature rises. The disease lasts from two days to a week and in most cases ends in recovery.
Food Intoxication of the child's body occurs as a result of eating, which contains poisons in the form of microbial waste products. They are called toxins. Most often, such poisoning is caused by staphylococcus aureus. It, as a rule, gets into ready meals from those who have pustular skin diseases. Poisoning through cakes, ice cream, pastries, sausage, ham, sausages and so on is common. Even when ingested in raw foods, this toxin is not easy to destroy. At the boiling point, it does not collapse for several hours. Symptoms of poisoning usually appear in time in the same way as with toxic infection. The clinical picture and course of the disease are similar.
Poisoning through cakes, ice cream, pastries, sausage, ham, sausages and so on is common. Even when ingested in raw foods, this toxin is not easy to destroy. At the boiling point, it does not collapse for several hours. Symptoms of poisoning usually appear in time in the same way as with toxic infection. The clinical picture and course of the disease are similar.
Botulism causes a very dangerous poisoning of the body, which without urgent medical intervention can result in the death of a child. Botulism bacteria thrive in an oxygen-free environment and produce a strong toxin. It is destroyed after 20 minutes of boiling, but in order to destroy the spores themselves, it is necessary to maintain a temperature of 120 degrees Celsius for 10 minutes. The most common source of poisoning are all kinds of canned foods, namely meat, fish, vegetables. But cases of intoxication were also observed through the earth, which was contaminated with the feces of sick animals. The onset of the disease occurs after a couple of hours, although an incubation period of several days is sometimes possible. The child feels dry mouth, dizziness, general weakness and shortness of breath, the pulse quickens, paralysis of the eye and facial muscles, as well as the muscles of the soft palate and tongue, occurs. Because of this, a disorder of speech, vision and swallowing occurs - the child chokes and begins to distinguish poorly between nearby objects and text. The toxin affects the nervous apparatus of the heart and the central nervous system. The disease lasts 4-8 days, is difficult and without medical intervention can lead to death due to paralysis of the respiratory center.
The onset of the disease occurs after a couple of hours, although an incubation period of several days is sometimes possible. The child feels dry mouth, dizziness, general weakness and shortness of breath, the pulse quickens, paralysis of the eye and facial muscles, as well as the muscles of the soft palate and tongue, occurs. Because of this, a disorder of speech, vision and swallowing occurs - the child chokes and begins to distinguish poorly between nearby objects and text. The toxin affects the nervous apparatus of the heart and the central nervous system. The disease lasts 4-8 days, is difficult and without medical intervention can lead to death due to paralysis of the respiratory center.
Please note that botulism spores may contain canned honey, even commercially produced honey. Therefore, in no case should you give such honey to children under one year old, they may develop infant botulism. And for adults, it is usually harmless.
In infants, botulism, as a rule, begins precisely with constipation, then the baby begins to make sucking movements poorly and swallows with difficulty, his eyelids begin to weaken, he weakly makes sounds or words, and general impotence develops.
Non-bacterial poisonings are usually due to the consumption of poisonous mushrooms, fish or light-green potatoes, which accumulate poisonous solanine under their skin. Many mushrooms are poisonous in nature, and there are many false mushrooms, remember that it is not recommended for children to eat mushrooms at all until they are 12 years old. Especially often they are poisoned by mushrooms - lines that are very similar to edible morels. Only stitches in dry weather develop poisonous gelvellic acid, a very potent poison that is resistant to heat. Pay attention to the photos and avoid buying and picking similar mushrooms.
Poisonous - line. Edible morel.
Toxin poisoning of some fish may be due to improper handling or transport. For example, mackerel produces poisons if it is not frozen in time. Also keep in mind that children should not be given Japanese sushi with fish or shrimp, which can also serve as a source of dangerous poisoning.
Food poisoning in children - disease prevention
Here are the basic rules for the prevention of food poisoning in children:
- Adults should remember the first and most important rule from school: “wash your hands before eating”, and this is not just a general slogan, but a vital necessity.
 Washing hands before eating reduces the risk of poisoning several times.
Washing hands before eating reduces the risk of poisoning several times. - Further, the second rule is to thoroughly wash the foods that you eat raw - vegetables and fruits. Do not give raw milk and eggs to children. Pasteurized milk from the store is also recommended to boil.
- Prevent children from eating "adult" foods such as Japanese sushi, smoked fish, mushrooms, and so on.
- The meat of birds, animals, must undergo careful temperature treatment, use the rule: "you can't digest the meat." The same applies to fish, seafood and eggs.
- When canning at home, strictly adhere to the technology and temperature regime for the destruction of botulism spores. Do not use homemade or factory-made products that bulge bags, jars, or lids (also called bombing). Do not eat foods with a suspicious smell or texture.
- Store perishable foods in the refrigerator only during their expiration date and in a container with a closed lid. Remember that cakes, cream cakes, salads with mayonnaise, open packages of food and drinks that do not contain preservatives, such as natural juices, spoil very quickly.
 Remember the approximate storage time of popular products in the cold up to 8 degrees (without cold, it is much less, and sometimes products cannot be stored without cold at all). Of course, modern preservatives can extend the life of some products, but do you need to risk the health of your children in vain.
Remember the approximate storage time of popular products in the cold up to 8 degrees (without cold, it is much less, and sometimes products cannot be stored without cold at all). Of course, modern preservatives can extend the life of some products, but do you need to risk the health of your children in vain. - Cottage cheese mass, curd cream or cheese curds - in the cold up to 24 hours (cannot be stored without cold).
- Pies fried with meat or fish - in the cold up to 24 hours, in a cool place up to 12 hours.
- Cake with butter cream - in the cold up to 6 C °, the shelf life is up to 36 hours, in a cool place up to 12 hours.
- Custard tart - refrigerate up to 6 hours, cannot be stored without refrigeration.
- Serve hot fish or meat dishes on the table soon after cooking, do not store perishable food outside the refrigerator.
- Always check the expiration date of products when buying and before eating.
- Do not buy very early fruits and vegetables (such as tomatoes, watermelons, melons or strawberries), they tend to be high in chemical growth stimulants that can cause acute poisoning.

- Do not buy food in questionable places from hands or trays. Especially in the hot season, especially on the beach, especially meat products (chebureks, belyashi, etc.), especially for children! Remember that meat in the sun after 20-30 minutes can turn into poison.
Parental actions if a child has food poisoning
Providing medical care for food poisoning
When a child has food poisoning, the most important thing is to provide the child with medical care promptly. If you are on vacation, then contact the administration of the hotel or recreation center so that they take urgent measures. If you are at home, then, depending on the situation, call a doctor, emergency or ambulance. In case of a sharp deterioration in the condition, immediately call an ambulance (even if you have previously called a doctor at home), dangerous syndromes include: vomiting or diarrhea with blood, delirium, hallucinations, loss of consciousness, asphyxia (the child is suffocating), weakening of the pulse, cyanosis skin (the child begins to turn blue).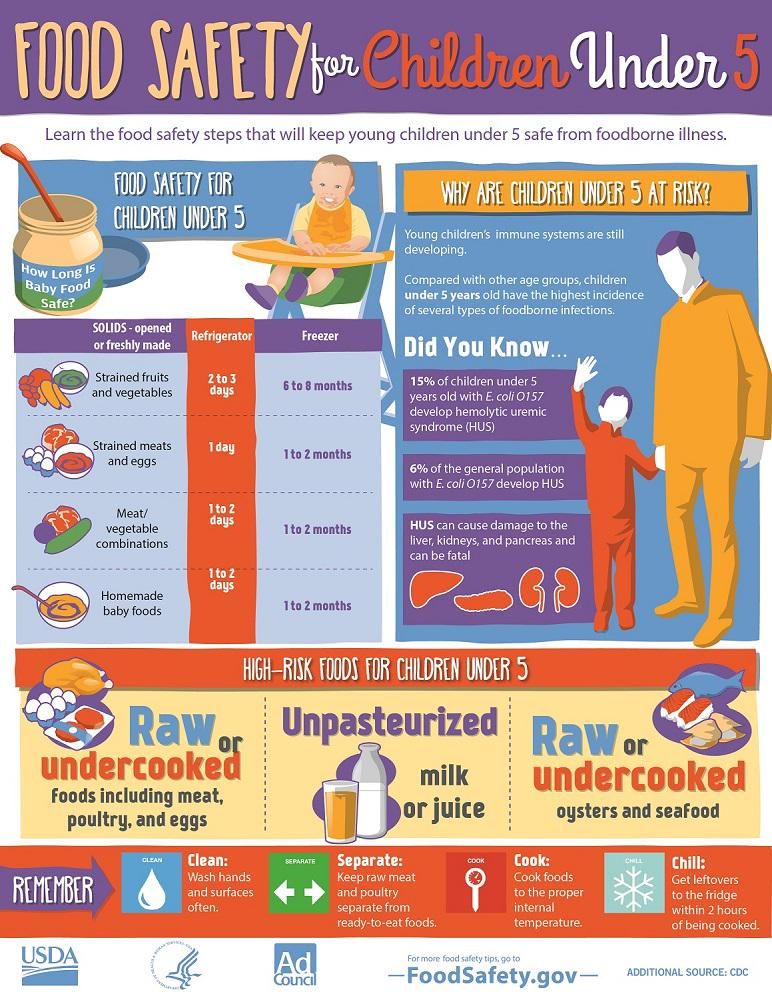
Always remain calm, do not scare, but rather calm the child. Clearly and in detail describe the essence of the problem and symptoms to the medical worker by phone, ask for general recommendations over the phone, what you need to do before the ambulance or doctor arrives.
Please note that the symptoms of an illness may only look like poisoning, but in fact it may be a completely different disease, such as sunstroke. Only a doctor can make a qualified diagnosis.
General actions in case of child poisoning
If you are sure that the child has food poisoning (preferably after consulting a doctor over the phone), then first of all ensure that the stomach is empty of the food that is most likely the cause of the illness. To do this, let the child drink a lot of warm boiled water, and then induce vomiting by pressing on the root of the tongue. Repeat the procedure until the vomit comes out clean, without pieces of food and mucus. We DO NOT RECOMMEND rinsing the stomach with potassium permanganate (potassium permanganate) without consulting a doctor. But if you are planning to make such a solution, then use either drops, or in the case of crystals, carefully pour the solution into another dish to avoid internal burns with small particles. Remember that the potassium permanganate solution should be slightly pink, and do not give potassium permanganate to children under 5 years old.
But if you are planning to make such a solution, then use either drops, or in the case of crystals, carefully pour the solution into another dish to avoid internal burns with small particles. Remember that the potassium permanganate solution should be slightly pink, and do not give potassium permanganate to children under 5 years old.
Use sorbents to remove absorbed harmful substances and toxins from the child's intestines. These are substances that draw toxins into themselves and then remove them from the body. Popular drugs are: activated carbon, Polyphepan, Karbolong. But remember that in some cases - with ulcerative and erosive lesions of the intestines and stomach, these drugs may be contraindicated. The drug Enterosgel is very popular, it does not irritate the mucous membranes and has excellent sorption properties of toxins, and it also sorbs bilirubin.
In case of poisoning accompanied by diarrhea and flatulence, Bifilact extra or Extralact can be used, they also contain microbial components that restore the normal intestinal flora. It’s also a good idea to use Smecta - it protects the inflamed mucous surfaces from the effects of viruses and toxins and restores the stool. Please note that Imodium (Loperamide) is not recommended to be used alone for food poisoning, since if used incorrectly, even more active absorption of harmful substances into the blood is possible.
It’s also a good idea to use Smecta - it protects the inflamed mucous surfaces from the effects of viruses and toxins and restores the stool. Please note that Imodium (Loperamide) is not recommended to be used alone for food poisoning, since if used incorrectly, even more active absorption of harmful substances into the blood is possible.
In any case, do not self-medicate your children with food poisoning, always consult a doctor!
Article of the site - "Safety of children"
Food poisoning in a child. What is Food Poisoning in a Child?
IMPORTANT
The information in this section should not be used for self-diagnosis or self-treatment. In case of pain or other exacerbation of the disease, only the attending physician should prescribe diagnostic tests. For diagnosis and proper treatment, you should contact your doctor.
Food poisoning in a child is an acute infectious-toxic lesion that occurs as a result of eating poor-quality products containing pathogens and their toxins, plant or other poisons. Food poisoning in a child is manifested by diarrhea, vomiting, fever, intoxication, dehydration. Diagnosis of food poisoning in children involves the clarification of the epidemiological history; identification of a pathogen or toxin in blood, feces, vomit, food samples. Treatment of food poisoning in children requires immediate gastric lavage or cleansing enema, enterosorbents, rehydration.
Food poisoning in a child is manifested by diarrhea, vomiting, fever, intoxication, dehydration. Diagnosis of food poisoning in children involves the clarification of the epidemiological history; identification of a pathogen or toxin in blood, feces, vomit, food samples. Treatment of food poisoning in children requires immediate gastric lavage or cleansing enema, enterosorbents, rehydration.
- Classification
- Causes
- Symptoms of food poisoning in a child
- Diagnosis of food poisoning in a child
- Treatment of food poisoning in a child
- Prognosis and prevention of food poisoning in a child
- Prices for treatment
General
Food poisoning in a child is food poisoning or intoxication associated with the consumption of infected food, water, or toxic (plant, chemical, medicinal) substances. Food poisoning in children occupies a leading place in the range of infectious pathology and toxicology of childhood and represents a serious problem in practical pediatrics.
Food poisoning in a child is much more severe than in adults, which is explained by the characteristics of the child's body: low acidity of gastric juice, incomplete formation of intestinal microflora, faster absorption of the poison and its distribution throughout the body, relatively low detoxification capacity of the liver and filtration function of the kidneys, etc. Often the same products that do not cause any signs of poisoning in an adult cause food poisoning in a child.
Food poisoning in a child
Classification
A child may have the following types of food poisoning:
In the clinical course of food poisoning in a child, 3 stages are distinguished:
- Latent (asymptomatic) - lasts from the moment the toxin/poison is taken until the first symptoms of food poisoning appear in the child.
 The duration of the latent period depends on the age and individual characteristics of the child, the amount of a toxic substance that has entered the body with food, and the rate of its absorption. The latent stage of food poisoning is the most favorable "window" for the treatment of a child, when the poison has not yet entered the bloodstream and has not exerted its toxic effect. First aid in this case is gastric lavage and the intake of enterosorbents.
The duration of the latent period depends on the age and individual characteristics of the child, the amount of a toxic substance that has entered the body with food, and the rate of its absorption. The latent stage of food poisoning is the most favorable "window" for the treatment of a child, when the poison has not yet entered the bloodstream and has not exerted its toxic effect. First aid in this case is gastric lavage and the intake of enterosorbents. - Toxicogenic - lasts from the appearance of the first signs of poisoning to the elimination of bacteria and poison from the body. The toxicogenic period is manifested by the developed symptoms of food poisoning in a child, characteristic of this toxic infection or poison. This stage requires identification of bacteria and poison, their removal (gastric lavage, cleansing enema, forced diuresis), detoxification, etc.
- Stage of convalescence - restoration of impaired functions (digestive, excretory, immune, etc.).
Causes
Infectious food poisoning in a child (food poisoning) can be caused by staphylococcus aureus, proteus, klebsiella, clostridia, citrobacter, enterotoxigenic strains of Escherichia coli, etc. These pathogens enter the body exclusively with food, in which they first multiply and produce toxins. Contamination of food and the accumulation of toxins are favored by non-compliance with sanitary and hygienic standards in the process of storing, preparing and selling food. At the same time, the products may look like poor quality (unpleasant smell, taste, changed color, texture) or have normal organoleptic qualities.
These pathogens enter the body exclusively with food, in which they first multiply and produce toxins. Contamination of food and the accumulation of toxins are favored by non-compliance with sanitary and hygienic standards in the process of storing, preparing and selling food. At the same time, the products may look like poor quality (unpleasant smell, taste, changed color, texture) or have normal organoleptic qualities.
Microbial sources that seed food can be persons suffering from intestinal infections, purulent diseases (tonsillitis, furunculosis, streptoderma, felons, mastitis, etc.), as well as animals that pollute water, soil, plants and other environmental objects with their feces. Food poisoning in a child can be caused by drinking unboiled water, contaminated milk and dairy products, eggs, cream confectionery, fish and seafood, sausages, meat (beef, pork, chicken, etc.), home-made canned food, etc.
Food poisoning in children can occur as sporadic, familial or mass outbreaks. They are characterized by an increase in the incidence in the summer-autumn period, when there are favorable conditions for the reproduction of microbial pathogens and the accumulation of toxins.
They are characterized by an increase in the incidence in the summer-autumn period, when there are favorable conditions for the reproduction of microbial pathogens and the accumulation of toxins.
Non-infectious food poisoning is usually associated with the child's accidental consumption of poisonous berries (nightshade, wolfberry, black elderberry, crow's eye, etc.), plants (hemlock, henbane, poisonous milestone, dope, etc.), mushrooms (pale toadstool, fly agaric, false chanterelles or honey mushrooms). Food poisoning in a child can occur when eating agricultural products contaminated with toxic chemical impurities (fungicides, insecticides, inorganic compounds).
Symptoms of food poisoning in a child
The clinical picture of food poisoning in a child with various toxic infections is very similar. Usually the latent stage lasts 2-6 hours; sometimes shortened to 30 minutes. or lengthens up to 24 hours. Food poisoning in a child is manifested by signs of gastroenteritis, general infectious symptoms, intoxication, dehydration.
The disease begins acutely, with nausea, repeated vomiting of food eaten, abdominal pain (mainly in the stomach area), watery diarrhea with impurities of greens, mucus, streaks of blood. The frequency of stool reaches 5-10 times a day.
Almost simultaneously with the phenomena of gastroenteritis, the body temperature rises to 38-39 ° C. The intoxication syndrome is rapidly growing, characterized by lethargy, refusal to eat, headache and muscle pain. Fluid loss with vomiting and stool leads to dehydration: facial features are sharpened, the skin becomes pale and dry to the touch. A child with food poisoning may have convulsions, oligo-, anuria, hemodynamic disorders, acidosis.
The course of food poisoning is short; in most cases, symptoms regress after 2–3 days, although weakness and abdominal pain may persist for longer. Severe forms of food poisoning can be observed in young children, debilitated individuals with a concomitant background (prematurity, malnutrition, dysbacteriosis, etc. ). In severe cases, the child may develop necrotic enteritis, infectious-toxic or hypovolemic shock, endocarditis, sepsis.
). In severe cases, the child may develop necrotic enteritis, infectious-toxic or hypovolemic shock, endocarditis, sepsis.
In case of food poisoning by poisonous plants in a child, the central nervous system is often affected, which can be manifested by lethargy, euphoria, hallucinations, visual impairment, speech disorders, convulsions, coma. With a toxic effect on the cardiovascular system, tachycardia or bradycardia, arrhythmia, and arterial hypotension occur. Most plants mainly affect the gastrointestinal tract, which makes food poisoning in a child less dangerous.
Food poisoning of a child with mushrooms always occurs through the fault of adults who allow the use of unknown or dubious "gifts of the forest" in food. Poisoning with a pale toadstool is accompanied by indomitable vomiting, intestinal colic, cholera-like diarrhea mixed with blood, convulsions, and respiratory distress. The action of the poison leads to the development of toxic hepatitis, and in 90% of cases - to death due to acute liver failure.
In case of fly agaric poisoning, increased salivation, vomiting, shortness of breath, bronchospasm, hallucinations, and convulsions occur. The mortality rate for fly agaric poisoning is 1%. The clinical picture, diagnosis and treatment of botulism can be found here.
Diagnosis of food poisoning in a child
Food poisoning in a child can usually be diagnosed by a pediatrician or pediatric infectious disease specialist. The diagnosis of food poisoning in a child is facilitated by the clarification of the epidemiological history, a typical clinical picture, an indication of group cases of poisoning of persons who consumed the same food.
Specific diagnostic tests include the isolation of the pathogen from bacteriological culture of feces, vomit, gastric lavage, and the remains of an infected product. In case of suspicion of a generalized form of infection, a blood culture is performed. During mass outbreaks of food poisoning in children's groups, kitchen workers are subject to examination, from whom swabs are taken from their hands, from the nasopharynx, and rectum. Express methods for detecting the pathogen (RIF, ELISA, PCR) are of secondary importance.
Express methods for detecting the pathogen (RIF, ELISA, PCR) are of secondary importance.
In some cases, a child with food poisoning may need to consult a pediatric neurologist, pediatric gastroenterologist, pediatric surgeon. Differential diagnosis of food poisoning is carried out with acute gastritis, acute appendicitis, cholecystitis, pancreatitis, giardiasis, acute intestinal infection, meningitis in a child.
Treatment of food poisoning in a child
Emergency assistance in establishing the fact of food poisoning in a child consists in washing the stomach to clean water and administering a cleansing enema to remove toxins from the gastrointestinal tract. For the same purpose, the appointment of enterosorbents (activated carbon, combined preparations) is shown.
To eliminate dehydration, oral rehydration (sweet tea, saline solutions) is necessary for moderate forms - parenteral rehydration therapy with saline solutions. In case of food poisoning, the child is prescribed replacement therapy with polyenzymatic preparations with pancreatin. Antimicrobial therapy for a child with food poisoning is carried out only for severe toxic infections under the supervision of a physician.
In case of food poisoning, the child is prescribed replacement therapy with polyenzymatic preparations with pancreatin. Antimicrobial therapy for a child with food poisoning is carried out only for severe toxic infections under the supervision of a physician.
It is advisable to abstain from eating for 12-24 hours. After the cessation of vomiting, a sparing diet is recommended to the child (liquid cereals, mucous soups, crackers, compotes, kefir).
In case of poisoning with a pale toadstool, a child needs an emergency extracorporeal hemocorrection (hemosorption).
Prediction and prevention of food poisoning in a child
Food poisoning in a child that occurs in mild or moderate severity usually ends in a complete recovery. The consequences of food poisoning in a child can be various dysfunctions of organs and systems. So, the outcome of food poisoning is often dysbacteriosis, and mushroom poisoning - kidney and liver failure. With severe food poisoning, a child may develop severe multiple organ failure, requiring intensive care. With toxic infections, the lethality is low (about 1%), which cannot be said about mushroom poisoning.
With severe food poisoning, a child may develop severe multiple organ failure, requiring intensive care. With toxic infections, the lethality is low (about 1%), which cannot be said about mushroom poisoning.
Prevention of food poisoning in a child dictates the need for proper storage and adequate heat treatment of food products, drinking only boiled water, thorough washing of hands and food under running water. Regular hygienic examination of persons working in children's kitchens and in public catering is necessary; preventing workers with pustular skin diseases (pyoderma), respiratory tract infections, intestinal infections from entering the catering department.
It is necessary to acquaint children with poisonous plants and mushrooms, and strictly forbid them to eat unknown berries, fruits, seeds, etc.
You can share your medical history, what helped you in the treatment of food poisoning in a child.
Sources
- In case of pain or other exacerbation of the disease, only the attending physician should prescribe diagnostic tests.