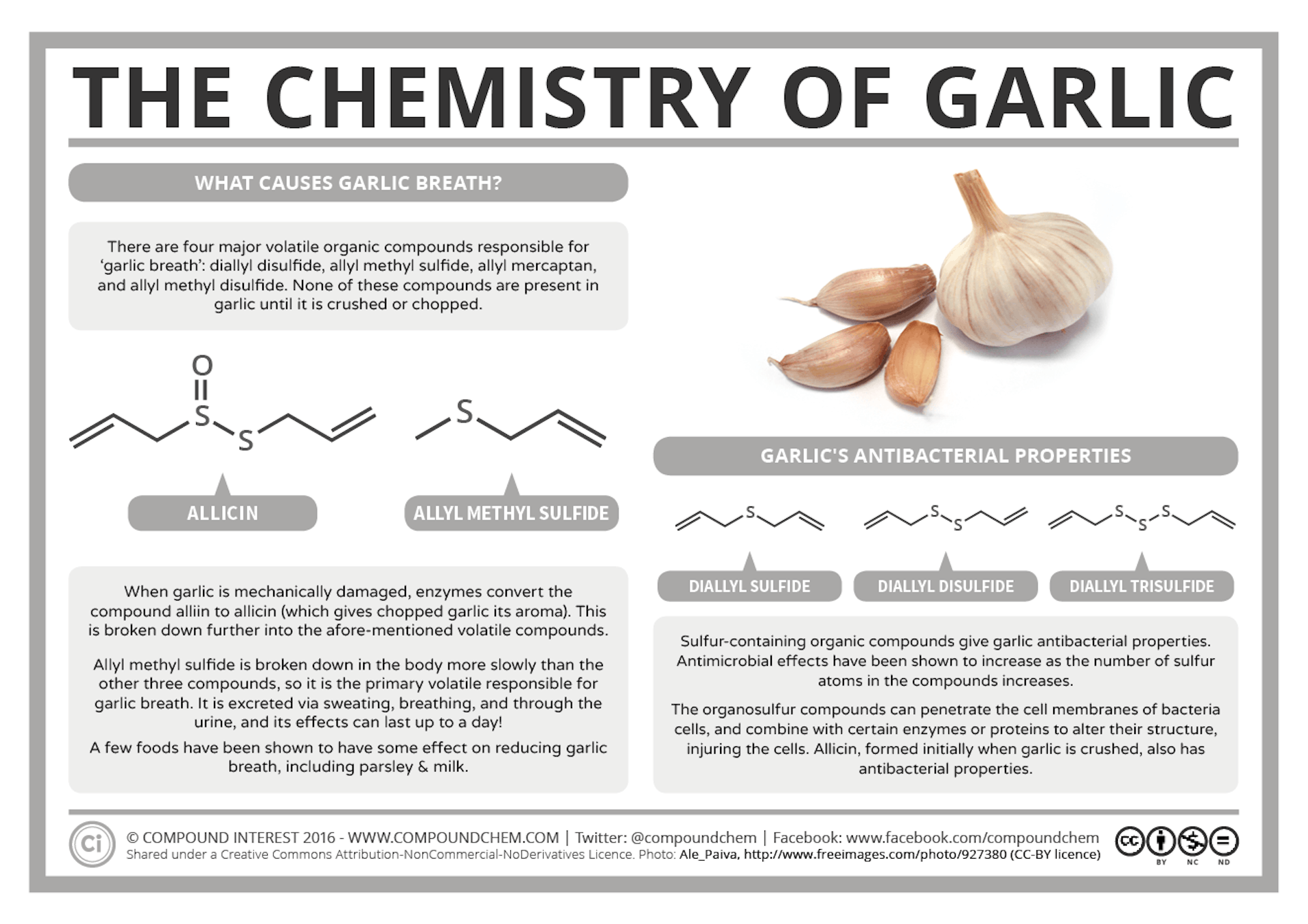
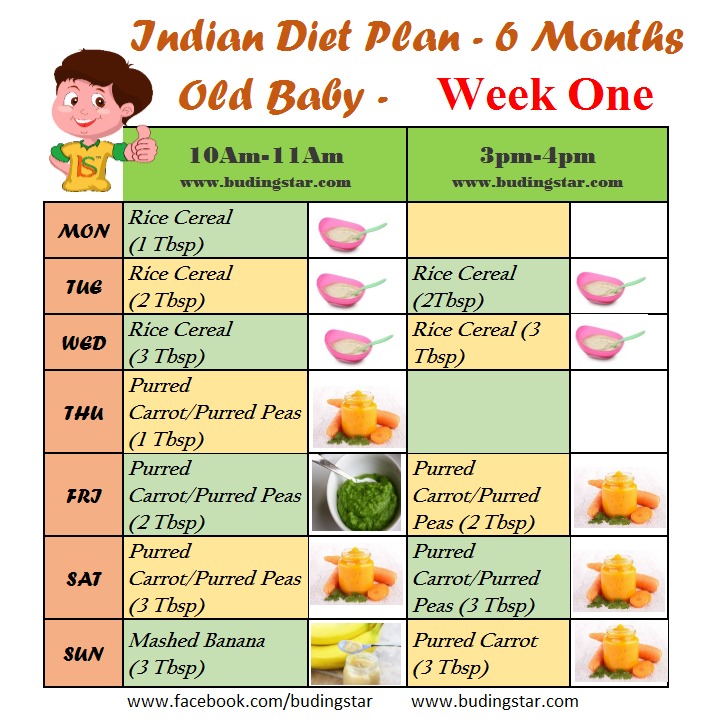
Feeding baby with finger
Using expressed breast milk for extra feeds
Using expressed breast milk for extra feeds
There are a number of ways to use your expressed breast milk to feed your baby.
Finger feeding
Finger feeding is a way of giving your baby expressed breast milk without using a bottle teat as some babies may take preference to a teat and refuse the breast. Finger feeding uses a bottle with a thin tube rather than a teat.
Note: Nails should be trimmed short and artificial nails should be secure.
How to finger feed
- After washing your hands, securely wrap your baby.
- Sit in a comfortable position.
- Support your baby with a pillow.
- Using the index or middle finger gently stroke your baby’s lips from the chin upwards until your baby’s mouth is open.
- Allow the baby to begin sucking your finger (with your finger pad towards the top of your baby’s mouth).
- If your baby is sleepy gently introduce your finger into their mouth. If your baby’s lower lip is sucked in, pull down on the chin to release baby’s lip.
- Insert large end of the tube into the bottle below the milk line.
- Gently insert the tube alongside your finger to the finger tip and raise the bottle so that the expressed breast milk flows down the tube.
- The technique is working if the baby is drinking. If the feeding is very slow – but the baby is swallowing well – raise the bottle to increase the flow. If your baby is gulping, lower the bottle to slow the flow.
Cup feeding
Cup feeding is an alternative means of providing colostrum (the first milk you produce which contains substances to nourish your baby and protect from disease) or expressed breast milk (not formula) to babies unable to attach and/or suck at the breast successfully. It is most successful when your baby is wide awake and interested.
How to cup feed
- Wrap your baby securely.
- Support your baby in an upright sitting position.
- Fill a small clean medicine cup half full with expressed breast milk.
- Tip the cup so that the milk is touching your baby’s lips. Do not pour the milk into your baby’s mouth.
- Tilt the rim of the cup touching the baby’s bottom lip, towards the upper lips and gums.
- As your baby’s jaw is lowered, a small amount of feed will be taken and swallowed.
- Leave the cup in the correct position during the feed as this allows your baby to self regulate the feed as desired.
- After use, wash the cup in warm soapy water and rinse well.
Paced bottle feeding for older breastfed infants
Using a bottle is another method of giving your baby expressed breast milk. A bottle teat does not always allow a baby to ‘pace’ their intake as they do when breastfeeding.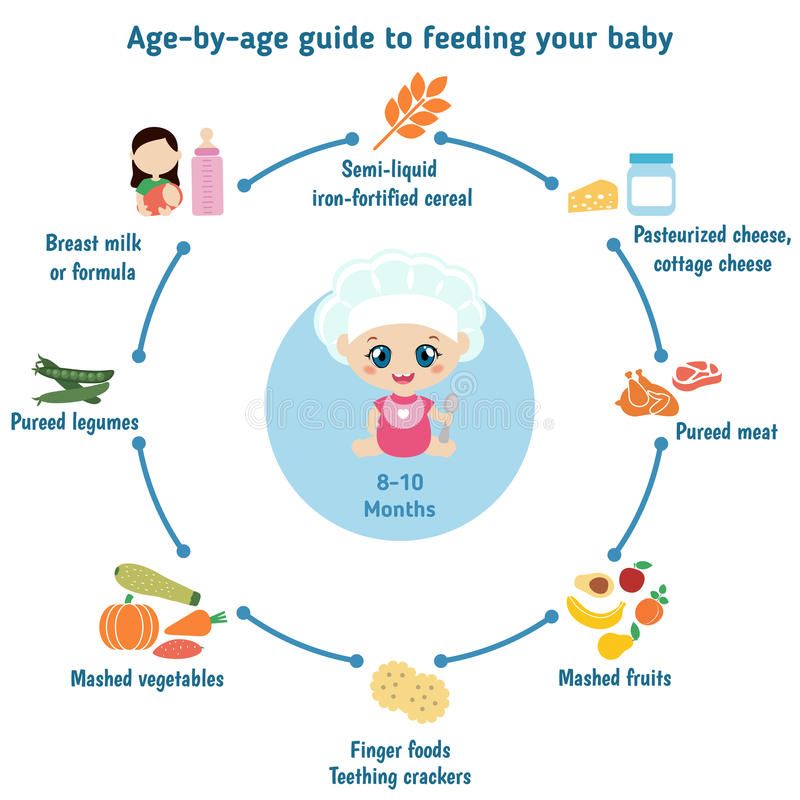 If the bottle is held vertically, the milk pours out. It is important to adjust the angle of the bottle to allow your baby to ‘pace’ themselves.
If the bottle is held vertically, the milk pours out. It is important to adjust the angle of the bottle to allow your baby to ‘pace’ themselves.
- Place your baby in a more upright position than ‘traditional’ bottle feeding techniques.
- Support the baby’s back so the baby’s head can extend into a natural drinking position.
- Use a slow-flow round teat.
- Stroke the bottle teat gently from the baby’s chin up to the lower lip to encourage him or her to make a wide-open mouth. When your baby has a wide-open mouth, place the entire teat into his or her mouth.
Important: Avoid pushing the teat into a baby’s mouth that is not open. - Hold the bottle horizontally so there is just enough milk in the teat. This will ensure no air is in the tip of the teat and encourage your baby to suck on the teat without gulping or using their tongue to slow the flow.

- Withdraw the teat slightly every few minutes to allow your baby to take a pause as they would naturally on the breast.
- Switch sides to assist with eye stimulation and to prevent preference for one side.
- As the amount of milk in the bottle decreases, gradually lean your baby backward.
How long should a ‘paced’ bottle feed take?
You should aim for the feed to take at least 20 minutes. If a feed takes less time than this the flow is too fast, and if the feed takes more than 45 minutes then the flow is too slow.
Watch your baby’s cues to know when to finish the feed rather than encouraging them to finish the bottle.
Where to get help
Breastfeeding Centre of WA
- Counselling and appointments 8.00am to 4.00pm Monday to Friday
- Phone: (08) 6458 1844
- More information about Breastfeeding Centre of WA
Australian Breastfeeding Association (ABA)
- National Breastfeeding Helpline available 24 hours, 7 days a week
- Phone: 1800 mum 2 mum (1800 686 268)
- Visit the ABA website (external site)
Ngala Parenting Line
- Phone: (08) 9368 9368 – 8.
 00am to 8.00pm 7 days a week
00am to 8.00pm 7 days a week - Outside metro area – Free call 1800 111 546 (free from land line only)
- Visit the Ngala website (external site)
You can also:
- See your doctor
- Visit healthdirect (external site) or call 1800 022 222
Acknowledgements
Breastfeeding Centre of WA
This publication is provided for education and information purposes only. It is not a substitute for professional medical care. Information about a therapy, service, product or treatment does not imply endorsement and is not intended to replace advice from your healthcare professional. Readers should note that over time currency and completeness of the information may change. All users should seek advice from a qualified healthcare professional for a diagnosis and answers to their medical questions.
See also
- Signs your breast milk is flowing
- Expressing and storing breast milk
What is Finger Feeding? - Breastfeeding Support
Finger feeding involves a baby receiving breast milk or formula via a very narrow feeding tube while they suckle your finger. When a baby sucks on finger and tube together with their tongue in the right position, and with their lips making a seal on the finger, milk is drawn up the feeding tube from a container of milk. A curved tip syringe can also be used to drip milk into a baby’s mouth alongside the finger instead of a tube. Finger feeding is an alternative to using a bottle or cup if a baby needs a supplement and it can also be used as a suck training technique. This article looks at the ways finger feeding can be useful, how to do it, and the pros and cons with this technique.
When a baby sucks on finger and tube together with their tongue in the right position, and with their lips making a seal on the finger, milk is drawn up the feeding tube from a container of milk. A curved tip syringe can also be used to drip milk into a baby’s mouth alongside the finger instead of a tube. Finger feeding is an alternative to using a bottle or cup if a baby needs a supplement and it can also be used as a suck training technique. This article looks at the ways finger feeding can be useful, how to do it, and the pros and cons with this technique.
Sign Up to the Newsletter
Get breastfeeding articles in your inbox
Advantages of finger feeding
When a baby needs supplementary feeds, some authors feel that finger feeding may help to preserve the breastfeeding relationship compared to cup feeding or bottle feeding. Reasons include:
- Finger feeding uses a similar sucking technique to breastfeeding ie the same muscles are used and both methods allow the baby to control the flow of milk and pace the feed.
 1
1 - Finger feeding promotes skin-to-skin contact (between tongue and finger) and the finger tip reaches the same position deep in the mouth as the nipple (Wambach and Spencer, 2021).
- Finger feeding avoids introducing nipple confusion or bottle preference before breastfeeding is well established which can sometimes happen with the use of artificial teats. Note: Although there are differences between breastfeeding and bottle feeding, bottle preference and nipple confusion can be minimised by these Tips to Bottle Feed a Breastfed Baby and see Best Bottle for a Breastfed Baby? If used regularly, babies could equally have “finger preference” and reject the breast in favour of a finger feed.
When is finger feeding useful?
Finger feeding can be useful in a number of situations:
#1 To feed a baby
- Finger feeding keeps a baby well fed if they are not latching (attaching) to the breast, not breastfeeding well, or refusing a bottle.

- Separation from mother. If a breastfed baby is separated from their mother, finger feeding could be a feeding option to consider alongside cup feeding, syringe feeding or bottle feeding. One study of 53 babies showed preterm babies who were finger-fed had less milk loss, and fewer complications compared with cup feeding.2
#2 When baby won’t latch
- If a baby can’t latch to the breast yet, finger feeding may help to prepare a baby for breastfeeding3 because the sucking technique needed is similar to that which will be used at breast. For more reading see When Baby Won’t Breastfeed.

- Finger feeding can be used to wake up a non-latching sleepy newborn baby to give them some calories4 or to calm a hungry and frustrated baby and take the edge off their appetite before latching. Note: a baby who is very sleepy or has low stamina from being underweight may struggle to take adequate volumes with finger feeding as a sole method of supplementation and careful use of a bottle and teat may be more appropriate.
#3 Improving sucking skills
Because finger feeding has similarities to breastfeeding, finger feeding is sometimes suggested as a suck training technique to improve sucking skills or tongue function (see below).5 Finger feeding is said to reinforce good breastfeeding technique because:
- Baby has to keep his tongue down and forward in his mouth to cover his gums
- Baby uses a wide open mouth on the finger to recreate a deep latch—use your largest finger
- Baby has to suck actively to bring milk up the tube, just as he does at the breast to initiate a let-down (milk ejection reflex)
- Baby can control the flow of milk, if he doesn’t suck there will be a pause in milk flow
- Baby becomes familiar with the feel of skin in their mouth rather than a silicone teat.
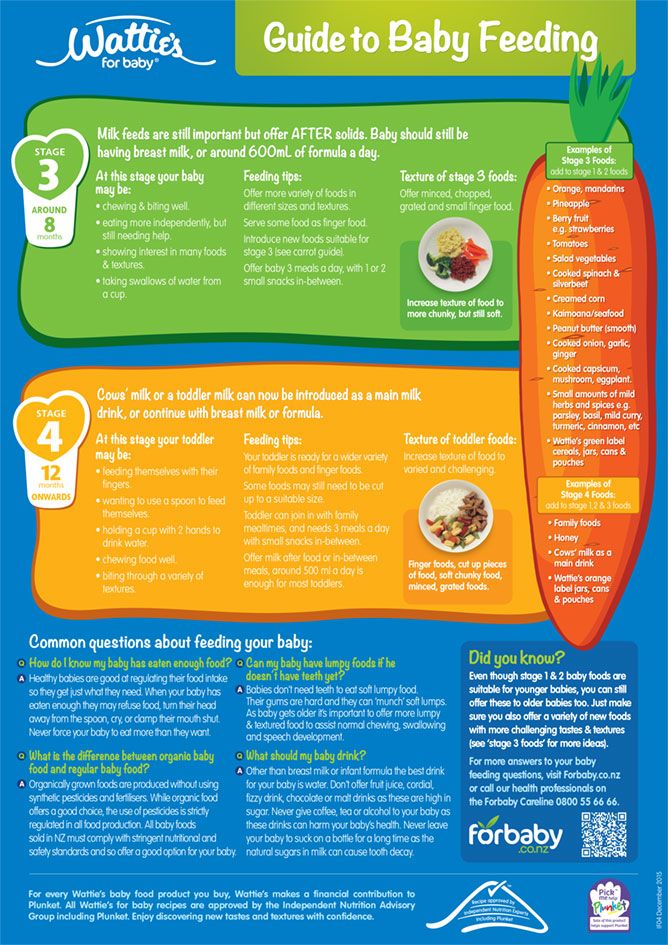
#4 Respite from sore nipples
Finger feeding can be used for a day or two if a mother’s nipples are too sore and damaged to breastfeed to give them a chance to heal without introducing bottles. However, Jack Newman, a Canadian paediatrician and breastfeeding expert, cautions against interrupting breastfeeding unless absolutely necessary as sometimes a baby can be reluctant to go back to the breast.6 Breastfeeding can often continue uninterrupted with sore nipples once positioning has improved the latch. See Causes of Sore Nipples and Treatments for Sore Nipples for help for sore nipples.
Finger feeding is when a baby gets milk from a narrow feeding tube while they suckle on a finger or thumbDisadvantages of finger feeding
- Finger feeding is not appropriate for all babies. Some babies may find it difficult to get milk via the tube.
 Underweight babies may not have enough stamina to use the tube effectively. Alternatives include cup feeding or see our Tips to Bottle Feed a Breastfed Baby. If the baby can breastfeed, then additional milk can be given via feeding tube directly at the breast, see Supplementing at the Breast.
Underweight babies may not have enough stamina to use the tube effectively. Alternatives include cup feeding or see our Tips to Bottle Feed a Breastfed Baby. If the baby can breastfeed, then additional milk can be given via feeding tube directly at the breast, see Supplementing at the Breast. - Cleaning the tubes properly is difficult and could put your baby at risk of an infection. See Homemade Supplemental Nursing System for more information about cleaning homemade systems and see below.
- It can be quite awkward to finger feed especially if milk leaks in a homemade system and it can be difficult to source feeding tubes. Some babies figure out a way to suck on the tube like a straw rather than use a breastfeeding technique.
- The flow of milk may be too fast or too slow—however flow rate can be increased with a larger diameter tube, using two tubes, or by holding the container of milk above baby’s head. Flow can be decreased with a smaller diameter tube or lowering the position of the container.

- A sore mouth? If the tube is held on top of a finger it could rub against the roof of your baby’s mouth (the hard palate) potentially causing soreness. Having the tube running along the side of your finger may help so that the tube enters the corner of baby’s mouth instead of running across the hard palate.
- A finger is not the same as a breast, more research is needed on the safety and long term implications of finger feeding. For some babies finger feeding may negatively affect breastfeeding. Pushing a finger too far into baby’s mouth, or the tube extending further than a finger tip could cause gagging or discomfort. It’s important to watch your baby closely for signs of stress or they could start to resist anything entering their mouth—including a breast (oral aversion).
A step by step guide to finger feeding
Finger feeding is best shown in person by your IBCLC lactation consultant or health care professional. Detailed instructions for finger feeding can be found in Jack Newman’s article Finger and Cup Feeding or in Supporting Sucking Skills in Breastfeeding Infants or Breastfeeding and Human Lactation (2021. p 196). Information for using the Hazelbaker™ FingerFeeder can be found on fingerfeeder.com
Detailed instructions for finger feeding can be found in Jack Newman’s article Finger and Cup Feeding or in Supporting Sucking Skills in Breastfeeding Infants or Breastfeeding and Human Lactation (2021. p 196). Information for using the Hazelbaker™ FingerFeeder can be found on fingerfeeder.com
The steps for finger feeding with a feeding tube include:
- Trim long finger nails and wash your hands prior to finger feeding.
- Hold your baby so that he can comfortably suckle your finger when it is held flat in his mouth. Baby’s head should be stable and slightly tilted back (Wambach and Spencer, 2021).
- Hold the rounded end of a small feeding tube (e.g. 5fr or 6fr) along the side of your finger or tape it in position if preferred, the end of the tube should be close to but not extend past your finger tip. Use a large finger or thumb to fill a baby’s mouth like the breast (Wambach and Spencer, 2021).

- Check that the opposite end of the tube is submerged in your expressed breast milk or formula and that the cap on this end of the tube is open.
- Encourage a wide gape—by brushing your finger against your baby’s lips. Never force a finger into your baby’s mouth always encourage the gaping reflex first.
- Slide your finger gently along your baby’s hard palate so that the soft pad of your finger tip is uppermost and resting against the roof of your baby’s mouth. Let your baby take your finger into his mouth as far as he is comfortable—avoid going too far to cause gagging or discomfort. Your baby will normally grasp the finger with his tongue and suck it deeply into his mouth so that the finger pad rests towards the back of his mouth at the junction of the hard and soft palates—some authors call this the “S-spot”.7 The nail side of your finger should be centred against the tongue.
 If your baby seems to gag on even your finger tip, contact your IBCLC lactation consultant.
If your baby seems to gag on even your finger tip, contact your IBCLC lactation consultant. - Check your baby’s lips are not folded in, the top lip should rest on your finger making a seal and the lower lip be turned out. Pull on the chin gently just enough to bring the lip out if it is tucked in. If baby doesn’t have good lip seal, milk may leak from the mouth.
- Try to keep your finger straight or flat to help encourage the correct tongue position and without applying pressure to the roof of your baby’s mouth, only maintain gentle contact. Good contact with the centre of baby’s tongue and his hard palate recreates the right position of the breast and nipple in baby’s mouth.
- Your baby will receive milk via the feeding tube at his own pace and the milk will gradually be drained from the bottle or container. Milk delivery is stopped when the tongue pulls back or the back of the tongue is humped against the finger, and resumed when the tongue tip is brought back over the gum ridge and the back of the tongue drops slightly.
 If your baby isn’t motivated to keep sucking long enough to draw milk up the tube, the tube can be prefilled with milk by inserting a blunt ended syringe of milk into the cap at the end of the tube.
If your baby isn’t motivated to keep sucking long enough to draw milk up the tube, the tube can be prefilled with milk by inserting a blunt ended syringe of milk into the cap at the end of the tube. - Monitor baby for signs of stress (frowning, finger splaying, turning away) and check whether they are coping well with organising sucking, swallowing and breathing when feeding with the tube in place. Check that the tube is not rubbing against the roof of your baby’s mouth.
Finger feeding variations with a syringe
- A blunt ended syringe can be used to house the supplement at the end of the feeding tube. The advantage of this system is that the feeder can slowly push the plunger down on the filled syringe to maintain a steady flow of milk when baby is sucking; pausing as needed for baby to swallow or rest.
- A curved tip syringe can also be used to introduce milk along your finger while baby suckles.
The disadvantage of using a syringe is that it can be difficult to hold baby and negotiate finger feeding and pushing the syringe at the same time without another pair of hands. The feed may need to be interrupted to refill the syringe and it is important to regulate the flow of milk carefully so as not to choke or overwhelm the baby.
The feed may need to be interrupted to refill the syringe and it is important to regulate the flow of milk carefully so as not to choke or overwhelm the baby.
Finger feeding for suck training
Suck training is when exercises are used to improve a baby’s immature or suboptimal sucking technique to help them breastfeed (or bottle feed) more effectively. This may involve stroking movements/massage of the tongue or gums and finger feeding can also be used as a suck training exercise. Advocates of suck training feel it can help to optimise feeding reflexes eg the way the tongue moves during feeding and familiarise a baby with the desired position of the nipple deep in baby’s mouth. Conversely, authors Wambach and Spencer point out that some practitioners feel that suck training is invasive and controlling and should never be used.8
There are many versions of suck training that individual therapists favour but no standard protocols (Wambach and Spencer, 2021 p80). Decisions on specific exercises are best discussed with speech and language therapists (SALT), your lactation consultant or see the latest editions of text books such as Breastfeeding and Human Lactation and Supporting Sucking Skills in Breastfeeding Infants for a detailed overview.
Decisions on specific exercises are best discussed with speech and language therapists (SALT), your lactation consultant or see the latest editions of text books such as Breastfeeding and Human Lactation and Supporting Sucking Skills in Breastfeeding Infants for a detailed overview.
Cautions for suck training exercises
- Carry out suck training under the guidance of your IBCLC lactation consultant or other experienced health care professional eg a speech and language therapist (SALT). It is important to rule out positioning, attachment, mother’s anatomy, baby’s oral anatomy or even whether baby is very underweight to explain any breastfeeding issues before embarking on suck training. A therapist will choose appropriate exercises for specific suck issues.
- Mouth and tongue exercises should always be gentle and enjoyable for a baby. It’s important to be sensitive to your baby’s responses and stop an exercise if your baby is not enjoying it.
 Irritating your baby with intrusive exercises in his mouth could cause him to refuse anything in his mouth including a breast (called oral aversion).
Irritating your baby with intrusive exercises in his mouth could cause him to refuse anything in his mouth including a breast (called oral aversion). - If finger feeding exercises don’t help or a baby doesn’t seem to enjoy the exercises, another strategy should be considered. Contact your IBCLC lactation consultant.
The need for a full assessment
Finger feeding can be used as a form of suck training to help improve the way the tongue moves during feeding and encourage the tongue forward in the baby’s mouth (tongue extension) (Watson Genna, 2017; Marmet and Shell, 1984). A baby who doesn’t bring his tongue forward to cup the breast will find it harder to maintain suction on the breast and if the tongue isn’t extended over the lower gum ridge during a breastfeed, the mother may feel a biting sensation or complain of sore nipples. However there can be many simple explanations for “biting” or soreness hence the need to first rule out other causes of sore nipples with your breastfeeding specialist such as poor positioning, shallow attachment at the breast, high muscle tone, fast-flow, tongue-tie or hunger, before using sucking exercises.
Where can I get a finger feeding supplementer?
It is possible to buy a purpose made finger feeder online called the Hazelbaker™ FingerFeeder (email [email protected]) or to use the tubes from a Medela Supplemental Nursing System. The instructions for making a homemade finger feeding tool for short term use can be found in Homemade Supplemental Nursing System. The equipment and the first four steps of “setting up” are the same as when making a homemade at-breast supplemental system.
Where can I get feeding tubes for a homemade system?
Your IBCLC lactation consultant may carry feeding tubes for finger feeding and plastic syringes to clean them, or they may know of a local supplier. Many medical suppliers in UK sell individually wrapped sterile feeding tubes (nasogastric tubes) by the box however it can be difficult for parents to source small numbers of tubes. Note: using a nasogastric tube for finger feeding is not using a device according to the manufacturer’s intended use. Nasogastric tubes are intended to carry milk to babies internally via the back of their nose and throat to the stomach. This means parents use tubes for finger feeding at their own risk without the protection of a manufacturer’s guarantee.
Nasogastric tubes are intended to carry milk to babies internally via the back of their nose and throat to the stomach. This means parents use tubes for finger feeding at their own risk without the protection of a manufacturer’s guarantee.
How can I clean the tubes?
While commercially made supplementers are made to withstand sterilising—disposable feeding tubes from a homemade system are not intended for reusing in this way and won’t stand up to boiling or steam sterilisation. See Homemade Supplemental Nursing System for cleaning information—tubes can be rinsed out straight after use by using a syringe in the end-cap to push cooled, previously boiled, water through the tube several times to remove milk.9 Some authors advocate flushing the tubes through with hot soapy water after removing the visible milk, and finally rinsing well.10 Residual water can be forced out of the tube by shaking the tube in a lasso action. Some mothers store washed tubes in a refrigerator between uses. Instructions for cleaning commercial devices will be supplied with the equipment or online e.g. see How Do I Clean the Hazelbaker™ FingerFeeder?
Some mothers store washed tubes in a refrigerator between uses. Instructions for cleaning commercial devices will be supplied with the equipment or online e.g. see How Do I Clean the Hazelbaker™ FingerFeeder?
Replace tubes regularly
If you are using a disposable feeding tube it should be replaced with a new tube frequently, some mothers use a new tube each feed or every day. If they are cleaned thoroughly however, Dr Jack Newman 11 suggests tubes can be washed and reused for a few days before replacing.
Baby receives milk via the feeding tube at his own paceIs long term finger feeding safe?
Finger feeding information does not seem to be based on any extensive research studies and relies on the experience of practitioners in the field who have used this technique. A breast widens a baby’s palate in a way that a bottle teat or finger can’t and tubes are difficult to clean properly. There is a risk of oral aversion if finger-feeding is not done respectfully. Until more research is available it would seem appropriate to limit finger feeding to short term use for encouraging a baby back to breast and suck training exercises under supervision. Alison Hazelbaker explains:
Until more research is available it would seem appropriate to limit finger feeding to short term use for encouraging a baby back to breast and suck training exercises under supervision. Alison Hazelbaker explains:
Excerpt from
FAQs, 2009, fingerfeeder.com
Breastfeeding still remains the ideal way to feed babies. Finger-feeding should be used only as a means to correct sucking problems or to keep the baby well fed until he or she can go to breast.
One study in Australia 12 found that finger-feeding as part of the feeding regimen ensured that a larger percentage of babies in the NICU were able to transition to breast successfully, whereas their bottle-feeding counterparts were less likely to do so. No other study has looked at finger-feeding.
Summary
Finger feeding is when a baby gets milk from a narrow feeding tube while they suckle on one of your fingers.![]() Variations include dripping milk into baby’s mouth with a curved tip syringe while they suckle on a finger, or pushing milk along the feeding tube into baby’s mouth via a reservoir of milk in a syringe. Finger feeding a baby can be an alternative to using a bottle or cup if a baby isn’t breastfeeding yet or needs supplements, and it can also be used as a suck training technique to improve a baby’s sucking skills. There isn’t any substantial research on the safety of finger feeding and most information has been provided through the experience of lactation consultants who have used finger feeding in their work. It is recommended to carry out finger feeding under the guidance of your IBCLC lactation consultant or other health care professional.
Variations include dripping milk into baby’s mouth with a curved tip syringe while they suckle on a finger, or pushing milk along the feeding tube into baby’s mouth via a reservoir of milk in a syringe. Finger feeding a baby can be an alternative to using a bottle or cup if a baby isn’t breastfeeding yet or needs supplements, and it can also be used as a suck training technique to improve a baby’s sucking skills. There isn’t any substantial research on the safety of finger feeding and most information has been provided through the experience of lactation consultants who have used finger feeding in their work. It is recommended to carry out finger feeding under the guidance of your IBCLC lactation consultant or other health care professional.
Footnotes & References
-
Wambach and Spencer. Breastfeeding and Human Lactation. 6e 2021 p 195
-
Moreira et al. Comparison of the finger-feeding versus cup feeding methods in the transition from gastric to oral feeding in preterm infants.
 J Pediatr (Rio J) 93(6):585-591, 2017
J Pediatr (Rio J) 93(6):585-591, 2017 -
Karabayir N, Mertturk Potak E, Karaman S, et al. (April 11, 2022) The Finger Feeding Method and Relactation. Cureus 14(4): e24044. doi:10.7759/cureus.24044
-
Finger and Cup Feeding, Jack Newman and Edith Kernerman, updated 2021
-
Buldur et al. Comparison of the Finger Feeding Method Versus Syringe Feeding Method in Supporting Sucking Skills of Preterm Babies. Breastfeeding Medicine. 2020
-
Finger and Cup Feeding, Jack Newman and Edith Kernerman,updated 2021
-
Training Neonates To Suck Correctly, Maternal Child Nursing, Marmet and Shell, 1984
-
Breastfeeding and Human Lactation, Wambach and Spencer, 2021 p80
-
Breastfeeding and Using a Supply Line, Royal Women’s Hospital, 2018
-
Counseling the Nursing Mother, Lauwers and Swisher, 2011
-
Lactation Aid, Jack Newman, updated 2021
-
Implementing the Baby Friendly Hospital Initiative: the role of finger feeding, Oddy and Glenn, 2003
Finger feeding as a safe way to supplement, Mom's Milk Center 99-76-60
04/07/2017 Views: 19533.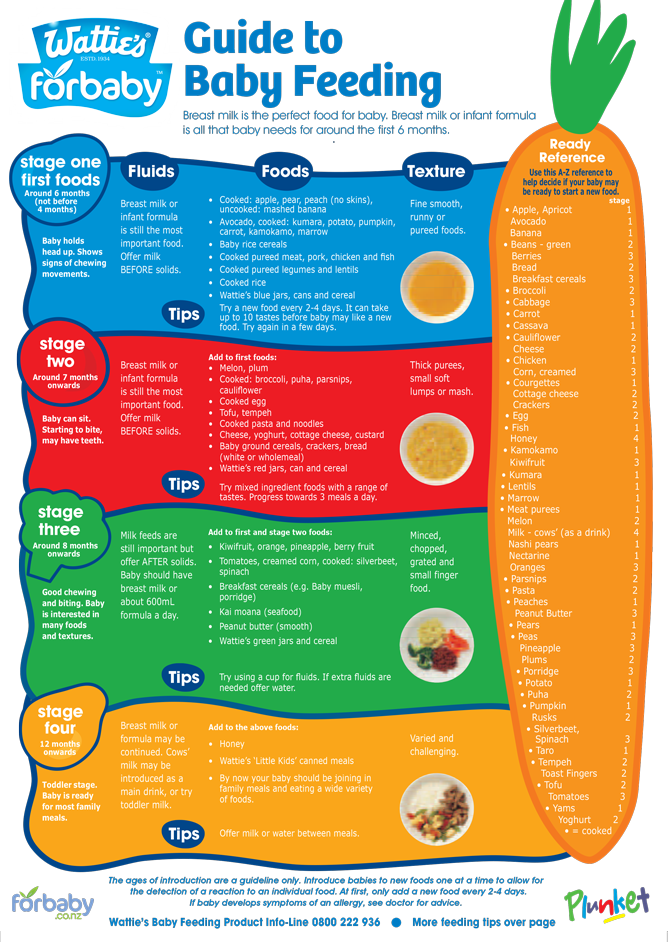
Olga Grigoryeva , Breastfeeding consultant, midwife Rodzala:
Sometimes mothers (and consultants) are faced with the fact that they have to give (temporarily!) the child is supplemented with expressed milk, and in the case of a consultant with a lack of milk in the mother, with an artificial mixture. nine0022
.
Of course, a bottle with a nipple is a more familiar, and unfortunately, widespread means of feeding an infant. But, despite the popularity of the method, this method of supplementation is the only wrong one.
If you want to breastfeed your baby, then you do not need to use a pacifier (pacifier, bottle). This method threatens your breastfeeding. Practice shows that when using bottle feeding, children often refuse to breastfeed, the breast latch deteriorates and other problems appear (see article on pacifiers). nine0005
nine0005
One of the safest and most convenient ways to supplement is by syringe and thumb sucking. It is very well suited for the introduction of large volumes of supplementary feeding, it is an easy and cheap way.
All you need for this method of supplementation is a disposable syringe (no needle) and clean hands (the counselor uses sterile gloves). Instead of a syringe, you can use a thin probe (sold in pharmacies)
But the main purpose of the finger feeding method is to help teach the child to take the breast, which for various reasons the child cannot (cannot) suck or sucks inefficiently.
Finger feeding can be used if:
- Baby refuses to breastfeed
- Weak sucking reflex
- If the baby is too sleepy at the breast, sluggish suckling ( a very good way to wake up a sleepy baby in the first days of life)
- The baby appears to be unable to latch on properly and therefore cannot suckle milk well.
- When switching from bottle feeding to breastfeeding.
- Mother and child are separated from each other for some reason.
- Breastfeeding had to be temporarily interrupted (although there are very LITTLE reasons why breastfeeding should really be interrupted). nine0022
But often, when offering such a method of feeding, lactation consultants have to see the negative reaction of mothers: unphysiological, unhygienic, not accepted, unusual, etc.
I want to dispel these myths. Even in utero, on ultrasound, we can see how the child entertains himself by sucking his thumb. Also, by sucking fingers and fists, a child can show us that he is hungry. that is, thumb sucking is a completely physiological phenomenon. nine0005
Also, finger feeding is LIKE breastfeeding, unlike bottle feeding.
To suck a finger, the child must lower and protrude the tongue over the lower gum, keep the mouth wide open (the larger the finger used, the better), and the lower jaw slightly forward (which does not happen at all when sucking a bottle). Moreover, the movements of the tongue and lower jaw are similar to those that a baby does when suckling at the breast . Therefore, finger feeding works best to prepare a baby who refuses to breastfeed for attachment.
Moreover, the movements of the tongue and lower jaw are similar to those that a baby does when suckling at the breast . Therefore, finger feeding works best to prepare a baby who refuses to breastfeed for attachment.
As a specialist in speech massage, I can say with confidence that thumb sucking during feeding or before attachment to the breast (in case of refusal, ineffective sucking) is similar to massage of the tongue by a speech therapist in older children with speech disorders. Finger feeding an infant (as well as speech therapy massage) results in better tongue function and reduced sucking problems (more effective sucking) in the same way that tongue massage helps to solve speech problems in children with speech disorders. nine0022
During feeding, mother regulates the degree of pressure on the tongue with her finger, controls the correct position of the tongue during sucking, the degree of suction of the tongue to the finger (vacuum).
Moms have doubts about hygiene and rejection of this method, but! firstly, the mother thoroughly washes her hands before feeding, her nails should be cut short, and secondly, this area of skin on the finger is practically no different from the area of skin on the chest in terms of the amount of bacteria on it. nine0005
As for what is stupid, funny, embarrassing, unusual - these are nothing more than unfounded prejudices and stereotypes that need to be disposed of by prioritizing in favor of breastfeeding.
Finger Feeding Technique (it is best learned by living example by watching and doing)
You will need a disposable syringe without a needle (5 ml, 10 ml or 20 ml)
1. Draw up expressed breast milk (mixture) into the syringe
2. Place the baby in a reclining position, at a 45 degree angle (you can use a pillow)
3. Let the baby suck his clean finger with the pad up (usually the baby sucks the finger very deeply
Let the baby suck his clean finger with the pad up (usually the baby sucks the finger very deeply
4. Gently press the back of your finger on the child's lower gum, making sure that the lower lip is not turned inward. tongue between the lower gum and mom's finger. nine0005
5. We put the spout (tube) of the syringe on the side surface of our finger and move the syringe along it, carefully inserting the tube into the corner of the child's mouth.
6. Baby begins to suck on his thumb and mother (or counselor) slowly squirts milk after every 1-2 sucking movements of the baby.
To feed a baby with a probe, we only need a tube, everything else needs to be cut off. We place one end of the probe in any container, glass or bottle of milk. We place the other end of the tube parallel to the index finger, so that it runs along its pad, but the tip of the probe should not protrude beyond the finger. Then we put the finger together with the tube in the child's mouth. The milk container should be slightly higher than a finger so that milk enters the baby's mouth. You can adjust the rate of milk flow - by raising it higher, or vice versa by lowering the bottle of milk lower. nine0005
Then we put the finger together with the tube in the child's mouth. The milk container should be slightly higher than a finger so that milk enters the baby's mouth. You can adjust the rate of milk flow - by raising it higher, or vice versa by lowering the bottle of milk lower. nine0005
Finger syringe feeding is recommended by WHO and is used in Baby Friendly Hospitals worldwide.
!!!If you want to breastfeed successfully, do not use other suckling objects other than breasts at least until your breastfeeding is well established!!!
nine0005
Breastfeeding Hotline Ryazan 99-76-60
A lactation consultant will teach you how to finger feed at visit
Breastfeeding Support Center Mamino Moloko would like to thank newborn photographer Tatyana Ivashkova>>
for help (taking photos and videos for the article)
nine0005
COMMENT ON THE ARTICLE ON THE FORUM>>
Photo of finger tube feeding see below
Call consultant
Nursing clothes, slings
Like this article? 38
Share
Various breastfeeding positions
Try different breastfeeding positions to find the one that works best for you and your baby. You can see the options in our selection of photos
You can see the options in our selection of photos
Share this information
There is no right or wrong way to hold the baby while feeding
, and mom and baby are sure to find their favorite position.
It is important that both you and your child feel comfortable. 1.2 It's good to learn a few different breastfeeding positions and techniques because life's circumstances often require us to be flexible, especially as your baby gets older and you start to leave the house more often. nine0005
Whatever position you choose to breastfeed your baby, remember a few simple rules.
- Prepare everything you need before feeding, including drinks, food, mobile phone, TV remote control, book or magazine. And do not forget to go to the toilet - the feeding process can take a long time!
- Make sure your baby is comfortable. Whichever position you choose, it's important to keep your baby strong, level, and provide good support for their head, neck, and spine.
 nine0075
nine0075 - You should also be comfortable. Don't stress. If necessary, use pillows of different sizes or rolls of towels to support your back or arms.
- Make sure your baby is latching on correctly. Proper grip is the key to comfort when breastfeeding.
- If your baby does not latch on well or you experience pain while feeding, contact a lactation consultant for help. The specialist will also be able to show you how to hold your baby more comfortably. nine0075
1. Relaxed feeding or reclining position
The relaxed feeding position, also known as biological feeding, 1 is often the first position for most mothers. If, immediately after birth, the baby is placed on the mother’s chest or stomach, normally, he instinctively reaches for the breast and tries to grab the nipple. This phenomenon is known as the breast seeking reflex. Skin-to-skin contact stimulates the infant's feeding instinct, and gravity helps him to latch onto the breast and maintain balance. nine0005
nine0005
But it's not just newborns that can be fed in the reclining position - this position is great for babies of all ages. It can be especially helpful if your baby does not latch well in other positions or does not like to be touched during feeding, and also if you have too much milk flow or too large breasts. Isabelle, a mother from the UK, shares her experience: “I had large breasts, and the baby was born small - 2.7 kg, so it was not easy to find a comfortable position at first. After a few weeks, it became clear that there was no “correct” posture for me. As a result, I most often fed lying down, putting the baby on my chest. ” nine0005
It is more convenient to feed not lying flat on your back, but half-sitting, leaning on pillows. So you will have a back support and you will be able to watch the baby during feeding.
2. Cradle position
This is the classic position that comes to mind first when we talk about breastfeeding
. Mom sits straight
, and the baby lies on her side on her arm, pressing her stomach against her stomach. 3 Although this is a very popular position, it is not always easy to master with newborns because it gives the baby less support. Try putting a pillow under your back, and put a special breastfeeding pillow on your knees and lean on it with your hands. So you can more reliably support the child, without overstraining your back and shoulders. Just make sure that the baby does not lie too high on the pillow for feeding. The breast should remain at a natural level so that the baby can grab it without effort, otherwise sore nipples cannot be avoided. nine0005
3 Although this is a very popular position, it is not always easy to master with newborns because it gives the baby less support. Try putting a pillow under your back, and put a special breastfeeding pillow on your knees and lean on it with your hands. So you can more reliably support the child, without overstraining your back and shoulders. Just make sure that the baby does not lie too high on the pillow for feeding. The breast should remain at a natural level so that the baby can grab it without effort, otherwise sore nipples cannot be avoided. nine0005
“I breastfed in the cradle position because it suited me perfectly! It was comfortable and I loved just sitting and looking at my little one,” recalls Rachel, a mother of two from Italy.
3. Cross Cradle
This breastfeeding position looks almost the same as the Cradle, but the baby is on the other arm. 3 This gives baby support around the neck and shoulders so he can tilt his head to latch on. This position is great for breastfeeding newborns and small babies, as well as for babies who do not latch well. Since the baby lies completely on the other hand, it becomes easier to control his position and you can adjust the chest with your free hand. nine0005
This position is great for breastfeeding newborns and small babies, as well as for babies who do not latch well. Since the baby lies completely on the other hand, it becomes easier to control his position and you can adjust the chest with your free hand. nine0005
Julie, a mother of two from the UK, finds this position very practical: “I usually breastfeed my youngest in the cross cradle position. So I have a free second hand, and I can take care of an older baby at the same time. ”
Do not hold the baby by the head at first, otherwise you may inadvertently press his chin against his chest. Because of this, the child will not be able to take the breast deeply, because the nipple will rest against the base of the tongue, and not against the palate, which will lead to inflammation of the nipples. As the child grows, this position becomes more comfortable, and he can rest his head on your palm (as shown in the photo above). nine0005
4. Underarm breastfeeding
In this position, also known as the "ball grip", the mother is seated and the baby lies along her arm at the side, legs towards the back of a chair (or any other seat).![]() 3 This is another comfortable position for newborn breastfeeding, in which you can give your baby good support, have full control of his position and have a good view of his face. And the baby feels safe in close contact with the mother's body. This position is especially good for those who have had a caesarean section or a premature birth, as well as mothers of twins and women with large breasts. nine0005
3 This is another comfortable position for newborn breastfeeding, in which you can give your baby good support, have full control of his position and have a good view of his face. And the baby feels safe in close contact with the mother's body. This position is especially good for those who have had a caesarean section or a premature birth, as well as mothers of twins and women with large breasts. nine0005
“When I breastfed my first daughter, I had very large K-sized breasts—twice the size of her head,” recalls Amy, an Australian mother of two. - I put rolls of towels under each breast, because they were very heavy, and fed my daughter in a pose from under the arm, but only sitting straighter so as not to crush her. This position was also convenient because I had a caesarean section and could not put the baby on my stomach.”
5. Side-lying position
The side-lying position is ideal for relaxed
feedings at night in bed or on the couch. If you had a
caesarean section or ruptures during childbirth, this position may be more comfortable than sitting down. 3 In this position, mother and baby lie side by side, tummy to tummy.
3 In this position, mother and baby lie side by side, tummy to tummy.
“It was difficult for me to sit during endless night feedings, firstly because of the caesarean section, and secondly because of lack of sleep,” recalls Francesca, a mother from the UK. “And then I discovered that you can feed your baby lying on your side and rest at the same time.” nine0005
“Because of the short tongue frenulum, Maisie could only properly latch on to her breasts while lying on her side. The lactation consultant showed me how it's done. In this position, the flow of milk was optimal for my daughter, and it was easier for her to keep the nipple in her mouth. As she got older, she became much better at grabbing her breasts in normal positions,” says Sarah, mother of two from Australia.
6. Relaxed breastfeeding after caesarean section
If you can't find a comfortable position for breastfeeding after caesarean section, 3 try to hold the baby on the shoulder while reclining — this does not create stress on the postoperative suture and allows you to comfortably breastfeed the baby. You can also try side feeding.
You can also try side feeding.
7. Sitting upright breastfeeding or “koala pose”
When breastfeeding in an upright position or “koala pose”, the baby sits with a straight back and a raised head on the mother's hip. 4 This position can be tried even with a newborn if it is well supported, but it is especially convenient for feeding a grown child who can already sit up by himself. The upright sitting position, or “koala pose,” is great for toddlers who suffer from reflux or ear infections and feel better sitting. In addition, this pose may be suitable for children with a shortened frenulum of the tongue or reduced muscle tone. nine0005
“When my daughter got a little older, I would often feed her in an upright position — it was more comfortable for both of us and I could still hold her close,” recalls Peggy, a mother from Switzerland. “Besides, it was possible to discreetly breastfeed her in public places.”
8. Overhanging position
In this position, the baby lies on his back, and the mother bends over him
on all fours so that the nipple falls directly into his mouth. 4 According to some mothers, this breastfeeding position is good to use from time to time for mastitis, when touching the breast is especially unpleasant. Some say that this breastfeeding position helps with blockage of the milk ducts, although there is no scientific evidence for this yet. You can also feed in the “overhanging” position while sitting, kneeling over the baby on a bed or sofa, as well as reclining on your stomach with support on your elbows. Pillows of various sizes that you can lean on will help you avoid back and shoulder strain. nine0005
4 According to some mothers, this breastfeeding position is good to use from time to time for mastitis, when touching the breast is especially unpleasant. Some say that this breastfeeding position helps with blockage of the milk ducts, although there is no scientific evidence for this yet. You can also feed in the “overhanging” position while sitting, kneeling over the baby on a bed or sofa, as well as reclining on your stomach with support on your elbows. Pillows of various sizes that you can lean on will help you avoid back and shoulder strain. nine0005
“I have breastfed several times in the 'overhang' position for clogged milk ducts when no other means of resolving the clogs worked. And this pose seems to have helped. I think it's because of gravity, and also because the breasts were at a completely different angle than with normal feeding, and my daughter sucked her differently, ”says Ellie, a mother of two from the UK.
Feeding in the "overhanging" position is unlikely to be practiced regularly, but in some cases this position may be useful. nine0005
nine0005
“I used to breastfeed in the overhang position when my baby was having trouble latch-on,” says Lorna, mother of two in the UK. - This, of course, is not the most convenient way, but then I was ready for anything, if only he could capture the chest. We succeeded and have been breastfeeding for eight months now!”
9. Feeding a baby in a sling or “on the fly”
Breastfeeding in a sling takes some practice, but it can be used to go out of the house, look after older children or even do a little household chores. nine0005
The sling is also useful if the baby does not like to lie down or is often attached to the breast. Lindsey, a mother of two in the US, notes: “I used the carrier frequently for both of my children. When we were out, I tied the sarong around my neck and covered the carrier with it. Under such a cape, the baby can eat as much as he wants until he falls asleep.
This breastfeeding position is best when the baby is already good at breastfeeding and can hold its head up by itself.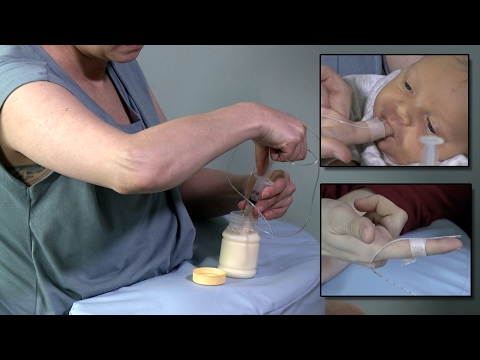 Any slings are suitable for breastfeeding, including elastic and rings, as well as carrying bags. Whatever option you choose, the main thing is that you can always see the face of the child, and his chin does not rest against his chest. nine0005
Any slings are suitable for breastfeeding, including elastic and rings, as well as carrying bags. Whatever option you choose, the main thing is that you can always see the face of the child, and his chin does not rest against his chest. nine0005
10. Double hand-held breastfeeding
Double hand-held breastfeeding (or “double-ball grab”) is great for mothers of twins—you can breastfeed both at the same time, while keeping your arms relatively free. 4 When feeding in this position, it is advisable to use a special pillow for breastfeeding twins, especially at first. It will provide extra support and help keep both babies in the correct position, as well as reduce the burden on the abdomen if you had a caesarean section. In addition, the hands are freer, and if necessary, you can deal with one child without interfering with the second. nine0005
“My twins were born very tiny and had to be fed every two hours at any time of the day or night. Very soon it became clear: if I want to do anything besides feeding, I need to feed them both at the same time, - says Emma, mother of two children from the UK. “I breastfed them two by hand using a breastfeeding pillow.”
“I breastfed them two by hand using a breastfeeding pillow.”
Other comfortable positions for breastfeeding twins are two criss-cross cradles, one baby in the cradle and the other close at hand, reclining feeding or sitting upright (one baby on one side, the other on the other). nine0005
11. Breastfeeding in the “arm-supported” or “dancer's-arm” position
muscle tone (which is typical for premature babies, children suffering from various diseases or Down syndrome), try supporting his head and your chest at the same time. 4 Grab your chest with your palm underneath so that your thumb is on one side and all the other fingers are on the other. Move your hand slightly forward so that your thumb and forefinger form a "U" just in front of your chest. With the other three fingers, continue to support the chest. With your thumb and forefinger, hold the baby's head while feeding so that his chin rests on the part of the palm between them, your thumb gently holds the baby on one cheek, and your index finger on the other. So the baby gets excellent support, and you can control his position and see if he is holding his breast. nine0005
So the baby gets excellent support, and you can control his position and see if he is holding his breast. nine0005
Literature
1 Colson SD et al. Optimal positions for the release of primitive neonatal reflexes stimulating breastfeeding. Early Hum Dev . 2008;84(7):441-449. - Colson S.D. et al., "Optimal Positions for Provoking Primitive Innate Reflexes to Induce Breastfeeding." Early Hume Dev. 2008;84(7):441-449.
2 UNICEF UK BFHI [ Internet ]. Off to the best start ; 2015 [ cited 2018 Feb ]. - UNICEF UK, Baby-Friendly Hospital Initiative, Start the Best You Can [Internet]. 2015 [cited February 2018].
3 Cadwell K. Latching - On and Suckling of the Healthy Term Neonate: Breastfeeding Assessment.