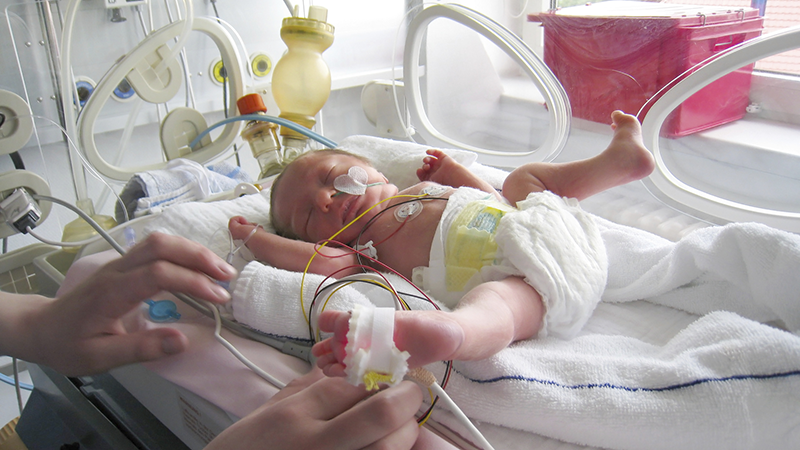
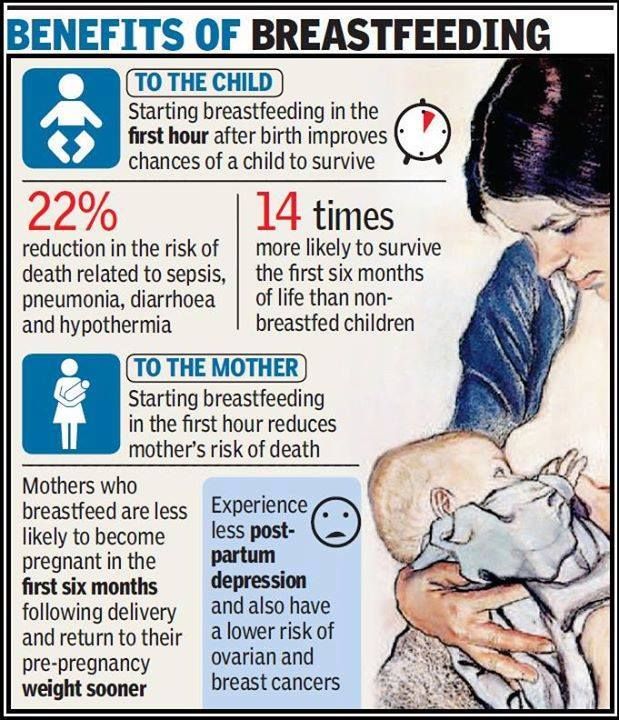
Feeding premature babies in nicu
Feeding your baby in the NICU
Breast milk is the best food for your baby. Breast milk has antibodies that help keep your baby from getting sick and nutrients that help her grow.
If you’re not breastfeeding, you can feed your baby formula or breast milk from a breast milk donor.
If your baby’s not ready to breastfeed, you can pump your breast milk.
If you have multiples, your babies may want to feed differently. Take time to find out what’s best for each baby.
Key If you need help with breastfeeding, talk to your nurse or lactation consultant.
What does your baby eat in the NICU?
Breast milk is the best food for your baby, even if she’s in the newborn intensive care unit (also called NICU). Breast milk has antibodies that help keep your baby from getting sick. It also contains nutrients that help your baby grow and develop. And breast milk changes as your baby grows so she gets exactly what she needs at the right time. This is true even if your baby was born prematurely. Premature birth is birth that happens before 37 weeks of pregnancy.
For the first few days after giving birth, your breasts make a thick, yellowish breast milk called colostrum. It has nutrients and antibodies that your baby needs. Even if you make only a few drops of colostrum, you can feed it to your baby. Your body starts to make breast milk about 3 to 4 days after giving birth.
If you’re not breastfeeding, your baby may get formula or breast milk from a donor (also called donor breast milk). Formula is a milk product you can feed your baby instead of breast milk. Donor breast milk is breast milk that’s been donated to a milk bank. A milk bank receives and stores donated breast milk, tests it to make sure it’s safe and sends it to families of babies who need it. Donor breast milk is prescribed by your baby’s provider. It has all the benefits of your own breast milk.
Sometimes babies get both breast milk and formula. Talk to your baby’s provider about the best food for your baby while he’s in the NICU.
Talk to your baby’s provider about the best food for your baby while he’s in the NICU.
How do you feed your baby in the NICU?
The way you feed your baby depends on her medical condition and how well she can suck and swallow. You can feed her:
- By breastfeeding. If your baby can’t breastfeed, you can feed her breast milk that you pump from your breasts.
- Breast milk or formula through a bottle
- Breast milk or formula through a feeding tube. A feeding tube is a tube that goes into your baby’s stomach to give her food when she can’t get it from regular feeding. Depending on your baby’s condition, she may need a gastronomy tube (also called a g-tube), a nasogastric tube (also called an NG tube) or an orogastric tube (also called an OG tube). A g-tube goes directly into your baby’s stomach. An NG tube goes through your baby’s nose, down the esophagus and into your baby’s stomach. An OG tube goes into your baby’s mouth, down the esophagus and into your baby’s stomach.
- Through an intravenous line (also called an IV). This is for babies who are very small or sick. Your baby’s health care provider places a small tube in a vein in your baby’s hand, foot, scalp or belly button. Your baby get fluids and important nutrients through the IV to help her grow.
Depending on your baby’s condition, you may use a few of these methods together to feed your baby. For example, your baby may get food from a feeding tube and an IV.
How can you give your baby breast milk if your baby can’t breastfeed yet?
If your baby isn’t ready to breastfeed, you can pump your breast milk. A breast pump helps remove milk from your breasts. Using a breast pump may feel awkward at first. But with practice, pumping gets easier and more comfortable. A nurse or lactation consultant in the NICU can show you how to use the pump. A lactation consultant is someone with special training to help all women breastfeed, even women who have special breastfeeding problems.
As soon as your baby can, let her practice sucking at your breast to get ready for breastfeeding. This is called non-nutritive sucking. Here’s how to do it: Pump your breasts until they’re empty. Then let your baby touch and taste your breast to help her get used to what breastfeeding is like.
What can you do if you’re not making enough breast milk?
Some moms may have trouble making breast milk. It can be hard for moms with health conditions before or during pregnancy or after their baby was born. If you’re worried that you’re not making enough breast milk, talk with a nurse or lactation consultant in the NICU. You also can get help from a breastfeeding support group. A support group is a group of people who have the same kind of concerns. They meet together to try to help each other. You can find a breastfeeding support group that meets together in person or online.
You may be able to build up your milk supply (the amount of milk you make when breastfeeding) by:
- Getting rest.
 Your body produces more milk when it’s rested.
Your body produces more milk when it’s rested. - Eating healthy foods and drinking a lot of fluid, like water, juice or milk. When you breastfeed, your body loses fluid. It’s important that you get that fluid back through what you drink.
- Using a breast pump after or between feedings. When you pump your breasts often, they make more breast milk.
- Pumping your breasts until they’re empty each time you pump
- Doing kangaroo care (also called skin-to-skin care). This is when you put your baby, dressed only in a diaper, on your bare chest.
How can you feed more than one baby?
If you have multiples (twins, triplets or more) in the NICU, learn how each baby feeds best. For example, you may find that one baby feeds better from the breast and one feeds better from the bottle. Or one baby may do better on breast milk and one does better on formula. Or you may decide to pump breast milk for all your babies and only use formula when needed.
Take your time to figure out what works best for you and your babies. And expect to adjust your plans as your babies grow. Once they’re healthy, you can breastfeed two babies at once. Ask for help holding one baby while you get settled with the other. With practice, you can manage both by yourself.
More information
- American Academy of Pediatrics
- La Leche League International
- International Lactation Consultant Association
- womenshealth.gov/breastfeeding
Last reviewed: April, 2019
See also: Breastfeeding is best, Feeding your baby formula, Keeping breast milk safe and healthy, Share your story, Using a breast pump
Feeding Your Baby in the NICU
Most babies that require specialized care in the Newborn Intensive Care Unit (NICU) were born prematurely, typically in the 22 to 32-week out of 40-week gestation age range.
A baby born early often requires extra support and can face unique health challenges, one of which includes feeding.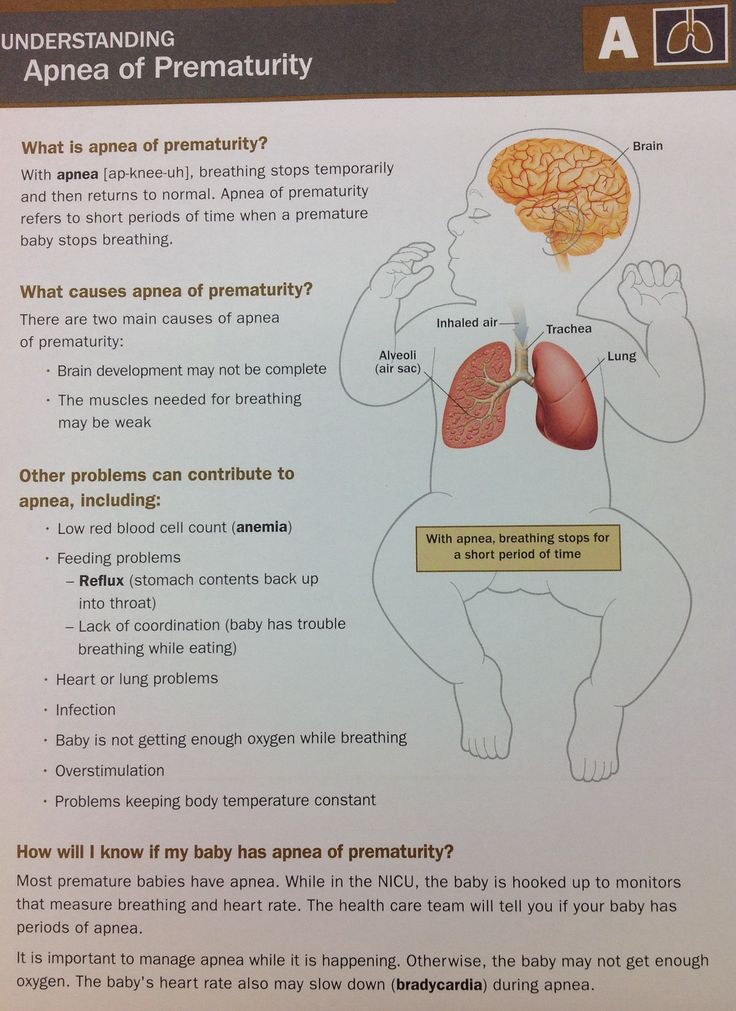 A premature baby may experience feeding challenges, because they:
A premature baby may experience feeding challenges, because they:
- Have an immature gastrointestinal tract.
- Are not medically stable enough to take regular feedings.
- Require help breathing, or are breathing fast, and are not safe to feed by mouth due to the risk of breathing food into the lungs.
- Don’t have the stamina to take all the nutrition they need by mouth.
“A team of neonatologists, expert nursing staff and health professionals in the NICU at Brigham and Women’s Hospital provide the most advanced care possible to newborns with critical health challenges, including the need for advanced feeding support,” says Terrie Inder, MBCHB, chair of the Department of Pediatric Newborn Medicine at the Brigham.
Medical care before breastfeeding
Many babies in the NICU are initially too small or sick to take a full milk feeding. Thus, medicines and fluids are often given through their veins or arteries. There are several ways a baby may receive fluids and medicines in the NICU, including:
- Intravenous line (IV): Babies may have an IV placed in a hand, foot or the scalp, where veins are easily accessed.
 Tubing connects the IV to a bag that contains nutritional fluids, which are delivered with a pump.
Tubing connects the IV to a bag that contains nutritional fluids, which are delivered with a pump. - Umbilical catheter (UVC or UAC): After the umbilical cord has been cut at birth, the short stump of the cord remains. Because the stump is still connected to the baby’s blood supply and circulatory system, a catheter can be inserted into one of the two arteries or the vein of the umbilical cord. Medicines, nutritional fluids and blood can be delivered through this catheter.
- Peripherally inserted central catheter (PICC) line: A catheter is placed in a deep vein or artery in the baby’s arm or leg and is used to meet a baby’s longer-term nutritional needs through an intravenous line.
“A premature baby may need IV lines or catheters for a short time or several days or weeks, in some cases. Once a baby is well enough to take milk feedings, and is gaining weight, IV lines are usually removed. Sometimes, an IV may be needed to give a baby antibiotics or other medicines even when the baby can be fed normally,” says Dr. Inder.
Inder.
Your baby’s nutrition
Every baby needs enough calories, protein and fats for adequate growth and development. Fluids, electrolytes and vitamins are also needed for growth, development and proper functioning of the body’s systems.
In the NICU at the Brigham, which is the largest and most state-of-the-art of its kind in Massachusetts, registered dietitians make rounds with medical teams daily to design and oversee nutrition plans for each baby. These plans may include IV nutrition, breast milk and/or formula.
A dietitian measures and evaluates a baby’s growth regularly, including weight, length and head circumference (a measure of brain growth). These measurements are then plotted on a growth chart specific to each baby’s sex and gestational age. The baby’s growth provides valuable information for the dietitian to recommend changes to a feeding plan.
Babies who cannot consume milk require a special preparation called parenteral nutrition (intravenous nutrition).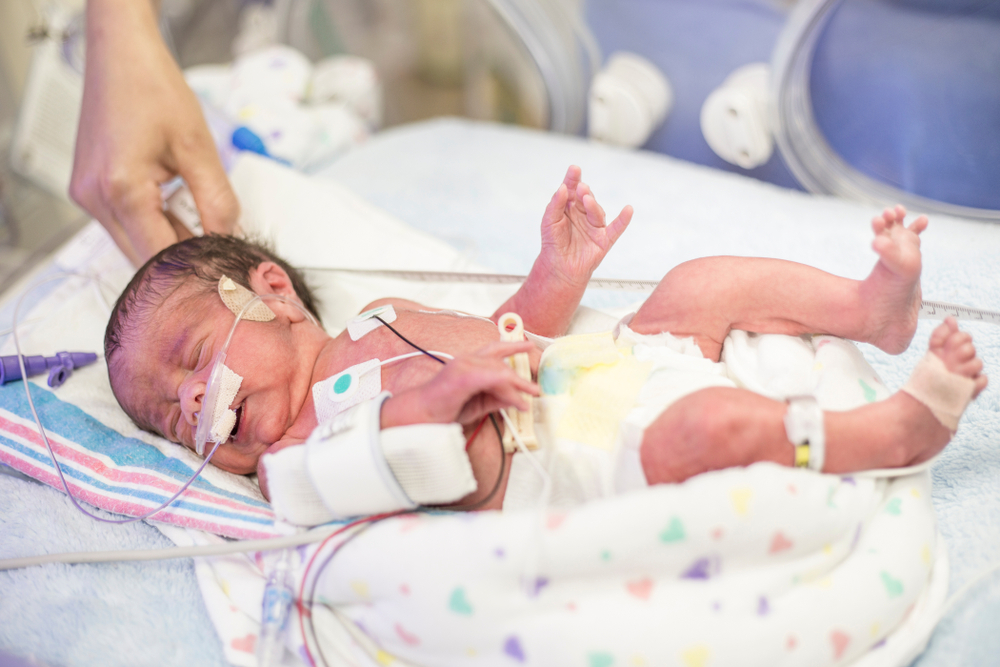 Parenteral nutrition bypasses the normal digestion in the stomach and bowel. It’s a special liquid nutrition mixture delivered into the blood through an intravenous catheter. The mixture contains the nutrients a baby needs until they can take milk feedings. The contents of parenteral nutrition are calculated for each baby. Calories, protein, fats and electrolytes, including sodium, potassium, chloride, magnesium, phosphorus and calcium, are all important components.
Parenteral nutrition bypasses the normal digestion in the stomach and bowel. It’s a special liquid nutrition mixture delivered into the blood through an intravenous catheter. The mixture contains the nutrients a baby needs until they can take milk feedings. The contents of parenteral nutrition are calculated for each baby. Calories, protein, fats and electrolytes, including sodium, potassium, chloride, magnesium, phosphorus and calcium, are all important components.
The NICU team supports parents and families as they navigate the challenges of having a premature baby in the hospital. There are many support services available to patients and their families, including built in support systems to identify and intervene in the event of any cognitive or emotional difficulties.
“We include parents in all clinical care decisions, including feeding decisions. We want to support families as they face the challenges that can happen when they have a sick baby in the hospital,” says Dr. Inder.
Inder.
How your baby is fed in the NICU
Gavage or tube feedings
Because premature babies often can’t be fed from the breast or bottle right away, gavage or tube feedings may be needed until the baby learns to feed for themselves. For gavage feedings, a small flexible tube is placed into a baby’s nostril or mouth and passed into the stomach. The tube usually remains in place until the baby is consistently able to feed by mouth. At first, tiny amounts of breastmilk or formula are given through the feeding tube. Because of their small stomach size, smaller babies may be fed using a pump that slowly delivers the milk in small amounts. As a baby grows, they can slowly take larger amounts at each feeding.
Breast and bottle feedings
Feeding practice from breast or bottle can begin as soon as babies are stable, breathing comfortably and can coordinate sucking, swallowing and breathing. Babies begin to practice feeding by mouth while still being tube fed. Even if the baby shows interest and participates in a feeding, it can be tiring for them.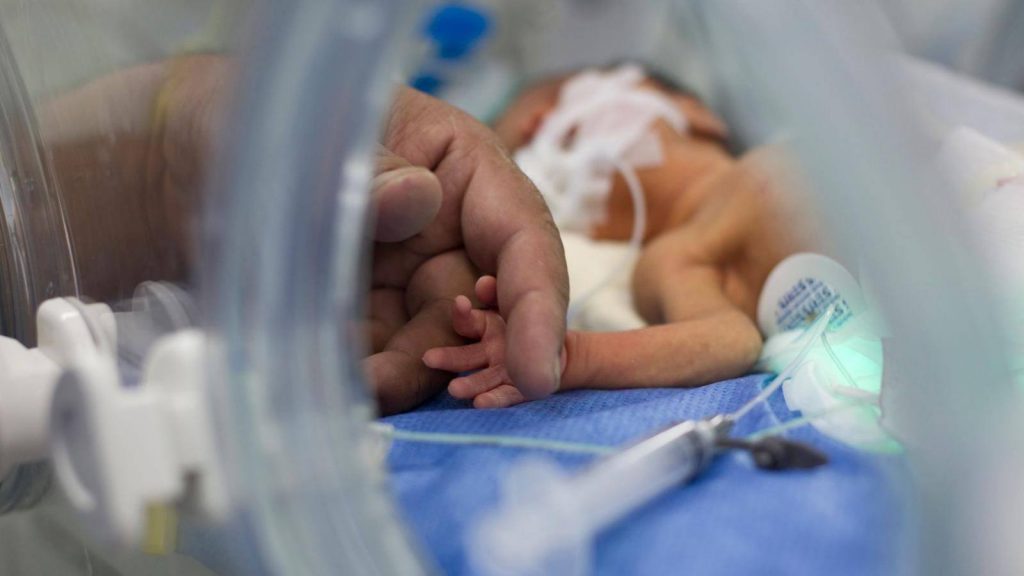
“It’s important to pay attention to behavioral cues that show tiredness. If you are using a bottle, it can be helpful to help your baby pace feedings. Learning to feed by mouth is a gradual process that can take weeks for premature babies. It’s normal to take only occasional small amounts by bottle or at the breast” says Dr. Inder.
The benefits of breastmilk for your baby
A mother’s milk is the preferred milk for all babies, especially the most premature babies. Breastmilk contains nutrients needed for growth and development. It also contains antibodies from the mother to help protect babies from infection. This protection is important when babies are sick or premature and have higher chances of developing an infection.
Additional benefits of mother’s milk for a premature baby include:
- Reduced risk of necrotizing enterocolitis, a rare but severe intestinal disease that affects preterm infants almost exclusively.
- Improved digestion and gastrointestinal function.
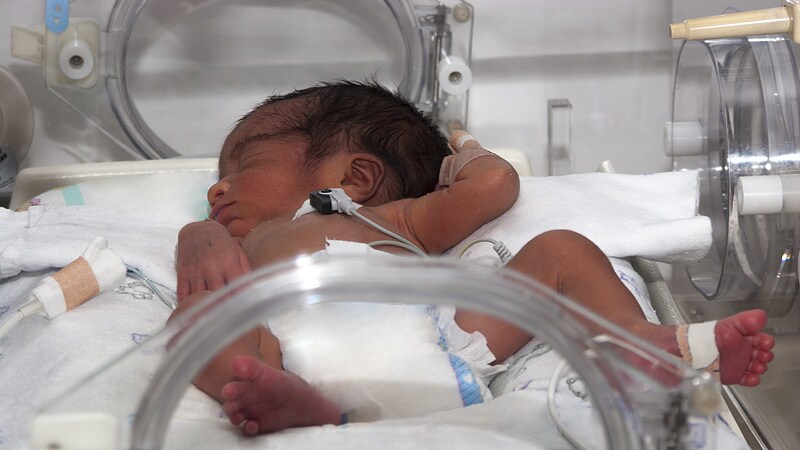
- Improved brain and eye development.
- Improved wellness of the mother and bonding with baby.
“Providing breastmilk for your baby lets you participate in your baby’s healthcare in a crucial way. Because the benefits of mother’s milk are so important to the high-risk newborn, you can do something for your baby that no one else can,” says Dr. Inder.
Babies younger than 28 weeks’ gestation can especially benefit from milk feedings. Very early preterm infants are given trophic feedings in small amounts that help the digestive tract mature and grow. The amount of milk is slowly increased over days to weeks. Once your baby can ingest larger amounts of milk feedings, intravenous fluids and/or parenteral nutrition can be slowly decreased.
Very premature babies need fortifiers added to breastmilk and supplements to meet their increased needs for protein, calcium and phosphorus. Even if your baby can’t breastfeed, you can pump your breastmilk and it can be stored for gavage or nipple feedings.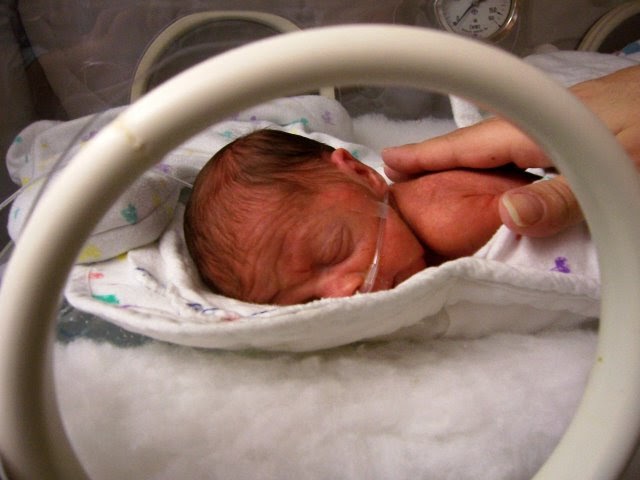 Depending on the amount of milk needed for feedings, donor milk or formula may need to be given temporarily in addition to a baby’s own mother’s milk.
Depending on the amount of milk needed for feedings, donor milk or formula may need to be given temporarily in addition to a baby’s own mother’s milk.
“If a mother has difficulty with milk production, she can supplement with donor milk. Our donor milk comes from Mother’s Milk Bank Northeast in Newton, MA. All milk donors undergo an extensive screening process. The donated milk is pasteurized and monitored to ensure its safety,” says Dr. Inder.
Lactation Services in the Newborn Intensive Care Unit
Certified lactation consultants are nurses or other healthcare providers who are specially trained and certified to help women with breastfeeding. In the NICU, lactation consultants help you and your baby become comfortable nursing.
They can also teach you about pumping and storing breastmilk. Because learning to feed by mouth is a process that can take you and your baby a few weeks, you will likely need to continue expressing milk even after leaving the NICU.
The lactation team at the Brigham are international board-certified professionals, as well as nurses that work closely with families from the time they enter the NICU to through discharge.
Feeding therapy services in the NICU
Feeding therapists are also available throughout the NICU. They work alongside nursing staff to assist babies who are having difficulty learning to feed by mouth. Many premature babies benefit from specialty feeding equipment and strategies to help them feed safely and feeding therapists can assist parents in identifying when these would be helpful.
“Our goal is for babies to feed safely and efficiently. We want babies and their parents to have enjoyable feeding interactions,” says Pamela Dodrill, PhD, CCC-SLP, a senior feeding therapist in the NICU.
The Brigham NICU uses an evidence-based algorithm to guide the transition from tube feeds to oral feeds, which allows parents to see where their baby is in their transition to independent oral feeding and readiness for discharge home. Feeding therapists also attend daily rounds prior to discharge and work closely with parents as they begin to transition home.
“Feeding therapists work together with other members of the NICU team to support parents to learn strategies to help their baby as their baby is learning to eat,” says Dr. Inder.
Inder.
Neonatal Resuscitation and Intensive Care Unit
Home / Maternity Hospital / Our departments/
Neonatal Intensive Care Unit is a structural subdivision of maternity hospital No. 10, consists of an intensive care unit and an intensive care unit and is designed for 20 beds.
The main mission and goal of the intensive care unit specialists is to save the life of the baby with the least negative consequences for his health.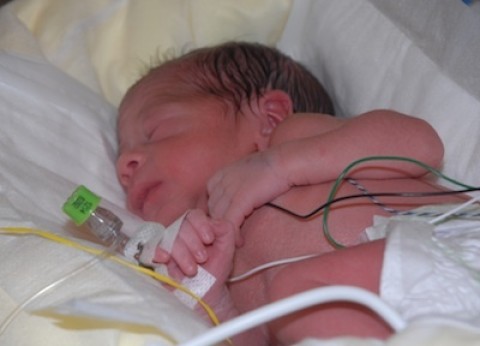 Children with various perinatal pathologies are admitted to the resuscitation and intensive care unit. Usually they require mechanical ventilation, parenteral nutrition, infusion therapy, correction and restoration of important body functions. Very premature babies with low body weight, who often have severe health disorders, are also transferred here. Parents are regularly provided with full information about the state of health of the newborn, about the characteristics of the disease and the tactics of its treatment.
Children with various perinatal pathologies are admitted to the resuscitation and intensive care unit. Usually they require mechanical ventilation, parenteral nutrition, infusion therapy, correction and restoration of important body functions. Very premature babies with low body weight, who often have severe health disorders, are also transferred here. Parents are regularly provided with full information about the state of health of the newborn, about the characteristics of the disease and the tactics of its treatment.
If your baby has been transferred to the intensive care unit, do not panic and despair. The department staff will teach you how to care for your baby, introduce you to new medical technologies, medical language, rules and procedures that are designed to help your child. Our specialists make every effort to ensure that parents get used to it as soon as possible and begin to understand the needs of their baby. This is very important, because the correct care of the child in these difficult first days depends on how quickly he will be able to adapt to new living conditions outside the mother's body. Only after the baby's health improves and does not cause concern, when he is ready for a full life under normal conditions, can we talk about discharge from the department.
Only after the baby's health improves and does not cause concern, when he is ready for a full life under normal conditions, can we talk about discharge from the department.
Resuscitation unit
This includes babies who need extra attention and resuscitation.
Children who have serious neurological problems, who cannot breathe on their own or who were born with very low birth weight are treated here. The resuscitation unit has everything for intensive treatment of the child and constant monitoring of his condition: incubators, monitor monitoring and, of course, qualified personnel.
Intensive care unit.
Rehabilitation treatment takes place here. Children are transferred here from the intensive care unit when adequate spontaneous breathing is restored, there is no need for continuous monitoring of vital functions, premature babies or babies with newborn jaundice.
The resuscitation and intensive care unit is equipped with modern medical equipment, which allows creating comfortable conditions for babies: modern incubators protect from noise and bright light, conditions are created for severely premature babies that are as close as possible to intrauterine conditions. For children who cannot feed on their own, nutrient solutions are introduced through a special probe. Also, if necessary, drugs are used to regulate the heart rate, stimulate breathing, blood pressure, ultrasound. In the premises of the department, the level of humidity and air temperature is constantly monitored.
For children who cannot feed on their own, nutrient solutions are introduced through a special probe. Also, if necessary, drugs are used to regulate the heart rate, stimulate breathing, blood pressure, ultrasound. In the premises of the department, the level of humidity and air temperature is constantly monitored.
Resuscitation and intensive care unit equipment:
- Incubators to maintain optimal temperature and humidity for the child;
- Open resuscitation systems for infusion, oxygen therapy with a heating system;
- Non-invasive ventilation apparatus for spontaneously breathing patients;
- ventilators for artificial lung ventilation;
- Monitors for round-the-clock monitoring of vital body functions (pulse rate, respiration, blood oxygen saturation, hemoglobin, pressure).
- Infusomats - devices for the dosed administration of medicines intravenously;
- Airway sanitation apparatus;
- Phototherapy lamps.

All devices used are certified and connected to a stand-alone station, which guarantees their trouble-free operation.
The medical staff of the intensive care unit is one of the most highly qualified. The team includes a medical unit, middle and junior medical personnel. The department is headed by the head, who is the chief of the doctors, and the senior nurse manages the sisters and junior staff.
The junior staff consists of assistant nurses and nurses who keep the department clean. Their work is very responsible, since the sanitary and hygienic requirements for treatment units are close to those established in operating rooms.
Nurses spend the most time with babies. They are around the clock with little patients, care for them, perform medical appointments, monitor the slightest changes in the condition of children, monitor readings, report on the dynamics of the condition of patients during medical rounds. Each sister is responsible for a certain number of newborns, and if the baby's condition is very serious, then there is only one patient per sister (and at the same time she is constantly busy, since the instability of the condition dictates a constant change in treatment).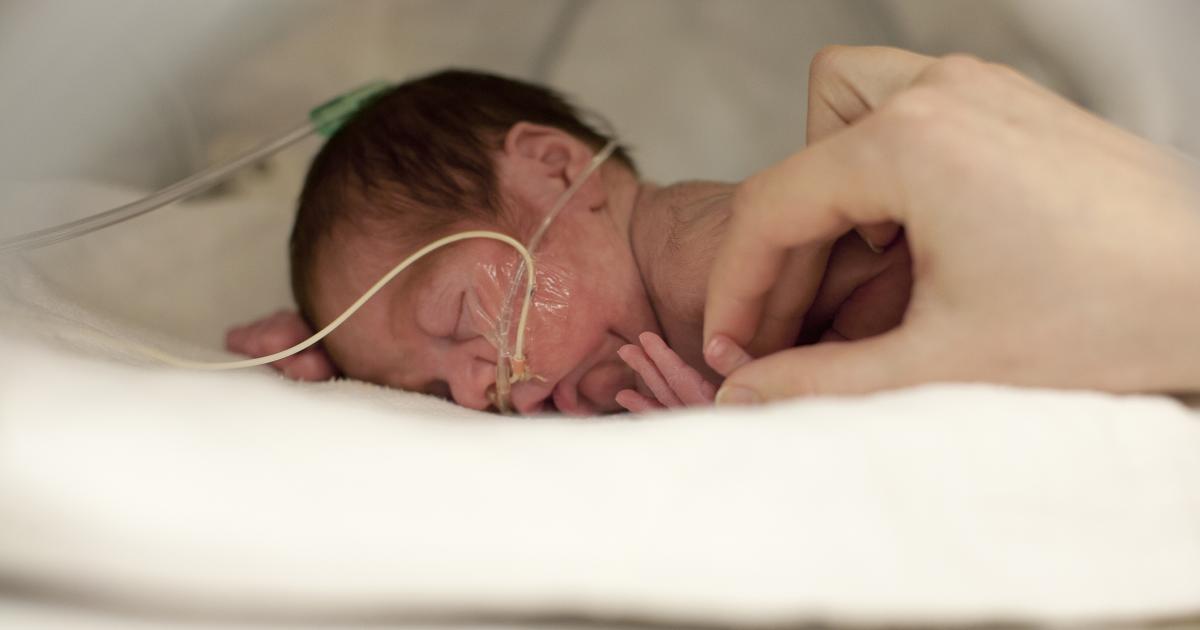
Since the department's nurses work in shifts, the parents of severely premature babies have time to get to know many of them. Without a doubt, the nurse is the central figure in the nursing of premature babies, his "mother" for the period of his stay in the department. Good sisters "feel" babies and have not only a kind heart, skillful hands, intuition, but are also extremely observant. They will always point out to the doctor about problems in the condition of the newborn, everyone feels good and calm with them - both patients and doctors.
There are also nurses who provide fluid therapy and therapeutic nutrition for newborns. They monitor the condition of intravascular catheters and infusion systems, the condition of medical equipment, and are responsible for the sterilization of instruments.
The main doctors of the department are anesthesiologists-resuscitators and neonatologists, there are fewer of them than nurses. Their task is to make a diagnosis, develop an intensive care program, monitor and adjust treatment.
Every day the doctor conducts a general examination, listens to the child's heartbeat and breathing pattern. The condition of patients is monitored by equipment and nurses, as well as during medical rounds, which are carried out day and night every 3 hours.
At each round, the doctor evaluates the child's condition: breathing stability, heart function, nutritional adequacy. The doctor of the department determines what tests are needed and with what frequency, what treatment is required. The doctor assesses the need and amount of medical support for cardiac activity, the advisability of prescribing antibiotics to protect against infections, develops a therapeutic nutrition program, and finally decides when the child can be disconnected from the ventilator and when he can be transferred from the intensive care unit to the intensive care unit.
In addition, on-call doctors assist premature babies in the delivery room, transfer them to the department, carry out primary stabilization and treatment until the end of their shift, as well as monitor and treat patients in the evening, at night and on weekends.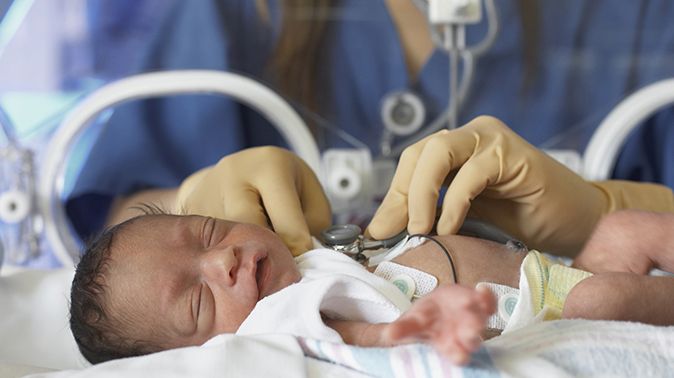 The duties of the doctors on duty also include registering the child in the intensive care and advisory bureau in order to transport the patient, if necessary, to other hospitals ( According to order No. examinations, children are transferred to specialized departments for newborns of city hospitals in a regulated time frame).
The duties of the doctors on duty also include registering the child in the intensive care and advisory bureau in order to transport the patient, if necessary, to other hospitals ( According to order No. examinations, children are transferred to specialized departments for newborns of city hospitals in a regulated time frame).
All doctors of the department have undergone the necessary training and improvement to provide resuscitation care to newborn children at the bases of the leading medical centers in Moscow and St. Petersburg.
Interaction of parents with department staff
According to the Health Law, the legal representatives of a newborn child are his parents (Article 18), to whom the attending physician provides information about the patient's condition (Article 17). The most complete information is provided in a personal conversation at a specially allotted time (over the phone it is impossible to make sure that the patient's mother or father is really on the other end).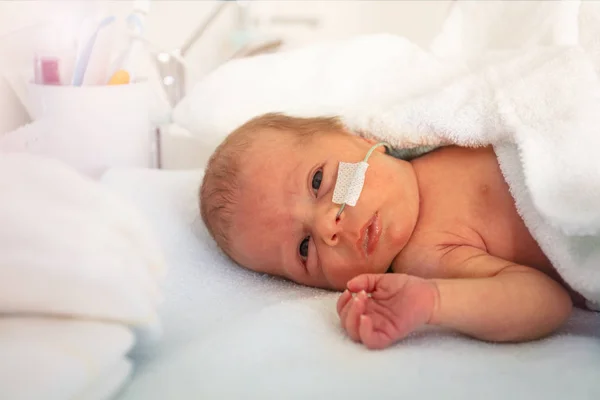 The attending doctor has the most complete picture of the diagnosis, changes in the condition, data of laboratory and instrumental studies of his patients, so it makes sense to ask him all the detailed questions. You can also inquire about the condition of the baby by phone.
The attending doctor has the most complete picture of the diagnosis, changes in the condition, data of laboratory and instrumental studies of his patients, so it makes sense to ask him all the detailed questions. You can also inquire about the condition of the baby by phone.
It is important for us that parents receive the most complete and accurate information, do not hesitate to ask even those questions that seem stupid, uncomfortable or inappropriate. We recommend that you write down questions as they arise, so that you can ask them later without forgetting anything.
What to ask your doctor:
- What is my child's condition?
- What is the severity of the condition?
- How is the baby treated (what does the intensive care program consist of)?
- What examinations are planned?
- What is the probability of normal development and possible complications?
- How do I get information about a change in condition and when can I visit my baby?
- Is it possible to perform the sacrament (rite) of baptism?
- How can I help my child get well?
Often, intensive care physicians have to tell relatives things that no one would like to hear, but objectively informing parents about the health of their children is part of our daily work. During meetings with doctors, parents have the opportunity to see and communicate with their children.
During meetings with doctors, parents have the opportunity to see and communicate with their children.
Maternity hospital No. 10 participates in the state program to support breastfeeding, and our specialists do their best to help maintain it. Regardless of the severity of the child's condition, we welcome the communication of parents with the newborn, we consider it necessary for the baby and contribute to his speedy recovery. Visits are limited only during SARS and influenza epidemics in order to protect seriously ill newborns from infection, which can worsen their condition.
Feeding premature babies | Breastfeeding premature babies
Premature babies have a special need for breast milk, but it can be difficult to breastfeed them directly. Our expert advice will help you provide your premature baby with healthy breast milk.
Share this information
Professor Katsumi Mizuno, Department of Paediatrics, Showa University Koto Toyosu Hospital:
Katsumi is a Certified Breastfeeding Consultant, Professor of Pediatrics at Showa Medical University, and one of Japan's leading pediatric neonatologists. His research focuses on neonatal suckling skills, breast milk banking, and the use of breast milk for feeding premature babies in neonatal intensive care units.
His research focuses on neonatal suckling skills, breast milk banking, and the use of breast milk for feeding premature babies in neonatal intensive care units.
Babies born before the 37th week of pregnancy are considered premature. 1 The causes of preterm labor are not always obvious, but certain factors increase the likelihood of such an event. These include: twin or multiple pregnancy, certain diseases of the mother or fetus, as well as a history of premature birth.
Because premature babies spend less time in the womb, they are not mature enough and may be more susceptible to infection and disease. They often require hospitalization in the neonatal intensive care unit.
Why is breast milk important for premature babies?
Breast milk is essential for optimal growth and development of term babies, but it is even more important for premature babies.
During pregnancy, the fetus receives important substances from the mother through the placenta, such as DHA (a fatty acid essential for brain and eye development) and immunoglobulin G (an antibody).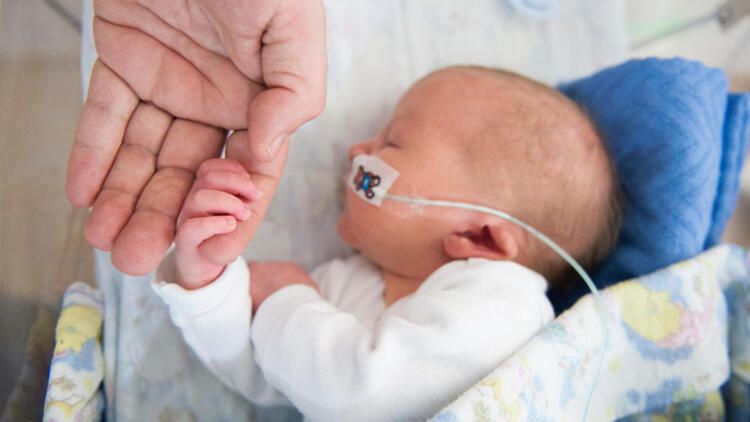 2.3 A premature infant did not receive all of these substances. However, the milk produced by a premature mother contains more fat and secretory immunoglobulin than mothers of full-term babies. 4
2.3 A premature infant did not receive all of these substances. However, the milk produced by a premature mother contains more fat and secretory immunoglobulin than mothers of full-term babies. 4
In addition, premature babies have an underdeveloped gastrointestinal tract, which can make digestion and absorption of nutrients difficult, so they need food that their sensitive stomach and intestines can easily digest. Breast milk contains enzymes that facilitate the digestion of the baby, 5 as well as epidermal growth factor, which accelerates the development of the gastrointestinal tract 6 . Premature infants who are predominantly breastfed have much lower intestinal permeability than formula-fed infants, meaning fewer potentially harmful particles from the stomach and intestines enter their bloodstream. 7
Breast milk is so important for premature babies that if the baby's mother does not produce enough breast milk at first for any reason, it is recommended to make up for the shortage with donor milk rather than formula.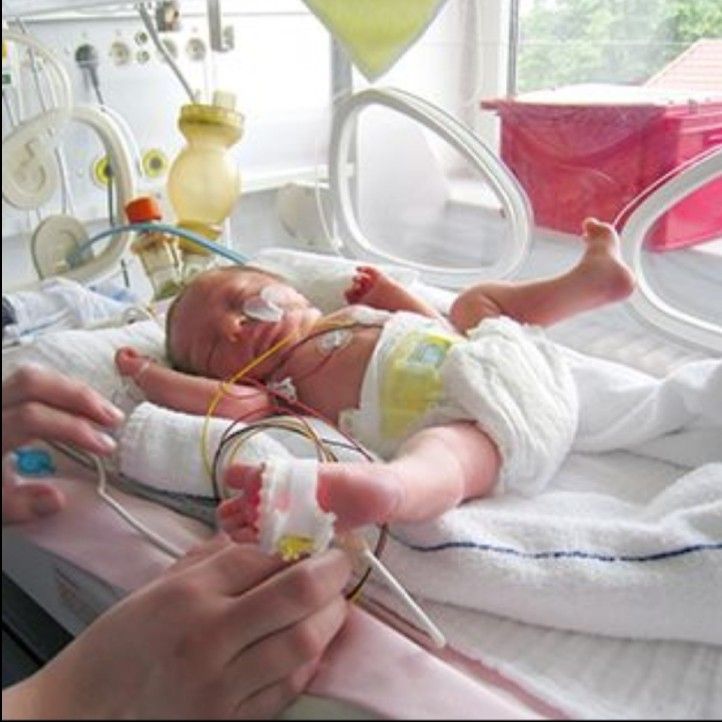
Does breast milk improve the condition of premature babies?
Breast milk contains protective substances that can prevent serious illnesses that preterm infants are susceptible to, 8 e.g. severe infections, 9 retinopathy of prematurity (which can cause vision loss) 10 and bronchopulmonary dysplasia (chronic lung disease). 11
The more milk your baby gets, the lower the risk of disease. 12 Every additional 10 ml of milk per kilogram of body weight per day reduces the risk of developing sepsis by 19%. 9 The risk of developing necrotizing enterocolitis (a potentially fatal bowel disease) in premature infants who are breastfed is ten times lower than those who are formula fed. 13 That's why every drop counts!
Most importantly, premature infants who are breastfed are typically discharged an average of two weeks earlier than formula-fed infants. 14 They also have a 6% lower risk of readmission in the first year of life. 15
15
Breast milk has been proven to have a beneficial effect on mental and physical development in the long term. Studies show that low-birth-weight babies who are breastfed in the neonatal intensive care unit have an average IQ of up to five points higher than those who are not breastfed. 15 In addition, their cardiovascular system works better during their lifetime. 17
Will milk be produced if the baby is born prematurely?
Yes, the mother's body is ready to produce milk by the middle of pregnancy. After the baby is born and the placenta is born, the level of progesterone, the pregnancy hormone, drops, and the production of colostrum, the first milk, starts in the breast. This usually happens after the newborn is put to the breast and begins to suckle rhythmically, but if the baby was born prematurely, he most likely will not be able to latch on at first.
To replicate the sensations that trigger milk production, you can manually stimulate the breasts and nipples, or use a breast pump to express nutrient-rich colostrum for your baby. 18 Read below for more information on what to do if your premature baby is not yet able to breastfeed.
18 Read below for more information on what to do if your premature baby is not yet able to breastfeed.
Breast milk usually comes in two to four days after birth, but if it was premature, the milk supply may be delayed. However, a recent study shows that moms who started pumping within one hour of giving birth had milk coming in as expected. 19 This is why it is important to start expressing breast milk as early as possible.
How to prepare if the baby is expected prematurely?
Visit the neonatal intensive care unit to see how it works and how premature babies are cared for. In addition, it will be useful to learn how breast milk is produced and secreted and why it is not only a healthy food, but also an important medicine for premature babies. Read more about this in our free e-book Surprising Breast Milk Facts .
What if a premature baby cannot breastfeed?
Many babies born before 34 weeks have difficulty coordinating sucking, swallowing and breathing. Until the baby masters these skills, nurses will feed him through a tube that is inserted into the nose or mouth and provides food directly into the stomach. In this way, the baby can be fed continuously until he is ready to breastfeed.
Until the baby masters these skills, nurses will feed him through a tube that is inserted into the nose or mouth and provides food directly into the stomach. In this way, the baby can be fed continuously until he is ready to breastfeed.
If your baby is too weak to latch on and suckle milk, you can use a breast pump* available at the hospital or maternity hospital to “do the job for the baby”. Breast stimulation with research-based technology, 20 reproducing the rhythm of the suckling of the baby, plays an important role in starting and maintaining milk production in the first hours after birth 21 .
Milk should be expressed at the same frequency as term infants are usually fed every two to three hours, i.e. 8 to 12 times a day.
You can try putting a small amount of expressed breast milk into the baby's mouth with a syringe, or putting milk-soaked cotton swabs in the baby's mouth. 22 This way your baby will recognize the taste of your milk, which will facilitate the transition to breastfeeding in the future. In addition, the protective substances that make up breast milk will help strengthen the local immunity of the baby's oral cavity. You can be involved in the care of your premature baby in a variety of ways - check with your healthcare provider for details.
In addition, the protective substances that make up breast milk will help strengthen the local immunity of the baby's oral cavity. You can be involved in the care of your premature baby in a variety of ways - check with your healthcare provider for details.
Very low birth weight babies - less than 1.5 kg - usually need extra protein, calcium and phosphorus, so they are given fortified breast milk. In some countries, such additives are made on human milk, and, for example, in Japan, on cow's milk.
Recommendations for pumping milk
If the baby will be in the neonatal intensive care unit for a long time, neonatologists recommend using a double breast pump for pumping. I always recommend Medela Symphony*. Double pumping not only speeds up the process, but also produces an average of 18% more milk than pumping from each breast in turn. 23
In addition, I advise you to create the most comfortable conditions for pumping. It is generally agreed that it is best to express milk during or after prolonged skin-to-skin contact with the baby (more on this "kangaroo method" below).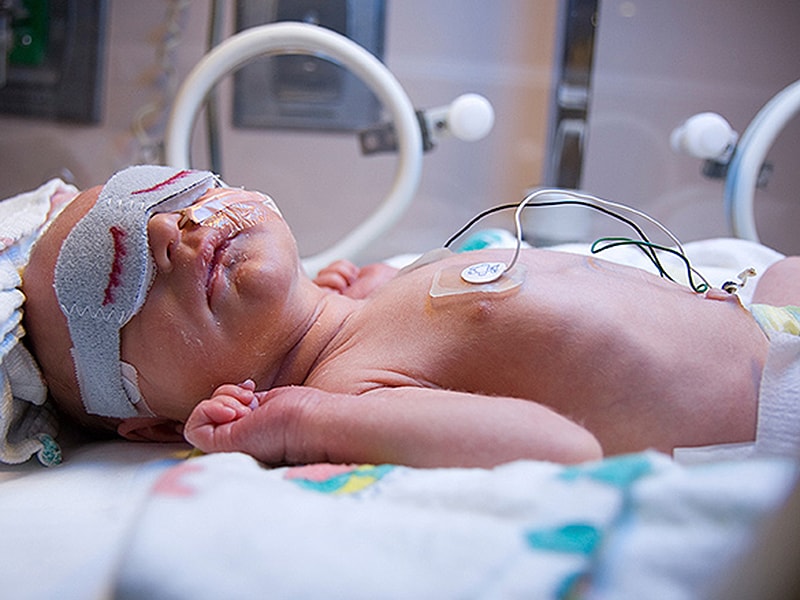 Another good option is to sit next to the crib and watch your baby while he pumps. Oxytocin (the hormone that stimulates milk flow) is released when you look at your baby, touch him, smell him and think about him, 24 Therefore, comfortable and calm conditions must be created for this in the neonatal intensive care unit.
Another good option is to sit next to the crib and watch your baby while he pumps. Oxytocin (the hormone that stimulates milk flow) is released when you look at your baby, touch him, smell him and think about him, 24 Therefore, comfortable and calm conditions must be created for this in the neonatal intensive care unit.
What is kangaroo care for premature babies?
The so-called kangaroo method involves prolonged skin-to-skin contact between parents and infant. This is extremely beneficial for you and your baby, as well as for milk production. Skin-to-skin contact normalizes the baby's breathing and heartbeat, keeps him warm and allows him to be as close to the parent as possible. Kangaroo care is believed to have a beneficial effect on the health of premature babies, 25 and it helps mothers express more milk 26 and breastfeed longer. 27 Skin-to-skin contact 30-60 minutes before feeding gives baby time to wake up and be hungry so he can eat without being forced.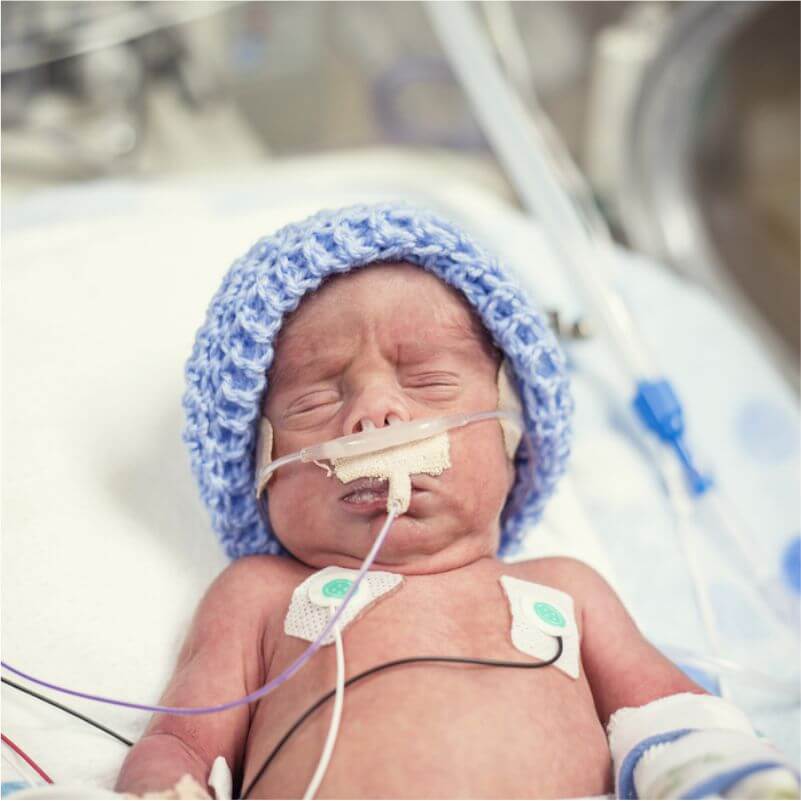
What if the neonatal intensive care unit offers formula feeding?
Feel free to state that you want to breastfeed your baby instead of formula. If you don't have enough breast milk to feed your baby, ask the ward for help to increase your milk supply.
It is natural for mothers whose babies are in the neonatal intensive care unit to experience anxiety and stress. Sometimes these experiences interfere with milk production, so it's important to ask for any help you may need. Remember that you have the right to seek support. Your healthcare provider may be able to recommend a suitable lactation specialist, such as a lactation consultant, for you.
How to switch from pumping to breastfeeding?
At whatever gestational age a baby is born, as long as the baby is stable enough for skin-to-skin contact, it can seek the breast for sedative suckling. This is the perfect way for your baby to learn sucking skills before they learn to coordinate sucking, swallowing and breathing.
Babies love the smell of breastmilk, so you can put some milk on the nipple before putting your baby to the breast to make him want to suckle. He might even be able to suck some milk. Don't worry if your baby seems to suck very little - he learns every time. He can start with one or two sips and gradually move on to full breastfeeding. Until then, the baby can be fed through a tube, pressed to the breast, so that the taste of milk and touching the breast is associated with a feeling of satiety.
You can put your baby to the breast for sedative suckling as soon as you are ready for kangaroo care, unless your baby is suffering from bradycardia (slow heartbeat) or low oxygen levels in the blood. You can switch to breastfeeding as soon as the baby is ready for it. Gradually, he will gain enough strength to suckle longer and suck out more milk.
Literature
1 World Health Organization. Geneva, Switzerland; 2018. Media Centre: Preterm birth fact sheet; November 2017 [03/26/2018]. Available from : http://www.who.int/mediacentre/factsheets/fs363/en/ - World Health Organization. Geneva, Switzerland; 2018. "Media Center: Prematurity Fact Sheet"; November 2017 [3/26/2018]. Article at: http://www.who.int/mediacentre/factsheets/fs363/en/
Available from : http://www.who.int/mediacentre/factsheets/fs363/en/ - World Health Organization. Geneva, Switzerland; 2018. "Media Center: Prematurity Fact Sheet"; November 2017 [3/26/2018]. Article at: http://www.who.int/mediacentre/factsheets/fs363/en/
2 Duttaroy AK. Transport of fatty acids across the human placenta: a review. Prog Lipid Res . 2009;48(1):52-61. - Duttaroy A.K., "Transfer of fatty acids across the human placenta: a review". Prog Lipid Res. 2009;48(1):52-61.
3 Palmeira P et al. IgG placental transfer in healthy and pathological pregnancies. Clin Dev Immunol. 2012;2012: 985646. - Palmeira P. et al., Placental transfer of immunoglobulin g through the placenta with healthy and pathological pregnancy. ” Klin Virgo Immunol. 2012: 985646.
2012: 985646.
4 Underwood Ma. Human Milk for the Prematy North Am . 2013;60(1):189-207. - Underwood, M.A., "Breast milk for the premature baby." 1):189-207.
5 Pamblanco M et al. Bile salt - stimulated lipase activity in human colostrum from mothers of infants of different gestational age and birthweight. Acta Paediatr. 1987;76(2):328-331. - Pamblanco M. et al., "Bile salt-activated lipase and its activity in colostrum of mothers of infants of various gestational ages and birth weights." Akta Pediatr. 1987;76(2):328-331.
6 Dvorak B. Milk epidermal growth factor and gut protection. J Pediatr. 2010;156(2): S 31-35. - Dvorak B., "Epidermal growth factor in milk and gut protection". Zh Pediatr (Journal of Pediatrics). 2010;156(2):S31-35.
- Dvorak B., "Epidermal growth factor in milk and gut protection". Zh Pediatr (Journal of Pediatrics). 2010;156(2):S31-35.
7 Taylor SN et al. Intestinal permeability in preterm infants by feeding type: mother's milk versus formula. Breastfeed Med . 2009;4(1):11-15.- Theilon S.N. et al., "Intestinal permeability in preterm infants and its association with type of feeding: breast milk or formula." Brestfeed Med (Breastfeeding Medicine). 2009;4(1):11-15.
8 Newburg DS. Innate immunity and human milk. J Nutr . 2005;135(5):1308-1312. — Newburgh, D.S., "Natural Immunity and Breast Milk." F Int. 2005;135(5):1308-1312.
9 Patel AL et al. Impact of early human milk on sepsis and health-care costs in very low birth weight infants. J Perinatol . 2013;33(7):514-519.- Patel A.L. et al., "Impact of early breast milk on sepsis and health care costs in extremely low birth weight infants". Zh Perinatol (Journal of Perinatology). 2013;33(7):514-519.
2013;33(7):514-519.- Patel A.L. et al., "Impact of early breast milk on sepsis and health care costs in extremely low birth weight infants". Zh Perinatol (Journal of Perinatology). 2013;33(7):514-519.
10 Zhou J et al . Human milk feeding as a protective factor for retinopathy of prematurity: a meta-analysis. Pediatrics. 2015;136(6): e 1576-1586. - Zhou Q. et al., "Breastfeeding as a protective factor against retinopathy of prematurity: a meta-analysis." Pediatrix (Pediatrics). 2015;136(6):e1576-1586.
11 Patel AL et al. Influence of own mother's milk on bronchopulmonary dysplasia and costs. Arch DIS Child Fetal Neonat ED . 2017;102(3): F 256- F 261. - Patel A.L. et al., "Effect of breast milk on bronchopulmonary dysplasia and health care costs." Arch Dis Child Fetal Neonate Ed. 2017;102(3): F 256- F 261.
- Patel A.L. et al., "Effect of breast milk on bronchopulmonary dysplasia and health care costs." Arch Dis Child Fetal Neonate Ed. 2017;102(3): F 256- F 261.
12 MEIER PP ET AL AL AL AL AL AL AL AL AL AL AL AL AL AL AL AL AL AL AL AL Improving the use of human milk during and after the NICU stay. Clin Perinatol. 2010;37(1):217-245. - Meyer P.P. et al., "Optimizing the use of breast milk during and after a stay in the neonatal intensive care unit." Wedge Perinatol. (Clinical perinatology). 2010;37(1):217-245.
13 Lucas A, Cole TJ. Breast milk and neonatal necrotising enterocolitis. Lancet. 1990;336(8730-8731):1519-1523. — Lucas A, Cole TJ, "Breast milk and neonatal necrotizing enterocolitis. " Lancet 1990;336(8730-8731):1519-1523.
" Lancet 1990;336(8730-8731):1519-1523.
14 Schanler RJ et al. Randomized trial of donor human milk versus preterm formula as substitutes for mothers' own milk in the feeding of extremely premature infants. Pediatrics. 2005;116(2):400-406. - Chanler R.J. et al., "Randomized Trial of Donor Human Milk Versus Prematurity Formula as a Breast Milk Substitute in Severely Preterm Infants". Pediatrix (Pediatrics). 2005;116(2):400-406.
15 Vohr BR et al. Beneficial effects of breast milk in the neonatal intensive care unit on the developmental outcome of extremely low birth weight infants at 18 months of age. Pediatrics. 2006;118(1): e 115-123. - Thief B.R. et al., Developmental Beneficial Effects of Breast Milk in the Intensive Care Unit on Extremely Low Birth Weight Infants by 18 Months of Age. Pediatrix (Pediatrics). 2006;118(1):e115-123.
16 Victora CG et al. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet. 2016;387(10017):475-490. - Victor S.J. et al., "Breastfeeding in the 21st century: epidemiology, mechanisms and long-term effects". Lancet (Lancet). 2016;387(10017):475-490.
17 Lewandowski AJ et al. Breast milk consumption in preterm neonates and cardiac shape in adulthood. Pediatrics. 2016;138(1): pii : e 20160050. - Lewandowski, A.J. et al., "Breastfeeding in preterm infants and cardiovascular health in adulthood." Pediatrix (Pediatrics). 2016;138(1):pii:e20160050.
18 Meier PP et al. Which breast pump for which mother: an evidence-based approach to individualizing breast pump technology. J. Perinatol. 2016;36(7):493-499. - Meyer P.P. et al., Breastpump Selection: A Scientific Approach to Customizing Pumping Technology. J Perinatol (Journal of Perinatology). 2016;36(7):493-499.
J Perinatol (Journal of Perinatology). 2016;36(7):493-499.
19 Parker LA et al. Effect of early breast milk expression on milk volume and timing of lactogenesis stage II among mothers of very low birth weight infants: a pilot study. J Perinatol. 2012;32(3):205-209. - Parker L.A. et al., "Effect of early pumping on milk supply and timing of the second stage of lactogenesis in mothers of extremely low birth weight infants: a pilot study." J Perinatol (Journal of Perinatology). 2012;32(3):205-209.
20 Meier PP et al. Breast pump suction patterns that mimic the human infant during breastfeeding: greater milk output in less time spent pumping for breast pump-dependent mothers with premature infants. J Perinatol. 2012;32(2):103-110. - Meyer P.P. et al., "Pumping patterns that mimic breastfeeding behavior: more milk and less time for constantly pumping mothers of preterm infants. " J Perinatol (Journal of Perinatology). 2012;32(2):103-110.
" J Perinatol (Journal of Perinatology). 2012;32(2):103-110.
21 Parker LA et al. Association of timing of initiation of breastmilk expression on milk volume and timing of lactogenesis stage II among mothers of very low-birth-weight infants. Breastfeed Med . 2015;10(2):84-91. - Parker L.A. et al., "Effect of early pumping on milk supply and timing of the second stage of lactogenesis in mothers of extremely low birth weight infants: a pilot study." Brestfeed Med (Breastfeeding Medicine). 2015;10(2):84-91.
22 Lee J et al. Oropharyngeal colostrum administration in extremely premature infants: an RCT. Pediatrics. 2015;135(2): e 357-366. - Lee J. et al., "Oropharyngeal colostrum ingestion in very preterm infants: a randomized controlled clinical trial." Pediatrix (Pediatrics). 2015;135(2):e357-366.
23 Prime PK et al. Simultaneous breast expression in breastfeeding women is more efficacious than sequential breast expression. Breastfeed Med 2012; 7(6):442–447. - Prime D.K. and co-authors. "During the period of breastfeeding, simultaneous pumping of both breasts is more productive than sequential pumping." Brestfeed Med (Breastfeeding Medicine). 2012;7(6):442-447.
Simultaneous breast expression in breastfeeding women is more efficacious than sequential breast expression. Breastfeed Med 2012; 7(6):442–447. - Prime D.K. and co-authors. "During the period of breastfeeding, simultaneous pumping of both breasts is more productive than sequential pumping." Brestfeed Med (Breastfeeding Medicine). 2012;7(6):442-447.
24 Uvn 9 ä s Oxytocin effects in mothers and infants during breastfeeding. Infant 2013; 9(6):201–206. - Uvenas-Moberg K, Prime DK, "Oxytocin effects on mother and child during breastfeeding". Infant. 2013;9(6):201-206.
25 Boundy EO et al. Kangaroo mother care and neonatal outcomes: a meta-analysis. Pediatrics. 2015;137(1): e 20152238. - Boundi I.O. and co-authors, "The Kangaroo Method and Its Impact on Newborns: A Meta-Analysis". Pediatrix (Pediatrics). 2015;137(1): e20152238.
Pediatrix (Pediatrics). 2015;137(1): e20152238.
26 Acuña-Muga J et al. Volume of milk obtained in relation to location and circumstances of expression in mothers of very low birth weight infants. J Hum Lact . 2014;30(1):41-46 - Akunya-Muga, J. et al., "The amount of milk expressed by location and circumstances of pumping in mothers of extremely low birth weight infants." F Hum Lakt. 2014;30(1):41-46
27 Nyqvist KH et al. Towards universal kangaroo mother care: recommendations and report from the first European conference and seventh international workshop on kangaroo mother care. Acta Paediatr . 2010;99(6):820-826.- Nukvist K.H. et al., "On the Universality of the Kangaroo Method: Recommendations and Report from the First European Conference and the Seventh International Kangaroo Method Workshop".