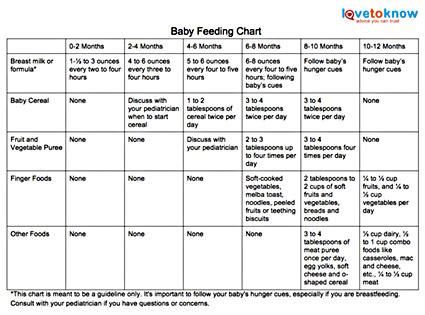
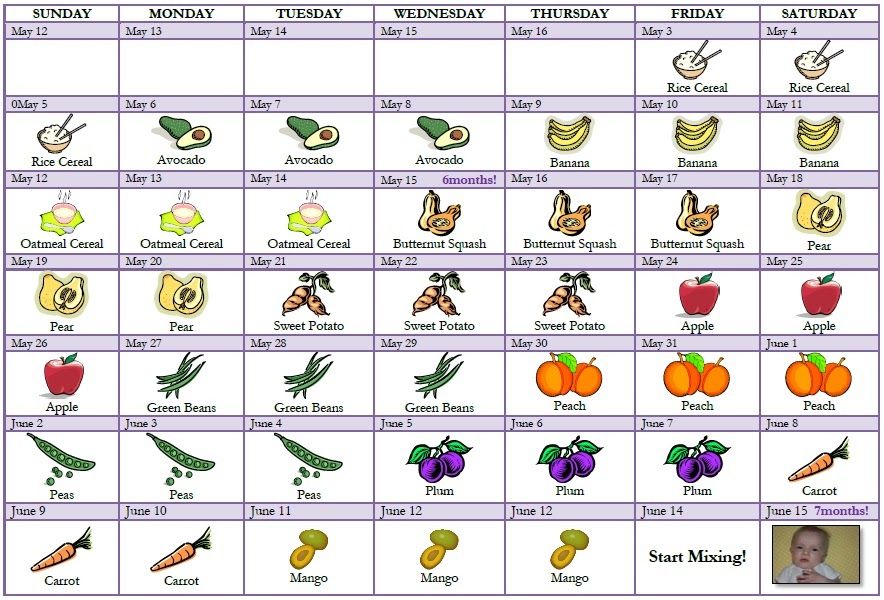
How to pump breast milk and feed baby
Pump and Store | Breastfeeding Basics
Home / Breastfeeding Basics / Pump and Store
Content begins herePlanning Ahead
If you will be away from your baby long enough to miss one or more feedings, pump or hand express your milk at the same time you would have normally breastfed your baby. This will help you keep up your milk supply so you can continue breastfeeding, even if you return to work or school. Storing your breastmilk safely after you pump will make sure your baby always has the nourishment he needs while you are away.
Pumping Tips
Express your milk faster
You can express your milk much faster if you use an electric breast pump and your hands at the same time.
Get a free pump
If you are going back to work or school, or are having a hard time building your milk supply, you can get a free pump from your health plan. Call the number on your health plan card to ask about this benefit. If you have trouble getting a pump from your health plan, call your WIC clinic. They can help.
Start pumping on your maternity leave
If you plan to go back to work, it's a good idea to begin pumping while you are still on maternity leave. It will help you get prepared and build a backup supply of breastmilk. You can begin anytime you feel ready. Start with pumping once a day between feedings. Many moms find that they are able to express more milk in the morning. Once you find a time that works best for you, try to pump around the same time each day.
Keep a consistent schedule
When you return to work, you will need to express your milk during the times you would normally feed your baby. Let your employer know about the importance of keeping that same schedule. Pumping at work will help you breastfeed your baby longer because it tells your body to keep making milk. It will also keep your body comfortable so that you can focus on work.
Thoughts of your baby can help milk flow
If you look at a picture of your baby, listen to a recording of your baby's voice, or think about nursing your baby, it can help you relax and start your milk flow.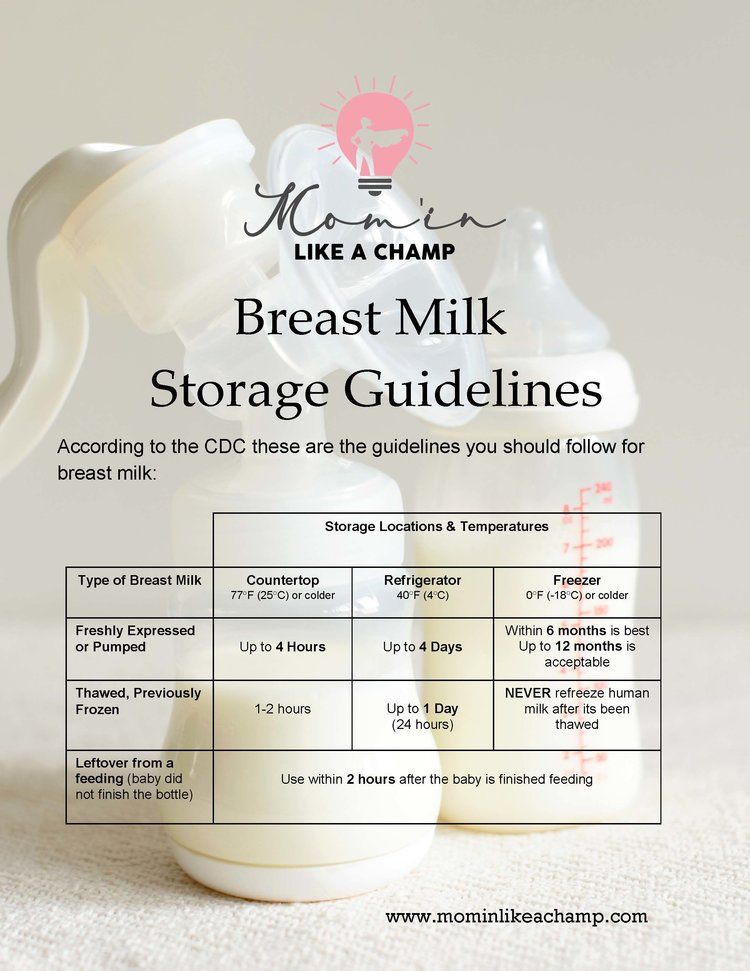
The basics of pumping
Wash your hands first
Wash your hands before pumping breastmilk, and then massage both breasts.
Start with a low suction
Pump both breasts at the same time, starting with low suction. Then increase to a comfortable suction. If you can free up one of your hands, try compressing your breasts (squeeze softly and then let go, over and over) to get more milk out. Continue until your milk flow slows to a trickle.
Massage
Massage your breasts again, especially in areas that feel full.
Express into the pump's bottle
Finish by hand expressing your milk into the pump's bottle shield or pumping one breast at a time. Do whichever way you are able to express the most milk.
Pump regularly
Your breasts make more milk than you will be able to pump, but it is important to pump regularly while you are away from your baby. It will keep up your milk supply.
Pumping shouldn't hurt
Pumping shouldn't hurt. If you have pain or difficulty with pumping, ask the WIC office or a lactation consultant for help.
If you have pain or difficulty with pumping, ask the WIC office or a lactation consultant for help.
If you have experienced an injury or infection from a breast pump, please report your breast pump issue to the FDA. This can help them to better understand the risks of breast pumps and potentially prevent problems from happening to others.
How to Store Breastmilk
Wash your hands before handling breastmilk.
You can store breastmilk in a plastic or glass bottle with a screw-on lid or in sterile zip-seal breastmilk storage bags. You can find these in the baby section of most grocery stores.
Label the containers with the date the milk was pumped and your baby's name. This is helpful if your baby goes to child care where there is more than one infant or if more than one mom is pumping at work.
Cool down the breastmilk you pump as soon as possible. You can store it in a refrigerator or in a cooler with ice packs. The milk can also be frozen if you aren't going to use it right away.
Store breastmilk in amounts that you use for a normal feeding. Since you can't re-freeze breastmilk, you may want to start by storing about 2 to 4 ounces per bottle or bag. Every ounce counts!
How to use pumped breastmilk
Color variations
- Many moms notice the breastmilk in their refrigerator looks blue, yellow, or brown and wonder if something is wrong. That is normal—the color of breastmilk can be different depending on the foods you eat.
- It is also normal for breastmilk to separate, so that the fatty part of the milk rises to the top.
- Gently tilt the bottle or the sealed bag back and forth, and the fat will go back into the milk. Do not shake the bag or bottle.
Breastmilk storage guidelines
| Storage method | Best used within | Still safe to use within |
|---|---|---|
| Insulated cooler bag | 24 hours | 24 hours |
| Refrigerator | 3 days | 5 days |
| Freezer section inside a refrigerator | 2 weeks | 2 weeks |
| Freezer with a separate door or deep freezer | 6 months | 12 months |
Related Articles
How to Pump and Store Your Breast Milk
Some women choose to pump and store their breast milk. You may decide to do this when you return to work after maternity leave. Or you may want to pump so that your partner can feed the baby breast milk. Whatever the reason, pumping allows you to continue to feed your baby breast milk through a bottle. You can buy or rent an electric or hand-operated breast pump to use. Some hospitals and insurance plans provide one for free.
You may decide to do this when you return to work after maternity leave. Or you may want to pump so that your partner can feed the baby breast milk. Whatever the reason, pumping allows you to continue to feed your baby breast milk through a bottle. You can buy or rent an electric or hand-operated breast pump to use. Some hospitals and insurance plans provide one for free.
This article answers common questions about pumping and storing breast milk.
Path to improved health
Pumping breast milk
When should I start to pump?
If you plan to pump when you return to work, start practicing 1 or 2 weeks in advance. This helps you learn how your pump works. You can pump right after your baby eats or between feedings. Or you may prefer to pump from one breast while you feed your baby from the other.
Starting at home also helps you build a collection of breast milk. You can store it for your baby’s feedings when you return to work.
How much milk will I get when I pump?
You may not get much milk when you first start pumping. This will change as you continue to pump regularly. Your breasts will begin to make more milk. The more often you pump, the more milk your breasts make. Drink lots of fluids to stay hydrated. This will also help your milk supply.
This will change as you continue to pump regularly. Your breasts will begin to make more milk. The more often you pump, the more milk your breasts make. Drink lots of fluids to stay hydrated. This will also help your milk supply.
How long should I pump each time?
It takes about the same time to pump milk as it does to breastfeed. With practice, you may be able to pump in as little as 10 to 15 minutes. While you are at work, try to pump as often as your baby usually feeds. This may be every 3 to 4 hours for 15 minutes each time. To keep up your milk supply, give your baby extra feedings when you are together. You also can pump right after your baby feeds to help your breasts make more milk.
Will there be times that my baby needs more milk than I have ready?
Yes, your baby needs more milk during growth spurts. These occur at about 2 weeks and 6 weeks of age and again at about 3 months and 6 months of age. The best way to increase your milk supply for a growth spurt is to breastfeed or pump more often.
Storing breast milk
How should I store my breast milk?
There are a couple of ways you can store breast milk. You can use a plastic or glass bottle with a sealable top. Or you can use a sterile, sealable bag. Store your breast milk in the amount your baby consumes in a feeding. This way, you don’t waste any milk. For example, if your baby eats 4 ounces in a feeding, put 4 ounces of breast milk in the storage container. Always put a date on the container of breast milk so you know how long to keep it.
Where should I store my breast milk?
Store your pumped breast milk in a refrigerator or cooler with ice as soon as possible. You also can freeze the milk if you aren’t going to use it right away.
How long can I store my breast milk?
The life of breast milk varies based on how it is stored.
- At room temperature (less than 77°F), it lasts up to 6 hours.
- In a cooler with ice packs, it lasts up to 24 hours.
- In the refrigerator, it lasts for 3 to 8 days.
- In the freezer, it lasts up to 6 months.
Things to consider
Stored breast milk can vary in color. It can be bluish, yellowish, or brownish. It is normal for breast milk to separate (the fatty part of the milk goes to the top). Shake the bottle or sealed bag and the fat should go back into the milk. If it does not, then the breast milk may be bad. You should smell the milk before feeding it to your baby. Bad milk smells sour. If you still aren’t sure, try tasting the milk. If it tastes sour, then it is bad and needs to be thrown away.
If you choose to freeze breast milk, you need to thaw it before giving it to your baby. There are 2 ways you can thaw the milk.
- Put the container of milk in warm water. Swirl the container around in the water until the milk thaws.
- Put the container of milk in the refrigerator the day before it is to be used.
Thawed breast milk can be refrigerated for up to 24 hours, but it should not be refrozen. Do not use hot water to thaw breast milk. The milk could get too hot and burn your baby’s mouth. Do not thaw frozen breast milk in a microwave. This can damage valuable proteins in breast milk.
Do not use hot water to thaw breast milk. The milk could get too hot and burn your baby’s mouth. Do not thaw frozen breast milk in a microwave. This can damage valuable proteins in breast milk.
Questions to ask your doctor
- How early after birth can I start pumping breast milk?
- How long can I pump and store breast milk?
- What type of bottles should I use to store breast milk?
- What should I do if my baby prefers bottle-feeding to breastfeeding?
- What happens if I accidentally give my baby bad breast milk?
- Can drugs or medicines I take get in my breast milk?
Resources
American Academy of Family Physicians: Breastfeeding: Returning to Work
Copyright © American Academy of Family Physicians
This information provides a general overview and may not apply to everyone. Talk to your family doctor to find out if this information applies to you and to get more information on this subject.
Expressing, storing and thawing breast milk
Unlike breastfeeding, which is a natural process, pumping works a little differently.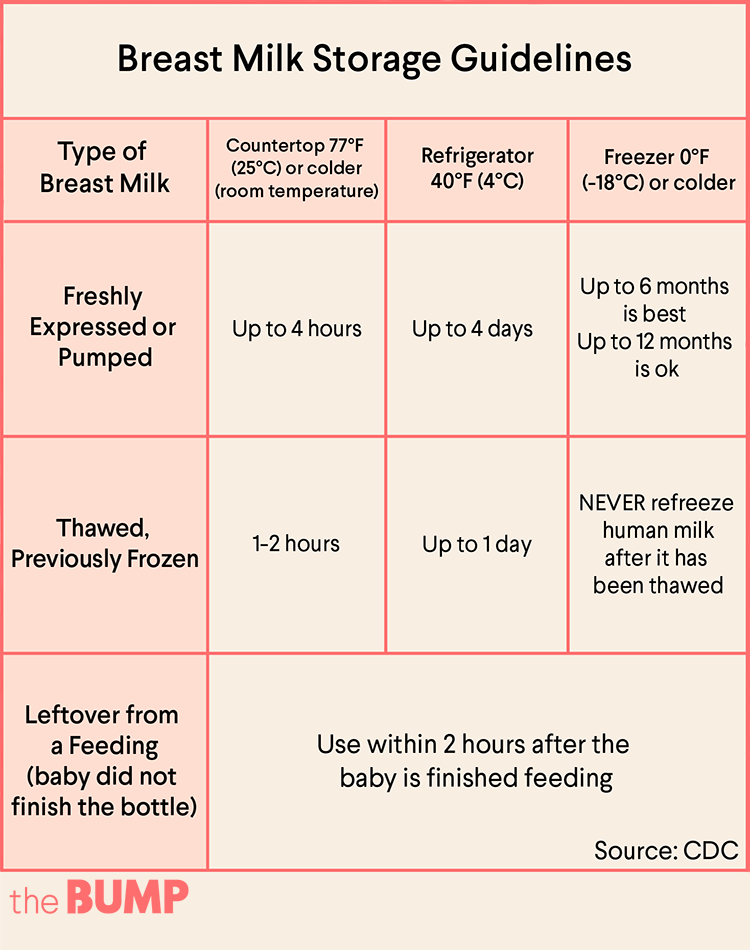 That is why efforts should be made to keep the milk flowing during pumping. Here are some ways that can make pumping easier:
That is why efforts should be made to keep the milk flowing during pumping. Here are some ways that can make pumping easier:
- Calm and pleasant environment
- Optimistic attitude
- Self-confidence and support of others
- Confidence in an emotional connection with the infant
- Having the baby present during pumping (if this is not possible, sometimes looking at his picture or smelling his clothes is enough)
- Soothing warm drink (not coffee)
- Hot shower or hot compresses before pumping
- Gently massage the nipples
- Gently stroke the areola and nipples with the fingertips
- Gently massage with clenched fists over the breast towards the nipple
- Massage the back between the shoulder blades along the spine with circular movements of the thumbs for several minutes
How to express milk?
First of all, wash your hands with soap and water. It is not necessary to wash the nipple specifically.
Principle of pumping:
In the first 3 days after birth, pump 5 minutes on each side, 3 times on each breast. From the fourth day (when milk already appears), you should express until the milk stops flowing and then switch to the second breast. A double-ended pump can express for at least 10 minutes. It should be pumped 8 times a day: once before bedtime, once after sleep and 6 more times during the day. There should be no more than 6 hours between evening and morning pumping, otherwise it may make pumping difficult. nine0003
You can massage your nipples with breast milk after every pumping.
If the mother is interested in breastfeeding in the future, this method is very important especially in the first weeks after childbirth, as it stimulates the production of milk in an amount sufficient for the child.
For your information: pumping is a temporary option. Once your baby is able to latch on (each baby has a different developmental rhythm), you can gradually transition to breastfeeding
- In the skin-to-skin position, you can let it slide a little lower towards the chest to get used to the position, sniff and lick the nipple name.
- It is advisable to give the baby fresh milk
- If you bring fresh milk in the morning or in the evening, they will prefer to use it first, and only then the frozen leftovers
- At a certain stage, the infant will begin to receive a breast milk supplement - HMF (Human Milk Fortifier), a fortifying supplement containing protein, calcium and phosphorus, which are not supplied to premature babies in sufficient quantities

Rules of behavior in the pumping room
- Wash hands before using the pumping device
- Only breastfeeding mothers are allowed to enter the pumping room, fathers are not allowed to enter so as not to cause discomfort to other women
- You can’t eat in the pumping room, you can and should drink
- Cleanliness and order should be observed
- After pumping, disassemble the bottles into parts and wash them in a specially designed machine
Storage of mother’s milk
Mother’s milk is stored in plastic sealed container, which can be obtained from a nurse. The label on the container will include your name, the date and time you pumped, and a sticker with your baby's details. nine0003
The label on the container will include your name, the date and time you pumped, and a sticker with your baby's details. nine0003
For premature babies and newborns, store milk in the refrigerator compartment for up to 24 hours, in the freezer for up to 4 months.
At home, you can store your expressed milk in the refrigerator for up to 4 days and in the freezer (not in the door) for up to 4 months.
In a cold place, breast milk separates into a more watery and fatty layer, you can shake it a little before drinking.
Again, freshly expressed milk is most preferred by the infant. If you are going to bring expressed milk from home, you must arrive at the office before 9in the morning so that fresh milk can be used on the same day, since the daily portions are prepared only in the morning.
Milk should be brought fresh or frozen in a container with ice.
Thawing breast milk
- Thawing breast milk is done at room temperature
- Thawed milk can be stored in the refrigerator for up to 24 hours
- Do not refreeze thawed milk
- Fresh milk is always preferred, but when the baby first starts eating it will be before total frozen colostrum used, in date and hour order (within the first 4 days of pumping).
 nine0006
nine0006 - Heating breast milk after being in the refrigerator will only be heated in a special device by the ward nurse. Parents are not allowed to touch it. Heating milk in a microwave oven is not recommended, as the radiation destroys some of the ingredients.
Feeding with expressed milk | breastfeeding
When can I start breastfeeding my baby with expressed breast milk? How to do it right? Is it worth worrying that the child will confuse the pacifier with the breast? In this article we will answer your questions. nine0003
Share this information
When can I start breastfeeding my baby?
If your baby is healthy and breastfeeding well, there is no need to give him expressed milk. For the first four weeks, you work together to start and increase milk production, and your baby also learns to suckle properly at the breast. There is not yet enough scientific evidence on this, 1 but there is an opinion that bottle feeding in the first month may negatively affect the process of establishing breastfeeding. nine0003
nine0003
However, if the newborn is unable to latch on or suckle for some reason, start expressing milk as soon as possible after birth. Read more about this in our articles on coping with problems in the first week, breastfeeding premature babies and babies with special needs, and seeking help from your healthcare provider.
How to feed your baby with expressed breast milk?
There are many expert feeding solutions that allow you to give your baby expressed milk in a variety of ways, depending on your and your baby's needs. nine0003
For example, the innovative Calma smart pacifier only lets milk through when the baby creates a vacuum by suckling. This means that when feeding from a bottle, he will make the same movements with his tongue and jaws as when sucking at the breast. 2.3 The Calma Smart Soother was developed with input from breastfeeding experts at the University of Western Australia. When using this pacifier, the baby can suck, swallow, pause and breathe in the same way as when breastfeeding. nine0109 4 Preservation of natural sucking skills allows the baby to easily transition from breast to bottle and back.
nine0109 4 Preservation of natural sucking skills allows the baby to easily transition from breast to bottle and back.
In addition, Medela also offers regular bottle teats* in two versions that produce milk at different rates. All Medela* nipples can be placed directly on bottles used for expressing milk, minimizing the risk of spillage.
If you need to feed your baby with expressed milk, but you do not want to bottle feed him until he is learning to breastfeed, you can use a sippy cup* for temporary feeding. The baby will be able to drink milk from such a mug, but you should be careful not to spill the milk. For the first time, it is advisable to feed the child from a drinking cup under the supervision of the attending physician in order to learn how to do it correctly. nine0003
If your baby needs to be supplemented with expressed milk in addition to regular breastfeeding, the Supplementary Feeding System (SNS)* can be used. It is equipped with a thin, flexible capillary that can be clipped close to the nipple to give your baby expressed milk while breastfeeding.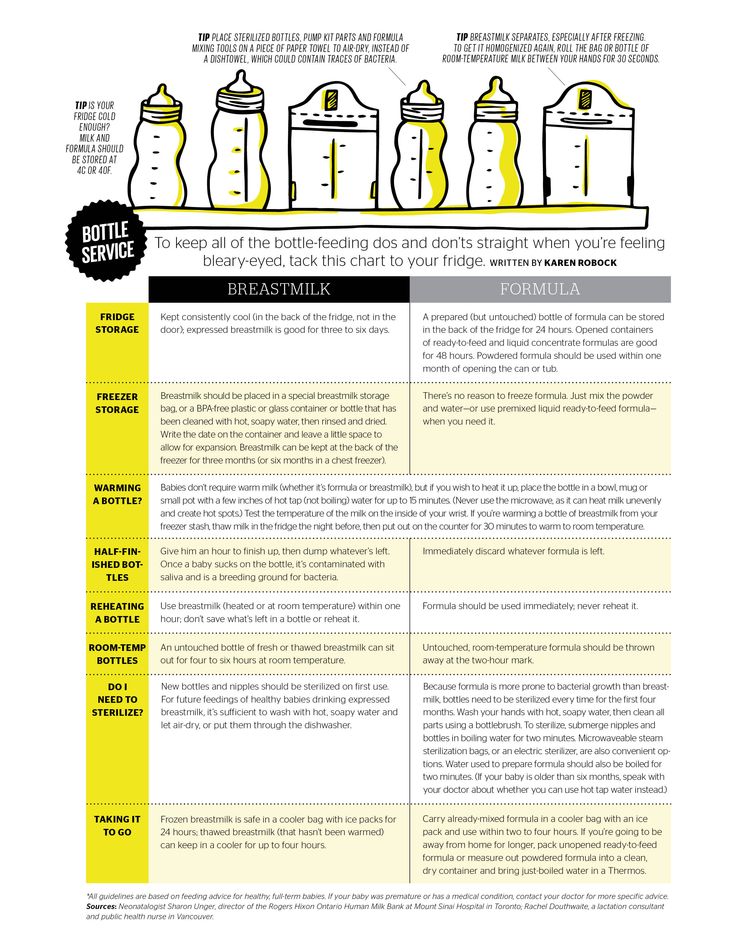 Thanks to this, the baby suckles the breast for longer, thereby developing sucking skills and stimulating the production of milk from the mother. This can be helpful when there is a shortage of breast milk, as well as when feeding adopted or surrogate children. nine0003
Thanks to this, the baby suckles the breast for longer, thereby developing sucking skills and stimulating the production of milk from the mother. This can be helpful when there is a shortage of breast milk, as well as when feeding adopted or surrogate children. nine0003
If the baby is unable to breastfeed because he is too weak or has a congenital disease, you can use the Special Needs Cup*, which releases milk with gentle pressure, making it suitable for feeding these babies.
How to teach a child to bottle feed?
If breastfeeding is going well and you decide to start bottle feeding your baby with expressed breast milk, follow these guidelines.
Start early and take your time
Don't wait until the first day of work or the first time you leave the house to start bottle feeding your baby. Start accustoming your baby to small portions of expressed milk a couple of weeks before the desired date, calmly and without haste. Gradually build up to one full serving of pumped milk from a bottle.
Choose a time
Ideally, at the first bottle feeding, the baby should be hungry, but not too hungry - in this state, he is as relaxed as possible. nine0003
Let others feed
Your baby is used to feeding from your breast, so when you offer him a bottle it can be confusing. The process can go faster if the first time the baby is bottle-fed by someone else while you are not in the room, so that your sight and smell do not embarrass the baby.
Maintain optimal temperature
Your baby will be more willing to eat expressed milk if the temperature is around 37°C, close to body temperature. nine0003
Dip a nipple in milk
Try dipping a nipple in expressed milk before offering it to your baby. This way it will taste and smell like your breast milk. Lightly touch the baby's upper lip with the nipple to open the mouth.
Choose the right position for bottle feeding
Feed your baby on demand and keep him reclining during feeding. Never bottle feed your baby when he is lying or sitting, otherwise he may choke. Listen to the wishes of the child - take as many pauses as he needs. You can even try to shift it from one hand to another during feeding. nine0003
Never bottle feed your baby when he is lying or sitting, otherwise he may choke. Listen to the wishes of the child - take as many pauses as he needs. You can even try to shift it from one hand to another during feeding. nine0003
Be patient
Don't worry if your baby doesn't take the bottle right away - it may take several tries. If he pushes the bottle away or starts crying, calm him down, wait a few minutes and try again. If he still doesn't want to bottle feed, wait a few more minutes and breastfeed him as usual. Repeat the bottle experiment at a different time of day.
How much expressed milk should I give my baby? nine0029
All children are different. Research shows that between the ages of one and six months, a baby can consume between 50 and 230 ml of milk per feeding. To start, prepare about 60 ml and observe how much your baby needs - more or less. You will soon realize how much milk he usually eats. Just never force him to finish the cooked portion.
How can I keep my baby safe when bottle feeding?
Always clean and sterilize your breast pump and bottles according to the manufacturer's instructions. Wash your hands before expressing, pouring milk, and feeding your baby. Follow our instructions for safely storing and thawing your expressed milk. nine0003
If breastmilk needs to be warmed, place the bottle or bag in a bowl of warm water or a heater or under running water at a maximum of 37°C. Never heat breast milk in the microwave or on the stove.
Will the baby be able to transition from breast to bottle?
Some mothers worry that if they start bottle feeding too early, they will get used to the artificial nipple and not want to breastfeed. Others, on the contrary, are worried that if the child is not immediately accustomed to the bottle, then he will no longer eat from it. In general, in these cases, they say that the child confuses the nipple with the breast. nine0003
Experts disagree on whether such confusion is a problem. 1 Without a doubt, it is easier for a baby to suckle milk from a regular bottle with a nipple, which does not require a vacuum, than from the breast, since the milk flows faster, also under the influence of gravity. And some babies really have clear preferences: only the breast or only the nipple. However, many babies are comfortable suckling both the breast and the pacifier.
1 Without a doubt, it is easier for a baby to suckle milk from a regular bottle with a nipple, which does not require a vacuum, than from the breast, since the milk flows faster, also under the influence of gravity. And some babies really have clear preferences: only the breast or only the nipple. However, many babies are comfortable suckling both the breast and the pacifier.
If you are unable to feed your baby with expressed breast milk, seek help from a lactation consultant or specialist. nine0003
Literature
1 Zimmerman E, Thompson K. Clarifying nipple confusion. J. Perinatol. 2015;35(11):895-899. - Zimmerman I., Thompson K., "On the issue of breastfeeding." J Perinatol (Journal of Perinatology). 2015;35(11):895-899.
2 Geddes DT et al. Tongue movement and intra-oral vacuum of term infants during breastfeeding and feeding from an experimental teat that released milk under vacuum only. Early Hum Dev .