Mothers feeding babies
Frequently Asked Questions (FAQs) | Breastfeeding
What are the benefits of breastfeeding?
Breastfeeding is good for both infants and mothers. Breast milk is the best source of nutrition for most infants. As an infant grows, breast milk changes to meet the infant’s nutritional needs. Breastfeeding can also help protect the infant and mother against certain illnesses and diseases:
Benefits to Infants
Infants who are breastfed have a lower risk of:
- Asthma.
- Obesity.
- Type 1 diabetes.
- Severe lower respiratory disease.
- Acute otitis media (ear infections).
- Sudden infant death syndrome (SIDS).
- Gastrointestinal infections (diarrhea/vomiting).
- Necrotizing enterocolitis (NEC) for preterm infants.
Benefit to Mothers
Mothers who breastfeed their infants have a lower risk of:
- Breast cancer.
- Ovarian cancer.
- Type 2 diabetes.
- High blood pressure.
Families can visit CDC’s Infant and Toddler Nutrition website to learn more about what to expect while breastfeeding.
When should a mother avoid breastfeeding (contraindications)?
Breast milk provides the best nutrition for most infants, including premature and sick newborns. However, there are rare exceptions when breast milk or breastfeeding is not recommended. Learn more about contraindications to breastfeeding.
Only a few medications are contraindicated (not recommended) while breastfeeding. Although many medications do pass into breast milk, most have little or no effect on milk supply or on an infant’s well-being. However, health care providers should always weigh the risks and benefits when prescribing medications to breastfeeding mothers.
Learn more about safe prescription medication use while breastfeeding.
Top of Page
How is growth assessed for breastfed infants?
In the United States, the World Health Organization (WHO) Growth Standard Charts are recommended for use with both breastfed and formula-fed infants and children, from birth to 2 years of age, to monitor growth. The WHO growth charts reflect growth patterns among children who were predominantly breastfed for at least 4 months and were still breastfeeding at 12 months. The WHO growth charts establish the growth of the breastfed infant as the norm for growth and are the standards for how children should grow when provided optimal conditions. Clinicians should be aware that healthy breastfed infants typically gain weight faster than formula-fed infants in the first few months of life but then gain weight more slowly for the remainder of infancy, even after complementary foods are introduced.
The WHO growth charts reflect growth patterns among children who were predominantly breastfed for at least 4 months and were still breastfeeding at 12 months. The WHO growth charts establish the growth of the breastfed infant as the norm for growth and are the standards for how children should grow when provided optimal conditions. Clinicians should be aware that healthy breastfed infants typically gain weight faster than formula-fed infants in the first few months of life but then gain weight more slowly for the remainder of infancy, even after complementary foods are introduced.
For children older than 2 years (2 to 19 years of age) CDC and the American Academy of Pediatrics recommend that health care providers use the CDC Growth Reference Charts.
Visit the Growth Chart Training website for a set of self-directed, interactive training courses.
Source: Grummer-Strawn LM, Reinold C, Krebs NF. Use of the World Health Organization and CDC growth charts for children aged 0 to 59 months in the United States. MMWR Recomm Rep. 2010;59(RR-9):1–15.
MMWR Recomm Rep. 2010;59(RR-9):1–15.
Top of Page
How long should a mother breastfeed?
The U.S. Dietary Guidelines for Americans [PDF-30.6MB] recommend that infants be exclusively breastfed for about the first 6 months, and then continuing breastfeeding while introducing appropriate complementary foods until your child is 12 months old or older. The American Academy of Pediatrics and the World Health Organization also recommend exclusive breastfeeding for about the first 6 months, with continued breastfeeding along with introducing appropriate complementary foods for up to 2 years of age or longer.
Mothers should be encouraged to breastfeed their children for at least 1 year. The longer an infant is breastfed, the greater the protection from certain illnesses and long-term diseases. The more months or years a woman breastfeeds (combined breastfeeding of all her children), the greater the benefits to her health as well.
The American Academy of Pediatrics recommends that children be introduced to foods other than breast milk or infant formula when they are about 6 months old. To learn more about infant and toddler feeding, visit CDC’s Infant and Toddler Nutrition website.
To learn more about infant and toddler feeding, visit CDC’s Infant and Toddler Nutrition website.
Top of Page
What can happen if someone else’s breast milk is given to another child?
Very few illnesses are transmitted via breast milk. Learn more about what to do if an infant or child is mistakenly fed another woman’s expressed breast milk.
Top of Page
Are special precautions needed for handling breast milk?
CDC does not list human breast milk as a body fluid to which universal precautions apply. Occupational exposure to human breast milk has not been shown to lead to transmission of HIV or Hepatitis B infection. However, because human breast milk has been implicated in transmitting HIV from mother to infant, gloves may be worn as a precaution by health care workers who are frequently exposed to breast milk (e.g., people working in human milk banks (defined below). For additional information regarding universal precautions as they apply to breast milk in the transmission of HIV and Hepatitis B infections, visit the following resources:
Centers for Disease Control and Prevention. Perspectives in disease prevention and health promotion update: universal precautions for prevention of transmission of human immunodeficiency virus, Hepatitis B virus, and other bloodborne pathogens in health-care settings. MMWR Morb Mortal Wkly Rep. 1988;37(24):377–388.
Perspectives in disease prevention and health promotion update: universal precautions for prevention of transmission of human immunodeficiency virus, Hepatitis B virus, and other bloodborne pathogens in health-care settings. MMWR Morb Mortal Wkly Rep. 1988;37(24):377–388.
Top of Page
Where can mothers find more information about preparation and storage of breast milk?
CDC has guidelines for proper storage and preparation of breast milk to maintain the safety and quality of expressed breast milk for the health of the baby.
For more information about specific storage and preparation of breast milk questions, such as where to store breast milk at work, and what to do when the power goes out, visit CDC’s Storage and Preparation of Breast Milk Frequently Asked Questions.
Top of Page
What are human milk banks?
Human milk banks are a service established for the purpose of collecting milk from donors and processing, screening, storing, and distributing donated milk to meet the specific needs of individuals for whom human milk is prescribed by licensed health care providers. When possible, human milk banks also serve healthy infants who have been adopted or are not able to get their own mother’s milk.
When possible, human milk banks also serve healthy infants who have been adopted or are not able to get their own mother’s milk.
Milk banks accept donations directly at their deposit sites or they can arrange for safe, overnight transportation of human milk at no cost to the donor. Learn more about donating to a milk bank by visiting the Human Milk Banking Association of North America (HMBANA).
Top of Page
Is it safe for families to buy breast milk on the internet?
The American Academy of Pediatrics and the Food and Drug Administration recommend avoiding Internet-based milk sharing sites and instead recommend contacting milk banks. Research has demonstrated that some milk samples sold online have been contaminated with a range of bacteria.1
Nonprofit donor human milk banks, where processed human milk comes from screened donors, have a long safety record in North America. All member banks of the Human Milk Banking Association of North America (HMBANA) must operate under specific evidence-based guidelines that require extensive testing and processing procedures as well as self-reported health information and a health statement from both the donor’s health care provider and the infant’s health care provider. Because most of the milk from milk banks is given to hospitalized and fragile infants, milk banks may not have enough to serve healthy infants at all times. To find a human milk bank, contact HMBANA.
Because most of the milk from milk banks is given to hospitalized and fragile infants, milk banks may not have enough to serve healthy infants at all times. To find a human milk bank, contact HMBANA.
1Keim, SA, Hogan, JS, McNamara, KA, et al. Microbial contamination of human milk purchased via the internet. Pediatrics. 2013;132(5).
Top of Page
What legal rights do breastfeeding mothers have?
Breastfeeding Laws
- All 50 states, the District of Columbia, Puerto Rico and the Virgin Islands have laws that specifically allow women to breastfeed in any public or private location. Visit the National Conference of State Legislatures to learn more about federal and state laws that protect and support breastfeeding.
Workplace Laws
- The “Break Time for Nursing Mothers Provision” of the Patient Protection and Affordable Care Act (ACA) requires employers to support breastfeeding mothers to express breast milk for 1 year after each child’s birth by providing mothers with reasonable break time and a private, non-bathroom space to express their breast milk.
 Visit the United States Department of Labor to learn more.
Visit the United States Department of Labor to learn more.
Travel Laws
- Air travelers are permitted by the Transportation Security Administration (TSA) to bring breast milk, formula, and juice in excess of 3.4 ounces in their carry-on baggage and it does not need to fit within a quart size bag. Ice packs, freezer packs, and other accessories needed to keep the liquid cool are also allowed in carry-on bags. All liquids and partially frozen accessories are subject to being screened by X-ray. TSA is required by the Bottles and Breastfeeding Equipment Screening Act (BABES act) to provide ongoing training to ensure TSA staff receive consistent training related to traveling with breast milk, formula, and infant feeding equipment. Visit the TSA to learn more about traveling with breast milk, formula, and juice. For tips on travel and breastfeeding, visit Travel Recommendations for the Nursing Mother.
Visit the Federal Policies, Programs, & Initiatives website to learn more about laws related to breastfeeding protections.
Top of Page
How can a mother continue to provide breast milk to her infant after returning to work or school?
Being prepared for returning to work or school can help a mother ease the transition and continue to breastfeed after her maternity leave is over. The Office on Women’s Health has information for making this transition easier.
When a mother is away from her infant, she can pump or hand express her breast milk so that her infant can drink breast milk from a bottle. Mothers can visit CDC’s Infant and Toddler Nutrition website to learn more about pumping breast milk.
Mothers who are expressing their breast milk should visit the CDC’s Proper Storage and Preparation of Breast Milk website to learn how to prepare and store breast milk safely for her infant.
The Patient Protection and Affordable Care Act (ACA) requires employers to support breastfeeding mothers to express breast milk for 1 year after each child’s birth by providing mothers with reasonable break time and a private, non-bathroom space to express their breast milk. For more information about the types of employees and employers to which the requirements apply, refer to the United States Department of Labor’s Frequently Asked Questions.
For more information about the types of employees and employers to which the requirements apply, refer to the United States Department of Labor’s Frequently Asked Questions.
Top of Page
Where can mothers find breastfeeding support and additional Information about breastfeeding?
Help mothers find lactation support through the following resources:
- International Lactation Consultant Association (IBCLCs)
- United States Lactation Consultant Association (IBCLCs)
- Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) clinics
- La Leche League
Help mothers find resources about breastfeeding by directing them to the following websites:
- CDC— Infant and Toddler Nutrition
- Office on Women’s Health—Breastfeeding
- American Academy of Pediatrics—Healthy Children
- United States Breastfeeding Committee—State Coalitions Directory
- US Department of Agriculture—WIC Breastfeeding Support
Top of Page
Does breastfeeding during a child’s vaccine injections help with pain management?
Parents who are breastfeeding should be encouraged to breastfeed children age 2 years or younger before, during, and after their child’s vaccination. Several aspects of breastfeeding are thought to decrease pain by multiple mechanisms: being held by the parent, feeling skin-to-skin contact, suckling, being distracted, and ingesting breast milk. Potential adverse events such as gagging or spitting up have not been reported. Alternatives to breastfeeding include bottle-feeding with expressed breast milk or formula throughout the child’s procedure, which simulates aspects of breastfeeding.
Several aspects of breastfeeding are thought to decrease pain by multiple mechanisms: being held by the parent, feeling skin-to-skin contact, suckling, being distracted, and ingesting breast milk. Potential adverse events such as gagging or spitting up have not been reported. Alternatives to breastfeeding include bottle-feeding with expressed breast milk or formula throughout the child’s procedure, which simulates aspects of breastfeeding.
Top of Page
Does breastfeeding after a child’s rotavirus vaccine impact the vaccine’s efficacy?
There is not sufficient evidence to suggest that breastfeeding can have a negative effect on rotavirus vaccine efficacy. A previous study found that human milk from women who live in areas with endemic rotavirus contains antibodies that can neutralize live rotavirus vaccine virus. However, in licensing trials, the effectiveness of rotavirus vaccine in breastfed infants was comparable to that in non-breastfed infants.
CDC does not recommend restricting or discontinuing breastfeeding before or after a child receives the rotavirus vaccine. Breastfed infants should be vaccinated according to the same schedule as non-breastfed infants.
Breastfed infants should be vaccinated according to the same schedule as non-breastfed infants.
Learn More about prevention of Rotavirus Gastroenteritis among infants and children.
Top of Page
The Benefits of Breastfeeding for Both Mother and Baby
Written by Rebecca Buffum Taylor
Reviewed by Dan Brennan, MD on July 05, 2022
In this Article
- What is Breastfeeding?
- Signs Your Baby is Hungry
- Benefits of Breastfeeding for the Baby
- Breastfeeding Benefits for the Mother
- Will You Make Enough Milk to Breastfeed?
- What's the Best Position for Breastfeeding?
- How to Get Your Baby to 'Latch on' During Breastfeeding
- Tips for New Breastfeeding Moms
- Are There Medical Considerations With Breastfeeding?
- What Are Some Common Challenges With Breastfeeding?
- Where Can I Get Help With Breastfeeding?
What is Breastfeeding?
Breastfeeding is when you feed your baby breast milk, usually directly from your breast. It’s also called nursing. Making the decision to breastfeed is a personal matter. It's also one that's likely to draw opinions from friends and family.
It’s also called nursing. Making the decision to breastfeed is a personal matter. It's also one that's likely to draw opinions from friends and family.
Many medical experts, including the American Academy of Pediatrics (AAP) and the American College of Obstetricians and Gynecologists, strongly recommend breastfeeding exclusively (no formula, juice, or water) for 6 months. After the introduction of other foods, it recommends continuing to breastfeed through the baby’s first year of life.
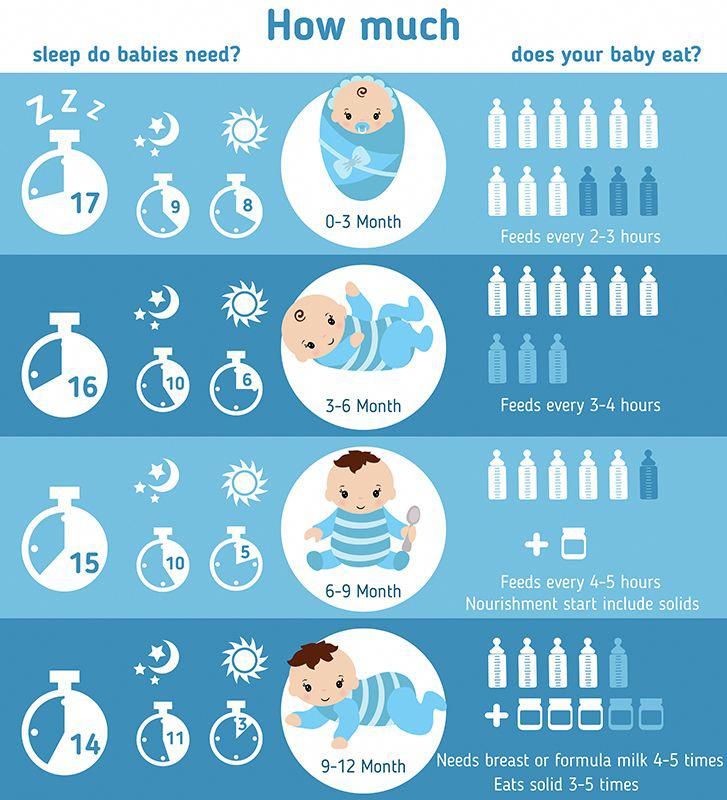
How often you should breastfeed your baby depends on whether your baby prefers small, frequent meals or longer feedings. This will change as your baby grows. Newborns often want to feed every 2-3 hours. By 2 months, feeding every 3-4 hours is common, and by six months, most babies feed every 4-5 hours.
You and your baby are unique, and the decision to breastfeed is up to you.
Signs Your Baby is Hungry
One of the most common ways your baby will let you know they're hungry is to cry.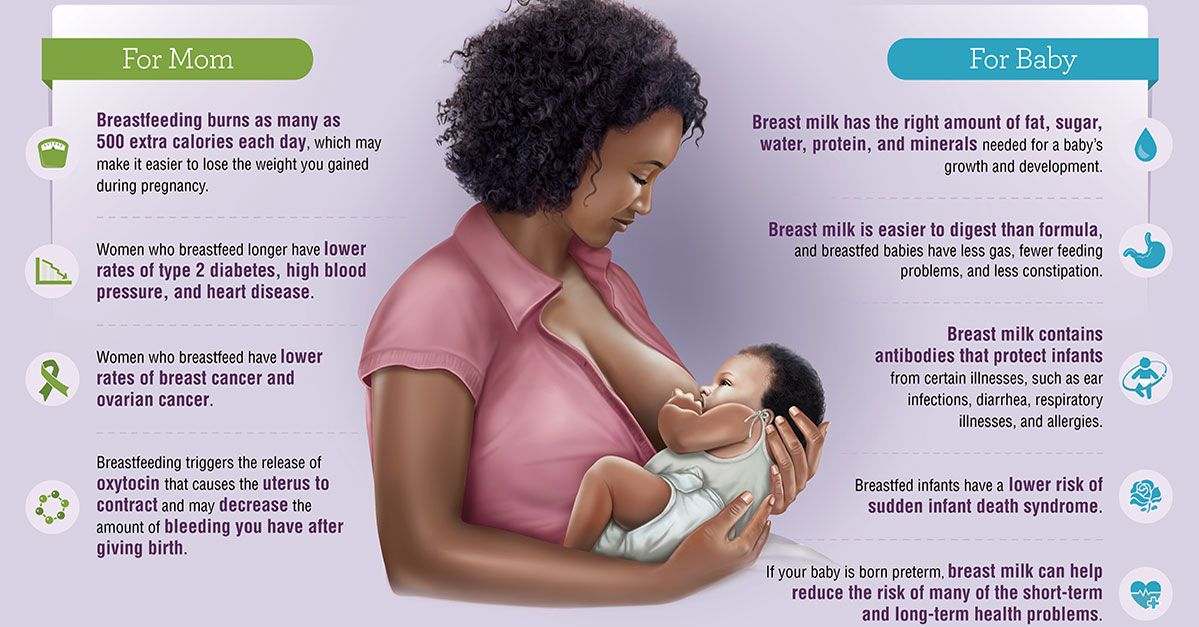 Other signs your baby is ready to be fed include:
Other signs your baby is ready to be fed include:
- Licking their lips or sticking out their tongue
- Rooting, which is moving their jaw, mouth, or head to look for your breast
- Putting their hand in their mouth
- Opening their mouth
- Fussiness
- Sucking on things
Benefits of Breastfeeding for the Baby
Breast milk provides the ideal nutrition for infants. It has a nearly perfect mix of vitamins, protein, and fat -- everything your baby needs to grow. And it's all provided in a form more easily digested than infant formula. Breast milk contains antibodies that help your baby fight off viruses and bacteria. Breastfeeding lowers your baby's risk of having asthma or allergies. Plus, babies who are breastfed exclusively for the first 6 months, without any formula, have fewer ear infections, respiratory illnesses, and bouts of diarrhea. They also have fewer hospitalizations and trips to the doctor.
They also have fewer hospitalizations and trips to the doctor.
Breastfeeding has been linked to higher IQ scores in later childhood in some studies. What's more, the physical closeness, skin-to-skin touching, and eye contact all help your baby bond with you and feel secure. Breastfed infants are more likely to gain the right amount of weight as they grow rather than become overweight children. The AAP says breastfeeding also plays a role in the prevention of SIDS (sudden infant death syndrome). It's been thought to lower the risk of diabetes, obesity, and certain cancers as well, but more research is needed.
Breastfeeding Benefits for the Mother
Breastfeeding burns extra calories, so it can help you lose pregnancy weight faster. It releases the hormone oxytocin, which helps your uterus return to its pre-pregnancy size and may reduce uterine bleeding after birth. There are continued benefits from breastfeeding beyond 1 year, and up to 2 years especially in the mother.Breastfeeding also lowers your risk of breast and ovarian cancer. It may lower your risk of osteoporosis, too.
There are continued benefits from breastfeeding beyond 1 year, and up to 2 years especially in the mother.Breastfeeding also lowers your risk of breast and ovarian cancer. It may lower your risk of osteoporosis, too.
Since you don't have to buy and measure formula, sterilize nipples, or warm bottles, it saves you time and money. It also gives you regular time to relax quietly with your newborn as you bond.
Will You Make Enough Milk to Breastfeed?
The first few days after birth, your breasts make an ideal "first milk." It's called colostrum. Colostrum is thick, yellowish, and there’s not a lot of it, but there's plenty to meet your baby's nutritional needs. Colostrum helps a newborn's digestive tract develop and prepare itself to digest breast milk.
Colostrum is the first phase of breast milk, which changes over time to give your baby the nutrition they need as they grow. The second phase is called transitional milk. You make this as your colostrum is gradually replaced with the third phase of breast milk, called mature milk.
You make this as your colostrum is gradually replaced with the third phase of breast milk, called mature milk.
You’ll start to make transitional milk a few days after birth. By 10 to 15 days after birth, you’ll make mature milk, which gives your baby all the nutrition they need.
Most babies lose a small amount of weight in the first 3 to 5 days after birth. This is unrelated to breastfeeding.
As your baby needs more milk and nurses more, your breasts respond by making more milk. Experts recommend trying to breastfeed exclusively (no formula, juice, or water) for 6 months. If you supplement with formula, your breasts might make less milk.
Even if you breastfeed less than the recommended 6 months, it's better to breastfeed for a short time than no time at all. You can add solid food at 6 months but also continue to breastfeed if you want to keep producing milk.
Is your baby getting enough milk?
Many breastfeeding moms wonder whether their babies get enough milk for good nutrition. If your baby is getting enough breastmilk they should:
If your baby is getting enough breastmilk they should:
- Not lose more than 7% of their birth weight in the first few days after delivery
- Seem content for about 1-3 hours between feedings
- Have at least 6 diapers a day wet with very pale or clear pee by the time they are 7-10 days old
What's the Best Position for Breastfeeding?
The best position for you is the one where you and your baby are both comfortable and relaxed, and you don't have to strain to hold the position or keep nursing. Here are some common positions for breastfeeding your baby:
- Cradle position. Rest the side of your baby's head in the crook of your elbow with their whole body facing you. Position your baby's belly against your body so they feel fully supported. Your other, "free" arm can wrap around to support your baby's head and neck -- or reach through your baby's legs to support the lower back.
- Football position. Line your baby's back along your forearm to hold your baby like a football, supporting the head and neck in your palm.
 This works best with newborns and small babies. It's also a good position if you're recovering from a cesarean birth and need to protect your belly from the pressure or weight of your baby.
This works best with newborns and small babies. It's also a good position if you're recovering from a cesarean birth and need to protect your belly from the pressure or weight of your baby. - Side-lying position. This position is great for night feedings in bed. Side-lying also works well if you're recovering from an episiotomy, an incision to widen the vaginal opening during delivery. Use pillows under your head to get comfortable. Then snuggle close to your baby and use your free hand to lift your breast and nipple into your baby's mouth. Once your baby is correctly "latched on," support the head and neck with your free hand so there's no twisting or straining to keep nursing.
- Cross-cradle hold. Sit straight in a comfortable chair that has armrests. Hold your baby in the crook of your arm that's opposite the breast you will use to feed them. Support their head with your hand. Bring your baby across your body so your tummies face each other.
 Use your other hand to cup your breast in a U-shaped hold. Bring your baby's mouth to your breast and cradle them close, and don't lean forward.
Use your other hand to cup your breast in a U-shaped hold. Bring your baby's mouth to your breast and cradle them close, and don't lean forward. - Laid-back position. This position, also called biological nurturing, is a lot like it sounds. It's meant to tap into the natural breastfeeding instincts you and your baby have. Lean back, but not flat, on a couch or bed. Have good support for your head and shoulders. Hold your baby so your entire fronts touch. Let your baby take any position they're comfortable in as long as their cheek rests near your breast. Help your baby latch on if they need it.
How to Get Your Baby to 'Latch on' During Breastfeeding
Position your baby facing you, so your baby is comfortable and doesn't have to twist their neck to feed. With one hand, cup your breast and gently stroke your baby's lower lip with your nipple. Your baby's instinctive reflex will be to open the mouth wide. With your hand supporting your baby's neck, bring the mouth closer around your nipple, trying to center your nipple in the mouth above the tongue.
You'll know your baby is "latched on" correctly when both lips are pursed outward around your nipple. Your infant should have all of your nipple and most of the areola, which is the darker skin around your nipple, in their mouth. While you may feel a slight tingling or tugging, breastfeeding should not be painful. If your baby isn't latched on correctly and nursing with a smooth, comfortable rhythm, gently nudge your pinky between your baby's gums to break the suction, remove your nipple, and try again. Good "latching on" helps prevent sore nipples.
Tips for New Breastfeeding Moms
Some things help you prepare for breastfeeding:
- Get regular prenatal care to help you avoid preterm birth.
- Tell your doctor you plan to breastfeed and ask what support the facility you plan to deliver in offers to help you breastfeed after birth.
- Take a breastfeeding class.
- Ask your doctor to connect you with a lactation consultant, who can teach you breastfeeding basics and help you if have issues.

- Talk to your doctor about any health conditions you have or medications you take that could interfere with breastfeeding.
- Tell your doctor and hospital health care providers that you want to breastfeed as soon as possible after delivery.
- Talk to friends who breastfeed or join a support group for breastfeeding.
- Stock up on the supplies you need for breastfeeding, such as nursing bras and other items.
These tips, called the ABCs of breastfeeding, will help you and your baby get comfortable with the process:
- Awareness. Watch for your baby's signs of hunger, and breastfeed whenever your baby is hungry. This is called "on demand" feeding. The first few weeks, you may be nursing eight to 12 times every 24 hours. Hungry infants move their hands toward their mouths, make sucking noises or mouth movements, or move toward your breast. Don't wait for your baby to cry. That's a sign their too hungry.

- Be patient. Breastfeed as long as your baby wants to nurse each time. Don't hurry your infant through feedings. Infants typically breastfeed for 10 to 20 minutes on each breast.
- Comfort. This is key. Relax while breastfeeding, and your milk is more likely to "let down" and flow. Get yourself comfortable with pillows as needed to support your arms, head, and neck, and a footrest to support your feet and legs before you begin to breastfeed.
Are There Medical Considerations With Breastfeeding?
In a few situations, breastfeeding could cause a baby harm. Here are some reasons you should not breastfeed:
- You are HIV positive. You can pass the HIV virus to your infant through breast milk.
- You have active, untreated tuberculosis.
- You're receiving chemotherapy for cancer.
- You're using an illegal drug, such as cocaine or marijuana.

- Your baby has a rare condition called galactosemia and cannot tolerate the natural sugar, called galactose, in breast milk.
- You're taking certain prescription medications, such as some drugs for migraine headaches, Parkinson's disease, or arthritis.
Talk with your doctor before starting to breastfeed if you're taking prescription drugs of any kind. Your doctor can help you make an informed decision based on your particular medication.
Having a cold or flu should not prevent you from breastfeeding. Breast milk won't give your baby the illness and may even give antibodies to your baby to help fight off the illness.
Also, the AAP suggests that -- starting at 4 months of age -- exclusively breastfed infants, and infants who are partially breastfed and receive more than half of their daily feedings as human milk, should be supplemented with oral iron. This should continue until foods with iron, such as iron-fortified cereals, are introduced in the diet. The AAP recommends checking iron levels in all children at age 1.
The AAP recommends checking iron levels in all children at age 1.
Discuss supplementation of both iron and vitamin D with your pediatrician. Your doctor can guide you on recommendations about the proper amounts for both your baby and you, when to start, and how often the supplements should be taken.
What Are Some Common Challenges With Breastfeeding?
- Sore nipples. You can expect some soreness in the first weeks of breastfeeding. Make sure your baby latches on correctly, and use one finger to break the suction of your baby's mouth after each feeding. That will help prevent sore nipples. If you still get sore, be sure you nurse with each breast fully enough to empty the milk ducts. If you don't, your breasts can become engorged, swollen, and painful. Holding ice or a bag of frozen peas against sore nipples can temporarily ease discomfort. Keeping your nipples dry and letting them "air dry" between feedings helps, too.
 Your baby tends to suck more actively at the start. So begin feedings with the less-sore nipple.
Your baby tends to suck more actively at the start. So begin feedings with the less-sore nipple. - Dry, cracked nipples. Avoid soaps, perfumed creams, or lotions with alcohol in them, which can make nipples even more dry and cracked. You can gently apply pure lanolin to your nipples after a feeding, but be sure you gently wash the lanolin off before breastfeeding again. Changing your bra pads often will help your nipples stay dry. And you should use only cotton bra pads.
- Worries about producing enough milk. A general rule of thumb is that a baby who's wetting six to eight diapers a day is most likely getting enough milk. It's best not to supplement your breast milk with formula, and never give your infant plain water. Your body needs the frequent, regular demand of your baby's nursing to keep producing milk. Some women mistakenly think they can't breastfeed if they have small breasts. But small-breasted women can make milk just as well as large-breasted women.
 Good nutrition, plenty of rest, and staying well hydrated all help, too.
Good nutrition, plenty of rest, and staying well hydrated all help, too. - Pumping and storing milk. You can get breast milk by hand or pump it with a breast pump. It may take a few days or weeks for your baby to get used to breast milk in a bottle. So begin practicing early if you're going back to work. Breast milk can be safely used within 2 days if it's stored in a refrigerator. You can freeze breast milk for up to 6 months. Don't warm up or thaw frozen breast milk in a microwave. That will destroy some of its immune-boosting qualities, and it can cause fatty portions of the breast milk to become super hot. Thaw breast milk in the refrigerator or in a bowl of warm water instead.
- Inverted nipples. An inverted nipple doesn't poke forward when you pinch the areola, the dark skin around the nipple. A lactation consultant -- a specialist in breastfeeding education -- can give you tips that allow women with inverted nipples to breastfeed successfully.

- Breast engorgement. Breast fullness is natural and healthy. It happens as your breasts become full of milk, staying soft and pliable. But breast engorgement means the blood vessels in your breast have become congested. This traps fluid in your breasts and makes them feel hard, painful, and swollen. Alternate heat and cold, for instance using ice packs and hot showers, to relieve mild symptoms. It can also help to release your milk by hand or use a breast pump.
- Blocked ducts. A single sore spot on your breast, which may be red and hot, can signal a plugged milk duct. This can often be relieved by warm compresses and gentle massage over the area to release the blockage. More frequent nursing can also help.
- Breast infection (mastitis). This occasionally results when bacteria enter the breast, often through a cracked nipple after breastfeeding. If you have a sore area on your breast along with flu-like symptoms, fever, and fatigue, call your doctor.
 Antibiotics are usually needed to clear up a breast infection, but you can most likely continue to breastfeed while you have the infection and take antibiotics. To relieve breast tenderness, apply moist heat to the sore area four times a day for 15 to 20 minutes each time.
Antibiotics are usually needed to clear up a breast infection, but you can most likely continue to breastfeed while you have the infection and take antibiotics. To relieve breast tenderness, apply moist heat to the sore area four times a day for 15 to 20 minutes each time. - Stress. Being overly anxious or stressed can interfere with your let-down reflex. That's your body's natural release of milk into the milk ducts. It's triggered by hormones released when your baby nurses. It can also be triggered just by hearing your baby cry or thinking about your baby. Stay as relaxed and calm as possible before and during nursing -- it can help your milk let down and flow more easily. That, in turn, can help calm and relax your infant.
- Premature babies may not be able to breastfeed right away. In some cases, mothers can release breast milk and feed it through a bottle or feeding tube.
- Warning signs.
 Breastfeeding is a natural, healthy process. But call your doctor if:
Breastfeeding is a natural, healthy process. But call your doctor if:- Your breasts become unusually red, swollen, hard, or sore.
- You have an unusual discharge or bleeding from your nipples.
- You're concerned your baby isn't gaining weight or getting enough milk.
Where Can I Get Help With Breastfeeding?
Images of mothers breastfeeding their babies make it look simple -- but some women need some help and coaching. It can come from a nurse, doctor, family member, or friend, and it helps mothers get over possible bumps in the road.
Reach out to friends, family, and your doctor with any questions you may have. Most likely, the women in your life have had those same questions.
Breastfeeding on demand
You can often hear from a nursing mother: "I feed on demand, my baby requires a breast every 3.5 hours." Or: “I have always fed on demand. In a year, we already had 1 feeding in the evening, and my child calmly refused to breastfeed.
Before talking about the demand of the child, it is necessary to find out what modern women mean when they say - "I breastfeed."
Modern mothers consider breastfeeding necessary for feeding their baby. Just for feeding. Breast milk is food, the mother supplies the baby with the nutrients necessary for growth and development. When a baby suckles at the breast, he eats. Breastfeeding makes sense only as a process of supplying proteins, fats, carbohydrates, vitamins and microelements.
During suckling, the baby receives the nutrients it needs with mother's milk. This is the absolute truth. There is another unconditional truth, which is not given any importance in modern society, it is not taken into account and is not considered. Breastfeeding for a child is communication with the mother. We need to figure out how the child understands feeding on demand? Can he understand anything at all? Is there any difference for him how he is fed, for 15-20 minutes after 3. 5 hours or in some other way?
5 hours or in some other way?
What is on-demand feeding
On-demand feeding of a newborn baby means putting it to the breast for every squeak or search. Squeak and search movements in newborns, even as early as the second or third day of life, begin to appear much more often than after 3.5 or 2.5 hours. The need for attachments increases rapidly, and by the 10-12th day of life, the need to attach to a child may occur 15-16 or more times a day. Applications vary in duration. The baby can fall asleep and sleep while sucking for, for example, 1.5-2 hours. Can release the breast after 1-2 minutes. And then ask her again. Why does a child need such frequent contact with his mother's breast?
That's why. Being in the mother's belly, in a calm, familiar environment, listening to the noises of the mother's body, being in a warm, cramped, confined space, the baby sucked his fist, fingers, loops of the umbilical cord, swallowed amniotic fluid. Learned to suck and swallow. After birth, experiencing discomfort for any, the most insignificant reason, the baby tries to get rid of it. You can get rid of discomfort by getting into the usual conditions of a comfortable stay. The only place where the baby after birth can feel the sensations familiar to him is in the arms of the mother. The only familiar action is sucking. The only familiar taste and smell is the taste and smell of milk and lube in the areola. Milk and lubricant have an odor and taste similar to the taste and smell of amniotic fluid. Therefore, experiencing discomfort, the baby squeaks, or begins to look for an object to suck with his mouth. Ideally, it is immediately applied to the chest. The baby becomes warm, cramped, he hears the beating of his mother's heart, breathing, grumbling in the intestines, he sucks and feels the familiar taste and smell. If such an action happens constantly, the baby gains confidence, no matter what happens, he will solve all his problems with his mother. The place of comfort is now under the breast, and you can suck on the breast.
After birth, experiencing discomfort for any, the most insignificant reason, the baby tries to get rid of it. You can get rid of discomfort by getting into the usual conditions of a comfortable stay. The only place where the baby after birth can feel the sensations familiar to him is in the arms of the mother. The only familiar action is sucking. The only familiar taste and smell is the taste and smell of milk and lube in the areola. Milk and lubricant have an odor and taste similar to the taste and smell of amniotic fluid. Therefore, experiencing discomfort, the baby squeaks, or begins to look for an object to suck with his mouth. Ideally, it is immediately applied to the chest. The baby becomes warm, cramped, he hears the beating of his mother's heart, breathing, grumbling in the intestines, he sucks and feels the familiar taste and smell. If such an action happens constantly, the baby gains confidence, no matter what happens, he will solve all his problems with his mother. The place of comfort is now under the breast, and you can suck on the breast.
This whole process is biologically justified. A newborn child does not feel the feeling of hunger, this feeling is not formed in him. It will begin to form at about two months of age. How to feed a creature that does not experience hunger ?! How to encourage him to take some action to get food? This can be done only at the expense of some other incentives. This stimulus for the newborn is constant bodily discomfort, thanks to which he wants to suckle all the time! The most intense, frequent and prolonged sucking in infants is observed in the first two or three months of life. It is in these first months that the main weight gain of the baby occurs.
Feeding in the first month
Baby falls asleep with breast in mouth, sleeps sucking for a while. Falling asleep deeply, lets go of the chest. After sleeping for a while, he wakes up, and is applied on waking. After sleep, he can stay awake for some time, for example, an hour and a half. During wakefulness, he may feel discomfort 2-3 times, for example, from a completely natural desire to pee, and having called his mother for help, having kissed for a couple of minutes, he will do his deeds. Then he will want to sleep, feel discomfort and, kissing his chest, will again fall asleep sucking. After some time, he will wake up and attach again. Then again a little "walk". And after some time, he will fall asleep at the chest again.
Then he will want to sleep, feel discomfort and, kissing his chest, will again fall asleep sucking. After some time, he will wake up and attach again. Then again a little "walk". And after some time, he will fall asleep at the chest again.
The daytime naps of a one-month-old infant feeding on demand vary in duration and number. There can be 4-6 dreams during the day, and they can last from 5-15 minutes to 2-2.5 sometimes 3 hours. "Around" each dream, the baby is applied to the chest, and applied between dreams several times. At night, the child falls asleep at the breast. Usually in the early morning hours, he begins to fuss and apply. In the morning, he almost never fully wakes up. The baby sleeps, from time to time, sucking on his mother's breast. Waking up in the morning, the baby is again applied to the chest. If you count all the attachments that have happened in a baby of one month of age, then approximately 16-20 attachments are obtained. This is how a newborn human cub behaves if it is given the opportunity to behave in accordance with physiological and psychological needs, which, by the way, are genetically determined. The child of the first months of life does not separate his personality from the personality of the mother and from her breast. Mom and her breasts, and everything connected with them, are the universe of the baby and himself.
The child of the first months of life does not separate his personality from the personality of the mother and from her breast. Mom and her breasts, and everything connected with them, are the universe of the baby and himself.
In most cases, a modern woman, being afraid to “accustom a child to hands”, strives to limit his requests for sucking. A pacifier and a bottle of tea or water come to her aid in this matter. They, too, can be sucked ... The need for sucking seems to be satisfied. But only the need for communication with the mother during suckling is not satisfied, the peculiar chain of mutual assistance and cooperation between mother and baby is destroyed, the formation of maternal affection and concentration is disrupted. Is the difference in the two actions noticeable to the reader: the baby cried, the mother took him, put him to her chest and started rocking him, or gave him a pacifier and started rocking the stroller, even with the words “Why are you crying, my sun?”
The modern woman who gives a pacifier and pumps a stroller is not a bad person deliberately harming an infant. She is simply in captivity of prejudices regarding the relationship between mother and baby. She does not know how to behave correctly, does not know what to do in accordance with the natural needs of the child. If you tell her what the child really needs, she will exclaim in horror: “What is it, don’t let him get away with?!” Indeed, the child of the first months of life must not be let off the hook. For a woman who does not know how to comfortably carry a baby, and who does not know how to feed him in various positions (sitting, lying, standing and even moving), this can be very difficult. Especially if she is not sure of the correctness of her actions.
She is simply in captivity of prejudices regarding the relationship between mother and baby. She does not know how to behave correctly, does not know what to do in accordance with the natural needs of the child. If you tell her what the child really needs, she will exclaim in horror: “What is it, don’t let him get away with?!” Indeed, the child of the first months of life must not be let off the hook. For a woman who does not know how to comfortably carry a baby, and who does not know how to feed him in various positions (sitting, lying, standing and even moving), this can be very difficult. Especially if she is not sure of the correctness of her actions.
An action that should become automatic for the mother of a newborn: when the baby cries or shows other signs of anxiety, put the baby to the breast.
What's next?
The baby is growing. A fairly stable rhythm of daytime sleep begins to form in him, and a 3-4-month-old baby behaves quite differently from a newborn. Feeding on demand at this age looks something like this...
Feeding on demand at this age looks something like this...
- At three months, the baby has 10-12 feeds during the day and 2-4 at night. There are frequent applications for a short time, but their number is reduced. There may be a long night break in feedings, about 5 hours, but this is very rare. Much more often the night break is 2.5-3.5 hours. By this age, the baby's body is noticeably rounded.
- At four months, the baby begins to breastfeed noticeably less frequently. The main feedings are associated with sleep: the baby suckles before bedtime, during awakening and during sleep, both daytime and nighttime. In this regard, he has a fairly accurate feeding regimen. And many babies stop breastfeeding when they wake up after daytime sleep, sometimes as early as 2.5-3 months.
- At five months, the baby has 8-10 daytime feedings and 2-3 nighttime, attachments as well as in the fourth month of life, are organized around dreams - the baby eats when going to bed and some babies suck during awakening.

- At six months, the feeding regimen changes. The most active sucking shifts to the last 2-3 hours before waking up from a night's sleep. The period of daytime wakefulness can be divided into two periods: in the morning, when the baby sucked during the night is rarely applied to the breast, and in the evening, when attachments become very frequent. In total, there can be 7-10 day applications and 3-4 night applications. At this age, the baby begins a period of acquaintance with new food - pedagogical complementary foods. Sometimes there are attachments associated with the introduction of complementary foods, the baby “washes down” samples of new food with mother's milk. But many children do not want to drink complementary foods. When complementary foods are introduced to an on-demand baby, it is never meant to replace feedings with complementary foods. This is practically impossible, because the main feedings of the baby are associated with sleep, and mother's breakfasts, lunches and dinners, during which the baby gets acquainted with new food, are located between the baby's dreams, during his wakefulness.

- At seven months, the frequency of application is about the same.
- At eight months, the feeding regimen changes. Since the baby shows high motor activity and is very busy exploring the surrounding space, in the daytime he forgets to breastfeed. In this regard, the number of daily feedings can be reduced to 6-8 times. The baby compensates for the reduction in daytime feedings by increasing the frequency and duration of nighttime feedings up to 6 times.
- In the second half of the year, babies who stopped breastfeeding when waking up after daytime naps recall this habit again. The baby’s daytime sleep in the second half of life, as well as in the region of a year and older, looks something like this: the baby falls asleep sucking, sleeps quietly for a while, for example 1-1.5 hours, then starts tossing and turning, fiddling, worrying, at this moment the mother lies down next to , gives him a breast and the baby can fill up 10-15-30 minutes sucking. Mom may well use this time for her own rest - lie down, read, while the baby sleeps while sucking.
 I know my mother, a lover of embroidery, who used this time specifically for embroidery ...
I know my mother, a lover of embroidery, who used this time specifically for embroidery ... - Breastfeeding becomes more frequent at nine to ten months. In the daytime, this is 4-6 full feedings and about the same number of attachments for various reasons. The baby has new reasons for attachment. If, during active actions to master the world, the baby fills a bump or gets scared, he calms down with his mother's breast. There may be situations when you can comfort the baby by sitting next to him and hugging him. At night, 4-6 feedings remain, the baby begins to suckle more actively in the morning between 3 and 8 hours.
- At eleven months, a baby can already have 2-3 complete complementary foods. Initiation to adult food in the mind of a child is not associated with breastfeeding: attachment to the mother's breast is something other than the desire to get enough of the product they like. As a rule, after the baby has eaten, he feels the need to attach himself to the breast.
 The number of daily feedings remains the same in the child, but the number of short-term attachments increases. There are active mid-morning feedings between 4 and 8 o'clock in the morning.
The number of daily feedings remains the same in the child, but the number of short-term attachments increases. There are active mid-morning feedings between 4 and 8 o'clock in the morning. - At ten or twelve months, the baby, if he is already walking, can sometimes breastfeed every time he comes to his mother, i.e. about every 15-30 minutes. Attachments around dreams and night sucking persist. Therefore, if a mother says that a child suckles once or twice a day, this means that there is no feeding at the request of the child. There are restrictions imposed by the mother, with which the baby has come to terms. He treats breast sucking like food, sucks on a pacifier or a finger to fall asleep or soothe, or falls asleep just like that, without calming down.
- At twelve months, the baby is applied in about the same way.
- At the age of one and a half years, there may already be one daytime nap, so there are fewer attachments associated with sleep. Preserved for morning sucking.
 The baby is very free with his mother's breasts. Sometimes it happens that he comes up to suck just for fun. For example, like this: he comes up, climbs on his knees, looks into his mother’s face, smiles, starts to swarm in his shirt, gets breasts, smiles at his breasts, sucks for 30 seconds and leaves.
The baby is very free with his mother's breasts. Sometimes it happens that he comes up to suck just for fun. For example, like this: he comes up, climbs on his knees, looks into his mother’s face, smiles, starts to swarm in his shirt, gets breasts, smiles at his breasts, sucks for 30 seconds and leaves.
As for the number of feedings per day when feeding a child on demand, their number is almost never less than 12. A newborn has 12 or more attachments, mostly they are all associated with dreams. And a child, say 1.5-2 years old, can also have about 12 attachments, only 3-4 are associated with sleep, and the rest are short-term attachments for various reasons. I suggest to all mothers reading this text - do not count the application, do not notice their duration. Breastfeed your baby as often as he asks, when you feel the need to.
Moms who don't think about breastfeeding without looking at the clock may get the impression that when breastfeeding on demand, the mother can do nothing but feed the baby. This is not true. After the birth of a baby, a mother begins another life, she is called life with a baby. That's all. The child is with the mother, not the mother with the child! Feel the difference! You need to be able to organize your life in a different way, in the first months, of course, the help of loved ones is very necessary. In the tradition of many peoples, it was customary for the first 40 days after childbirth to remove a woman from any housework and household chores, she was engaged only in a child. In some nations, objects that the mother of a newborn touched were considered “unclean”, therefore, they preferred to protect the mother from the rest of the household, allocating her a separate “corner” of the house, where no one bothered her and she did not interfere with anyone. Among the Slavs, such a restrictive custom was called a six-week. By 1.5-2 months, the rhythm of daytime dreams begins to form, and the baby has a kind of “regime”, the mother becomes more free.
This is not true. After the birth of a baby, a mother begins another life, she is called life with a baby. That's all. The child is with the mother, not the mother with the child! Feel the difference! You need to be able to organize your life in a different way, in the first months, of course, the help of loved ones is very necessary. In the tradition of many peoples, it was customary for the first 40 days after childbirth to remove a woman from any housework and household chores, she was engaged only in a child. In some nations, objects that the mother of a newborn touched were considered “unclean”, therefore, they preferred to protect the mother from the rest of the household, allocating her a separate “corner” of the house, where no one bothered her and she did not interfere with anyone. Among the Slavs, such a restrictive custom was called a six-week. By 1.5-2 months, the rhythm of daytime dreams begins to form, and the baby has a kind of “regime”, the mother becomes more free.
For a mother who can't imagine breastfeeding without looking back at the clock, and who is sure that the “right” baby is the baby lying quietly in her crib all the time, feeding on demand will be a complete hassle. It will be much easier for such a mother if she stops looking at the clock and ties the baby to herself with a large scarf or uses a patchwork holder (sling). It will become easier for her if she stops running between the nursery and the kitchen, but takes the baby with her to the kitchen and carries him around the house with her, doing housework, in a box, a cradle, a special chair, if she tries not to put him off often, and pick up as soon as possible, postponing the baby only in case of emergency and not for long.
It will be much easier for such a mother if she stops looking at the clock and ties the baby to herself with a large scarf or uses a patchwork holder (sling). It will become easier for her if she stops running between the nursery and the kitchen, but takes the baby with her to the kitchen and carries him around the house with her, doing housework, in a box, a cradle, a special chair, if she tries not to put him off often, and pick up as soon as possible, postponing the baby only in case of emergency and not for long.
Breastfeeding is not the same as house arrest. In the conditions of modern society, it is possible to organize the exit of a nursing mother to work from about 6 months of age of the baby. If necessary, you can start working from the age of 4 months, but, of course, it is better not every day of the week and not full time. It is the responsibility of a breastfeeding consultant to help a mother organize her return to work.
Sometimes, when I advise mothers on breastfeeding, I suggest that they forget for a second that they are already living in the 21st century. I propose to return, for example, to the cave and ask what they will do if the child woke up at night, how to calm him down? If you are walking through the forest and trying not to attract the attention of predators, how to make the baby silent? If the child is thirsty, what will you give him? What is the baby used to, for thousands of years of its existence? To the fact that he sleeps on his mother while she wanders through the forest with a digging stick in search of roots, and wakes up when mother stops. Since mom stopped, then there is time to wake up and suck. Therefore, even now the child sleeps well, tied to the mother with a patchwork holder, wakes up when the mother, having done a few household chores, sits in a chair to take care of the baby.
I propose to return, for example, to the cave and ask what they will do if the child woke up at night, how to calm him down? If you are walking through the forest and trying not to attract the attention of predators, how to make the baby silent? If the child is thirsty, what will you give him? What is the baby used to, for thousands of years of its existence? To the fact that he sleeps on his mother while she wanders through the forest with a digging stick in search of roots, and wakes up when mother stops. Since mom stopped, then there is time to wake up and suck. Therefore, even now the child sleeps well, tied to the mother with a patchwork holder, wakes up when the mother, having done a few household chores, sits in a chair to take care of the baby.
Some mother, reading about the cave, will be offended, saying that she is a civilized creature. But please think. Man, mother's breast and mother's milk have been created by evolution over millions of years. They are made for each other. Baby food has created progress and more recently. The skills of motherhood and breastfeeding have also been lost by our society quite recently. A person is not physiologically adapted to artificial feeding and a pacifier. The mother's breast will not produce enough milk at 6-7 feedings per day. Nature did not know, when creating man as a mammal, that the time would come when the need for breastfeeding would be satisfied by some kind of pacifiers and nipples.
Changes that occur during the formation of the personality of a child who did not have full contact with the mother during prolonged breastfeeding are noted by modern research by psychologists and sociologists. These are changes with a minus sign. It would be better if they were not, these changes.
Breastfeeding is important not only for the baby, it is also important for the mother. During on-demand feeding, the woman's feelings change, a stronger attachment to the baby is formed, the woman becomes more sensitive to the needs of the baby. Deeper affection and understanding are not only preserved in infancy. They persist for life. For clarity, imagine what happens to a woman’s feelings if she tries to “withstand” a child, endures his crying, anxiety. What happens to a woman if she uses the recommendation from one very popular parenting book: "Go to the child if he cries for more than 15 minutes"? Speaking in abstract terms, humanity is interested in reviving the practice of breastfeeding. The revival of this practice is impossible without mothers realizing the true reasons for the child's need for attachment to the breast.
Lilia Kazakova, pediatrician,
Head of Breastfeeding and Child Care Counselors
Breastfeeding the newborn | What to Expect in the First Week
The first week of a baby's life is a wonderful but hectic time, especially if you haven't breastfed before. Our breastfeeding tips will help you settle in as quickly as possible
Share this information
The first time after childbirth, mothers are often confused. The body is still recovering, and you are already starting to get to know your newborn baby. The emotional state during this period can be unstable, especially between the second and fifth day, when many women have milk 1 and at the same time postpartum depression begins 2 . In addition, people around often expect (and demand) that a woman come to her senses as soon as possible and become a “super mom”. But the best thing to do this first week is just to be with your baby and get breastfeeding going.
When should I start breastfeeding my newborn?
Try to breastfeed your baby within the first hour after birth. When the baby latch onto the breast and begins sucking rhythmically, it stimulates the mammary gland cells and starts milk production. 1 No wonder this time is called the "magic hour"!
“Ideally, the baby should be placed on the mother's stomach immediately after birth, so that it can immediately attach to the breast. He won't necessarily eat, but he should be able to,” explains Cathy Garbin, an internationally recognized expert on breastfeeding.
“Hold your baby and let him find the breast on his own and put the nipple in his mouth. This is called the breast-seeking reflex. On the Internet you can watch videos that show what this process looks like. If the baby does not latch onto the nipple on its own, the midwife will help to properly attach it to the breast. But for starters, it’s good to give the baby the opportunity to do it on their own. In this case, the optimal position for the mother is reclining. ”
Don't spend that special first hour of your baby's life weighing and swaddling—or at least wait until he's suckling for the first time. Enjoy hugs and close skin-to-skin contact. This promotes the production of oxytocin, the hormone of love, in you and your baby, and oxytocin plays a key role in the supply of the first breast milk - colostrum. 3
“As soon as the obstetricians were convinced that our son was healthy, the three of us — me, my husband and our baby — were left to give us the opportunity to get to know each other. It was a very special hour - an hour of awkwardness, turbulent emotions and bliss. During this time, I breastfed my son twice, ”recalls Ellie, a mother of two from the UK.
Did you know that breastfeeding helps to recover after childbirth? This is because oxytocin stimulates uterine contractions. In the first hours after childbirth, this contributes to the natural release of the placenta and reduces blood loss. 4
What to do if the birth did not go according to plan?
If you had a caesarean section or other complications during childbirth,
You can still establish skin-to-skin contact with your baby and breastfeed him in the first hours after birth.
“If you can't hold your baby, have your partner do it for you and ensure skin-to-skin contact with the baby. This will give the baby a sense of security, care and warmth so that he can hold on until you recover, ”Katie advises.
If the baby is unable to breastfeed, it is advisable to start expressing milk as early as possible and do so as often as possible until the baby is able to feed on its own. “While breastfeeding in the first hours after birth lays an excellent foundation for the future, it is not so important,” Cathy reassures. “It is much more important to start lactation so that in the future, if necessary, you can start breastfeeding.”
To start milk production, you can express milk manually or use a breast pump, which can be given to you at the hospital. 5 And the precious colostrum can be fed to the baby. This is especially important if the baby was born premature or weak, since breast milk is extremely healthy.
If a baby is born prematurely or has a medical condition and cannot be breastfed immediately, this is no reason not to continue breastfeeding. “I have worked with many new mothers who were unable to breastfeed their baby for the first six weeks due to preterm labor or other reasons. Nevertheless, all of them later successfully switched to breastfeeding,” says Kathy.
Does the baby latch on correctly?
Correct breastfeeding is essential for successful breastfeeding 6 , because it determines how effectively the baby will suckle milk, and therefore grow and develop. Latching on the breast incorrectly can cause sore or damaged nipples, so don't hesitate to ask your doctor to check that your baby is properly attached to the breast, even if you are told that everything is fine and you do not see obvious problems - especially while you are in the hospital.
“While I was in the hospital, I called the doctor at every feed and asked me to check if I was breastfeeding correctly,” says Emma, mother of two from Australia. - There were several cases when it seemed to me that everything seemed to be right, but it was painful to feed, and the doctor helped me take the baby off the breast and attach it correctly. By the time I was discharged, I had already learned to do it confidently.”
When applying to the breast, point the nipple towards the palate. This will allow the baby to take the nipple and part of the areola under it into their mouth. It will be easier for him to suck if he has both the nipple and part of the areola around in his mouth. 6
“When a baby latch on properly, it doesn't cause discomfort and it causes a pulling sensation, not pain,” Cathy explains. - The baby's mouth is wide open, the lower lip may be slightly turned outward, and the upper one lies comfortably on the chest. The body language of the child indicates that he is comfortable. There isn't much milk at this early stage, so you probably won't notice your baby swallowing, but he will suckle a lot and nurse frequently."
How often should a newborn be fed?
The frequency and duration of breastfeeding in the first week can vary greatly. “The first 24 hours of life are completely different for different children. Someone sleeps a lot (after all, childbirth is tiring!), And someone often eats, says Katie. - Such a variety greatly confuses young mothers. Everyone gives different advice, so it's important to remember that every mother and child is different."
“Colostrum is thicker than mature breast milk and produced in smaller quantities, but it provides many benefits. When the baby eats colostrum, he learns to suck, swallow and breathe until milk begins to flow in more volume, ”explains Cathy.
Milk usually arrives on the second or fourth day after delivery. Until this time, the baby is applied to the breast 8-12 times a day (and sometimes more often!), including at night. 7 Feeding may last 10-15 minutes at this stage, or 45 minutes or even an hour, as the baby is just beginning to develop the muscles and coordination needed to suckle effectively.
“At first, the intensity of feeding is very high, often higher than many people realize, and this is shocking to most new mothers,” says Cathy. - Sometimes mom has no time to go to the toilet, take a shower and have a snack. It usually comes as a surprise."
Camille, a mother from Australia, experienced this. “The first week, Frankie ate every two hours, day and night, and each time it took half an hour to an hour to feed,” she recalls. “My husband and I were completely exhausted!”
Do I need to feed my newborn on a schedule?
The good news is that frequent feeding promotes lactation and stimulates milk production. 7 The more your baby eats, the more milk you will have. Therefore, forget about feeding your newborn on a schedule - this way he will have less chance of feeding. Try to feed your baby when he signals that he is hungry 8 :
- tossing and turning in his sleep;
- opens eyes;
- turns his head if he feels a touch on his cheek;
- sticks out tongue;
- groans;
- licks lips;
- sucks fingers;
- is naughty;
- whimpers;
- is crying.
Crying is the last sign of hunger, so if in doubt, just offer your baby the breast. If he bursts into tears, it will be more difficult to feed him, especially at first, when both of you are just learning how to do it. As your baby grows, he will likely eat less frequently and take less time to feed, so breastfeeding will seem more predictable.
Does breastfeeding hurt?
You may have heard that breastfeeding is not painful at all, but in fact, in the first days, many new mothers experience discomfort. And this is not at all surprising, given that the nipples are not used to such frequent and strong sucking.
“Breastfeeding can be uncomfortable for the first couple of days – your body and your baby are just getting used to it. If a baby eats too long and does not latch well, the sensations are almost the same as from unworn new shoes, Cathy compares. Just as tight shoes can rub your feet, improper suckling can damage your nipples. Prevention is always better than cure, so if the pain persists after a few days of feeding, contact a lactation consultant or healthcare professional.”
Maria, a mother from Canada, agrees: “Although my son seemed to latch onto the breast well, he damaged his nipples while feeding, and I was in pain. As it turned out, the reason was a shortened frenulum of the tongue. The breastfeeding specialists at our city clinic have been of great help in diagnosis and treatment.”
In addition, you may experience period-like cramps in the early days after breastfeeding, especially if this is not your first baby. This is the so-called postpartum pain. The fact is that oxytocin, which is released during breastfeeding, contributes to further contraction of the uterus to restore its normal size. 4
When milk arrives, the breasts usually become fuller, firmer and larger than before delivery. In some women, the breasts swell, harden and become very sensitive - swelling of the mammary glands occurs. 10 Frequent breastfeeding relieves these symptoms. For more breast care tips, read our article What is Breast Swelling?
How often does the newborn urinate and defecate?
What goes into the body must go back out. Colostrum
has a laxative effect, helping to eliminate meconium - the original feces. It looks a little scary - black and sticky, like tar. 11 But don't worry, it won't always be like this. Breastfed babies usually have a slightly sweet smell of stool.
How many times a day you will need to change diapers and what the contents should look like, see below.
Day one
- Frequency: once or more.
- Colour: greenish black.
- Texture: sticky like tar.
Second day
- Frequency: twice or more.
- Colour: dark greenish brown.
- Texture: less sticky.
Day three
- Frequency: twice or more.
- Colour: greenish brown to brownish yellow.
- Texture: non-sticky.
Fourth day and then the entire first month
- Frequency: twice or more.
- Color: yellow (feces should turn yellow no later than the end of the fourth day).
- Texture: grainy (like mustard with grains interspersed). Leaky and watery.
The baby's urine should be light yellow. On average, babies urinate once a day for the first two days. Starting around the third day, the number of wet diapers increases to three, and from the fifth day onwards, diapers have to be changed five times a day or more often. In addition, during the first few days, the weight of wet diapers increases. 11
Is the baby getting enough breast milk?
Since very little milk is produced at first,
You may feel that your baby is not getting enough milk. But if you feed your baby on demand, you will produce exactly as much milk as he needs. If you want to keep the process under control, be guided by the frequency of diaper changes given above. If your baby soils less diapers, check with your doctor.
“For the first three or four weeks, most babies just eat and sleep. If the child is worried and constantly asks for a breast, you should consult with your doctor, ”recommends Katie.
Sometimes the baby may vomit after feeding. If the vomit is the color of milk, this is not a cause for concern. But if there are orange, red, green, brown or black blotches in it, or the child vomits with a "fountain", consult a doctor. A doctor should also be consulted if the baby has a high temperature, the fontanel (soft spot on the head) has sunk, blood is found in the feces, and also if the weight recorded at birth has not recovered within two weeks. 11
But if there are no frightening symptoms and the baby is growing at a normal pace, then he has enough milk. Soon you will both get used to breastfeeding and establish a more stable routine.
For the next step in breastfeeding, see Breastfeeding in the First Month: What to Expect.
Literature
1 Pang WW, Hartmann PE. Initiation of human lactation: secretory differentiation and secretory activation. J9 Mammary Gland Biol Neoplasia . 2007;12(4):211-221. - Pang, W.W., Hartmann, P.I., "Lactation initiation in the lactating mother: secretory differentiation and secretory activation." G Mammary Gland Biol Neoplasia. 2007;12(4):211-221.
2 Shashi R et al. Postpartum psychiatric disorders: Early diagnosis and management. Indian J Psychiatry . 2015; 57( Suppl 2): S 216– S 221. - Shashi R. et al., Postnatal mental disorders: early diagnosis and treatment. Indian J Saikiatri. 2015; 57(App 2):S216-S221.
3 Moberg KU, Prime DK. Oxytocin effects in mothers and infants during breastfeeding. Infant . 2013;9(6):201-206. - Moberg K, Prime DK, "The effects of oxytocin on mother and child during breastfeeding." Infant. 2013;9(6):201-206.
4 Sobhy SI, Mohame NA. The effect of early initiation of breast feeding on the amount of vaginal blood loss during the fourth stage of labor. J Egypt Public Health Assoc . 2004;79(1-2):1-12. - Sobhi SI, Moham NA, "Early initiation of breastfeeding and its effect on vaginal bleeding in the fourth stage of labor." G Egyptian Public Health Assoc. 2004;79(1-2):1-2.
5 Meier PP et al. Which breast pump for which mother: an evidence-based approach to individualizing breast pump technology. J Perinatol . 2016;36(7):493. - Meyer P.P. et al., Breastpump Selection: A Scientific Approach to Customizing Pumping Technology. J Perinatol (Journal of Perinatology). 2016;36(7):493-499.
6 Cadwell K. Latching - On and Suckling of the Healthy Term Neonate: Breastfeeding Assessment. J Midwifery & Women s 2007;52(6):638-642. — Cadwell, K., "Latching and sucking in healthy newborns: evaluation of breastfeeding." F Midwifery Women Health. 2007;52(6):638-642.
7 Kent JC et al. Principles for maintaining or increasing breast milk production. 2012;41(1):114-121. - Kent J.S. et al., "Principles for Maintaining and Increasing Milk Production". J Obstet Ginecol Neoneutal Nurs. 2012;41(1):114-121.
8 Australian Breastfeeding Association [ Internet ].