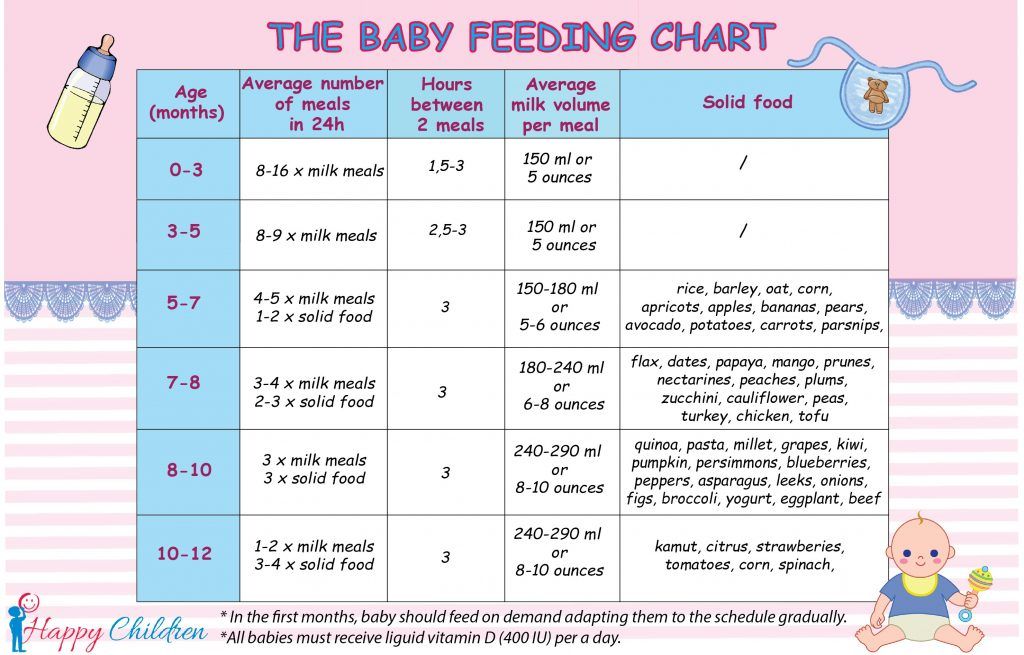
Newborn baby after feeding
Burping Your Baby (for Parents)
Reviewed by: Madhu Desiraju, MD
Primary Care Pediatrics at Nemours Children's Health
en español Hacer eructar a su bebé
An important part of feeding a baby is burping. Burping helps to get rid of some of the air that babies tend to swallow during feeding. Not being burped often and swallowing too much air can make a baby spit up, or seem cranky or gassy.
How to Burp Your Baby
When burping your baby, repeated gentle patting on your baby's back should do the trick. Cup your hand while patting — this is gentler on the baby than a flat palm.
To prevent messy cleanups when your baby spits up or has a "wet burp," you might want to place a towel or bib under your baby's chin or on your shoulder.
Try different positions for burping that are comfortable for you and your baby. Many parents use one of these three methods:
- Sit upright and hold your baby against your chest. Your baby's chin should rest on your shoulder as you support the baby with one hand.
With the other hand, gently pat your baby's back. Sitting in a rocking chair and gently rocking with your baby while you do this may also help.
- Hold your baby sitting up, in your lap or across your knee. Support your baby's chest and head with one hand by cradling your baby's chin in the palm of your hand. Rest the heel of your hand on your baby's chest, but be careful to grip your baby's chin, not the throat. Use the other hand to pat your baby's back.
- Lay your baby on your lap on his or her belly. Support your baby's head and make sure it's higher than their chest. Gently pat your baby's back.
If your baby seems fussy while feeding, stop the session, burp your baby, and then begin feeding again. Try burping your baby every 2 to 3 ounces (60 to 90 milliliters) if you bottle-feed and each time you switch breasts if you breastfeed.
Try burping your baby every ounce during bottle-feeding or every 5 minutes during breastfeeding if your baby:
- tends to be gassy
- spits a lot
- has gastroesophageal reflux (GER)
- seems fussy during feeding
If your baby doesn't burp after a few minutes, change the baby's position and try burping for another few minutes before feeding again. Always burp your baby when feeding time is over.
Always burp your baby when feeding time is over.
To help prevent the milk from coming back up, keep your baby upright after feeding for 10 to 15 minutes, or longer if your baby spits up or has GERD. But don't worry if your baby spits sometimes. It's probably more unpleasant for you than it is for your baby.
Sometimes your baby may awaken because of gas. Picking your little one up to burp might put them back to sleep. As your baby gets older, don't worry if your child doesn't burp during or after every feeding. Usually, it means that your baby has learned to eat without swallowing too much air.
Babies with colic (3 or more hours a day of continued crying) might have gas from swallowing too much air during crying spells, which can make the baby even more uncomfortable. Check with your pediatrician before giving your baby anti-gas drops.
Reviewed by: Madhu Desiraju, MD
Date reviewed: June 2022
Feeding Your Newborn (for Parents)
How you feed your newborn is the first nutrition decision you make for your child.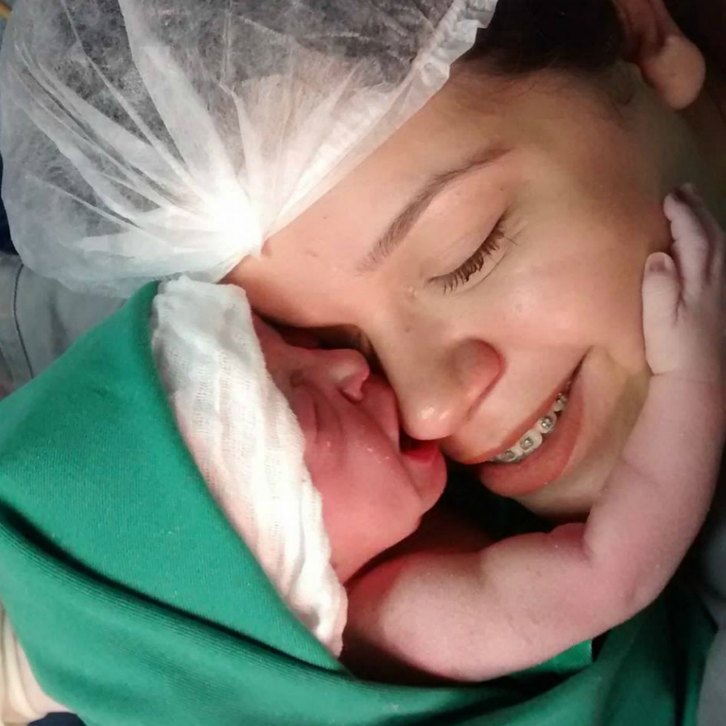 These guidelines on breastfeeding and bottle feeding can help you know what's right for you and your baby.
These guidelines on breastfeeding and bottle feeding can help you know what's right for you and your baby.
Breast or Bottle?
The American Academy of Pediatrics (AAP) recommends that babies be breastfed exclusively for about the first 6 months. After they start on solid foods, babies should breastfeed through the first year of life and even beyond, if desired.
But breastfeeding isn't possible or preferable for all new moms. Deciding to breastfeed or bottle feed a baby is usually based on the mother's comfort level with breastfeeding and her lifestyle. In some cases, breastfeeding may not be recommended for a mom and her baby. If you have any questions about whether to breastfeed or formula feed, talk to your pediatrician.
Remember, your baby's nutritional and emotional needs will be met whether you choose to breastfeed or formula feed.
Benefits of Breastfeeding
Breastfeeding your newborn has many benefits. Perhaps most important, breast milk is the perfect food for a baby's digestive system. It has the nutrients that a newborn needs, and it’s easily digested. Commercial formulas try to imitate breast milk, and come close, but can't match it exactly.
It has the nutrients that a newborn needs, and it’s easily digested. Commercial formulas try to imitate breast milk, and come close, but can't match it exactly.
Breast milk has
antibodiesthat help protect babies from many infections, including diarrhea and ear and lung infections. Breastfed babies are less likely to develop medical problems such as diabetes, high cholesterol, asthma, and allergies. Breastfeeding also might make a child less likely to become overweight.
Breastfeeding is great for moms too. It burns calories, so can help nursing moms lose the weight gained during pregnancy. Breastfeeding also may offer protection from breast cancer and ovarian cancer.
Some moms find breastfeeding easier and quicker than formula feeding — it needs no preparation, and you don't run out of breast milk in the middle of the night. Also, breastfeeding costs little. Nursing mothers do need to eat more and may want to buy nursing bras and pads, a breast pump, or other equipment. But these expenses are generally less than the cost of formula.
But these expenses are generally less than the cost of formula.
Breastfeeding meets a variety of emotional needs for both moms and babies. The skin-to-skin contact can enhance the emotional connection, and providing complete nourishment can help new moms feel confident in their ability to care for their newborn.
Limitations of Breastfeeding
With all the good things known about breastfeeding, why doesn't every mother choose to breastfeed?
Breastfeeding requires a big commitment from a mother. Some new moms feel tied down by the demands of a nursing newborn. Because breast milk is easily digested, breastfed babies tend to eat more often than babies who are fed formula. This means moms can be in demand as often as every 2 or 3 hours in the first few weeks. This can be tiring, but it's not long before babies feed less often and sleep longer at night.
Some new mothers need to get back to work outside the home or separate from their babies from time to time for other reasons.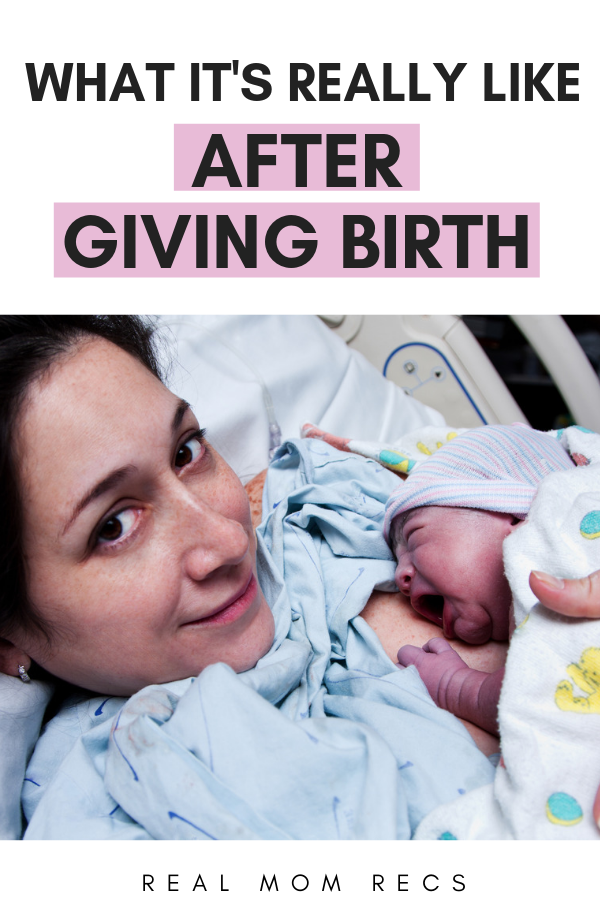 Some opt for formula feeding so other caregivers can give the baby a bottle. Mothers who want to continue breastfeeding can use a breast pump to collect breast milk to be given in a bottle, so their babies still get its benefits even when mom isn't there to breastfeed.
Some opt for formula feeding so other caregivers can give the baby a bottle. Mothers who want to continue breastfeeding can use a breast pump to collect breast milk to be given in a bottle, so their babies still get its benefits even when mom isn't there to breastfeed.
Fathers and other family members may want to share in feeding the baby. When mom is breastfeeding, dad or siblings may want to stay close by. Helping mom get comfortable, or providing a burp cloth when needed, will let them be part of the experience.
When breastfeeding is going well, other family members can help by giving the baby pumped breast milk in a bottle when mom needs a break.
Some moms may feel embarrassed or worried about breastfeeding. These feelings usually end after a successful breastfeeding process is set. It can help to get advice from those who've gone through the experience. Most hospitals and birthing centers offer in-depth instruction on breastfeeding to new moms. Your pediatrician, nurse practitioner, or nurse can answer questions or put you in touch with a lactation consultant or a breastfeeding support group.
In some cases, a mother's health may affect her ability to breastfeed. Moms getting chemotherapy for cancer and those who have HIV should not breastfeed, for example.
If you have a medical condition or take any medicines regularly, talk with your doctor about whether it's OK to breastfeed. If you have to stop nursing temporarily, continue to pump breast milk to maintain milk production. If you or your baby are sick, continue to breastfeed if you can. Talk to the doctor if you have any concerns.
In some situations, it may not possible to breastfeed, such as when a baby is very sick or born early. Mothers should talk with their baby's doctor about expressing and storing milk. Often, a baby who can't breastfeed can get breast milk through a feeding tube or bottle.
Some moms who have inverted nipples may have trouble breastfeeding, but a lactation consultant usually can help them overcome this. Likewise, women who have had plastic surgery on their breasts should be able to successfully breastfeed. Talk with your doctor if you have any concerns.
Talk with your doctor if you have any concerns.
Hold off on pacifiers or bottles until your baby has gotten used to and is good at breastfeeding. Lactation professionals recommend waiting until a baby is about 3–4 weeks old before offering artificial nipples of any kind (including pacifiers).
Benefits of Formula Feeding
Commercially prepared infant formula is a nutritious alternative to breast milk. Bottle feeding can offer more freedom and flexibility for moms, and make it easier to know how much the baby is getting.
Because babies digest formula more slowly than breast milk, a baby who is getting formula may need fewer feedings than one who breastfeeds. Formula feeding also can make it easier to feed the baby in public, and lets the father and other family members help feed the baby, which can enhance bonding.
Limitations of Formula Feeding
Just as breastfeeding has its unique demands, so does bottle feeding. Bottle feeding takes organization and preparation, especially if you want to take your baby out.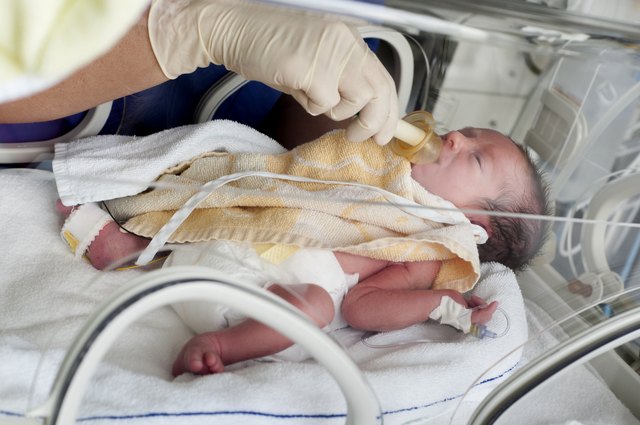 Store-bought formula can be pretty expensive, but do not try to make your own formula at home.
Store-bought formula can be pretty expensive, but do not try to make your own formula at home.
It's important to make sure that you have enough formula on hand, and bottles that are clean and ready to be used.
Here are a few guidelines for formula feeding:
- Carefully follow directions on the label when preparing formula. Do not add more water than directed.
- Bottles left out of the refrigerator longer than 1 hour and any formula left in the bottle that a baby doesn't finish should be discarded.
- Prepared bottles of formula can be stored in the refrigerator up to 24 hours and carefully warmed just before feeding. You don't have to warm formula, but most babies prefer it.
- A bottle of formula can be warmed by holding it in running warm water or setting it in a pan of warm water. A bottle of formula (or breast milk) should never be warmed in a microwave. The bottle can heat unevenly and leave "hot spots" that can burn a baby's mouth.

How Often Do Newborns Eat?
Your newborn will nurse about 8 to 12 times per day during the first weeks of life. In the beginning, mothers may want to try nursing 10–15 minutes on each breast, then adjust the time as needed.
Breastfeeding should be on demand (when your baby is hungry), which is generally every 1–3 hours. As newborns get older, they'll nurse less often and have longer stretches between feedings. Newborn babies who are getting formula will likely take about 2–3 ounces every 2–4 hours. Newborns should not go more than about 4–5 hours without feeding.
Signs that babies are hungry include:
- moving their heads from side to side
- opening their mouths
- sticking out their tongues
- placing their hands and fists to their mouths
- puckering their lips as if to suck
- nuzzling against their mothers' breasts
- crying
A feeding schedule is not necessary — you and your baby will get into a routine. Babies know (and will let their parents know) when they're hungry and when they've had enough. Watch for signs that your baby is full (slowing down, spitting out the bottle or unlatching from breast, closing the mouth, turning away from the breast or bottle) and stop the feeding when these signs appear.
Babies know (and will let their parents know) when they're hungry and when they've had enough. Watch for signs that your baby is full (slowing down, spitting out the bottle or unlatching from breast, closing the mouth, turning away from the breast or bottle) and stop the feeding when these signs appear.
As babies grow, they begin to eat more at each feeding and can go longer between feedings. There may be other times when your infant seems hungrier than usual. Continue to nurse or feed on demand. Nursing mothers need not worry — breastfeeding stimulates milk production, and your supply of breast milk will adjust to your baby's demand for it.
Is My Newborn Getting Enough to Eat?
New parents often worry about whether their babies are getting enough to eat.
Babies are getting enough to eat if they:
- seem satisfied
- have about 6–8 wet diapers a day
- have regular bowel movements (poops)
- sleep well
- are alert when awake
- are gaining weight
A baby who is fussing, crying, seems hungry, does not appear satisfied after feeding, and has fewer wet diapers may not be getting enough to eat. If you're concerned that your baby isn't getting enough to eat, call your doctor.
If you're concerned that your baby isn't getting enough to eat, call your doctor.
Most infants "spit up" a small amount after eating or during burping, but a baby should not vomit after feeding. Vomiting after every feeding might be a sign of an allergy, digestive problem, or other problem that needs medical care. If you have concerns that your baby is spitting up too much, call your doctor.
Should Newborns Get Nutritional Supplements?
Breast milk has the right combination of vitamins and easily absorbed iron for newborns. A healthy infant being nursed by a healthy mother doesn't need extra vitamins or nutritional supplements, with the exception of vitamin D. Breastfed babies should begin vitamin D supplements within the first few days of life, continuing until they get enough vitamin D-fortified formula or milk (after 1 year of age).
Breastfeeding mothers who follow vegetarian diets that do not include animal products need vitamin B12 supplements.
Iron-fortified formula has the right blend of vitamins and minerals for a baby, so supplements usually aren't needed.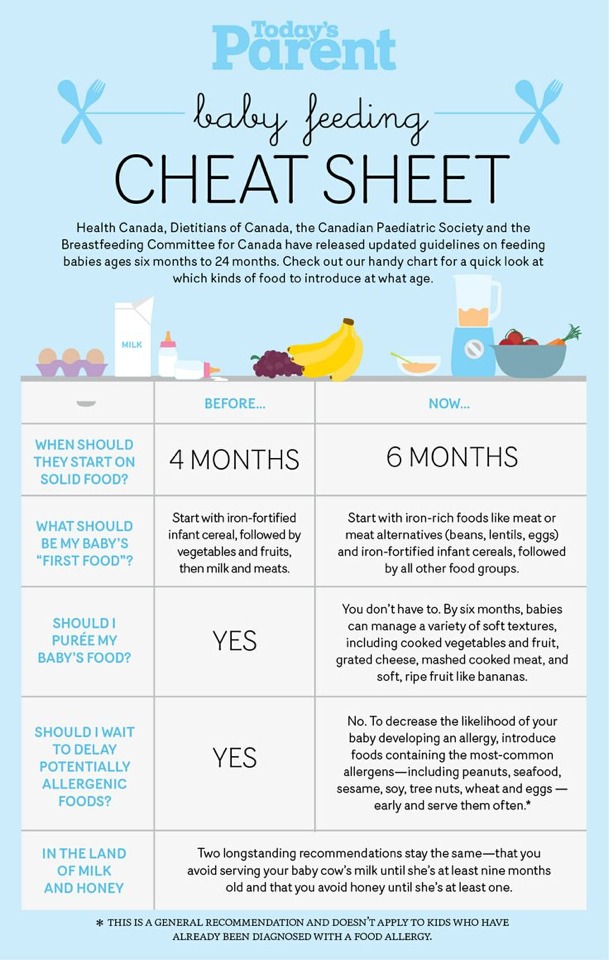 Infants drinking less than 1 liter, or about a quart, of formula a day may need a vitamin D supplement.
Infants drinking less than 1 liter, or about a quart, of formula a day may need a vitamin D supplement.
Water, juice, and other foods usually aren't necessary during a baby's first 6 months. Breast milk and formula provide everything babies need nutritionally until they start eating solid foods. Talk to your doctor if you have any questions about feeding your newborn.
Reviewed by: Mary L. Gavin, MD
Date reviewed: February 2021
How to help the baby when regulating
Support icon ofKeywords for searching
Home ›!! How to help a child in sprinkling
Home Home ›!! How to help a child in regurgitation
↑ Verki
Breastal feeding - completely special time for mom and her newborn baby. Together with the feeling of closeness and affection that feeding brings, understanding its nuances cannot but raise many questions, including the question of how to help an infant spit up. Regurgitation in a newborn is by no means always the result of a simple pat on his back.
In this article, we'll talk about the basics of helping a newborn spit up, as well as other questions you may have about spitting up.
Why do babies spit up?
Let's get it straight: why do newborns need to burp in the first place? During feeding, children usually swallow extra air - this is called aerophagia. Spitting up helps prevent this air from entering the intestines, as well as vomiting, gas, and crankiness in the baby. To avoid the return of milk after feeding, you should give the baby the opportunity to burp more often.
How to help a newborn spit up?
During the first six months, the baby should be kept upright in a column for 10-15 minutes after each feed. This will help keep the milk in his stomach, but if the baby occasionally burps anyway, parents need not worry. While carrying your baby in an upright position, you can put a baby diaper or wipes on your shoulder to keep your clothes clean.
We've already seen why spitting up is important, now let's find out how to help your baby spit up. Parents should gently pat the baby on the back with a hand folded in a handful until he burps. Folding your hand into a handful is important because clapping with a flat palm may be too strong for an infant.
Every baby is different and there is no one right position for spitting up. To get started, you can try the following options:
- Sitting position with the baby on the chest. In this position, the parent puts the baby's head with his chin on his shoulder and with one hand supports the baby under the back. With the other hand, you can gently pat the baby on the back. This method is most effective in a rocking chair or when the baby is gently rocking.
- Holding the child upright on your legs. With one hand, parents can hold the baby by the back and head, supporting his chin and placing his palm on the baby’s chest, with the other hand, you can gently pat him on the back.
 At the same time, it is important to be careful: do not press the child on the throat, but only gently support his chin.
At the same time, it is important to be careful: do not press the child on the throat, but only gently support his chin. - Holding a baby on your lap while lying on your tummy. Make sure his head is above his chest and gently pat your baby on the back until he burps.
Here are some tips on how best to help your newborn spit up:
- Let your baby spit up during feeding. If the baby is restless or has swallowed air, it is worth giving him the opportunity to burp during feeding, and not just after.
- When bottle feeding, let the newborn burp after every 50-60 ml.
- When breastfeeding, let the baby burp at every breast change.
It is important to let your baby spit up after eating, even if he spit up during feeding!
If your baby is gassy, spit up more often. Also, if he vomits frequently or suffers from gastroesophageal reflux disease (GERD), have him spit up after every 30 ml bottle-feeding or every five minutes while breastfeeding.
How long should a baby be held for it to burp? It's different for everyone, but generally keeping a newborn upright for 15 to 20 minutes after a feed helps the milk stay in the baby's stomach.
Minimize the amount of air you swallow. Gas production and regurgitation result from aerophagia during feeding. The baby will inevitably swallow air, but there are ways to prevent it from swallowing too much. Whether you bottle feed your baby or combine breastfeeding with bottle feeding, the Philips Avent anti-colic bottle with AirFree valve is designed so that the nipple is always filled with milk without excess air, even in a horizontal position, thus preventing the baby from swallowing excess air during feeding.
Reducing the amount of air your baby swallows can help reduce your baby's risk of colic, gas, and spitting up.
Breastfeeding is a wonderful time to strengthen the bond between parent and baby. Every mom and every baby is different, so learning to help your newborn burp properly can take time and practice.
Articles and tips from Philips Avent
Baby+ app
Download the app and track your child's development and growth with trackers, and keep those special moments forever.
Download app:
You are leaving the Philips Healthcare (“Philips”) official website. Any links to third party websites that may be included on this site are provided solely as a convenience to you. Philips makes no warranties regarding any third party websites or the information they contain.
I understand
You are about to visit a Philips global content page
Continue
You are about to visit the Philips USA website.
I understand
Infant Reflux: Symptoms and Treatment
Search Support IconSearch Keywords
Home ›› What is Reflux in Infants?
Home ›› What is reflux in babies?
↑ Top
Signs and what to do
Post-feed spitting up is common in the first few months of life. This is usually harmless and completely normal, but parents should read about gastroesophageal reflux (GER) and laryngopharyngeal reflux (LPR) in infants and how long it lasts to give them peace of mind.
This is usually harmless and completely normal, but parents should read about gastroesophageal reflux (GER) and laryngopharyngeal reflux (LPR) in infants and how long it lasts to give them peace of mind.
We look at signs of reflux in babies, symptoms of different types of reflux, and how to help a child with signs of reflux. If you require further information, always contact your healthcare provider.
What is reflux in babies?
So we know reflux is common, but what causes reflux in babies? Because young children have not yet fully developed the lower esophageal sphincter (LES), that is, the muscle at the bottom of the esophagus that opens and closes to let food into the stomach and keep it there, food can easily pass back up the esophagus.
Acid reflux, also known as gastroesophageal reflux (GER), is a normal reflux that occurs in babies. This type of reflux is considered normal and occurs in 40-65% of babies.
How do I know if my child has acid (gastroesophageal) reflux?
If a baby is spitting up milk after a feed, it is most likely acid reflux. As babies get older, GER usually goes away on its own without any intervention. If a baby has complications beyond just spitting up a small amount of milk (such as feeding difficulties and discomfort), they may have gastroesophageal reflux disease (GERD).
As babies get older, GER usually goes away on its own without any intervention. If a baby has complications beyond just spitting up a small amount of milk (such as feeding difficulties and discomfort), they may have gastroesophageal reflux disease (GERD).
Symptoms of GERD include:
- baby arching during or after feeding;
- crying more than three hours a day for no apparent reason;
- cough;
- gag reflex or difficulty swallowing;
- irritability, restlessness after eating;
- eating little or not eating;
- poor weight gain or loss;
- difficult breathing;
- severe or frequent vomiting.
GERD usually occurs when the muscle tone of the LES muscles fails in time, causing stomach contents to back up into the esophagus.
How do I know if my child has Laryngopharyngeal Reflux?
Another type of reflux, laryngopharyngeal reflux (LPR), also called silent reflux, is when the contents of a child's stomach leak back into the larynx, the back of the nasopharynx. This type of reflux does not always cause external symptoms, which is why it is called "silent". Babies can have GERD and silent reflux at the same time, but their symptoms are somewhat different.
This type of reflux does not always cause external symptoms, which is why it is called "silent". Babies can have GERD and silent reflux at the same time, but their symptoms are somewhat different.
The following are some of the symptoms of laryngopharyngeal reflux:
- trouble breathing;
- gag reflex;
- chronic cough;
- swallowing problems;
- hoarseness;
- regurgitation;
- poor weight gain or weight loss.
We have looked at the signs of reflux in infants, now we will move on to the treatment and duration of silent reflux in children, as well as the treatment of GERD.
How to deal with laryngopharyngeal reflux in babies while breastfeeding?
Breastfeeding mothers may need to review their diet if their babies show signs of reflux. The American Academy of Pediatrics (AAP) recommends breastfeeding mothers cut eggs and milk from their diet for two to four weeks to see if their baby's reflux symptoms improve or disappear. It may be worth eliminating acidic foods from your diet.
It may be worth eliminating acidic foods from your diet.
In most cases, GER and laryngopharyngeal reflux go away on their own. Typically, children outgrow reflux in the first year of life. If a child has persistent symptoms of laryngopharyngeal reflux, parents should consult a doctor. If your baby has severe vomiting, blood in the stool, or any of the symptoms of GERD listed above, parents should contact their pediatrician as soon as possible.
How can I help my child with reflux or GERD?
Reflux symptoms in babies usually go away on their own, but the following tips can help relieve symptoms:
- Thicken your food with rice or a special milk thickener.
- Hold the bottle at an angle that fills the nipple completely with milk to reduce the amount of air your baby swallows. This can help prevent colic, gas, and reflux.
- Try the AirFree anti-colic bottle, designed to reduce air swallowing during feeding.

4. Let your baby burp during and after feeding. If the baby is bottle fed, parents can let him burp after every 30-60 ml. If the mother is breastfeeding, she may let the baby burp when changing breasts.
5. Hold baby upright after feeding. As a rule, in order for the milk to remain in the stomach, after feeding the baby, it is necessary to hold it in an upright position for 10-15 minutes. But, if the child has reflux, parents should keep him upright a little longer.
These tips may help relieve symptoms, but they do not replace a doctor's advice.
Parents should not change their infant formula without first talking to their doctor.
Don't panic! Reflux is very common in babies during the first three months of life, and most babies outgrow it without any consequences. Although GERD is a slightly more serious condition, there are many treatments, ways to manage it, and help newborns. Feel free to contact your doctor with any questions or concerns you may have.