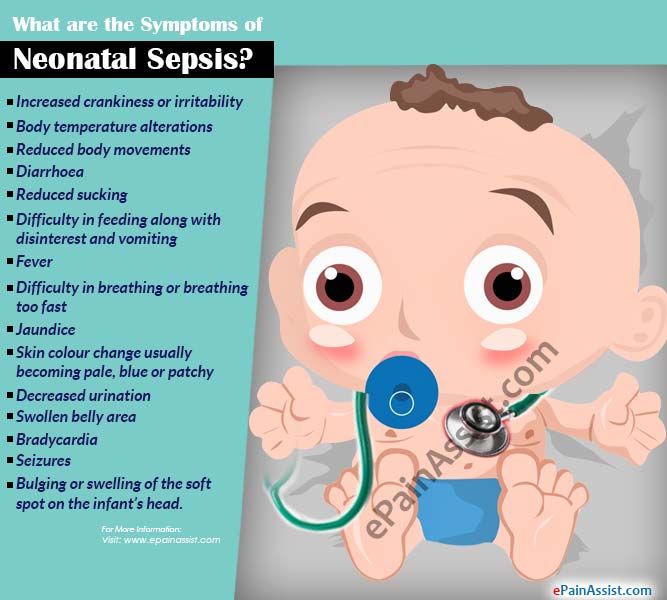
What to feed babies when they are vomiting
Vomiting in children and babies
It's normal for babies and children to vomit occasionally. In most cases, it will last no longer than one to two days and isn't a sign of anything serious.
The most common cause of vomiting in children and babies is gastroenteritis. This is an infection of the gut usually caused by a virus or bacteria, which also causes diarrhoea. The symptoms can be unpleasant but your child will usually start to feel better after a few days.
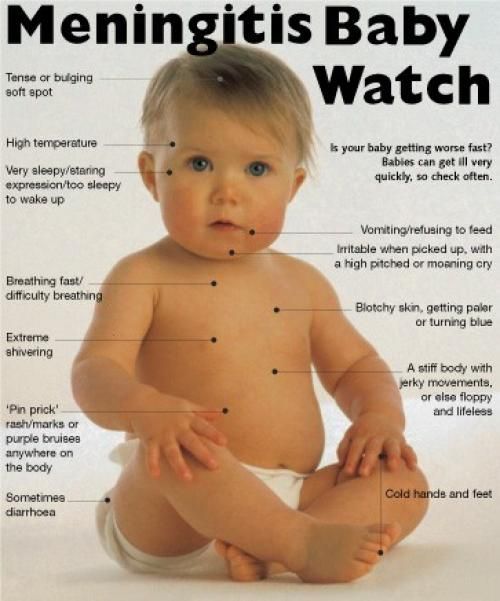
However, persistent vomiting can sometimes cause your child to become severely dehydrated and occasionally it can be a sign of something more serious, such as meningitis.
This page outlines what to do if your child keeps vomiting and describes some of the common causes of vomiting in children and babies.
If your child has a high temperature, you can also read a separate page about fever in children.
What to do
If your child vomits, you should keep a close eye on them. Trust your instincts and contact your GP immediately if you're worried.
If the cause is just a tummy bug, your child should still be feeling well enough to eat, play and be their usual self. In this case, keep feeding them as normal and offer them regular drinks (see below).
But if they don't seem themself – for example, if they're floppy, irritable or less responsive – they may be seriously ill, so you should get medical help immediately.
When to get medical advice
You should contact your GP if:
- your child is repeatedly vomiting and is unable to hold down fluids
- you think they're dehydrated – symptoms of dehydration can include a dry mouth, crying without producing tears, urinating less or not wetting many nappies, and drowsiness
- their vomit is green or contains blood
- they have been vomiting for more than a day or two
Go to your nearest accident and emergency (A&E) department if your child is vomiting and develops sudden and severe tummy pain, or they're floppy, irritable or less responsive
Call 999 for an ambulance or go to your nearest A&E department immediately if they're vomiting and have a headache, stiff neck and a rash.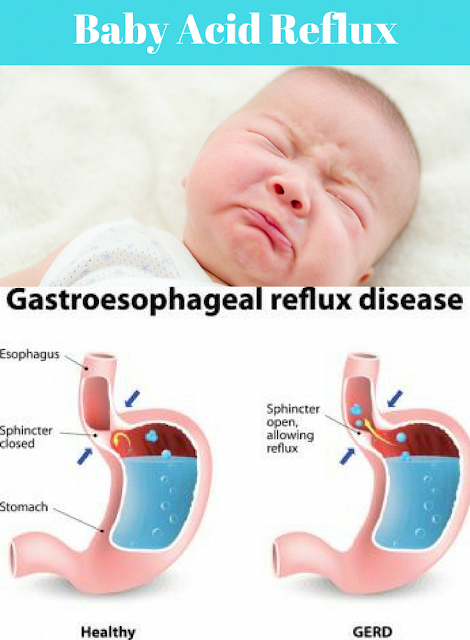
Looking after your child at home
In most cases, you can treat your child safely at home. The most important thing you can do is make sure they keep drinking fluids to prevent dehydration.
If your baby is vomiting, carry on breastfeeding or giving them milk feeds. If they seem dehydrated, they will need extra fluids. Ask your GP or pharmacist whether you should give your baby oral rehydration solution.
Oral rehydration solution is a special powder that you make into a drink. It contains sugar and salts to help replace the water and salts lost through vomiting and diarrhoea.
Children who are vomiting should keep taking small sips of clear fluid, such as water or clear broth. Fruit juice and fizzy drinks should be avoided until they're feeling better. If they're not dehydrated and haven't lost their appetite, it's fine for your child to eat solid foods as normal.
Again, speak to your GP or pharmacist if you're concerned about dehydration. They may recommend an oral rehydration solution for your child. Contact your GP or practice nurse if your child is unable to hold down oral rehydration solution.
Contact your GP or practice nurse if your child is unable to hold down oral rehydration solution.
If your child has diarrhoea and is vomiting, they shouldn't go to school or any other childcare facility until 48 hours after the last episode of diarrhoea or vomiting.
Read more about treating gastroenteritis in children.
Causes of vomiting in children
There are a number of possible causes of vomiting in children, which are described below.
Gastroenteritis
Gastroenteritis is an infection of the gut. It's a common cause of vomiting in children and usually lasts a few days.
Food allergy
Food allergies can cause vomiting in children, as well as other symptoms, such as a raised, red, itchy skin rash (urticaria) and swelling of the face, around the eyes, lips, tongue or the roof of the mouth.
Watch out for foods that may bring on vomiting and see your GP for a diagnosis if you think your child may have a food allergy.
Other infections
Vomiting can sometimes be a sign of an infection other than gastroenteritis, such as urinary tract infections (UTIs), middle ear infections, pneumonia or meningitis.
Contact your child's GP if they're vomiting and experiencing additional symptoms of an infection, such as a high temperature (fever) and irritability.
Appendicitis
Appendicitis is a painful swelling of the appendix, a finger-like pouch connected to the large intestine. It causes severe tummy pain that gets worse over time.
If your child has tummy pain that's gradually getting worse, contact your GP, or if they aren't open call NHS 24's 111 service immediately. You should call 999 for an ambulance if they have pain that gets worse quickly and spreads across their tummy.
In most cases of appendicitis, the appendix will need to be surgically removed as soon as possible.
Poison
Accidentally swallowing something poisonous can cause your child to vomit. If you think this is the case, contact your GP immediately or take your child to your nearest accident and emergency (A&E) department.
Causes of vomiting in babies
These include:
- gastroenteritis
- a food allergy or milk intolerance
- gastro-oesophageal reflux – where stomach contents escape back up the gullet
- too big a hole in the bottle teat, which causes your baby to swallow too much milk
- accidentally swallowing something poisonous
- congenital pyloric stenosis – a condition present at birth where the passage from the stomach to the bowel has narrowed, so food is unable to pass through easily; this causes projectile vomiting
- a strangulated hernia – your baby will vomit frequently and cry as if they are in a lot of pain; this should be treated as a medical emergency
- intussusception (where the bowel telescopes in on itself) – as well as vomiting, your baby may look pale, floppy and have symptoms of dehydration
Vomiting (0-12 Months)
Is this your child's symptom?
- Vomiting (throwing up) stomach contents
- Other names for vomiting are puking, barfing and heaving
Causes of Vomiting
- Viral Gastritis.
 Stomach infection from a stomach virus is the most common cause. Also called stomach flu. A common cause is the Rotavirus. The illness starts with vomiting. Watery loose stools may follow within 12-24 hours.
Stomach infection from a stomach virus is the most common cause. Also called stomach flu. A common cause is the Rotavirus. The illness starts with vomiting. Watery loose stools may follow within 12-24 hours. - Food Allergy. Vomiting can be the only symptom of a food reaction. The vomiting comes on quickly after eating the food. Uncommon in infants, but main foods are eggs and peanut butter.
- Coughing. Hard coughing can also cause your child to throw up. This is more common in children with reflux.
- Serious Causes. Vomiting alone should stop within about 24 hours. If it lasts over 24 hours, you must think about more serious causes. An example is a kidney infection. A serious cause in young babies is pyloric stenosis. See below for more on this.
Pyloric Stenosis (Serious Cause)
- The most common cause of true vomiting in young babies.
- Onset of vomiting is age 2 weeks to 2 months
- Vomiting is forceful.
 It becomes projectile and shoots out.
It becomes projectile and shoots out. - Right after vomiting, the baby is hungry and wants to feed. ("hungry vomiter")
- Cause: The pylorus is the channel between the stomach and the gut. In these babies, it becomes narrow and tight.
- Risk: Weight loss or dehydration
- Treatment: Cured by surgery.
Vomiting Scale
- Mild: 1 - 2 times/day
- Moderate: 3 - 7 times/day
- Severe: Vomits everything, nearly everything or 8 or more times/day
- Severity relates even more to how long the vomiting goes on for. At the start of the illness, it's common for a child to vomit everything. This can last for 3 or 4 hours. Children then often become stable and change to mild vomiting.
- The main risk of vomiting is dehydration. Dehydration means the body has lost too much fluid.
- The younger the child, the greater the risk for dehydration.
Dehydration: How to Tell
- The main risk of vomiting is dehydration. Dehydration means the body has lost too much water.
- Vomiting with watery diarrhea is the most common cause of dehydration.
- Dehydration is a reason to see a doctor right away.
- Your child may have dehydration if not drinking much fluid and:
- The urine is dark yellow and has not passed any in over 8 hours.
- Inside of the mouth and tongue are very dry.
- No tears if your child cries.
- Slow blood refill test: Longer than 2 seconds. First, press on the thumbnail and make it pale. Then let go. Count the seconds it takes for the nail to turn pink again. Ask your doctor to teach you how to do this test.
When to Call for Vomiting (0-12 Months)
Call 911 Now
- Can't wake up
- Not moving
- You think your child has a life-threatening emergency
Call Doctor or Seek Care Now
- Dehydration suspected.
 No urine in over 8 hours, dark urine, very dry mouth and no tears.
No urine in over 8 hours, dark urine, very dry mouth and no tears. - Stomach pain when not vomiting. Exception: stomach pain or crying just before vomiting is quite common.
- Age less than 12 weeks old with vomiting 2 or more times. Exception: normal spitting up.
- Vomited 3 or more times and also has diarrhea
- Severe vomiting (vomits everything) more than 8 hours while getting Pedialyte (or breastmilk)
- Head injury within the last 24 hours
- Weak immune system. Examples are sickle cell disease, HIV, cancer, organ transplant, taking oral steroids.
- Vomiting a prescription medicine
- Fever over 104° F (40° C)
- Fever in baby less than 12 weeks old. Caution: Do NOT give your baby any fever medicine before being seen.
- Your child looks or acts very sick
- You think your child needs to be seen, and the problem is urgent
Contact Doctor Within 24 Hours
- All other infants (age less than 1 year) with vomiting.
 See Care Advice while waiting to discuss with doctor.
See Care Advice while waiting to discuss with doctor.
Seattle Children's Urgent Care Locations
If your child’s illness or injury is life-threatening, call 911.
- Bellevue
- Everett
- Federal Way
- Seattle
Care Advice for Vomiting
- What You Should Know About Vomiting:
- Most vomiting is caused by a viral infection of the stomach.
- Vomiting is the body's way of protecting the lower gut.
- The good news is that stomach illnesses last only a short time.
- The main risk of vomiting is dehydration. Dehydration means the body has lost too much fluid.
- Here is some care advice that should help.
- Formula Fed Babies - May Give Oral Rehydration Solution (ORS) for 8 Hours:
- If vomits once, give half the regular amount of formula every 1 to 2 hours.
- If vomits formula more than once, offer ORS for 8 hours. If you don't have ORS, use formula until you can get some.
- ORS is a special fluid that can help your child stay hydrated. You can use Pedialyte or the store brand of ORS. It can be bought in food stores or drug stores.
- Spoon or syringe feed small amounts. Give 1-2 teaspoons (5-10 mL) every 5 minutes.
- After 4 hours without throwing up, double the amount.
- Return to Formula. After 8 hours without throwing up, go back to regular formula.
- Breastfed Babies - Reduce the Amount Per Feeding:
- If vomits once, nurse half the regular time every 1 to 2 hours.

- If vomits more than once, nurse for 5 minutes every 30 to 60 minutes. After 4 hours without throwing up, return to regular nursing.
- If continues to vomit, switch to pumped breastmilk. (ORS is rarely needed in breastfed babies. It can be used if vomiting becomes worse).
- Spoon or syringe feed small amounts of pumped milk. Give 1-2 teaspoons (5-10 mL) every 5 minutes.
- After 4 hours without throwing up, return to regular feeding at the breast. Start with small feedings of 5 minutes every 30 minutes. As your baby keeps down the smaller amounts, slowly give more.
- If vomits once, nurse half the regular time every 1 to 2 hours.
- Pumped Breastmilk Bottle-Fed Infants - Reduce the Amount per Feeding:
- If vomits once and bottle-feeding breastmilk, give half the regular amount every 1-2 hours.
- If vomits more than once within last 2 hours, give 1 ounce (30 mL) every 30 to 60 minutes.
- If continues to vomit, give 1-2 teaspoons (5-10 mL) every 5 minutes. Only if not tolerating breastmilk, switch to ORS (e.
 g., Pedialyte) for every 5 minutes for a few hours.
g., Pedialyte) for every 5 minutes for a few hours. - After 4 hours without vomiting, return to regular feedings. Start with 1 ounce (30 mL) every 30 minutes and slowly increase as tolerated.
- Stop All Solid Foods:
- Avoid all solid foods and baby foods in kids who are vomiting.
- After 8 hours without throwing up, gradually add them back.
- If on solid foods, start with starchy foods that are easy to digest. Examples are cereals, crackers and bread.
- Do Not Give Medicines:
- Stop using any drug that is over-the-counter for 8 hours. Reason: Some of these can make vomiting worse.
- Fever. Mild fevers don't need to be treated with any drugs. For higher fevers, you can use an acetaminophen suppository (such as FeverAll). This is a form of the drug you put in the rectum (bottom). Ask a pharmacist for help finding this product. Do not use ibuprofen. It can upset the stomach.
- Call your doctor if: Your child vomits a drug ordered by your doctor.
- Try to Sleep:
- Help your child go to sleep for a few hours.
- Reason: Sleep often empties the stomach and removes the need to vomit.
- Your child doesn't have to drink anything if his stomach feels upset and he doesn't have any diarrhea.
- Return to Child Care:
- Your child can return to child care after the vomiting and fever are gone.
- What to Expect:
- For the first 3 or 4 hours, your child may vomit everything. Then the stomach settles down.
- Vomiting from a viral illness often stops in 12 to 24 hours.
- Mild vomiting and nausea may last up to 3 days.
- Call Your Doctor If:
- Vomits clear fluids for more than 8 hours
- Vomiting lasts more than 24 hours
- Blood or bile (green color) in the vomit
- Stomach ache present when not vomiting
- Dehydration suspected (no urine in over 8 hours, dark urine, very dry mouth, and no tears)
- You think your child needs to be seen
- Your child becomes worse
And remember, contact your doctor if your child develops any of the 'Call Your Doctor' symptoms.

Disclaimer: this health information is for educational purposes only. You, the reader, assume full responsibility for how you choose to use it.
Last Reviewed: 01/03/2023
Last Revised: 12/30/2022
Copyright 2000-2023 Schmitt Pediatric Guidelines LLC.
How to feed a child with vomiting: principles of gentle nutrition
During and after a child's vomiting, parents should review the diet. This condition disrupts the electrolyte balance, microflora, and causes dehydration. The body does not take food well - the rich taste and smell of the dish can provoke nausea, in addition, appetite often decreases. What to feed the baby?
Contents [ show ]
- Why children vomit
- What to do after vomiting and how to feed the child? nine0008
- Sample daily menu for a child older than one year
- What foods not to eat when vomiting
- Tips for parents when a baby vomits
- Drinking regimen for vomiting
Why children vomit
The following problems can provoke vomiting06 disease;

Vomiting accompanies diseases more serious than ordinary food poisoning: appendicitis, helminthiasis, kidney failure, intestinal obstruction. But in this case it is combined with other characteristic symptoms. nine0003
In addition, vomiting is a natural human reaction to feeding against will. Don't be surprised if you run into her when you try to feed your baby when he doesn't want to. This is not a whim of a child. So his body reacts to the excess portion size. Another situation in which vomiting can begin is exposure to a new, most often exotic food with an unusual smell, taste or texture.
What to do after vomiting and what to feed the baby?
In case of poisoning, the digestive organs begin to suffer. The mucous membranes become inflamed, nausea and diarrhea occur. The body loses a huge amount of water, dehydration occurs, which can lead to serious consequences. nine0003
First of all, you need to compensate for the lack of liquid - give weak, slightly sweet black tea, you can also green, dried fruit compotes, pharmacy (for example, Regidron) or a salt solution prepared by yourself.
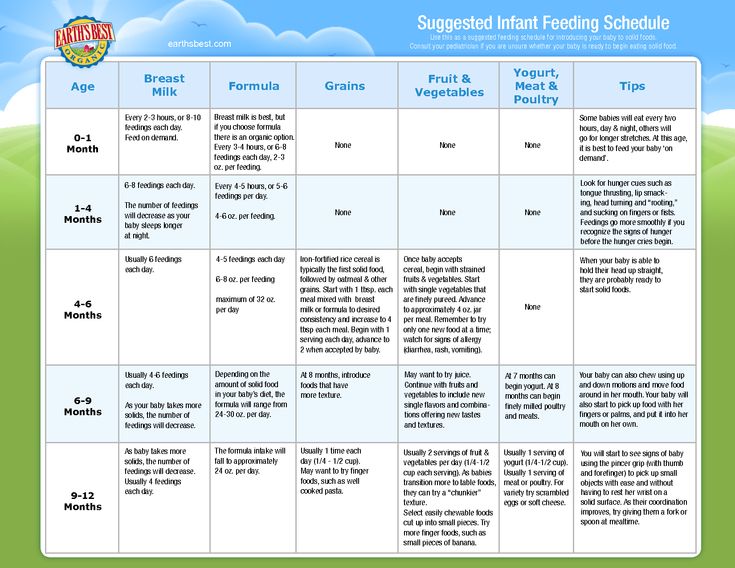
For newborns, follow the following feeding schedule :
- When breastfeeding: before the condition returns to normal, do not breastfeed the baby for at least 3-6 hours - this may provoke a new attack of vomiting. Drinking is allowed. When the vomiting has passed, you can return to the usual feeding pattern. nine0008
- When formula-feeding: with the approval of a pediatrician, stop feeding, give the newborn only water. When the condition normalizes, start offering the mixture at first in small portions, gradually returning to the usual ones.
If complementary foods have already been introduced, on the first day after vomiting, offer:
- first courses: chicken broth, rice soup, soups with broccoli or homemade noodles;
- biscuits;
- boiled round rice porridge (mucilaginous). nine0008
A day after the baby has been poisoned, second courses can also be included in the diet. Buckwheat or rice porridge will do. Cook them with water, formula, breast or cow's milk diluted with water.
Cook them with water, formula, breast or cow's milk diluted with water.
Gradually, as with the introduction of complementary foods, return to the menu the dishes familiar to the child in accordance with his age - meat soufflé, vegetable / fruit puree, fish, cottage cheese, eggs.
Older children (from 8-12 months) can include in the diet not very fatty fish, lean broth with chicken, boiled rice, and a baked apple will not harm. Introduce fruits later - they contain acids that can irritate the stomach lining already damaged by vomiting. Bananas, pears and apples are suitable, preferably boiled or baked, wait a while with sour berries and fruits. nine0003
Sample daily menu for a child older than one year old
If the child has already become familiar with the main complementary foods and almost switched to a common table, after vomiting, you can make the following menu for the day:
2. Oatmeal, buckwheat or rice porridge
3.
 Sweet tea with cookies
Sweet tea with cookies Lunch
2. Cooks prepared from white bread
222 9,
What foods not to eat when vomiting
The baby's diet during the recovery period after poisoning is not very diverse. Contraindicated:
- barley, barley, millet groats and all legumes;
- pasta;
- fatty meats, smoked meats, lard;
- raw vegetables (rich in fibre) and berries and fruits, except baked apples, bananas and pears;
- biscuits, cakes, soft white bread;
- candy, chocolate;
- fast food, carbonated drinks, chips.
 nine0008
nine0008
With a therapeutic diet, the child will receive all the important nutrients, relieve the gastrointestinal tract as much as possible. In addition, the correct diet after suffering vomiting contributes to the speedy recovery of the body.
Tips for parents in case of vomiting in a baby
By following simple rules, you will alleviate the child's condition and speed up recovery:
- Appetite can normalize after 3-5 days. At this time, the baby should be fed often, but in small portions. Breaks between meals - no more than 2-3 hours. This mode improves the regulation of the functions of the liver, pancreas, improves intestinal motility. nine0008
- It is important to reduce portions, especially on the first day, when all energy reserves are aimed at cleansing the body of toxins.
- Foods are best cooked, stewed, steamed, baked in the oven. Eliminate spices, marinades and sauces.
- Puree or grind food. In this embodiment, it is absorbed faster, which reduces the risk of a new attack of vomiting.

- No hot or cold food should be given, it should be warm.
- When dehydrated, it is important to drink more - often, but in small portions, literally in a sip. nine0008
- Separate power supply. When forming the menu, do not mix different products. Some of them are incompatible, they can be poorly absorbed if they are not combined correctly.
- Do not force feed. Even a 2-3-day sparing regimen, during which the child will eat at a minimum, will not cause health problems - curative fasting is practiced by official medicine.
Refusal to eat during vomiting is a defensive reaction of the body. He throws all his strength into the fight against infection or toxins, so do not interfere with him, but help him with light food and drinking regimen. nine0003
Drinking regimen for vomiting
Drinking regimen is a necessary component of the diet when the child has been poisoned . The body spends a huge amount of water during diarrhea and vomiting. You can compensate for the loss by drinking plenty of water.
You can compensate for the loss by drinking plenty of water.
It is ideal to drink 1-2 tablespoons of water every 10 minutes. It can be water, saline (ideally), but if the child agrees to drink, for example, only dried fruit compote, let him drink - it is important to make up for the loss of fluid at any cost. nine0003
Permitted drinking:
- still mineral water;
- weak, slightly sweet black/green tea;
- dried fruit compote, raisin decoction;
- ordinary purified or boiled water.
Do not drink freshly squeezed or store-bought juices, strong tea, carbonated drinks.
Be sure to consult a doctor! In case of severe vomiting and the inability to drink the baby, intravenous solutions are used to replenish fluid losses. nine0003
Vomiting and loose stools in a child
Ambulance for children: +7 (812) 327-13-13
In a child (especially in the first year of life), the digestive system is very sensitive not only to the quality of food and its compliance with age, but also to any drastic changes in diet. Naturally, having received something unacceptable or unusual, the body seeks to get rid of it as soon as possible, either by regurgitating the contents of the stomach through the mouth (vomiting), or by dramatically accelerating the passage of uncomfortable food through the intestines (diarrhea). However, nutritional errors, like food poisoning, are not actually the most common causes of vomiting and/or loose stools in children - most intestinal disorders in babies are associated with intestinal infections (bacterial or viral). nine0106 Of course, careful personal hygiene reduces the risk of intestinal infections, but there are no methods that guarantee 100% protection against them for your baby - the child lives in an unsterile world inhabited by pathogens, many of which can be transmitted not only by contact, but also by air - by drip. Therefore, it is not worth conducting an investigation to find out which of the family members infected the child - all claims are against the one who created the microbes.
Naturally, having received something unacceptable or unusual, the body seeks to get rid of it as soon as possible, either by regurgitating the contents of the stomach through the mouth (vomiting), or by dramatically accelerating the passage of uncomfortable food through the intestines (diarrhea). However, nutritional errors, like food poisoning, are not actually the most common causes of vomiting and/or loose stools in children - most intestinal disorders in babies are associated with intestinal infections (bacterial or viral). nine0106 Of course, careful personal hygiene reduces the risk of intestinal infections, but there are no methods that guarantee 100% protection against them for your baby - the child lives in an unsterile world inhabited by pathogens, many of which can be transmitted not only by contact, but also by air - by drip. Therefore, it is not worth conducting an investigation to find out which of the family members infected the child - all claims are against the one who created the microbes. nine0003
nine0003
In the event of vomiting and loose stools, a doctor's consultation is absolutely essential. This is especially true of vomiting - this symptom can be a sign of a number of serious diseases that have nothing to do with the gastrointestinal tract. If vomiting is combined with a headache or appeared after a head injury, call an ambulance without waiting for the visit of the local doctor. Save the last few stools until the doctor arrives by sealing the diaper or panties in a plastic bag - most likely the doctor will want to examine them. nine0106 Naturally, with vomiting and diarrhea, the main function of the digestive system, the absorption of nutrients, is disrupted. However, if a child’s body can tolerate a nutritional deficiency for quite a long time without serious consequences, then a lack of fluid and salt (the so-called dehydration or dehydration caused by vomiting or loose stools) can dramatically worsen the child’s condition and cause serious complications. Therefore, the first therapeutic measures for vomiting and diarrhea are hunger and drink. nine0003
nine0003
Hunger
If a doctor's visit is expected in the next few hours, the baby should not be fed until the doctor arrives. In the case where urgent medical advice is not possible, you should take a break in the diet for 6-8 hours (for infants, this means skipping one feeding). In the future, the child is fed fractionally (that is, often and little by little). Breastfed babies need to be fed after two hours, while reducing the feeding time. In children of the first year of life, complementary foods should be abandoned on the first day, limiting themselves to breast milk or its substitute. Older children can be offered crackers, biscuits, rice porridge on the water. The basic principle of nutrition in this case is better not to give than to give (if the child does not ask for food, you do not need to feed him at all). Further dietary recommendations are best obtained from your doctor - as already mentioned, with the problems described, a doctor's consultation is absolutely necessary. nine0003
nine0003
Drinking
It must also be fractional. A single volume of liquid for infants should not exceed 10-15 ml, for older children - 30-100 ml (large volumes, stretching the stomach wall, can provoke vomiting). It is necessary to water the child in 10-30 minutes (the smaller the one-time volume, the more often you should drink). The daily volume of fluid taken should not be less than the daily need of the child, taking into account the increased losses: for an infant, this is 800–1000 ml, for older children, up to two or three liters. Do not be afraid to overdose the liquid - here the principle is exactly the opposite: it is better to pass than not to give (meaning the daily volume, not a single serving). nine0106 Having dealt with the amount of liquid, it makes sense to discuss what should a child drink? The main drink may be water, weakly brewed tea, herbal teas (for example, chamomile or children's stomach tea). If the child is not accustomed to unsweetened drinks, it is better to use fructose for sweetening, since the sucrose contained in regular sugar activates the fermentation processes in the intestines.
However, such drinking is unable to compensate for the loss of salts (especially these losses are great with vomiting). Therefore, at least half of the daily volume of liquid should be represented by saline solutions. In this capacity, it is most convenient to use Regidron powders (they are sold at any pharmacy). The contents of the package are dissolved in one liter of water. In the absence of Regidron, you can prepare a similar solution yourself: 8 teaspoons of fructose or sugar and ⅔ teaspoon of salt per liter of water. It is also necessary to give the child saline solutions because even with a significant water deficit in the body, the baby will refuse to drink if the salt deficiency is even greater than the water deficit. nine0106 Note that in gastrointestinal disorders, the correction of water-salt disorders is the main therapeutic factor, much more important than the use of the most modern and effective drugs.
Medicines
And yet, what medicines can be given to a child with diarrhea and vomiting before the doctor arrives?
At the very beginning of the disease, enterosorbents may be useful - Polysorb, Zosterin-Ultra, Polypefan, Filtrum (it is very difficult to give the child favorite activated charcoal in an effective dose). It will also help to normalize Smekta's stool - three doses a day, children over two years old - a whole sachet, young children - one sachet per day for a year of life. Before use, a sachet of Smecta should be dissolved in 50 ml of boiled water (allowed - in milk mixtures). If diarrhea or vomiting is accompanied by an increase in temperature above 38 ºС, the temperature should be reduced, since at elevated temperatures fluid losses increase to humidify the exhaled air. nine0003
It will also help to normalize Smekta's stool - three doses a day, children over two years old - a whole sachet, young children - one sachet per day for a year of life. Before use, a sachet of Smecta should be dissolved in 50 ml of boiled water (allowed - in milk mixtures). If diarrhea or vomiting is accompanied by an increase in temperature above 38 ºС, the temperature should be reduced, since at elevated temperatures fluid losses increase to humidify the exhaled air. nine0003
WHAT NOT TO DO?
First of all, you should not try to wash your child's stomach - this violent event can only lead to additional loss of salts. In addition, after this unpleasant procedure, you are unlikely to be able to give the child a drink or give him the necessary medicine.
In no case should you also give your child antibiotics without a doctor's prescription. First, today antibiotics in the treatment of intestinal infections are not used so often. Secondly, they begin to act only on the second or third day of course use, so a few hours do not solve anything. nine0106 The widely advertised Imodium (synonyms - Lopedium, Loperamide) also cannot be used alone - the drug does not have a therapeutic effect on the disease that caused loose stools, it simply inhibits intestinal motility. In addition, age restrictions and possible side effects of this drug make it possible to use it in children only under the supervision of the attending physician.
nine0106 The widely advertised Imodium (synonyms - Lopedium, Loperamide) also cannot be used alone - the drug does not have a therapeutic effect on the disease that caused loose stools, it simply inhibits intestinal motility. In addition, age restrictions and possible side effects of this drug make it possible to use it in children only under the supervision of the attending physician.
Let me emphasize once again that in case of vomiting and (or) loose stools in a child, timely (that is, immediate) consultation with a doctor is absolutely necessary. Usually, the delay in going to the doctor is due to a banal reason - parents are simply afraid that the child will be “taken to the hospital”. With early treatment, these fears are completely unfounded - most cases of intestinal disorders in children proceed without any problems and can be treated at home. The need for hospitalization is more often associated not with the severe course of the disease itself (although this also happens), but with dehydration that has developed during unsuccessful attempts to cope with the disease on their own.











