Why is my baby sick after breast feeding
Reflux | Breastfeeding Challenges | Start for Life
Breastfeeding challenges
There may be times when breastfeeding is challenging. Never ignore any issues you may have – talk to your health visitor, midwife, GP or breastfeeding specialist as soon as possible, they will be able to help you sort it out quickly.
Here are some common breastfeeding issues, and tips on what to do.
- Colic
- Constipation
- Mastitis
- Milk supply
- Reflux
- Sore nipples
- Thrush
- Tongue-tie
Baby reflux
If your baby brings up milk, or is sick during or after feeding, this is known as reflux. Reflux, also called posseting or spitting up, is quite common and your baby should grow out of it, usually by the time they are 12 months old.
What causes baby reflux?
The muscle at the bottom of the food pipe acts as a kind of door into the stomach – so when food or milk travels down, the muscle opens allowing the food into the stomach.
However, while this muscle is still developing in the first year, it can open when it shouldn't (usually when your baby's tummy is full) allowing some food and stomach acid to travel back up again. Acid in the stomach is normal and a necessary part of the digestion process – it helps break down food.
In most babies, reflux is nothing to worry about as long as they are healthy and gaining weight as expected.
Baby reflux symptoms
- Constant or sudden crying when feeding.
- Bringing up milk during or after feeds (regularly).
- Frequent ear infections.
- Lots of hiccups or coughing.
- Refusing, gagging, or choking during feeds.
- Poor weight gain.
- Waking up at night a lot.
GORD
When reflux becomes painful and it happens frequently, this is known as 'gastro-oesophageal reflux disease' (GORD). GORD is more serious than mild, everyday reflux. The strong stomach acid can irritate and make the food pipe sore and inflamed, which is painful for your baby and may result in them needing medication.
The main signs and symptoms of GORD in your baby are:
- spitting up frequently
- abdominal pain
- feeding difficulties
- seeming unsettled and grizzly after a feed
These symptoms can lead to your baby not gaining weight, or even losing weight.
Silent reflux
Silent reflux can be confusing as there are no obvious signs or clues (such as spitting up). It's when the food travels back up the food pipe – but it's swallowed rather than spat out so is harder to identify. But your baby may display similar symptoms to those of regular reflux.
Breastfeeding Friend from Start for Life
The Breastfeeding Friend, a digital tool from Start for Life, has lots of useful information and expert advice to share with you – and because it's a digital tool, you can access it 24 / 7.
Breastfeeding tips for babies with reflux
- Feeding little and often (smaller feeds stop their tummy getting too full).
- Burping them requently during feeds – have a look at our guide to burping your baby for techniques.

- Try a different feeding position – check out our our guide to breastfeeding positions.
- Keep your baby upright, for at least an hour after feeding, this should help keep the milk down.
If you are mixed feeding (combining breastmilk and formula feeds), have a look at our advice on bottle feeding and reflux.
When to see the GP
If your baby has difficulty feeding or refuses to feed, regularly brings milk back up and seems uncomfortable after a feed, talk to your pharmacist, GP, or health visitor. They'll be able to give you practical advice on how to ease the symptoms and manage it – they may also need to rule out other causes (such as cow's milk allergy).
It might be helpful to keep a record of when your baby feeds, with details of how often and how much your baby brings the food back up, and how often your baby cries or seems distressed. This will help your health visitor or GP decide if your baby needs treatment.
Breastfeeding FAQs: Some Common Concerns (for Parents)
Breastfeeding is natural, but it takes practice to get it right. Here are answers to common concerns about breastfeeding.
Here are answers to common concerns about breastfeeding.
Can I Still Breastfeed if I’m Sick?
In most cases, yes — most illnesses are not dangerous to your baby. If you aren’t feeling well, remember that as your body makes antibodies to fight an illness, those antibodies go to the baby through your breast milk.
If you have coronavirus, it’s not likely to get into your breast milk. But you could spread the virus to your infant through tiny droplets that spread when you talk, cough, or sneeze. Talk to your doctor about whether you should continue to breastfeed or instead express your milk so that a healthy caregiver can give it to your baby.
If it’s OK to breastfeed, wear a mask while nursing and wash your hands before and after touching your baby. Otherwise, have a healthy caregiver from your household give your baby your expressed breast milk. This person should also wear a mask and wash hands before and after touching your baby.
Other illnesses or medicines you take may affect your ability to breastfeed. Talk to a lactation consultant or your doctor before deciding to stop breastfeeding.
Talk to a lactation consultant or your doctor before deciding to stop breastfeeding.
My Baby Doesn't Want to Nurse. What's Going On?
Babies may stop nursing — and go “on strike” — for many reasons. Something might be making your baby uncomfortable, such as sore gums from teething, an ear infection, or mouth infection called oral thrush, or even a stuffy or runny nose. Other reasons might be because you smell different — by trying a new soap or perfume — or have changed your diet and your milk tastes different.
Whatever the cause, you and your baby can get over this temporary hurdle. Here are some tips:
- Make the experience as enjoyable as possible for your baby. Praise, caress, and kiss your little one while stopping to comfort whenever he or she gets upset or frustrated.
- Nurse when your baby is sleepy and may be more willing to cooperate. Make sure there are no distractions.
- Stimulate your milk let-down by hand expressing or pumping before breastfeeding so your baby gets the milk right away.
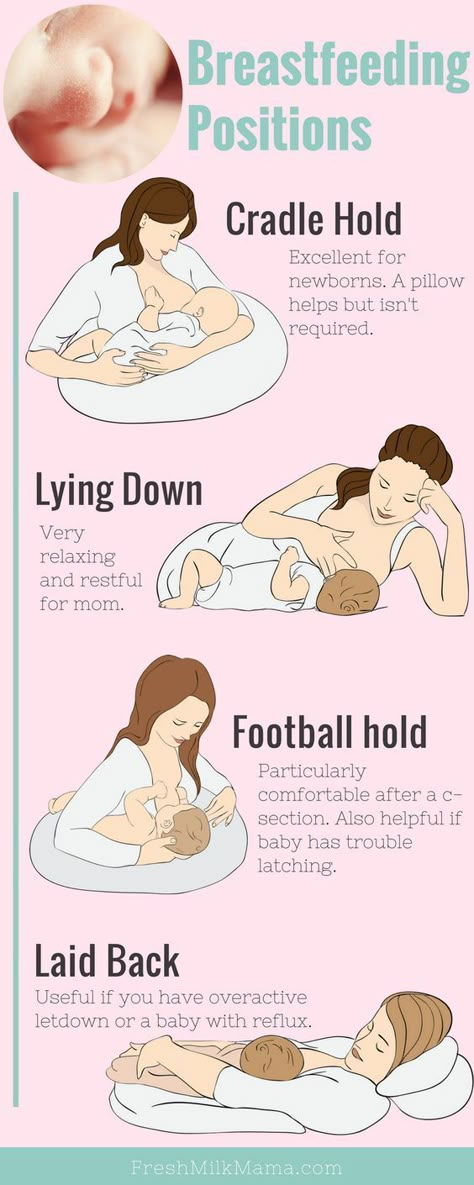
- Nurse while you're rocking your baby or walking around while carrying your little one in a sling.
Breastfeeding strikes are normal and many last only a few days. Until your nursing schedule is back to normal, pump or hand express to keep your milk supply up and to make sure the baby gets enough to eat. When your child is really ready to stop breastfeeding (or wean), they’ll probably do it over a period of weeks or months.
Is it OK to Give My Baby a Pacifier?
Pacifiers can make bebies less likely to have sudden infant death syndrome (SIDS). They also can soothe babies and satisfy their desire to suck on something. So experts recommend giving babies a pacifier at naptime and bedtime starting from when a baby is 3–4 weeks old. By then, breastfeeding usually is well-established. Continue offering the pacifier until your baby turns 1. If your baby doesn’t take the pacifier, you don’t need to force it.
Some parents worry that giving pacifiers before 3–4 weeks of age could “confuse” babies and make them less likely to take the breast. Or they might worry that it could make it hard to tell when a baby is hungry. But giving a pacifier once in a while during the first month of life (such as during a circumcision) is OK and won’t hurt breastfeeding efforts.
Or they might worry that it could make it hard to tell when a baby is hungry. But giving a pacifier once in a while during the first month of life (such as during a circumcision) is OK and won’t hurt breastfeeding efforts.
My Baby Is Nursing for Comfort. Is This OK?
If your baby seems to be getting enough milk, but continues to suck for an hour or more, your little one might be nursing for comfort rather than for nourishment. This is called non-nutritive sucking or pacifying.
So, how do you know? A baby that has fed well may stay on the breast but:
- seem satisfied
- stop sucking and swallowing
- play with your nipple
If you notice this happening, you may want to offer your baby’s thumb or hand to suck on. You also could consider giving a pacifier, but only if breastfeeding is well-established (after your baby is 3–4 weeks old).
If you have questions about breastfeeding your baby, talk to your doctor or lactation consultant.
Reviewed by: Jamila H. Richardson, BSN, RN, IBCLC
Date reviewed: January 2021
Why do babies get sick? - articles of the Cosma clinic
It is known that acute respiratory viral infections (ARVI) or colds make up two thirds of visits to a pediatrician, and infants are no exception.
Abdulova Rufiya Kosymovna
pediatrician of the highest category
Children's Polyclinic "KOSMA"
It is known that acute respiratory viral infections (ARVI) or colds make up two thirds of visits to the pediatrician, and infants are no exception.
At what age can a child become ill?
It is known that up to six months, children still retain the immunity received from the mother, especially if the child is breastfed. In addition, infants are practically isolated from unnecessary contacts, which reduces the likelihood of contracting viral infections. After 6 months, unfortunately, the risk of morbidity of the child increases. With age, the child begins to form his own immune system, training to give responses to infections.
What determines the child's morbidity?
Due to the functional immaturity of their immunity, children under 4 years of age get sick more often than adults. Children who are breastfed normally can get sick no more than 2 times a year. Children traveling with their parents and attending events with a large crowd of people, as well as babies who are bottle-fed, can get sick at the age of 1 year - up to 4 times, at the age of 4 children - up to 8 times a year. This is considered the norm.
How does breast milk protect the baby's health?
Breast milk is a living biologically active medium. It is impossible to synthesize and repeat in the milk mixture the diversity of all the ingredients of human milk - micronutrients, hormones, growth-stimulating factors, vitamins.
Every year, scientists discover more and more components in breast milk that are important for a child's health. It is known that every day a child receives with breast milk 50 mg of immunoglobulin A (a humoral immunity factor that inhibits infection on the mucous membranes), which is equivalent to 50 doses of immunoglobulin that are administered to children with various immunopathological conditions.
Artificial feeding is stressful for the tiny human body.
And any stress causes a sharp decrease in the child's immunity. Therefore, artificers get sick 2 times more often than babies.
How does ARVI get infected?
ARVI infection occurs from a sick person - an adult, a child attending a kindergarten or school. It has been proven that almost 80% of people are infected with various types of viruses that constantly live inside cells. With a decrease in immunity, viruses turn into aggressors for the immune system of their host. This applies, first of all, to persistent viruses that are more often manifested in the first year of life - herpes, cytomegalovirus, Epstein-Barr virus (causing infectious mononucleosis). Most SARS are caused by viruses. These are influenza virus, adenovirus, rhinovirus, rhinosincitial viruses, enteroviruses. In the first month of life, the baby is protected by antibodies and other immune factors received through the placenta from the mother. In addition, infants are practically isolated from unnecessary contacts, which reduces the likelihood of contracting SARS. With age, the child begins to form his own immune system, training to give responses to infections.
In addition, infants are practically isolated from unnecessary contacts, which reduces the likelihood of contracting SARS. With age, the child begins to form his own immune system, training to give responses to infections.
How to recognize SARS?
The first signs of ARVI in babies are a violation of well-being, inappropriate behavior. Children become capricious, often cry, sleep and appetite worsen. In some cases, vomiting occurs. The temperature rises: from subfebrile (from 37.1 degrees C) to high numbers (39-40 degrees C). Catarrhal phenomena (runny nose, cough) with various viral infections appear at different times - from the first hours to 2-3 days of illness. There may be difficulty breathing due to swelling and inflammation of the nasal passages (no discharge) or a watery, profuse coryza. The cough (at first dry) gradually turns into a wet one. If a child still falls ill with ARVI in the 1st month of life, in most cases, this will be an indication for his hospitalization in a hospital. For infants, the most common acute respiratory viral infection is a fairly serious disease that can worsen within a few hours with the development of complications such as otitis media, obstructive bronchitis, pneumonia, ethmoid sinusitis (accompanied by swelling, cyanosis in the eye area around the orbit of the eye, may appear within a few hours on the background of a runny nose and even without a temperature).
For infants, the most common acute respiratory viral infection is a fairly serious disease that can worsen within a few hours with the development of complications such as otitis media, obstructive bronchitis, pneumonia, ethmoid sinusitis (accompanied by swelling, cyanosis in the eye area around the orbit of the eye, may appear within a few hours on the background of a runny nose and even without a temperature).
Why is the baby snoring?
Sniffling in children of the first 3 months of life is considered a physiological condition, and can even serve as a means of communication with the mother. The baby regulates the frequency, the pace of the sounds made by the nose. If the mother does not respond, he starts screaming. Usually, sniffing does not interfere with the act of sucking, in contrast to sniffing with SARS, when there is rhinitis.
Infants have abundant vascularization (blood supply) of the nasal mucosa in the presence of narrow and short nasal passages. And any irritation (hypothermia, dry air in the room or frequent cleanings of the nose) leads to swelling of the mucous membrane, clear discharge from the nose, or a large number of crusts.
In ARVI, sniffing becomes noisier, frequent due to difficulty in nasal breathing, mucous discharges appear. The child learns to breathe through an open mouth. With SARS, swelling of the mucosa with copious discharge from the nose is seriously reflected in the well-being of the baby.
Your baby needs a humidifier to breathe freely. In its absence, you can place vases with water in different places in the room. On a hot radiator, wet sheets dry too quickly, leaving the smell of washing powder in the air.
What should I do if my baby is sick?
If a baby falls ill before a year old, you should definitely call a doctor who will adequately assess the child's condition and prescribe treatment! In no case should you treat a child of the first months on your own!
When breastfeeding, breastfeed more often. It has been proven that depending on the condition of the child, milk changes its composition even during the act of sucking, there appear active substances necessary for the child.
During any illness, the child should be well watered, because the dry cell does not respond to drugs at all.
If the baby does not latch well, he should be given additional boiled water.
Do not change the child's diet during illness!
Why is a high temperature dangerous in a child?
A child's fever is considered to be above 38°C measured in the rectum, or above 37.5°C in the armpit. It is important not to allow the temperature to rise above 38.5 g C. In children under one year old, it is necessary to measure the temperature every 15 minutes, in babies older than 12 months - after 30 minutes. High temperature (over 38.5 C) adversely affects not only viruses and microbes, but also the child's body, up to the development of dehydration or seizures.
How can I lower my child's temperature?
It's good when, against the background of a temperature, the child is all warm, willingly drinks, he is hot. If the temperature continues to rise, physical cooling methods should be used, which should be recommended by a doctor. To lower the temperature, undress the child, give an antipyretic syrup, or insert an antipyretic suppository. It is desirable that antipyretic drugs paracetamol (allowed from 0 years of age) and ibuprofen (allowed from 3 months of age) and in various forms (syrup, suppositories) are always present in the home medicine cabinet. It is necessary to use this or that drug only as prescribed by a doctor! Usually the temperature drops within 30-40 minutes after taking the medicine. Do not try to quickly reduce the temperature, it is also hard for the body, as its rapid increase (with chills). If the temperature was 39gr C, then it is enough to reduce it to 38 gr C. After that, it is necessary to solder the child, regularly ventilate the room. The first sign that the temperature has dropped is increased sweating. Become wet axillary folds, occipital region, inguinal folds.
To lower the temperature, undress the child, give an antipyretic syrup, or insert an antipyretic suppository. It is desirable that antipyretic drugs paracetamol (allowed from 0 years of age) and ibuprofen (allowed from 3 months of age) and in various forms (syrup, suppositories) are always present in the home medicine cabinet. It is necessary to use this or that drug only as prescribed by a doctor! Usually the temperature drops within 30-40 minutes after taking the medicine. Do not try to quickly reduce the temperature, it is also hard for the body, as its rapid increase (with chills). If the temperature was 39gr C, then it is enough to reduce it to 38 gr C. After that, it is necessary to solder the child, regularly ventilate the room. The first sign that the temperature has dropped is increased sweating. Become wet axillary folds, occipital region, inguinal folds.
When is an ambulance required?
It happens that in a child, against the background of a high temperature, the limbs become cold and "marble", ears, nose, or the temperature increases with severe chills. This temperature is more difficult to decrease, so you should immediately call an ambulance.
This temperature is more difficult to decrease, so you should immediately call an ambulance.
How to prevent SARS infection?
Prevention of acute respiratory viral infections and frequent colds begins even before the conception of a child. Ideally, future parents should be examined and treated for chronic viral infections - herpesvirus, cytomegalovirus, papillomavirus. Nursing women should receive a balanced diet, and take multivitamins for nursing mothers during the cold season. For the baby, it is important to prevent background diseases that worsen the state of immunity - rickets, anemia. It is important for children (especially those who are breastfed) to give vitamin D in prophylactic doses in the autumn-winter period. Very useful are frequent walks in the fresh air in the green zone, where there are fewer children. Useful courses of treatment with probiotics, which are prescribed by a doctor. It is especially recommended for formula-fed children, as well as during the introduction of complementary foods and when the season changes. During these periods, intestinal epithelial cells that produce immunoglobulin A suffer. Adults and older children in the family, when symptoms of SARS appear, must wear disposable masks, use disposable handkerchiefs and start treatment in a timely manner. Masks should be changed every 3 hours. It is necessary to remember the importance of disposing of masks and disposable handkerchiefs, since numerous viruses settle on them: do not forget to tightly tie the mask / handkerchief in a plastic bag before disposal!
During these periods, intestinal epithelial cells that produce immunoglobulin A suffer. Adults and older children in the family, when symptoms of SARS appear, must wear disposable masks, use disposable handkerchiefs and start treatment in a timely manner. Masks should be changed every 3 hours. It is necessary to remember the importance of disposing of masks and disposable handkerchiefs, since numerous viruses settle on them: do not forget to tightly tie the mask / handkerchief in a plastic bag before disposal!
In addition, daily measures are important ways to prevent SARS: frequent wet cleaning of the premises by wiping all surfaces, including door handles, with a damp cloth; washing hands with soap at every opportunity, moreover, you need to wash not only the palms, but also the lower third of the forearms.
What other factors affect children's health?
For infants, a close connection with the mother, her emotional balance is very important.
When a mother rarely takes the baby in her arms (“let the baby cry, it develops the lungs”), or she is busy with work during the breastfeeding period and leaves the baby in the care of nannies or grandmothers, the baby develops emotional rejection from the person closest to him. And this is the strongest stress in the life of a child, which leads to the development of a hypoimmune state (weakened immunity) and frequent colds. The health of children largely depends on the microclimate in the family. Frequent scandals in the family in the presence of children and the low emotional background of the mother reduce the immunity of the child and lead to illness. If a mother is going on vacation or on a business trip alone, a wise child can fall ill at this particular time, as if showing that she cannot do without her mother.
And this is the strongest stress in the life of a child, which leads to the development of a hypoimmune state (weakened immunity) and frequent colds. The health of children largely depends on the microclimate in the family. Frequent scandals in the family in the presence of children and the low emotional background of the mother reduce the immunity of the child and lead to illness. If a mother is going on vacation or on a business trip alone, a wise child can fall ill at this particular time, as if showing that she cannot do without her mother.
The health of your children largely depends on you, dear parents, on your emotional background, on the way of life of your family, on how much you learn to feel your child subtly, predict his condition, take reasonable and timely measures when the disease develops.
Good health to your little ones!
Feeding in sickness | Medela
If you or your baby are unwell, you may wonder if it is safe to breastfeed. The great news is that breastfeeding when you're sick is most often good for both of you. Read more about this in our article.
Read more about this in our article.
Share this information
Did you know that a breastfed baby is usually much less prone to illness? Although it is impossible to avoid them completely, the protective properties of breast milk help babies get sick less often and recover faster than formula-fed babies.
Breast milk contains antibacterial and antiviral agents. 2 The longer you breastfeed your baby, the lower the risk of colds and flu, ear and respiratory infections, nausea and diarrhoea. 1 Scientists are already exploring the use of breast milk to treat everything from conjunctivitis to cancer. 3.4
Should a sick baby be breastfed?
Yes. Breastfeeding promotes recovery and also helps to calm the baby. Breast milk contains antibodies, white blood cells, stem cells, and protective enzymes that help fight infections and help your baby recover faster. 1,5,6 In addition, the composition of breast milk (the balance of vitamins and nutrients) is constantly adjusted to the baby's body to help him recover as soon as possible. Thus, you will spend less time on sick leave and visit the doctor less often. 7
Thus, you will spend less time on sick leave and visit the doctor less often. 7
“Breastfeeding gives the baby everything she needs when she is sick. This is his medicine, food, drink and comfort. For a baby, this is the best thing in the world,” says Sarah Beeson, a health visitor from the UK.
Surprisingly, when a child becomes ill, the composition of breast milk changes. When you come into contact with pathogens of bacterial and viral infections, your body begins to produce antibodies to fight them, which are then passed through milk to your baby. 8 When your baby is sick, the levels of immune-boosting cells (white blood cells) in your milk also skyrocket. 5
In addition, breast milk is very easy to digest, making it ideal for babies with indigestion.
“At 12 months my daughter contracted norovirus and could only breastfeed,” recalls Maya, a mother of two in Spain. produce more milk. It was amazing. After 48 hours, I was able to meet the daily requirement for milk. It saved my baby from a drip."
It saved my baby from a drip."
It should be taken into account that sometimes during an illness it is necessary to change the habitual breastfeeding regimen. For example, with a cold, a baby may want to eat more often, but little by little, both to calm down and because of nasal congestion, which makes it difficult to apply to the chest for a long time. If your baby has a stuffy nose, an upright breastfeeding position may be more comfortable, so don't be afraid to try different breastfeeding positions.
What if the baby is seriously unwell and cannot breastfeed?
Occasionally, if a child is unwell, they may not have an appetite or energy to feed. If your baby is not eating well, seek advice from your healthcare provider, nurse practitioner, or lactation consultant to help prevent dehydration.
You may be asked to express milk to feed your baby with a bottle, a Soft Cup*, or other suitable method that requires minimal effort from the baby. Pumping on a regular breastfeeding schedule will also help keep your milk supply stable.
You can express milk with one of our convenient breast pumps, such as the modern electronic Swing Flex** or the Harmony** manual breast pump. Rest assured, freshly expressed breast milk is just as good as breast milk, so your baby will get all the protection and support it needs.
If you have concerns about your baby's health or how much milk they are drinking, see your doctor as soon as possible.
Can I continue to breastfeed if I become ill myself?
If you feel unwell, you may not want to, but in most cases it is best to continue breastfeeding. If you have a cold, runny nose, diarrhoea, vomiting, or mastitis, continue breastfeeding as normal with your doctor's approval. The baby is unlikely to become infected through breast milk. What's more, the antibodies in your milk will help reduce your baby's risk of contracting the same 13 virus.
“Breastfeeding when sick is not only safe most of the time, but also beneficial. Your baby is the least at risk of catching your upset stomach or cold, as he is already in close contact with you and receives a daily dose of protective antibodies from milk, ”says Sarah Beeson.
If there is a risk of contracting a viral infection by airborne droplets, it is advisable to temporarily switch to expressing breast milk and bottle feeding.
In order not to lose the amount of milk produced when the body is still weakened by the disease, it is best to use the Swing Maxi Flex ** double breast pump, which helps to stimulate lactation, increase the amount of milk (by 18% on average) and increase its fat content (+1% ) 14 .
However, breastfeeding and pumping when sick can be very tiring. You need to take care of yourself so that you can take care of the baby. Try to drink more fluids, eat when you can, and get plenty of rest. Crawl under the covers for a few days and ask family or friends to help care for your baby if possible, so you can put all your energy into recovery.
“Don't worry about your milk supply, it will last. Most importantly, do not stop breastfeeding abruptly so that mastitis does not develop, ”adds Sarah.
Proper hygiene is very important to reduce the risk of spreading the disease. Wash your hands with soap and water before and after breastfeeding and pumping, preparing and eating food, using the toilet and changing diapers. Use a tissue when coughing and sneezing, or cover your mouth with the crook of your elbow (not your palm) if you don't have a tissue handy. Be sure to wash or sanitize your hands after coughing, sneezing, and blowing your nose.
Wash your hands with soap and water before and after breastfeeding and pumping, preparing and eating food, using the toilet and changing diapers. Use a tissue when coughing and sneezing, or cover your mouth with the crook of your elbow (not your palm) if you don't have a tissue handy. Be sure to wash or sanitize your hands after coughing, sneezing, and blowing your nose.
Can I take medication while breastfeeding?
In agreement with the attending physician and compliance with the dosage, it is permissible to take certain medications. 9.10
.
“When talking to a doctor or pharmacist for any reason, always state that you are breastfeeding,” she continues.
What about long-term treatment?
If you are on long-term treatment for diabetes, asthma, depression, or other chronic conditions, the benefits of breastfeeding may outweigh the risks. “Breastfeeding is often possible for almost any disease, with the exception of some very rare conditions,” Sarah says, “you will be very familiar with the drugs you are taking, and during pregnancy you can discuss them with your doctor or other specialist. There is guidance on the safe use of various medicines that all healthcare professionals use.” In any case, you should consult with your doctor.
There is guidance on the safe use of various medicines that all healthcare professionals use.” In any case, you should consult with your doctor.
“I was on high doses of epilepsy medication, but I was still able to breastfeed,” recalls Nicola, a mother from the UK. “I saw a neurologist to ensure my son was safe and to minimize the risk of a seizure. Seizures can happen due to lack of sleep, and I fed day and night, but I took good care of myself, and my husband supported me. It was a positive experience."
What if I have to go to the hospital?
If you need to be hospitalized or urgently hospitalized, there are different ways to continue feeding your baby healthy breast milk so that you can return to normal breastfeeding after you are discharged.
“Express and freeze breast milk so that the caregiver can feed the baby. Practice at home ahead of time and be sure to let your doctors know that you are a breastfeeding mother, both before entering the hospital and while in it, ”recommends Sarah.
“If the baby is very small, you may be allowed to take him with you. Find out if the hospital has a supervising doctor or lactation consultant to contact. This specialist will support you, especially if you are in a general ward. If hospitalization is urgent, warn the doctors that you have a baby so that they take this into account.
Surgery under local or general anesthesia does not necessarily mean that breastfeeding will have to be stopped, or milk will need to be pumped and discarded. By the time you recover from surgery and can hold your baby, the amount of anesthetic in your breast milk will be minimal, so breastfeeding will be safe in most cases. 10 However, it is always best to consult your doctor or attending physician first.
To ensure that the situation of treatment or departure does not affect the baby's diet, it is advisable to create a breast milk bank. This should be done daily by expressing one extra serving and freezing it in the handy, durable Medela Breast Milk Storage Bags. Even stored for several months and then thawed, your carefully prepared milk will still be incomparably healthier than formula.
Even stored for several months and then thawed, your carefully prepared milk will still be incomparably healthier than formula.
For hygienic and easy pumping, use a breast pump with 2-Phase Expression technology for a fast, full flow of milk. For example, the ultra-comfortable Swing Flex** breastpump that adapts to the shape of your breasts and allows you to pump milk in a comfortable position, even lying back on the pillows 15 .
Don't forget to sterilize your breast pump with the Quick Clean microwave bags. Medela milk storage bags do not need to be handled as they are aseptically packaged and ready to use immediately.
Are there times when breastfeeding is not allowed?
In some cases, for the safety of the baby, breastfeeding should be stopped for a while, and instead, milk should be expressed and discarded to maintain milk production until the end of treatment. This includes radiotherapy and chemotherapy for cancer, herpes sores on the chest, and infections such as tuberculosis, measles, or blood poisoning that can be transmitted through breast milk. 11.12 Consult with a qualified professional about your condition to decide whether breastfeeding can continue in such cases.
11.12 Consult with a qualified professional about your condition to decide whether breastfeeding can continue in such cases.
For quality lactation support during this period, you can use the dual electronic breast pump with innovative Flex technology or rent a Symphony Clinical Breast Pump** if possible. A list of cities where you can rent a breast pump can be found on the "Rent a Medela Clinical Breast Pump" page.
Literature
1 Victora CG et al. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet . 2016;387(10017):475-490. - Victor S.J. et al., Breastfeeding in the 21st century: epidemiology, mechanisms and long-term effects. Lancet 2016;387(10017):475-490.
2 Lönnerdal B. Bioactive proteins in breast milk. J Pediatric Child Health. 2013;49 Suppl 1:1-7. - Lönnerdahl B., "Biologically active proteins of breast milk". F Pediatrician Child Health. 2013;49 Suppl 1:1-7.
F Pediatrician Child Health. 2013;49 Suppl 1:1-7.
3 Australian Breastfeeding Association [Internet]. Topical treatment with breastmilk: randomized trials. [ cited 2018 Apr 4]. Available from https://www.breastfeeding.asn.au - Australian Breastfeeding Association [Internet]. "Topical treatment with breast milk: a randomized trial". [cited 4 April 2018] See article at https://www.breastfeeding.asn.au
4 Ho JCS et al. HAMLET–A protein-lipid complex with broad tumoricidal activity. Biochem Biophys Res Commun. 2017;482(3):454-458. - Ho J.S.S. et al., "HAMLET - a protein-lipid complex with extensive antitumor activity". Biochem Biophys Res Comm. 2017;482(3):454-458.
5 Hassiotou F et al. Maternal and infant infections stimulate a rapid leukocyte response in breastmilk. Clin Transl Immunology . 2013;2(4): e 3. - Hassiot F. et al., "Infectious diseases of the mother and child stimulate a rapid leukocyte reaction in breast milk." Clean Transl Immunology. 2013;2(4):e3.
Clin Transl Immunology . 2013;2(4): e 3. - Hassiot F. et al., "Infectious diseases of the mother and child stimulate a rapid leukocyte reaction in breast milk." Clean Transl Immunology. 2013;2(4):e3.
6 Hassiotou F, Hartmann PE. At the dawn of a new discovery: the potential of breast milk stem cells . Adv Nutr . 2014;5(6):770-778. - Hassiot F, Hartmann PI, "On the threshold of a new discovery: the potential of breast milk stem cells." Adv. 2014;5(6):770-778.
7 Ladomenou F et al. Protective effect of exclusive breastfeeding against infections during infancy: a prospective study. Arch Dis Child . 2010;95(12):1004-1008. - Ladomenu, F. et al., "The effect of exclusive breastfeeding on infection protection in infancy: a prospective study. " Arch Dis Child. 2010;95(12):1004-1008.
" Arch Dis Child. 2010;95(12):1004-1008.
8 Hanson LA. Breastfeeding provides passive and likely long-lasting active immunity. Ann Allergy Asthma Immunol . 1998;81(6):523-533. — Hanson, L.A., "Breastfeeding provides passive and likely long-term active protection against disease." Ann Allergy Asthma Immunol. 1998;81(6):523-533.
9 Hale TW, Rowe HE. Medications and Mothers' Milk 2017. 17th ed. New York, USA: Springer Publishing Company; 2017. 1095 p . — Hale T.W., Rowe H.I., Medications and Breast Milk 2017. 17th edition. New York, USA: Publishing House Springer Publishing Company ; 2017. p. 1095.
10 Reece-Stremtan S et al. ABM Clinical Protocol# 15: Analgesia and anesthesia for the breastfeeding mother, Revised 2017. Breastfeed Med . 2017;12(9):500-506. - Rees-Stromtan S. et al., AVM Clinical Protocol #15: Analgesia and Anesthesia for Nursing Mothers, 2017 edition. Brestfeed Med (Breastfeeding Medicine). 2017;12(9):500-506.
Breastfeed Med . 2017;12(9):500-506. - Rees-Stromtan S. et al., AVM Clinical Protocol #15: Analgesia and Anesthesia for Nursing Mothers, 2017 edition. Brestfeed Med (Breastfeeding Medicine). 2017;12(9):500-506.
11 Lamounier JA et al. Recommendations for breastfeeding during maternal infections. J Pediatr 2004;80(5 Suppl ):181-188. - Lamunier J.A. et al., Guidelines for Breastfeeding during Maternal Infectious Diseases. J Pediatrician (Journal of Pediatrics) (Rio J). 2004;80(5 Suppl):181-188.
12 Hema M et al., Management of newborn infant born to mother suffering from tuberculosis: Current recommendations & gaps in knowledge. Indian J Med Res . 2014;140(1):32-39. - Hema M. et al., "Working with the Infant Born to a Mother with Tuberculosis: Current Recommendations and Gaps".










