Baby choked on food
Choking (for Parents) - Nemours KidsHealth
What Is Choking?
When a child is choking, it means that an object — usually food or a toy — is stuck in the
trachea(the airway). When this happens, air can't flow normally into or out of the lungs, so the child can't breathe properly.
The trachea is usually protected by a small flap of tissue called the
epiglottis. The trachea and the esophagusshare an opening at the back of the throat. The epiglottis acts like a lid, snapping shut over the trachea each time a person swallows. It allows food to pass down the esophagus and prevents it from going down the trachea.
But every once in a while, the epiglottis doesn't close fast enough and an object can slip into the trachea. This is what happens when something "goes down the wrong pipe."
Most of the time, the food or object only partially blocks the trachea, is coughed up, and breathing returns to normal quickly. Kids who seem to be choking and coughing but still can breathe and talk usually recover without help. It can be uncomfortable and upsetting for them, but they're generally fine after a few seconds.
Is Choking an Emergency?
Sometimes, an object can get into the trachea and completely block the airway. If airflow into and out of the lungs is blocked and the brain is deprived of oxygen, choking can become a life-threatening emergency.
A child may be choking and need help right away if he or she:
- can't breathe
- is gasping or wheezing
- can't talk, cry, or make noise
- turns blue
- grabs at his or her throat or waves arms
- appears panicked
- becomes limp or unconscious
In these cases, if you've been trained, immediately start abdominal thrusts (also known as the Heimlich maneuver), the standard rescue procedure for choking.
What Are Abdominal Thrusts (the Heimlich Maneuver)?
If you have kids, it's important to get trained in both cardiopulmonary resuscitation (CPR) and the technique of abdominal thrusts (the Heimlich maneuver).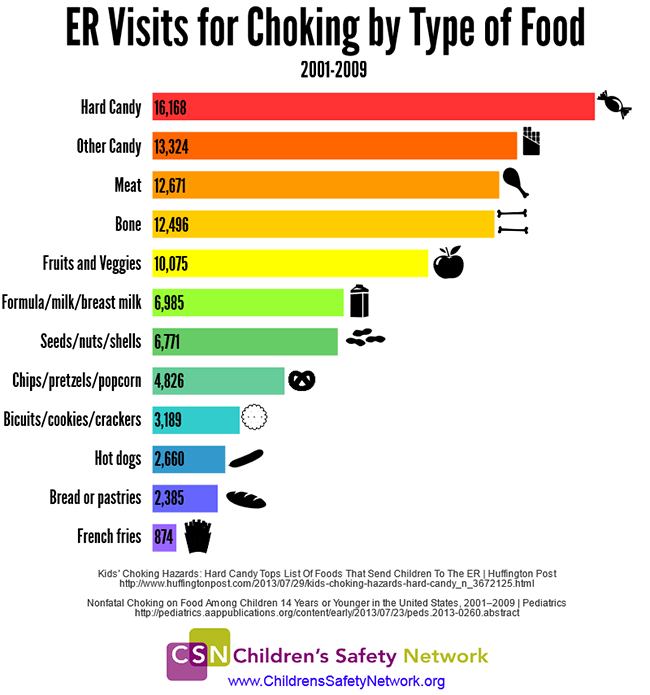 Even if you don't have kids, knowing how to perform these first-aid procedures will let you help if someone is choking.
Even if you don't have kids, knowing how to perform these first-aid procedures will let you help if someone is choking.
When a person does abdominal thrusts, a sudden burst of air is forced upward through the trachea from the diaphragm and will dislodge a foreign object and send it flying up into (or even out of) the mouth.
Though the technique is pretty simple, abdominal thrusts must be done with caution, especially on young children. They are safest when done by someone trained to do them. If done the wrong way, the choking person — especially a baby or child — could be hurt. There's a special version of abdominal thrusts just for infants that is designed to lower the risk of injury to their small bodies.
The technique of abdominal thrusts and CPR are usually taught as part of basic first-aid courses, which are offered by YMCAs, hospitals, and local chapters of the American Heart Association (AHA) and the American Red Cross.
What Should I Do?
Call 911 for any serious choking situation.
Here are several possible situations you might face and tips on how to handle them:
If a child is choking and coughing but can breathe and talk:
- This means the airway is not completely blocked. It's best to do nothing. Watch the child carefully and make sure he or she recovers completely. The child will likely be fine after a good coughing spell.
- Don't reach into the mouth to grab the object or even pat the child on the back. Either of these steps could push the object farther down the airway and make the situation worse.
- Stay with the child and remain calm until the episode passes.
If a child is conscious but can't breathe, talk, or make noise, or is turning blue:
- The situation calls for abdominal thrusts.
- Call 911 or tell someone nearby to call 911 immediately.
- Begin the thrusts if you've been trained to do so.
- If you haven't been trained, and no one else is available who has been, wait until help arrives.

If the child was choking and is now unconscious and no longer breathing:
- Shout for help and call 911, or tell someone nearby to call 911 immediately.
- Start CPR right away, if you've been trained in it.
- If you have not been trained, and no one else is available who has been, wait until help arrives.
When Should I Call the Doctor or Go to the ER?
After any major choking episode, a child needs to go to the ER.
Get emergency medical care for a child if:
- The child has a lasting cough, drooling, gagging, wheezing, trouble swallowing, or trouble breathing.
- The child turned blue, became limp, or was unconscious during the episode, even if he or she seemed to recover.
- You think the child has swallowed an object, such as a toy or battery.
If a child had an episode that seemed like choking but fully recovered after a coughing spell, there is no need to get emergency medical care, but you should call your doctor.
How Can We Prevent Choking?
All kids are at risk for choking, but those younger than 3 are especially at risk. Young kids tend to put things in their mouths, have smaller airways that are easily blocked, and don't have a lot of experience chewing, so they might swallow things whole.
To help protect kids:
- Avoid foods that pose choking risks (like hot dogs, grapes, raw carrots, nuts, raisins, hard or gummy candy, spoonfuls of peanut butter, chunks of meat or cheese, and popcorn), which are a similar size and shape as a child's airway.
- At mealtime, be sure to serve a child's food in small bites. That means cutting whole grapes into quarters, cutting hot dogs lengthwise and into pieces (and remove the tough skin), and cooking vegetables rather than serving them raw. Teach kids to sit down for all meals and snacks and not to talk or laugh with food in their mouths.
- Toys and household items also can be choking hazards — beware of deflated balloons, coins, beads, small toy parts, and batteries.
 Get down on the floor often to check for objects that kids who are learning to walk or crawl could put in their mouths and choke on.
Get down on the floor often to check for objects that kids who are learning to walk or crawl could put in their mouths and choke on. - Choose safe, age-appropriate toys. Always follow the manufacturer's age recommendations — some toys have small parts that can cause choking. To determine if a toy is too small, see if it passes easily through an empty cardboard toilet paper tube. If it does, it's too small.
Take the time now to become prepared. CPR and first-aid courses are a must for parents, other caregivers, and babysitters. To find one in your area, contact your local American Red Cross, YMCA, or American Heart Association chapter, or check with hospitals and health departments in your community.
Reviewed by: Kate M. Cronan, MD
Date reviewed: February 2019
What to Do If Baby Is Choking: Step-By-Step First Aid
Do you know what to do if your baby is choking? While it’s something no caregiver wants to think about, even seconds count if your child’s airway is obstructed.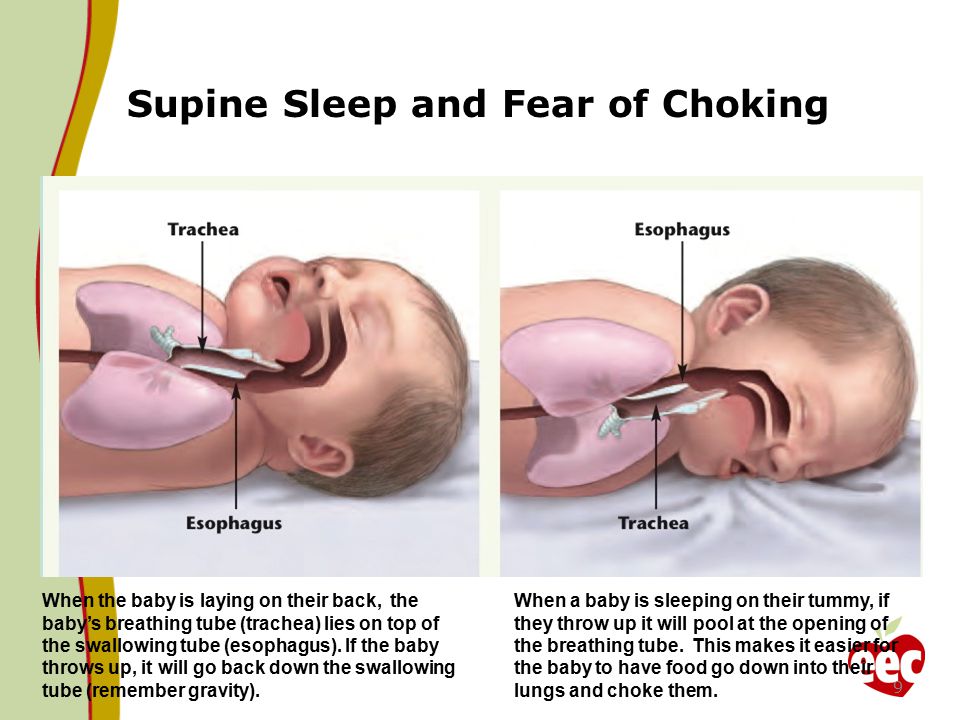 Knowing the basics can help you potentially dislodge an object or know what to do until help arrives.
Knowing the basics can help you potentially dislodge an object or know what to do until help arrives.
Here’s more about how you can help a baby (under 12 months old), what you definitely shouldn’t do, and some tips to prevent choking accidents in your home.
Things can happen very quickly in emergencies, so we’ve kept our descriptions clear and to the point.
Step 1: Verify that your baby is actually choking
Your baby may be coughing or gagging. This can sound and look scary, but if they’re making noise and able to take breaths, they’re likely not choking.
Choking is when a baby is unable to cry or cough. They also won’t be able to make any noise or breathe because their airway is completely obstructed.
Step 2: Call 911
Ideally, you can have a friend or family member call 911 or local emergency services while you take care of your baby.
Explain the steps you’re following to the operator and provide updates. It’s especially important that you tell the operator if your child becomes unconscious at any point during the process.
Step 3: Place your baby face down on your forearm
Use your thigh for support. With the heel of your free hand, deliver five blows to the area between their shoulder blades. These blows should be both quick and strong to be effective.
This action creates vibrations and pressure in your baby’s airway that will hopefully force the object out.
Step 4: Turn baby over onto their back
Rest your baby on your thigh, keeping their head lower than their chest. With your index and middle fingers, find your baby’s breastbone (between and slightly below the nipples). Press down five times with enough pressure to press the chest down about one-third.
This action helps to push air from the lungs into the airway to potentially force the object out.
Step 5: Repeat
If the object still hasn’t dislodged, return to back blows following the same instructions above. Then repeat the chest thrusts. Again, tell the 911 operator immediately if your baby loses consciousness.
Related: Why every anaphylactic reaction requires a trip to the emergency room
It’s beyond scary to think about this whole scenario playing out in real life. But it happens.
You may or may not be surprised to learn that food is the most common cause of choking with infants. That’s why it’s important to introduce only age-appropriate foods — usually purees — to your child after they turn 4 months old.
Watch out for these foods in particular:
- grapes (If giving these to your older baby — they’re not appropriate until closer to a year of age — peel off the skin and cut in half first.)
- hot dogs
- chunks of raw fruits or vegetables
- chunks of meat or cheese
- popcorn
- nuts and seeds
- peanut butter (While perhaps technically a puree, the thickness and stickiness makes it a hazard.)
- marshmallows
- hard candies
- chewing gum
Of course, we know you’re likely not giving chewing gum or hard candy to an infant — but consider if your baby found some on the ground. Even the most careful caregiver may miss certain objects that land places where little eyes end up seeing them.
Even the most careful caregiver may miss certain objects that land places where little eyes end up seeing them.
Other choking hazards found around the home include:
- marbles
- toys with small parts
- latex balloons (uninflated)
- coins
- button batteries
- pen caps
- dice
- other small household items
Young babies may also choke on liquids, like breast milk, formula, or even their own spit-up or mucus. Their airways are particularly small and easily obstructed.
This is one reason that you hold your baby with his head below his chest when attempting to help. Gravity may allow the liquid to drain out and clear the airway.
Related: Choking on saliva — causes and treatments
While it’s tempting, resist the urge to reach in your baby’s mouth and grab an object out unless it’s visible and easy to grasp with your fingertips.
Grasping around something that you can’t see in their throat may be harder than you think. And you may actually push the object farther down into the airway.
And you may actually push the object farther down into the airway.
Also, don’t attempt to do the Heimlich maneuver (abdominal thrusts) with an infant. While abdominal thrusts can help children and adults move objects in their airways, they can be damaging to a baby’s developing organs.
You may also have heard to turn your baby upside down and hold them by their feet. This isn’t a good idea because it may force the object deeper into the throat — or you could accidentally drop your child in the process.
Related: Introduction to first aid for babies, children, and adults
If your baby does lose consciousness, the 911 operator may instruct you to do CPR until help can arrive. The goal of CPR isn’t necessarily to bring your baby back to consciousness. Instead, it’s to keep the blood and oxygen circulating to their body and — even more importantly — to their brain.
One set of CPR includes 30 chest compressions and 2 rescue breaths:
- Place your infant on a flat, firm surface, like the ground.

- Look for an object in your baby’s mouth. Remove it only if it’s visible and easy to grasp.
- Place two fingers on your baby’s breastbone (the area where you applied pressure for chest thrusts). Apply pressure that compresses their chest about one-third (1 1/2 inches) at a rhythm of around 100 to 120 compressions each minute. Complete 30 chest compressions in all.
- Tilt your baby’s head back and lift their chin to open the airway. Give two rescue breaths by making a seal around the baby’s mouth and nose. Blow each breath in for 1 full second.
- Then repeat this process until help arrives.
You may not be able to prevent all choking accidents. That said, you can take measures to make your home as safe as possible for your baby.
Pay attention at mealtime
Especially as the foods you offer get chunkier, it’s important to keep good watch on your little one as they eat. And be sure to have your child sitting at meals versus walking or running around.
Provide age-appropriate foods
“Age-appropriate” means starting with purees at first and then progressively offering larger pieces of soft foods that can mash in your baby’s mouth. Think boiled sweet potatoes versus raw carrots or bits of avocado versus chunks of orange.
That said, if you do choose to do the baby-led weaning approach to feeding your infant, you don’t necessarily need to worry. Multiple studies (like research from 2016 and 2017) have shown no significant difference in risk with spoon feeding and feeding soft finger foods.
Speak with your doctor
Before offering high-risk foods, like grapes and peanut butter, check in with your pediatrician. They can help you decide when the best time is to introduce these foods and the best way to present them so they aren’t as much of a choking risk.
Read labels on toys
Check toy labels to ensure you’re buying ones that are age appropriate for your baby. And examine other toys in your home that might belong to older siblings. Consider creating a special spot for toys with small parts so they stay off the ground.
Consider creating a special spot for toys with small parts so they stay off the ground.
Create a safe space
Keep other hazards, like batteries or coins, out of your baby’s reach. If babyproofing your entire home seems overwhelming, you might try creating a dedicated “safe space” that’s gated off while you work on babyproofing the rest.
If you’re still feeling a bit uneasy about your ability to help your baby in an emergency, consider taking an infant first aid class that covers both choking and CPR skills.
You may be able to find classes near you by calling your local hospital. A 2019 study showed that practicing on mannequins can help with learning and confidence in executing these procedures.
Otherwise, do your best to keep choking hazards out of your baby’s play areas and pay close attention to anything you see in your baby’s mouth that shouldn’t necessarily be there.
What to do if a child chokes
It is impossible to control 100% of all the actions of the baby, therefore, cases when children get something into the respiratory tract or they choke on something often occur.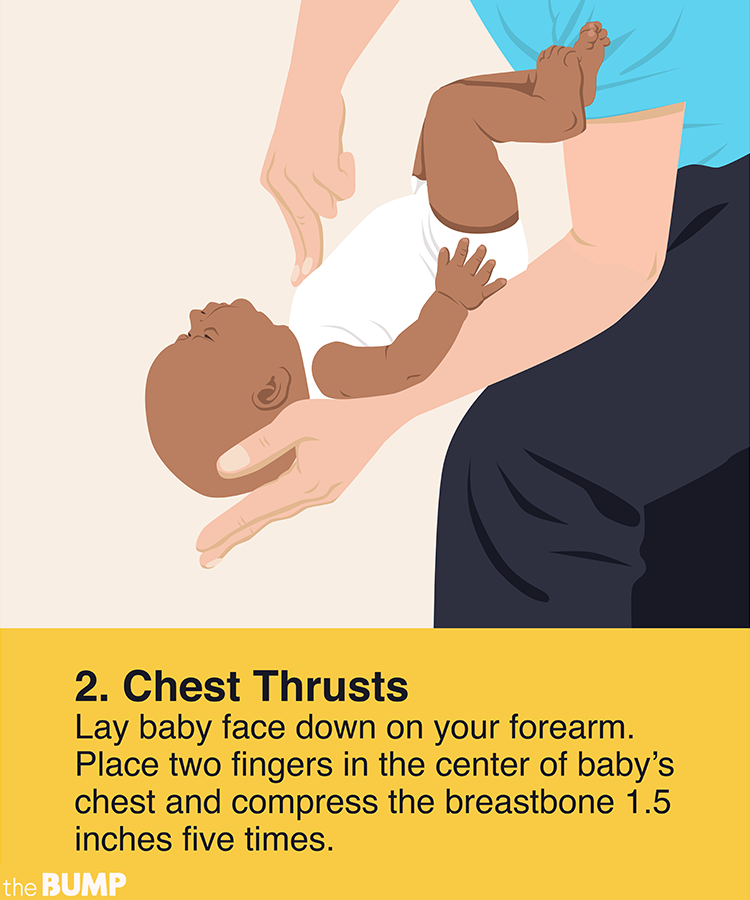 Most often, parents do not need to take any action, because. the child's body is able to independently get rid of a foreign object with the help of a cough. A sign that the airway is not blocked is that the child may cry and/or call for help. Then you just calm the baby and keep the situation under control. nine0003
Most often, parents do not need to take any action, because. the child's body is able to independently get rid of a foreign object with the help of a cough. A sign that the airway is not blocked is that the child may cry and/or call for help. Then you just calm the baby and keep the situation under control. nine0003
Signs that intervention is needed?
- eyes wide open in panic
- he cannot utter words, cry and scream, or does it quietly and wheezing
- there is increased salivation
- baby opens mouth wide
- skin turns red and then turns blue
- older children may hold their throats
- loss of consciousness
The first thing to do is to call an ambulance. It is advisable to have someone else do this so that you can immediately begin to provide first aid.
First aid for children under one year old
As a rule, infants choke while eating or drinking due to incorrect posture.
Your possible actions:
1. Raise the baby's hands up. Despite its unusualness and simplicity, this method helps to normalize the breathing process by expanding the airways. nine0003
2. Put the child on your hand with your stomach down and make five pats between the shoulder blades with the edge of your palm.
3. In the case when the baby choked on a small object, it is necessary by the child's legs so that the head is down and also pat between the shoulder blades
4. Tilt the body of the child down, press on the root of the tongue, thereby causing vomiting.
5. If the baby choked on the liquid and began to cough, choke with a cough, breathe noisily, and also in case of a solid object getting stuck, it is necessary to turn it with its back to you, hug your hand while pressing it on the stomach area, tilt the child forward and pat on the back, as described in the first paragraph. nine0003
If there are no signs of improvement, lay him on his back so that his head is lower than his torso.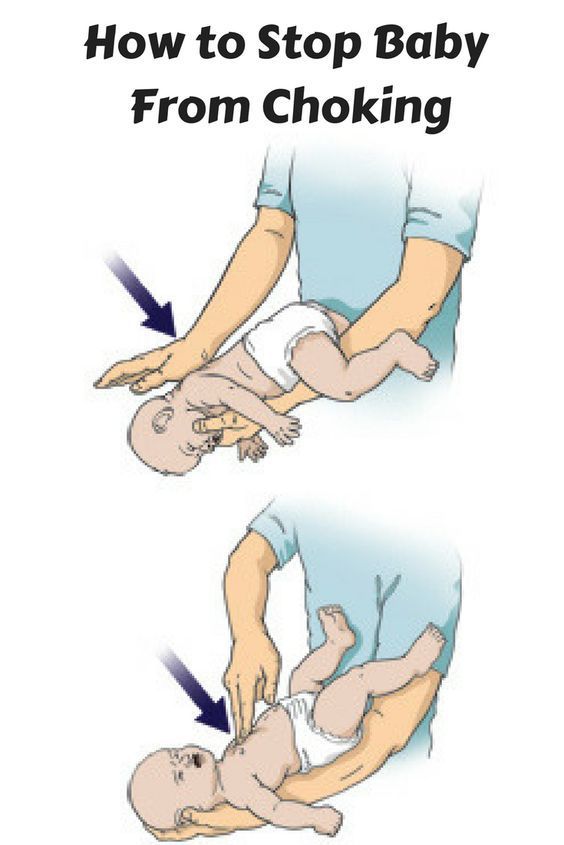 Place your middle and index fingers under your baby's breastbone. Do five pressures to a depth of 1-2 cm, making sure that after each of them the baby's sternum straightens without removing the fingers. You should alternate pressure and pats on the back until the doctors arrive. After each pop, check to see if the airway blockage has been cleared.
Place your middle and index fingers under your baby's breastbone. Do five pressures to a depth of 1-2 cm, making sure that after each of them the baby's sternum straightens without removing the fingers. You should alternate pressure and pats on the back until the doctors arrive. After each pop, check to see if the airway blockage has been cleared.
Attention! All pressing and patting should be gentle but sharp! nine0003
You can find on the Internet a recommendation to check the child's larynx with your finger and, if possible, remove the stuck object. Such advice is useful if the foreign object is something soft, such as cotton wool. In other cases, there is a great risk of aggravating the situation by accidentally moving the subject even further.
First aid for a child older than one year
Remain calm so as not to aggravate the child's panic. nine0003
You can use the above methods for older children as well. 5 point will differ by the posture of the child. See picture below:
See picture below:
Also for children aged from a year (in no case for children younger!) The Helmich method is effective. The sequence of your actions will be as follows:
- stand behind the baby, you can kneel if his height is still small
- clench the hand of one hand into a fist and place the thumb inside between the ribs and the navel of the child
- clasp the fist with the palm of the other hand
- spread your elbows to the sides and press on the child's stomach from the bottom up
- continue until the foreign object is out of the respiratory tract
If the child's breathing has stopped
If the child's breathing stops during removal of the foreign body and does not resume after removal, this may be the result of a spasm in the throat due to stress. Breathing resumption method:
- lay the child on its side on a flat hard surface
- tilt head back a little
- lift chin
If the attempt was unsuccessful, it is urgent to start performing artificial respiration and chest compressions.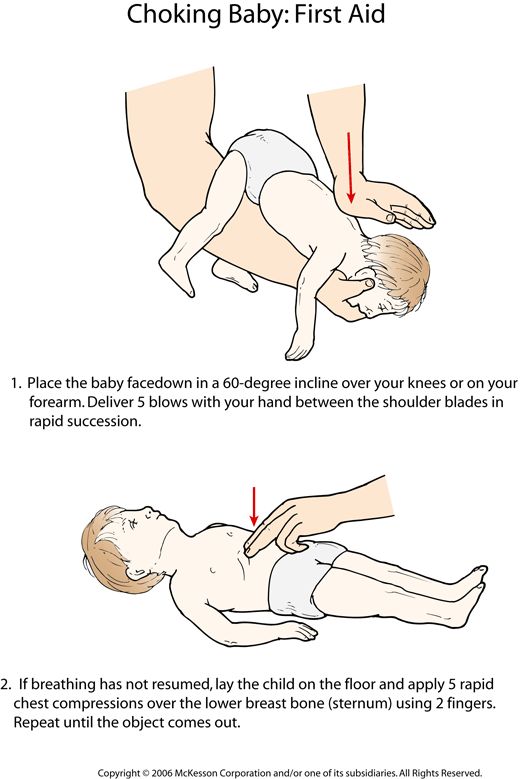 How to do this can be read, for example, here. nine0003
How to do this can be read, for example, here. nine0003
Even if you managed to solve the problem on your own, you should definitely consult a doctor to check if the baby has damaged the airways.
What should I do if my child chokes?
What to do if the baby is choking? Everyone needs to know this. And if this happened, it is dangerous to waste time, every second counts here. But let's start with what you don't need to do.
Useful and useless measures
The potential danger for the baby is often formed by his mother and father. Teeth are cut, and the baby strives to gnaw on all the objects that it can reach. What is the point of giving foreign objects to gnaw - it is much more logical to give the baby something edible, useful. For example, a piece of banana, apple or cucumber. This is the point of view of some parents. The child is under supervision - what can threaten him? But trouble can happen in the blink of an eye.
If at least the top of a milk tooth has hatched in a baby, he will certainly bite off at least a small crumb from the fruit.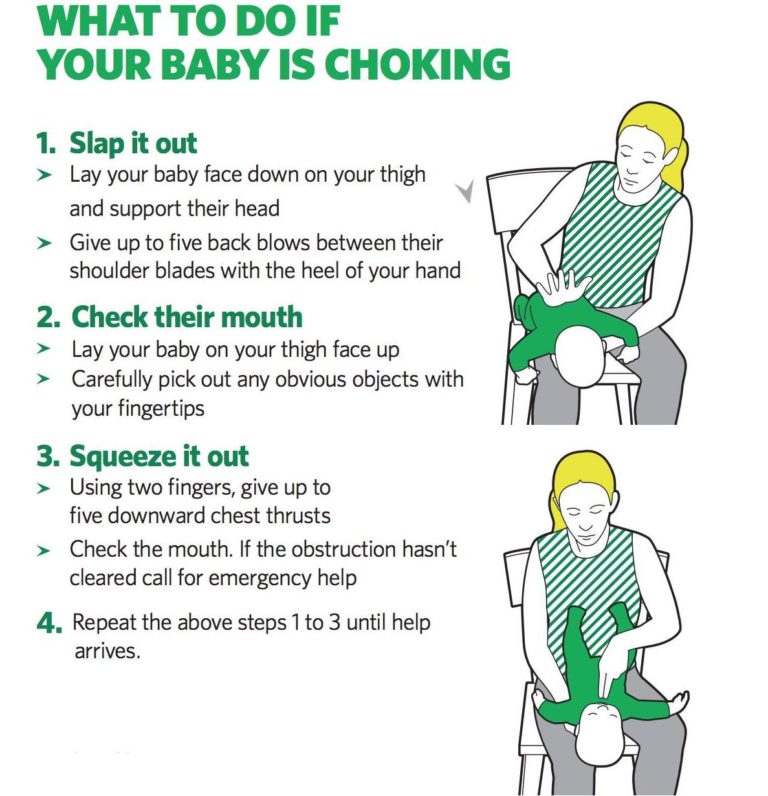 He was delighted, frightened, inhaled sharply - and now the fool choked on food. nine0003
He was delighted, frightened, inhaled sharply - and now the fool choked on food. nine0003
Slightly older babies can be harmed by small fragments of toys - because they need to taste everything. Yes, and during a normal meal, a child can form and make a voice, laugh, whimper - and choke. A typical situation is when an ordinary candy becomes the cause of such an incident.
- In other words, in no case do not neglect the age restrictions indicated on the toys;
- the baby should not touch things from which a small part or detail can be separated; nine0003
- as early as possible wean him to give voice during meals;
- do not let the baby play or fall asleep with candy in his mouth.
Despite any preventive measures, one should never relax and one must constantly be vigilant. If the baby choked and it became difficult for him to breathe, you can’t hesitate, we begin a set of urgent measures.
Procedure for choking a baby under one year of age:
- you should raise the handles up - thereby expanding the airways a little, it will become easier for the child to inhale and exhale;
- if breathing is not restored, we put the baby face in the palm, lifting his ass a little higher than his head. Slightly patting on the back, successively directing these claps from the pelvic region to the back of the head. Then the child needs to be turned over, and the butt is still above the level of his head, and lightly press on the sternum 4-6 times, trying to force the fluid out of the lungs. These techniques should be repeated until free breathing is fully restored. nine0003
Slightly patting on the back, successively directing these claps from the pelvic region to the back of the head. Then the child needs to be turned over, and the butt is still above the level of his head, and lightly press on the sternum 4-6 times, trying to force the fluid out of the lungs. These techniques should be repeated until free breathing is fully restored. nine0003
- if the reason that the baby choked was food, you should gently lift him up, holding his legs or stimulate the child to vomit by pressing a finger on the root section of his tongue.
If a foreign object is in the airways, preventing the child from crying and raising a voice, if he waves his arms and pulls in his tummy, immediately call the emergency medical service, before she arrives, you need to do this:
- When the liquid became the cause, the baby has a cough and shortness of breath, take the child with his back to you, hugging and pressing on the tummy near the stomach, tilting the baby, pat him on the back. nine0003
nine0003
- If this does not work, put the baby on the back with his head below the body. Place your middle and index fingers under the baby's breastbone and apply pressure five times. Make sure your chest expands after each press.
- If the cause of the accident was a small solid object (bead, part from the designer), lay the child on his tummy over your arm, placing his head below the torso. With the palm of your other hand, lightly tap on the back. You can also lift the child by the legs to also pat on the back. nine0003
- Combine the above techniques, controlling whether the foreign object came out. If you did everything right and this object appeared in your mouth, carefully remove it from there.
- If these techniques do not give the desired result, artificial respiration should be started. For babies up to 8 months of age, it is done immediately both in the nose and in the mouth. Here you do not need to tilt your head back, just slightly raise the child's chin.
Exhale 3-5 times and make sure the baby's chest expands. If this happens, then the baby can breathe. Take a few more breaths to help the child return to a normal breathing rhythm. nine0003
All movements must be done in no way abruptly, without effort. Overdone, you can injure the baby and harm him even more.
What NOT to do when the baby is choking
If this happens, then the most important thing is not to lose your cool and determine whether you need to call emergency medical care. Mom's commotion will frighten the child much more.
For example, choking, the baby retains the ability to breathe in and out. He cries, screams. In this case, you do not need to tap him on the back: let him clear his throat, after which the child needs to be reassured. nine0003
If a foreign object is in the airways, it is strictly forbidden to pat the child on the back when he is in a vertical position. In this case, it can be harmed by involuntarily pushing a foreign object much deeper. In such a situation, it is necessary to tilt the head and body of the baby.
In such a situation, it is necessary to tilt the head and body of the baby.
Remember the strict requirement: in any case, do not try to remove the stuck object on your own! You can make the child much worse, and his breathing can be completely blocked. In this case, you need to call the "ambulance". nine0003
Measures to help babies over one year of age
You need to start with one thing: no panic! One-year-old children and older are already well aware and perceive the emotions of their parents. And with your unbridled panic, you can alarm the child too much.
In essence, the measures of immediate assistance to infants of this age category approximately coincide with the methods of assistance to infants. If a foreign object or food crumbs gets into the larynx, lift the baby, firmly grasping the legs, or stimulate his gag reflex. However, in most cases, the child manages to cough without outside help. nine0003
But if the situation turned out to be more complicated and the above measures did not give the desired result, then the procedure is as follows. You need to put the baby face up on the crib. Press under the ribs into the upper abdomen, pushing up slightly, repeat several times. These movements stimulate the movement of a foreign object back into the oral cavity.
You need to put the baby face up on the crib. Press under the ribs into the upper abdomen, pushing up slightly, repeat several times. These movements stimulate the movement of a foreign object back into the oral cavity.
Often another method is used. The child is in front of you, with his back to you. Place your palm on his chest so that the baby rests on your arm. His body should be slightly tilted forward. With the other hand, tap on the back between the shoulder blades 4-5 times. nine0003
In the event that a foreign object has become the cause of the accident, it is also recommended to use the direct aid method for suffocation, developed by the American surgeon Henry Heimlich. This technique includes two different ways of helping, depending on whether the patient is conscious or not.
First way
Standing behind, clench your right hand into a fist, on top - the left. Press vigorously with the fist of your right hand on the area under the ribs above the navel, directing the movement from the bottom up, towards the sternum, while the arms are bent at the elbows. Continue until then. Until the subject exits and breathes back. This method is suitable for babies from the age of one. nine0003
Continue until then. Until the subject exits and breathes back. This method is suitable for babies from the age of one. nine0003
Second way
Lay the child face up and place the hands in the same way as in the first example. With vigorous movements, push up towards the diaphragm until the victim resumes independent inhalations and exhalations. If these efforts fail, artificial respiration and chest compressions may be needed.
These exercises should be done until the foreign object returns to the oral cavity. This method does not apply to babies under 1 year old. nine0003
Baby is choking and not breathing: what to do
When the child chokes, it is likely that breathing stops due to spasms in the larynx. The most common cause of them is a stressful situation for the child.
The order of urgent action in such a situation is as follows:
- you need to lay the child sideways on the table;
- slightly tilt your head back;
- slightly raise your head by the chin. nine0003
nine0003
If breathing is not restored, begin artificial respiration immediately:
- in the same way, put the baby on the table;
- take the head back and open your mouth;
- make sure there are no foreign objects in the oral cavity;
- exhale into the child's mouth for a long time;
- repeat 3-4 times. If the chest expands, then you have achieved the desired result, the air enters the lungs of the child. If the baby's chest is immobile, then take urgent measures to eliminate obstructions to breathing; nine0003
- after this, we place one palm on top of the other on the child's chest and press sharply - the chest should straighten out each time;
- alternate this massage and exhalation into the mouth at least 16 times.
What to do when the baby chokes
This can happen in various circumstances: bathing in a bathtub, splashing in a summer inflatable pool or in a pond, falling into a pond, or accidentally inhaling liquid while drinking. Measures to save a choked baby must also be taken as quickly as possible: nine0003
Measures to save a choked baby must also be taken as quickly as possible: nine0003
- Place the baby on your thigh prone, lowering his head below the body, and press on his back. By doing this, you will help eliminate water from his respiratory tract.
- Make sure that there are no foreign objects or vomit in the child's mouth.
- Following this, it is necessary to take measures, according to the basic requirements:
- Respiratory patency should be achieved. The baby lies prone, his neck is not bent, the lower jaw is advanced, the tip of the tongue is retracted. We massage the heart, do artificial respiration. nine0003
If we do everything as it should be, then we observe the rhythmic movement of the breathing baby's chest. If these regular movements are absent, but the abdomen is swollen, then breathing does not occur.
For every couple of exhalations, press the chest 15 times. Toddlers up to one year of age should do these movements with two fingers, and only starting from a year old can you use your palm.