Nestle baby food guide chart
Baby Nutrition and Feeding Guide
0-6 Months: Parenting Tips & Articles
Article
How will you feed your newborn?
8 mins to read Jul 31, 2017
It’s a common and important question for any parent or parent-to-be, and it’s never too early to start making decisions about baby nutrition. You can turn to this guide to help prep your infant feeding plan and find out valuable facts about baby nutrition. Constantly craving information? Add to the info below with guidance on first-year feeding from the Canadian Paediatric Society.
Breast milk is best
It’s the perfect food for a newborn baby in that it’s nutrient-rich,¤ it can change feeding by feeding to meet the nutritional needs of your baby as they grow, and it’s naturally produced to give your baby the best start in life.
Breastfeeding is great for you as well. It can help you return to your pre-pregnancy weight faster and help create an intimate bond between you and your baby.
Health Canada recommends that for the nutrition, immunologic protection, growth, and development of infants and toddlers, you breastfeed exclusively for the first six months, and you sustain it for up to two years or longer with appropriate complementary feeding.1,2
Learn more about the benefits of breastfeeding now.
Your infant feeding plan
How you feed your baby is a very personal decision. Here’s what you should consider while you personalize a baby nutrition plan:
- Base it on the right information, advice and support from your healthcare professional and your family.
- Know that breast milk is the ideal food for baby nutrition during the first six months of life.
- Look over the variety of infant formulas available, should you choose to introduce one.
As you get ready to give your baby all the nourishment they’ll need by developing an infant feeding plan, consider the following for yourself:
As you get ready to give your baby all the nourishment she’ll need by developing an infant feeding plan—consider this:
1.
 Healthy Mom, healthy Baby
Healthy Mom, healthy Baby- Eat healthy (and enough. Newborns feed every 2-3 hours, you gotta eat, too).
- Hydrate.
- Get lots of rest.
- Call on family and friends for help around the house (or just let the chores wait).
- Keep "Eating Well with Canada's Food Guide" on your fridge.
2. Learn about breastfeeding
Ready, set, breastfeed! Make it a fulfilling experience for both of you by arming yourself with helpful hints, as well as tips on how to cope with challenges.
3. Get right to it!
- Breastfeed ASAP after birth (within 30 to 60 minutes is recommended if you are healthy enough to do so).
- Hold your baby to skin-to-skin often to promote successful breastfeeding initiation.
- Confirm your hospital supports 24-hour rooming-in (so you never keep your hungry baby waiting).,
4. Know your supplementing options for optimum baby nutrition
- Your choices include breastfeeding (ideally), supplementing breast milk with infant formula or feeding with infant formula only.
- Health Canada recommends cow milk-based commercial infant formula as the only safe and nutritious alternative to breast milk.1,2
- Canadian healthcare experts recommend cow's-milk based infant formula from birth until 9 to 12 months of age.1,2
- Iron-fortified infant formula offers a complete source of nutrition for your baby during the first year (The Canadian government actually regulates the composition of infant formula).
- Infant formulas contain the recommended amounts of fat, carbohydrates, protein, vitamins, and minerals needed for baby's growth and development.
- You have several choices of infant formulas – always speak to your doctor before making changes to what you feed your baby.
When can my baby have cow's milk?
Whole (3.25 percent) cow's milk isn't recommended as a part of a baby nutrition plan until the 9- to 12-month mark for these reasons:
Iron should be part of a baby nutrition plan
As you strengthen your iron knowledge with the info below, know that your baby’s initial iron reserves may start to run low at about the 6-month mark1.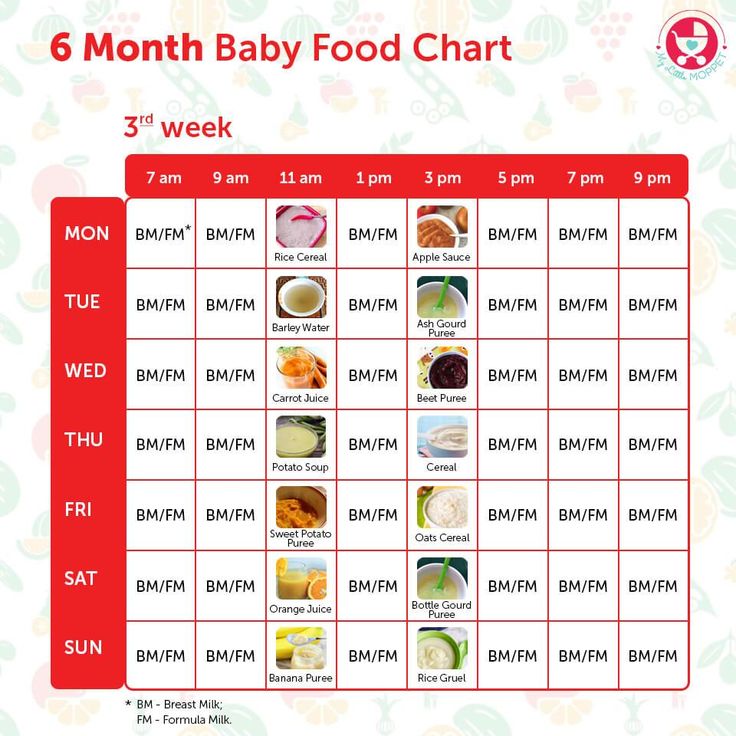
Why iron?
- It’s a vital nutrient that contributes to the normal growth and development of your baby.
- It’s essential in building red blood cells that transport oxygen throughout her little body.
How does a baby get iron?
- Healthy full- term infants are born with iron stores, which meet their needs until about six months of age.
- Your own iron-rich diet will help ensure that these stores stay topped up.
- Breast milk will provide your baby with adequate iron for those first 6 months1.
- Should you choose to supplement or exclusively formula feed, choose an iron-fortified formula.
- Introduce iron-rich solid foods after the 6-month mark1.
Wait, solid foods?
- Yep, your baby will be ready to start eating solid foods by around six months.
- The introduction of foods into a baby nutrition plan should be a steady progression of single ingredients and portion sizes between six and 12 months of age.

- Health Canada recommends baby’s first foods be iron-rich.1
- Healthy iron-rich options are meat, meat alternatives and iron-fortified baby cereal.
- Babies should be offered iron-rich foods two or more times a day.1,2
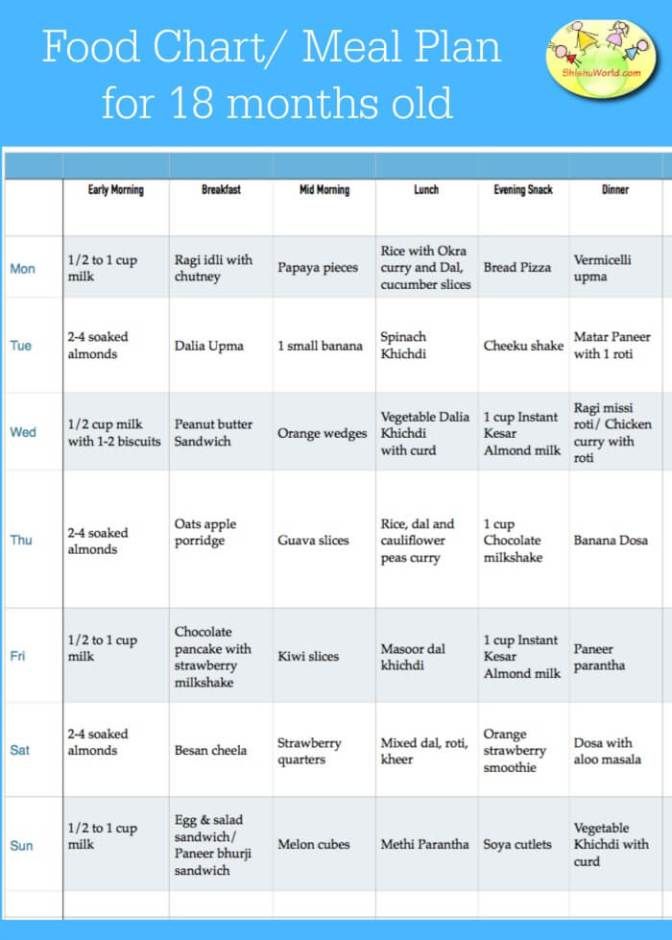
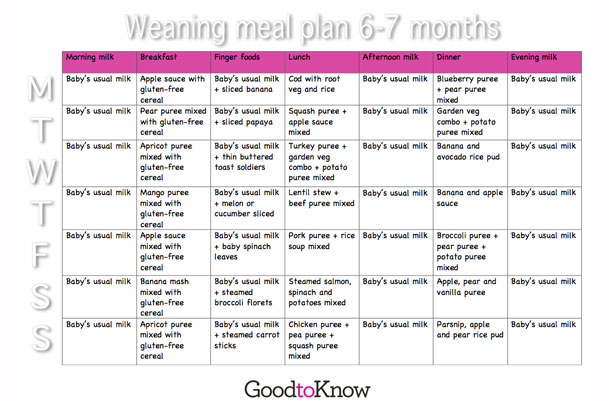
- Still not sure how to meet your baby’s iron needs once she’s accustomed to solid food? Just follow the baby nutrition recommendations in the chart below.3
Ironclad Reminders
- Breastfeeding is ideal ¾ and nature’s way of delivering iron to your baby for the first six months
- Always choose an iron-fortified infant formula if you decide to supplement or exclusively formula-feed
- Introduce iron-rich foods at around six months of age whether you're breastfeeding or formula feeding (just talk to your baby's doctor, first)
- Avoid whole cow's milk until at least nine to 12 months of age as it is a poor source of iron
- Be aware of the myths and know there is no scientific data that shows a correlation between iron-fortified formulas and gastrointestinal problems such as colic, constipation and fussiness
- Store all vitamin supplements that contain iron, including your prenatal and postpartum vitamins out of children's reach ¾ large amounts can be harmful to children
- If you suspect excessive iron intake, call your doctor or visit your local emergency room immediately.

Talk to your doctor about your baby’s iron needs and iron deficiency. Iron deficiency can cause your baby to be less active than usual, and perhaps even develop more slowly.
DHA and ARA
You’re probably aware of these two fatty acids that offer health benefits: DHA (you know it as docosahexaenoic acid, right?), an omega-3 fat, and ARA (arachidonic acid, of course), an omega-6 fat.
What makes them so important to baby nutrition?
Experts agree that DHA and ARA are essential for healthy brain and eye development4,5 (they actually accumulate in the brain and eye tissue of your baby before birth).
The earlier you can start getting DHA, a major brain-nourishing nutrient, the better—up to 90% of your baby’s brain growth will be complete by age three6.
How do I get them?
Your body will produce DHA and ARA from two essential omega-3 and omega-6 fatty acids: alpha-linolenic (ALA) and linoleic acid.
It all starts though, with your healthy diet—so eat foods rich in DHA5, like:
- Fatty fish: Atlantic salmon, herring, mackerel, sardines and cod are your best DHA bets (in that order).
- Omega-3 eggs fortified with DHA: A great substitute if you’re not a fish fan.
- Flaxseed and walnuts: Decent sources, yes, but you’ll only get a small amount of DHA once your body processes these.
How does my baby get them?
These nutrients are passed through your breast milk.
Your baby’s body produces them the same way yours does, from alpha-linoleic and linoleic acid that are added to all infant formulas. These essential fatty acids are also found in a variety of solid foods5. Plus, most infant formulas in Canada also contain DHA and ARA to support baby’s normal physical brain and eye development. Your healthcare professional can answer any more of your questions about DHA and ARA.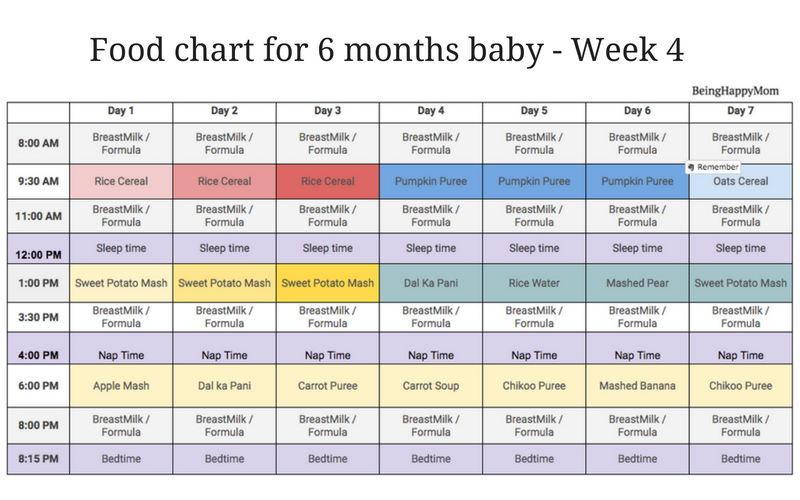
The Pros of Probiotics: Developing A Baby Nutrition Plan for Bolstering A Baby Immune System
Ah, yes, another miracle of nature—your baby’s developing immune system, it works hard as a:
- Shield from sickness and infection.
- Main support in her growth and overall health.
- Key in maintaining natural protective barriers.
The skin is obviously most important for protection, but another important barrier is the digestive tract, which is home to:
- 80% of the body's immune cells.7
- The gut flora, a delicately balanced community of around 500 different kinds of bacteria.
In a healthy digestive system, part of the task of keeping baby’s immune system and body safe from illness relies on good bacteria (or bacterial cultures)—they can also help to balance potentially harmful bacteria. One way to help support this protective barrier is to increase the levels of good bacteria in your baby’s digestive tract.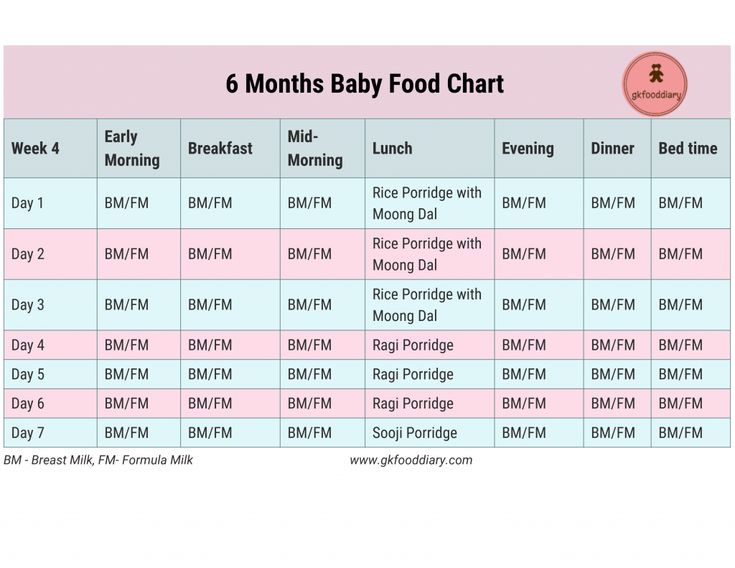
Recent research has shown that breast milk naturally contains probiotics including Bifidobacteria8,9 that:
- Are good bacteria
- Make up to 90% of the naturally occurring bacteria found in the gut flora of healthy, breastfed babies.10
- Aid in building a healthy digestive tract flora.
- Help with the healthy development of a strong immune system.11,12
These facts alone make it easy to see why breast milk is an ideal source of probiotics for your baby.
What are probiotics?
The meaning of “probiotic” is literally “for life”.
Probiotics are live, safe microorganisms, found in food and you’ll also hear them called “natural cultures” or “good bacteria”.
They offer specific health benefits, like aiding in digestion and supporting the immune system, when taken in adequate amounts.13
The probiotic Bifidobacterium lactis or B. lactis is a common type of Bifidobacteria and is recognized by Health Canada as a probiotic that contributes to baby’s healthy digestive tract flora.14 B. lactis has also been extensively studied for its baby nutrition benefits in infants.
lactis is a common type of Bifidobacteria and is recognized by Health Canada as a probiotic that contributes to baby’s healthy digestive tract flora.14 B. lactis has also been extensively studied for its baby nutrition benefits in infants.
Research suggests that, when ingested, probiotics only temporarily reside in the digestive system11,13,14 and continued, daily consumption of B. lactis is necessary for health benefits.14,15
B. lactis has been shown to help increase levels of antibodies, the immune protectors of your body, and an important part of a healthy baby's immune system and natural defences.15,16,17
¤ All breastfed, full term infants in Canada should receive a daily vitamin D supplement of 10 mg (400 IU).
Introduce First Food to your Baby
6 to 8 months
Article
Around the six-month mark, your baby will probably show signs of being ready for bites of their first food. This is unofficially called the “om-nom-nom” stage because it’s among the more common sounds you’ll hear from them around this time.
This is unofficially called the “om-nom-nom” stage because it’s among the more common sounds you’ll hear from them around this time.
6 mins to read Jul 31, 2017
2. Introduce new foods in the morning
You may find that morning is the best time to offer new foods because your baby is more likely to be hungry, happy and receptive to trying new things. Plus, you’ll have the full day to monitor for food intolerances or allergic reactions.
3. Offer small amounts at the beginning
Start slowly, with one to two teaspoons of food, and see how your baby does. You can offer more if they seem hungry and interested — it’s all they need for the first go-round.
4. Pay attention to texture
Your baby’s first food should be smooth in consistency and lump-free to prevent choking. Mixing solid food with breast milk or with infant formula may help with the consistency and also make it taste more familiar.
Instructions for first feedings with baby cereal: Place one tablespoon of cereal into a bowl and mix with three or four tablespoons of previously boiled, lukewarm water, breast milk or iron-fortified infant formula (depending on the cereal you’re trying). Mix in enough to make a runny mixture.
5. Experiment with temperature
Practise serving foods at different temperatures. But remember, too cold is unenjoyable and too hot is unsafe! Both would likely lead to a negative experience for both of you.
6. Get comfortable using a baby spoon
Dip the tip of a soft slim spoon into the food and offer it to your baby, but don’t force it in. Wait until they open their mouth. If they reach for the spoon, let them try it! They may even want to use their fingers to catch the food. You’ll succeed with a bit of patience.
Make mealtime fun: Positive reinforcement works. Saying “Yay! Good job!” in an excited and proud way will make your baby more likely to want to try the food again.
7. Cook everything thoroughly
Babies are more vulnerable than adults are to bacteria that can grow in food. Raw or undercooked meat, poultry/eggs or fish should never be offered to infants or young children.
8. Offer a new food for at least 2 days before introducing another one
In case of an adverse reaction, this delay will help you better identify the culprit. If this happens, stop feeding the food right away and talk to your baby's doctor.
9. Don’t get discouraged — it’ll come
It may take a few days before any food actually makes it into your baby’s tummy. That’s okay! Eating food is a skill you take for granted, but you had to learn it just as your baby does. Looking at, touching or smelling the food without eating it is common — these are all senses your baby’s still learning. Continue to pay attention to your baby’s hunger cues so you can breastfeed or formula feed accordingly. Learn more about your little one's hunger cues here.
Health experts advise not to delay the introduction of any specific solid food beyond six months of age, regardless of family history of allergy. You can introduce peanuts, soy, whole eggs, fish and wheat as you would any other food and monitor for allergic reactions. Consult your doctor if you have concerns about introducing solid foods or about allergies in your baby.
You can introduce peanuts, soy, whole eggs, fish and wheat as you would any other food and monitor for allergic reactions. Consult your doctor if you have concerns about introducing solid foods or about allergies in your baby.
Food for thought:
Always use a spoon, never a bottle, when feeding solids.
These foods are not appropriate for your little ones at the early stages of food introduction:
Choking hazards
Foods that are hard or crunchy, small and round shaped, or sticky can block your baby or small child’s airway. Be sure to prepare foods according to your child’s age and their ability to chew and swallow. And, you should always supervise your baby while they are eating.
Whole (3.25%) cow’s milk
Whole (homogenized) cow’s milk (3.25% milk fat) can be introduced between 9 and 12 months of age, once your baby is eating a variety of iron-rich foods. Cow’s milk is low in iron, can take up room in baby’s tummy and displace iron-rich foods, and can even inhibit iron absorption.
See why your baby isn't ready for cow's milk right away when they start solid foods.
Honey
Do not feed honey (pasteurized or unpasteurized) to infants under one year of age. Honey, including pasteurized honey, has been linked to a type food poisoning called infant botulism, and should not be added to baby foods or used on soothers, nipples or teething toys.
Sugar & salt
Avoid adding sugar and salt when preparing food for your baby. This will help your little one fully experience new foods and develop a taste for its natural flavours.
Sweetened beverages
Choose fruits and vegetables over fruit juice and avoid other sweetened beverages. You can also offer water regularly. For older babies no longer eating breastmilk or formula, their main milk source should be whole cow’s milk. Plant-based beverages don’t offer enough nutrition for toddlers under two, and raw or unpasteurized beverages are not safe for babies and toddlers. For more information on what to avoid, see Safe Food Handling: Making safe food choices for your baby.
Wondering which new foods to try? For more on foods appropriate for your little one, check out the Nestle Baby Feeding Guide.
Responsible promotion of baby food
Breastmilk is the optimal nutrition for babies, providing the best start in life. We promote, support, protect breastfeeding and are responsible for the marketing of breast milk substitutes. Nestlé manufactures high quality breast milk substitutes for use when there is a need for a safe alternative to breast milk, i.e. when mother's milk is not available to a breastfed baby or when specially adapted infant formulas are required. nine0003
Nestlé publicly declares its support for the WHO International Code of Marketing of Breast-milk Substitutes, which aims:
- to protect and promote breastfeeding;
- to ensure the correct use of breast milk substitutes when needed.
The Code recognizes the importance of breastfeeding and the legitimacy of the breastmilk substitute market in settings where breastfeeding is not possible. nine0003
nine0003
Our Commitment
Supporting and protecting breastfeeding with continued implementation of an industry-leading policy for the responsible marketing of breast-milk substitutes
Our approach
All of our actions in this area are based on WHO recommendations for breastfeeding support, especially with regard to the marketing of substitutes breast milk and creating favorable conditions for breastfeeding.
Breastfeeding support worldwide
We support breastfeeding with an industry-leading policy for the responsible promotion of breast-milk substitutes (BMS). Our strict Policies and Procedures for the implementation of the WHO International Code of Marketing of Breast Milk Substitutes apply in all countries where Nestlé operates. At a minimum, we comply with the provisions of the WHO Code implemented by the governments of the countries.
As of 2018, only 35 countries out of 194 have enacted laws or regulations that incorporate the full provisions of the Code. That's why, in 152 countries at high risk of child mortality and malnutrition, we follow the Nestlé Procedures if the company's requirements are more stringent than local regulations. We also support efforts to create an enabling environment for breastfeeding, for example by working with governments to ensure that breastfeeding rooms are accessible.
That's why, in 152 countries at high risk of child mortality and malnutrition, we follow the Nestlé Procedures if the company's requirements are more stringent than local regulations. We also support efforts to create an enabling environment for breastfeeding, for example by working with governments to ensure that breastfeeding rooms are accessible.
Compliance with the Nestlé Policy
All Nestlé employees involved in the marketing and sale of products regulated by the Policy know and strictly follow all of its provisions, as well as all partners and distributors of Nestlé products. All materials related to these products must comply with the rules established by the Policy. It is Nestlé's policy to prevent these products from being promoted at retail outlets.
Products covered by the Nestlé Policy
- All infant formula intended to feed healthy infants from birth to 12 months of age. nine0009
- Follow-up infant formula marketed openly for feeding healthy infants up to 12 months of age.
Unless required by national law, this Policy does not apply:
- Complementary foods, including cereals for infants, sterilized (or aseptically prepared) meats, vegetables, fruits and/or dairy products for infants, when provided on the market for feeding children over 6 months of age, provided that they do not contain instructions for their modification for use as a breast-milk substitute. This provision is intended to highlight Nestlé's commitment to exclusive breastfeeding for the first 6 months of life. nine0009
- To products intended for children of any age with special medical needs (eg, phenylketonuria, shortened or abnormal digestive tracts) or extremely preterm infants. Such children are unable to absorb, digest or metabolize breast milk or standard infant formula; they are under medical supervision and are at risk of death or malformation without access to such products. The text of the Policy can be found at the link. nine0009
How to stop breastfeeding | Philips Avent
search support iconSearch Keywords
Home ›› How to end breastfeeding comfortably for mom and baby
Home ›› How to end breastfeeding comfortably for mom and baby
9003 ↑ 05 ↑
When and how to stop breastfeeding? Like all good things, breastfeeding eventually comes to an end.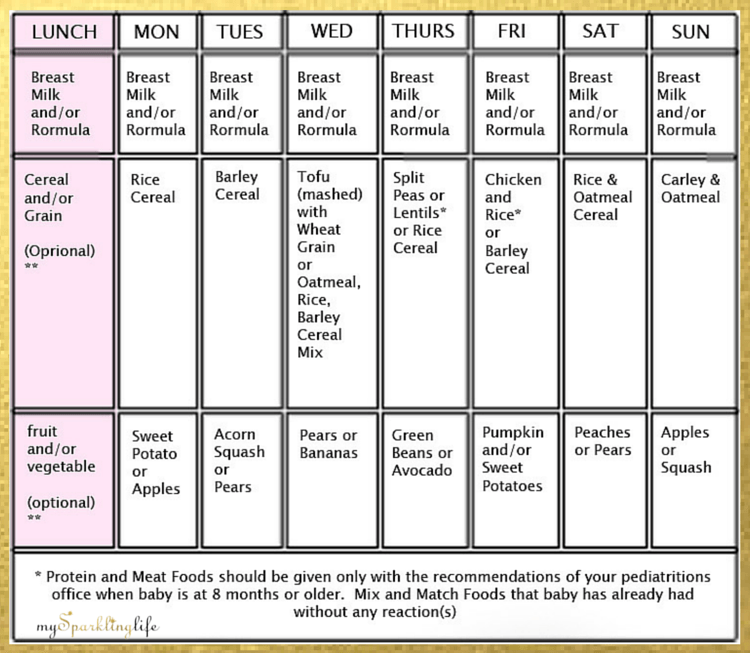 nine0008
nine0008
Weaning is an important decision for both mother and baby, and the decision is entirely up to them. When the mother and baby are ready to start weaning, there are a few tips and techniques to help make the transition a positive one.
3 Philips Avent products to help you stop breastfeeding:
When should I start weaning my baby? nine0057
There is no definite and correct period for weaning a child. The mother-child relationship is different for everyone, and weaning is a purely personal decision for mother and baby, which they make when both are ready.
The World Health Organization (WHO) recommends exclusive breastfeeding for infants up to six months of age. Until a child reaches the age of one year, both solid food and breast milk must be present in his diet. If the baby is weaned before he is one year old, adapted infant formula can be fed instead of breast milk. If a baby is stopped breastfeeding at one year of age or older, infant formula milk products can be given instead. While the recommendations are, many mothers stop breastfeeding before their babies are 12 months old, and others breastfeed for up to two years or longer. The second option is called extended breastfeeding, and it's a completely healthy choice for mothers and babies who want to continue breastfeeding. nine0003
While the recommendations are, many mothers stop breastfeeding before their babies are 12 months old, and others breastfeed for up to two years or longer. The second option is called extended breastfeeding, and it's a completely healthy choice for mothers and babies who want to continue breastfeeding. nine0003
Signs that a baby is ready to wean
Mothers often wonder how to stop breastfeeding, because babies rarely just stop suckling. Weaning a baby from the breast is usually a gradual process for both the mother and the baby.
There are several signs that will let you know that the baby is ready to start weaning:
- disinterest or fussiness during feeding; nine0009
- reducing the duration of feedings;
- child is easily distracted while feeding;
- the child plays while suckling, eg pulling or biting the breast;
- baby suckles lightly but does not extract milk.
How do I wean a baby?
When mom and baby decide it's time to stop breastfeeding, there are a few things to keep in mind to make the transition smoother. nine0008
nine0008
Here are our tips for weaning your baby when the time is right:
1. Wean gradually. When you decide to wean a baby, remember the main thing: do it gradually. This is necessary so that both mother and baby can adapt to physical and emotional changes. In addition, the gradual cessation of breastfeeding helps mothers avoid problems such as engorgement and general breast discomfort.
2. Express milk. To prevent breast engorgement when breastfeeding is stopped, the mother may need to express her milk, especially if the baby is less than a year old. One way to reduce and gradually stop breast milk production is to express less and less milk so that less milk is produced. Since pumping stimulates the flow of milk, it is important to use the pump for a shorter time than the duration of feeding the baby. Gradually, milk production will decrease and eventually stop completely. nine0008
Check out the Natural Motion Electronic Breast Pump, which combines nipple stimulation and pumping like a baby does for natural and gentle pumping.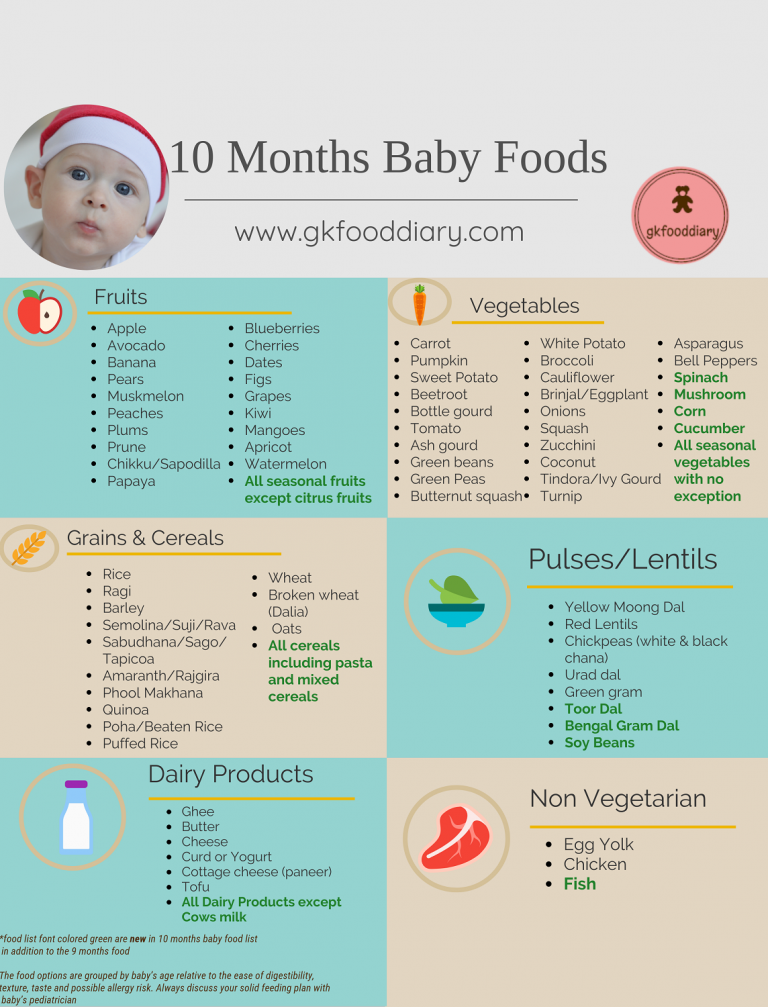
3. Reduce the number of daily feedings by one every week. We recommend eliminating one of the daily feedings each week, such as feeding at noon or at another time, depending on which one the child likes the least. The latter, as a rule, exclude feeding before bedtime and immediately after waking up. nine0003
During the weaning period, the mother's breasts will continue to produce milk until she completely stops breastfeeding.
During this period, mums will love these soft bra pads to keep their clothes dry and clean all day long.
Check out this Natural bottle with an ultra-soft, breast-like nipple to help make the transition from breast to bottle easier. nine0003
4. Extra hugs may be needed. In addition to the physical changes that stopping breastfeeding brings, moms and babies will also experience emotional changes. During this period, you should hug the baby more often and express your love to him. Caress and other acts of love can help mother and baby retain the closeness and togetherness that breastfeeding has given them.
5. Introduce complementary foods at your baby's usual feeding times. Another way to help your baby adjust to change is to give him complementary foods at his usual feeding times. Babies who are a year old or older can substitute cow's milk for breast milk or offer other foods if the baby has already switched to solid foods. nine0003
We also recommend watching the webinar "How to End Breastfeeding Comfortably and Painlessly: Tips and Tricks".
Although weaning is the natural end to breastfeeding, a mother can make a huge difference in her baby's life at this stage. Along with a new sense of pride in a child who is growing and developing, it is quite natural for a mother to feel sadness. Breastfeeding creates a special bond between mother and baby. Therefore, breastfeeding mothers often find it difficult to say goodbye to breastfeeding. nine0008
If you have any questions, be sure to ask a specialist for their opinion.
Articles & tips from Philips Avent
Baby+ app
Download the app and track your baby's development and growth with trackers and keep those special moments forever.











