Trying to bottle feed a breastfed baby
Introducing a Bottle to a Breastfed Baby
The information in this post is also contained in our Working & Breastfeeding.
Here is one approach to beginning pumping and introducing bottles that has worked well for many mothers as they prepared to return to work:
- Once breastfeeding is well established – usually after about four weeks – begin pumping after one feeding a day where your breasts still feel a little full. Remember you are pumping “leftovers” and should only expect a small amount.
- Freeze that first pumping immediately. You can add other pumpings to it after they have been cooled in the freezer.
- Your pediatrician may have given you a total number of ounces your baby may feed in a day or a range from the smallest probable amount to the largest, based on your baby’s weight.
- If dealing with a total volume over a 24-hour period, divide that by the typical number of times your baby feeds for a target volume for the first bottle.
- If dealing with a range, store volumes of the lower amount.
- Store some extra small volumes in case baby is hungrier than expected.
- When you have enough stored to equal the expected volume and a bit more, you can begin to plan a time to introduce a bottle.
- EXAMPLE for offering the first bottle:
- Your pediatrician suggests that your baby probably takes about 24 ounces a day.
- You know that he feeds between eight and 12 times a day.
- That means he could take anywhere from 2 to 3 ounces.
- You pump until you have a 2-ounce bottle and then have several 1/2 ounce bottles to equal at least three ounces or more saved.
- Choose a day that your primary support person will be available and a feeding time where baby tends to be more pleasant and patient for his feeding.
- Baby may accept a bottle more easily from someone other than you. He knows milk comes from you and may not understand why he’s not going there instead of to this foreign object.

- Thaw out the 2-ounce bottle in the refrigerator overnight.
- When baby begins to stir, place the bottle from the refrigerator in a bowl of warm water (bath temperature) or a bottle warmer while the person offering the bottle goes to get baby from his bed, changed and ready for the feeding.
- Often it helps to run the bottle nipple under warm water, if it was also in the refrigerator, to make it more acceptable to the baby.
- Baby should be held in an upright, almost sitting, position that is similar to the position usually used by the support person.
- The warmed bottle should be held at an angle tilted just enough to fill the nipple to allow baby to keep control of when and how fast the milk comes.
- Tickle the baby’s mouth to encourage an open mouth then bring baby up onto the bottle nipple, aiming the nipple toward the palate.
- Some have found that it can help to have an article of clothing you have worn, like a nightgown or t-shirt, to place on their arm, shoulder, or chest where the baby can smell your scent.

- It is usually best if you are close but not present in the room during this first “experiment” with bottle feeding. Your baby is very wise and will wait for you to come feed her if she knows you are nearby.
- If dealing with a total volume over a 24-hour period, divide that by the typical number of times your baby feeds for a target volume for the first bottle.
Once the feeding is completed, you will pump to create a bottle equal to what the baby consumed. Remember that the baby is always better than a pump! If you do not pump as much as the baby took, it is more likely a pump issue than an issue of not enough milk. Just pump after another breastfeeding and add that amount to what you pumped to get the amount baby took.
You will continue this pattern until you have enough milk stored in your freezer to get you through a normal work day plus a few extra for any hectic day at work where you may not have been able to pump as often. Plan to fully breastfeed for all feedings when not separated from your baby.
Working and Breastfeeding
Feeding Breastmilk From a Bottle
Pumping
Cleaning and Sanitizing Pumping Accessories
Hand Expressing
Published August 2018.
When and how to introduce a bottle to your breastfed baby
Wondering how to introduce a bottle to your breastfed baby? Wait until 3 to 4 weeks postpartum to ensure your milk supply is well established. Have someone else make the first few attempts if possible. If your baby won't take the bottle, try varying the bottle and nipple temperature, moving around, and switching positions. Though some breastfed babies reject bottles vociferously, which can be a real challenge for parents and caregivers, many will come around.
You may be planning to give your breastfed baby bottles because you're pumping breast milk, supplementing with formula, or switching to formula feeding. The transition can be tricky, but there are ways to make it easier. Here's what you need to know to successfully introduce a bottle to your breastfed baby.
When to introduce the bottle to your breastfed baby
If you're breastfeeding, most experts suggest waiting until your baby is 3 to 4 weeks old and breastfeeding is well established before introducing a bottle. In addition to helping launch your milk supply, waiting a few weeks helps reduce the risk of nipple confusion, or a preference for bottles over the breast.
In addition to helping launch your milk supply, waiting a few weeks helps reduce the risk of nipple confusion, or a preference for bottles over the breast.
Exactly when to first introduce the bottle varies depending on whether you're bottle feeding because you'll be separated from your baby, or because you need to add formula to your routine.
If you're returning to work after maternity leave, start bottle-feeding several weeks before you go back. That way, you'll have plenty of time for them to adjust to the bottle.
If you're pumping breast milk, you'll want to keep up your milk supply by pumping every time your baby has a bottle. If you can, use a double electric breast pump: It's the most efficient way to express milk and stimulate milk production. (These are usually free through insurance.)
If breastfeeding isn't going according to plan for you and you're thinking about supplementing your baby's diet with formula or switching to exclusively formula feeding, try talking with a lactation consultant before making any big changes. A lactation consultant can assess why you're having trouble breastfeeding and offer tricks to address challenges.
A lactation consultant can assess why you're having trouble breastfeeding and offer tricks to address challenges.
But there's no need to feel guilty if you make the switch to formula: Healthy and happy babies can be formula-fed or breastfed. Focus on nourishing your baby and giving them the love, attention, and cuddles they need to thrive.
How to bottle feed a baby
Sucking milk from a bottle requires different mouth and tongue movements than breastfeeding, so it may take your baby a little time to get used to the change. Try these tips for a smooth transition.
Offer a bottle in place of a regular feeding. Choose a time that your baby tends to not be too fussy at mealtime – say, in the morning. The amount of formula or breast milk you'll need to give at each feeding varies depending on your baby's age and weight. Our articles on how much formula and breast milk babies need break it down for you, and you can always ask your pediatrician for a recommendation if you're not sure.
Or, offer the bottle after a regular feeding. If you're especially anxious about offering the bottle, or if your baby balked at the bottle in place of the breast on your first attempt, you may want to get them used to the nipple by offering the bottle an hour or two after they're already fed. That way your baby won't be frenzied for food and may be more open to experimenting with a new food source. Start with a small amount of breast milk – about 1/2 ounce.
Let someone else feed them the first bottle. If you try to give your baby their first bottle, they may wonder why they're not getting your breast. They may be less confused if someone else makes the introduction. Ask your partner, a grandparent, a childcare provider, or a friend to help. Choose a spot other than where you regularly breastfeed.
Make sure the bottle is the right temperature. Breastfed babies can be particular about the warmth of their milk; many prefer milk that's the temperature of your body or a bath (about 98 degrees Fahrenheit). You can soak the bottle in a bowl of hot water or use a bottle warmer to bring it up to temperature.
You can soak the bottle in a bowl of hot water or use a bottle warmer to bring it up to temperature.
Stay away. A baby can smell their mother, even from a distance, so they may know that you (and your breasts) are nearby. If your baby refuses a bottle with you nearby, try going to a different room during feedings.
Don't force it. The first time you introduce the bottle, don't force the nipple into your baby's mouth. Try tickling your baby's upper lip and nose with the nipple and then letting your baby "latch" onto the nipple as they would with your breast. If your baby seems frustrated or hasn't eaten anything after 10 minutes, stop and try again the next day.
Try paced (or responsive, or cue-based) feeding. This method slows down the flow of milk to mimic breastfeeding and reduce the chances that your baby will drink too much. Use a slow-flow nipple, keep the bottle horizontal, pause every 20 to 30 seconds during feedings, and switch sides as you would when breastfeeding.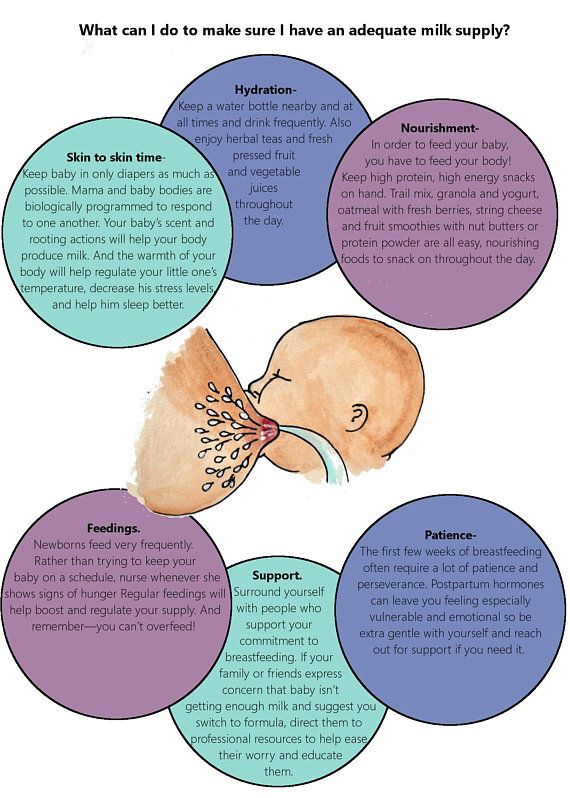 Stop feeding your baby when they show signs of being full, which include not sucking anymore and turning away from the bottle. Research suggests a responsive feeding style encourages healthy eating habits that last well beyond the bottle.
Stop feeding your baby when they show signs of being full, which include not sucking anymore and turning away from the bottle. Research suggests a responsive feeding style encourages healthy eating habits that last well beyond the bottle.
Bond with your baby. Talk to your baby and look into their eyes as you bottle-feed to bond and help them feel secure. You can even take off your shirt for skin-to-skin contact, which helps babies to relax while stimulating digestion and interest in feeding, among other benefits.
Be patient. It may take a while for your baby to accept the bottle.
Be consistent. Babies love routines, so aim to give the bottle the same time every day.
What to do if your baby won't take a bottle
Some babies take to the bottle without much fuss, but others struggle quite a bit with the transition.
Make sure you have lots of time and take it slow during this process. If your baby starts crying and pushes the bottle away, back off, comfort them, and then try again. If you've tried offering the bottle several times and your baby seems frustrated, or if they refuse to eat for 10 minutes, let it go for now. (Wait at least five minutes before breastfeeding after an unsuccessful bottle-feeding – that way they won't associate refusing the bottle with immediate gratification.)
If you've tried offering the bottle several times and your baby seems frustrated, or if they refuse to eat for 10 minutes, let it go for now. (Wait at least five minutes before breastfeeding after an unsuccessful bottle-feeding – that way they won't associate refusing the bottle with immediate gratification.)
Offer the bottle again in an hour or two, when your baby is alert and receptive but not very hungry.
If your baby is having a hard time, try these techniques:
- Test a few different nipples. Babies can be very particular about bottle nipples. If you've tried the bottle a couple of times and your baby still refuses to eat, test out a few other options. Your baby may prefer a wide-based nipple, which more closely simulates the breast. Or your baby may accept a nipple that's similar to the pacifier they use (if you use one), so try giving them a nipple that's the same shape or made out of the same material as the pacifier.
- Change the temperature of the nipple.
 If your baby is teething, they may prefer a nipple that's been chilled in the fridge. Otherwise, try warming the nipple under running water.
If your baby is teething, they may prefer a nipple that's been chilled in the fridge. Otherwise, try warming the nipple under running water. - Introduce breast milk outside of the bottle. Put a few drops of breast milk on your baby's lips or the nipple before feeding them from a bottle, to give them a preview of what's to come. When your baby tastes it, they may start sucking to get more.
- Let your baby play with the nipple so they can get familiar with it. If your baby just chews on it at first, don't worry. They may actually start sucking on it soon.
- Hold them in a different position during the feeding. Put your baby in an infant or car seat so they're semi-upright, and then feed them the bottle while you're facing each other. Or try feeding them on your lap with their back to your chest. Once your baby is used to taking a bottle, you can hold them in a more standard feeding position.
- Move around. Try walking or lightly bouncing your baby. Gentle, rhythmic movement may encourage them to take the bottle.

- Try different temperatures. Your baby might prefer milk that's slightly warmer or colder. Experiment with different temperatures to see what they prefer.
- Check the taste. Expressed breast milk sometimes has a soapy taste, so you may want to try a drop.
- Offer the bottle at other times of day. If your baby won't take the bottle during the day, offer it during a nighttime feeding or vice versa.
If your baby is still refusing the bottle
For most babies, bottle refusal is a short-lived developmental step. That's why it's best to give everyone time to transition by introducing the bottle well before you have to go back to work or otherwise be separated from your baby.
If your baby continues to refuse the bottle, keep trying: It can be frustrating, but your baby may eventually accept it. Until they do, you may have to make serious adjustments to your life. Some working moms have had to extend their maternity leave, change jobs, work from home with a nanny or sitter, or visit their child's daycare every two to three hours to breastfeed their bottle-refusing baby.
If you've tried everything, don't blame yourself if your baby still won't bottle-feed. Some babies never take to the bottle – but talk to your child's doctor to rule out a medical reason.
Some babies can learn to drink from an open cup or a sippy cup instead of a bottle. Make sure your baby can hold their head up on their own before trying (usually around 4 to 6 months), though, to reduce the risk of choking. Here's how to start using a sippy cup:
- Support your baby's head and shoulders with your arm and sit them upright in your lap.
- Place the cup on your baby's lower lip and tilt it until the milk or formula is close to their lips.
- Wait until your baby laps up the milk with their tongue, which may take a few minutes. Don't pour the milk straight into your baby's mouth.
- Continue to offer the milk until your baby turns away their head or offers other cues that they're finished.
- You may want to try this method first with another adult for practice.
 Once you're ready to test it out on your baby, be prepared with a bib and burp cloth nearby to wipe up spills.
Once you're ready to test it out on your baby, be prepared with a bib and burp cloth nearby to wipe up spills.
advertisement | page continues below
Baby won't take the bottle | Philips Avent
search support iconSearch Keywords
Home ›› What to do when your baby refuses a bottle
↑ top
any problems. If your breastfed baby refuses a bottle, don't worry. This is a common occurrence in many babies who are used to breastfeeding. Obviously, this can create certain difficulties for moms, especially if you need to return to work in the near future.
3 Philips Avent products to help you bottle feed:
So why is your baby refusing to bottle and crying? There are many ways to quickly and easily teach a breastfed baby to a bottle. Here are important tips on what to do when your baby refuses a bottle.
Is the baby refusing the bottle? Take a step back
If your baby cries while bottle feeding, the first thing to do is to start over and rethink your feeding approach and technique. Try the following steps when bottle feeding your baby: [1]
Try the following steps when bottle feeding your baby: [1]
- Lift and tilt your baby's head forward. Before inserting the pacifier into the baby's mouth, make sure that the baby's head is raised and tilted over his body to avoid choking: so that the baby does not choke and have the opportunity to burp during bottle feeding.
- Insert the pacifier. Bring the pacifier to the baby's lips and gently guide it into the baby's mouth. In no case do not try to press the nipple on the baby's lips and try to push it into his mouth. After touching the pacifier to the baby's lips, wait for the baby to open his mouth and take the pacifier.
- Hold the bottle at an angle. Tilt the bottle at an angle so that the nipple is only half full. So the child can eat at his own pace.
- Let the baby burp during and after feeding. It can be useful for a child to burp not only after feeding, but also approximately in the middle of the process. This will help reduce gas or tummy discomfort that your baby may experience from swallowing too much air.

- Stop in time, do not overfeed the baby. If the baby begins to turn his head away from the bottle or closes his mouth, then he is full and you need to stop feeding.
- Perhaps the flow of milk from the nipple to the baby is weak or, on the contrary, too fast, so he is naughty and refuses the bottle. Try changing the nipple to a nipple with a different flow.
Other tips if your baby refuses the bottle
If you've followed the steps above and your baby still refuses the bottle, don't worry. There are other ways to help bottle feed your baby. Here are some simple tricks you can add to your bottle feeding process. [2]
1. Remind your child about mom.
Sometimes a child can be fed by someone other than his mother - dad, grandmother or, for example, a nanny. If your baby fusses while bottle feeding, try wrapping the bottle in something that smells like mommy, like a piece of clothing or some fabric. This will make it easier to feed the baby when the mother is not around.
This will make it easier to feed the baby when the mother is not around.
2. Try to maintain skin contact while bottle feeding.
Some babies need contact with their mother, so try bottle feeding while leaning against you. However, some babies are better at bottle feeding when they are in the exact opposite position than when they are breastfed. For example, there is a position with bent legs. Lay the child on your bent knees, facing you, pointing the child's legs towards your stomach. During feeding, the baby will be able to look at you and contact you in this way. If your baby refuses a bottle, experiment to see which works best.
3. Move while feeding.
Sometimes all it takes to get your baby to take the bottle is a little wiggle or walk. The next time your baby starts crying while bottle feeding, try moving around a little rhythmically to calm him down.
4. Try changing the milk temperature.
Try changing the milk temperature.
If the baby still does not want to take the bottle, check if the milk in the bottle is too hot or too cold. Before feeding, put some warm breast milk on the inside of your wrist to check the temperature. Milk should be warm, but if it seemed hot to you, just place the bottle for a short while under a stream of cold water.
Choosing the right bottle for your baby If you plan to combine bottle feeding with breastfeeding, it is advisable to choose bottles with a nipple that will have a wide base as the bottle will grip closer to the breast. Also pay attention to the fact that the nipple is firm and flexible, the child must make an effort to drink from the bottle, as well as from the breast. Give preference to nipples with an anti-colic valve that vents air out of the bottle.
Natural bottle allows you to combine breast and bottle feeding. 83.3% of babies switch from a Natural bottle to breastfeeding and back. *
*
If you choose a bottle for artificial feeding, traditional bottles are fine, but it is desirable that the nipple is made of a hypoallergenic material, such as silicone, has an anti-colic valve and did not stick together when bottle fed. In case your baby spit up often, then use special bottles with anti-colic and anti-reflux valve, which reduces the risk of spitting up and colic.
Bottle with unique AirFree valve reduces the risk of colic, gas and spitting up. With this bottle, you can feed your baby in an upright or semi-upright position to reduce spitting up. Due to the fact that the nipple is filled with milk and not air during feeding, the baby does not swallow air, which means that feeding will be more comfortable.
Both bottles are indispensable if you want to breastfeed, bottle feed or just bottle feed your baby.
“My baby refuses to breastfeed but bottle feeds – help!”
Sometimes a baby gets used to bottle feeding and refuses to breastfeed. Therefore, it is important to use bottles that are suitable for combining breastfeeding with bottle feeding. If, nevertheless, you are faced with the fact that the child refuses to take the breast, try using silicone nipple covers to make the transition from the bottle to the breast and back more imperceptible.
Therefore, it is important to use bottles that are suitable for combining breastfeeding with bottle feeding. If, nevertheless, you are faced with the fact that the child refuses to take the breast, try using silicone nipple covers to make the transition from the bottle to the breast and back more imperceptible.
Remember that if you want to combine breastfeeding and bottle feeding, it is worth waiting at least a month before offering a bottle, so that you are lactating and have time to get used to each other and develop a breastfeeding regimen.
Breastfeed and bottle feed your baby with pleasure
Remember that it takes a while for your baby to get used to bottle feeding. This is completely normal. If you have to go to work, be sure to set aside enough time to bottle train your baby beforehand.
Remember that every child is different, so what works for one may not work for another. With a little time and patience, you will find out what works best for your baby when he refuses a bottle.
You will identify your child's unique needs. However, if your baby still refuses the bottle after all the steps above, check with your pediatrician.
Articles and tips from Philips Avent
References:
*O.L. Lukoyanova, T.E. Borovik, I.A. Belyaeva, G.V. Yatsyk; NTsZD RAMS; 1st Moscow State Medical University THEM. Sechenova, "The use of modern technological methods to maintain successful breastfeeding", RF, 10/02/2012 3 llli.org - The Baby Who Doesn't Nurse
llli.org - Introducing a Bottle to a Breastfed Baby
Baby+ app
Download the app and track your child's development and growth with trackers and save those special moments forever.
Download app:
You are leaving the Philips Healthcare (“Philips”) official website. Any links to third party websites that may be included on this site are provided solely as a convenience to you. Philips makes no warranties regarding any third party websites or the information they contain.
I understand
You are about to visit a Philips global content page
Continue
You are about to visit the Philips USA website.
I understand
Bottle feeding
Establishing breastfeeding is one of the most significant processes for a mother in the first month after the birth of a baby. This is a sacrament in which a lot of important moments for the development of the baby are hidden: ideal food for the baby, contact between the baby and the mother, normalization of sleep. In addition, for many mothers, this is a very pleasant and healing process in the postpartum period. The release of the hormone oxytocin contributes to the contraction of the uterus and the restoration of its former shape. The production of milk by the body helps mom lose extra pounds. Long-term breastfeeding acts as a prophylactic against a number of female diseases.
However, not everyone succeeds in easily coping with this process (albeit natural). In the first month, many women may experience difficulties: unprepared nipples, irregular or insufficient milk production, etc. These problems are the norm and should not become a reason for the growth of anxiety and self-blame. Most likely, in a month the process will improve. But even if this is not the case, alternative options can be used, for example: feeding with expressed milk from a bottle or supplementing with formula. In any case, it is worth remembering: you are the best mother for your child.
In the first month, many women may experience difficulties: unprepared nipples, irregular or insufficient milk production, etc. These problems are the norm and should not become a reason for the growth of anxiety and self-blame. Most likely, in a month the process will improve. But even if this is not the case, alternative options can be used, for example: feeding with expressed milk from a bottle or supplementing with formula. In any case, it is worth remembering: you are the best mother for your child.
At what age can you bottle feed your baby with expressed milk?
If there is significant difficulty in breastfeeding, you can use the bottle almost immediately. Today, a feeding bottle with a teat labeled "0+" is available in every pharmacy or baby store. There are bottles of foreign and domestic manufacturers on sale (for example, DINO & RHINO bottles are produced in Russia).
Bottle feeding may also be recommended if the baby is not suckling well at the breast, has a weak latch on the nipple, and is not gaining weight (this is sometimes the case with babies who were born a little early).
In other cases, in the first month it is recommended to establish a natural process of breastfeeding. In the future, you can use the bottle as an aid, for example, if you need to go away on business, and leave the child with dad, grandmother, nanny.
How to feed your baby with expressed milk?
To begin with, the bottle must be sterilized. How to do it correctly, you can read in our other article. Then fresh or thawed, warmed to body temperature (37 ° C) expressed breast milk is poured into a bottle, and the baby sucks it out through the nipple.
Modern bottle nipples are designed so that when sucking, the baby must make the same movements and efforts as when sucking milk from the breast. The nipples have a flow rate close to the anatomical shape and the actual age of the baby. They are made from safe and hypoallergenic BPA-free materials, so you don't have to worry about your child's health.
How to offer the baby a bottle for the first time and teach the child to eat from it?
Usually this does not cause difficulties, many children begin to actively drink from a bottle the first time.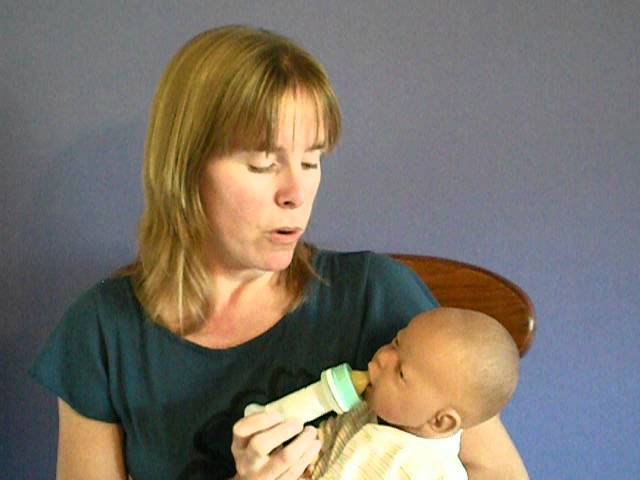 But sometimes it takes several tries. The baby may push the pacifier away, crying is normal. Try again and again.
But sometimes it takes several tries. The baby may push the pacifier away, crying is normal. Try again and again.
To offer a bottle for the first time, wait until the baby is hungry (but not too hungry) and bring the nipple to the mouth in the same way as you do with the breast nipple, at the same angle. Lightly touch her lips to the child so that he opens his mouth. The optimal position of the baby when feeding is reclining.
If up to this point you have been breastfeeding for a long time and the child has a clear connection in the head (mother - breast), ask one of the relatives to offer him a bottle, so he will not be distracted by your smell and expect the usual way of feeding.
If the baby does not want to take the nipple in any way, dip its tip in expressed milk, perhaps he will readily react to the smell.
If he wants to pause, listen to his desire.
How much expressed milk should you give your baby?
There are norms recommended by pediatricians: how many ml of milk a child of one age or another should eat. For example, at the stage of 1-6 months, the average child should eat 50-230 ml of milk per meal (you can find a detailed table by month in the relevant reminders). But there is also an individual norm. If your child eats less or more than the average amount, but is healthy and developing well, there is no reason to worry.
For example, at the stage of 1-6 months, the average child should eat 50-230 ml of milk per meal (you can find a detailed table by month in the relevant reminders). But there is also an individual norm. If your child eats less or more than the average amount, but is healthy and developing well, there is no reason to worry.
How to make bottle feeding as safe as possible?
- Choose a nipple with an age-appropriate flow and ensure your baby is in the correct feeding position to prevent choking.
- Sterilize the nipple, bottle, and pump before each feeding during the first few months of your baby's life.
- Be sure to wash your hands before feeding and pumping.
- Store expressed milk correctly: no more than 4 hours at room temperature. If you need to store longer, use the refrigerator or freezer.
Can I alternate between breastfeeding and bottle feeding?
Yes, for most children this does not cause discomfort. Although there are babies who eventually choose only one way: breast or bottle.











