Breast pain during feeding baby
Breast pain and breastfeeding - NHS
There are a number of reasons why you may experience breast pain while you're breastfeeding.
Always ask for help from your midwife, health visitor or breastfeeding specialist if you're having problems breastfeeding.
Here's how to deal with some of the most common causes.
Breast engorgement
Breast engorgement is when, for whatever reason, your breasts become overly full. They may feel hard, tight and painful.
In the early days, engorgement can be due to your milk coming in. Newborns need feeding little and often. It can take a few days for your milk supply to match your baby's needs.
If your baby is not well attached to the breast, it may be hard for them to take your milk when your breast is engorged.
The nipple can become a little overstretched and flattened, and possibly painful.
Ask your midwife, health visitor or a breastfeeding specialist for advice immediately to help your baby relieve the engorgement and prevent it happening again.
Find out more about positioning and attachment
Engorgement can still happen once you have learnt the skill of positioning and attachment, usually when your baby has not fed for a while.
Your baby usually knows when they need a feed, for how long and from which breast.
Early signs (cues) that your baby is ready to feed can include:
- moving their eyes rapidly
- putting their fingers into their mouth
- rooting (turning to 1 side with their mouth open as if seeking the breast)
- becoming restless
Crying is the very last sign that your baby needs feeding.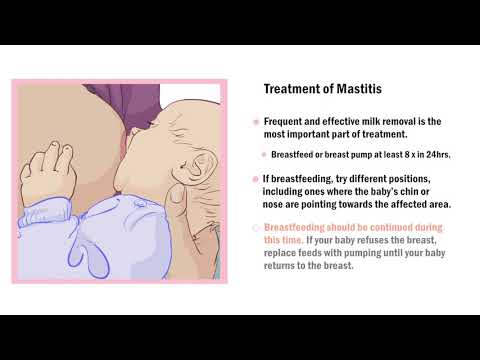 Feeding them before they cry often leads to a much calmer feed.
Feeding them before they cry often leads to a much calmer feed.
Keeping your baby close so you can watch and learn their early feeding cues will help.
How to ease breast engorgement
To ease the discomfort of engorgement, apart from your baby feeding, you could try expressing a little breast milk by hand. Only express enough to relieve the discomfort because expressing more will make you produce more milk.
Ask your midwife, health visitor or breastfeeding specialist to show you how.
Find out more about expressing breast milk
You may also find it helps to:
- wear a well-fitting breastfeeding bra that does not restrict your breasts
- put warm flannels on your breasts just before hand expressing if they're leaking
- take some paracetamol or ibuprofen at the recommended dose to ease the pain (these are safe to take while you're breastfeeding)
Too much breast milk
Occasionally women make too much breast milk and their babies struggle to cope.
It's best to get your midwife, health visitor or breastfeeding specialist to watch a feed to see if they can spot why this is happening.
They can also suggest ways to decrease your supply.
Blocked breast milk ducts
The milk-making glands in your breasts are divided up into segments, rather like an orange.
Narrow tubes called ducts carry the milk from each segment to your nipple.
If one of the segments is not drained properly during a feed (perhaps because your baby is not attached properly), this can lead to a blocked duct.
You may feel a small, tender lump in your breast.
Avoid wearing tight clothes or bras so your milk can flow freely from every part of your breast.
Other things that may help include:
- frequent feeding from the affected breast
- warm flannels or a warm shower to encourage the flow
- gently massaging the lump towards your nipple while your baby feeds
It's important to deal with a blocked duct quickly as, if left, it could lead to mastitis.
Mastitis
Mastitis (inflammation in the breast) happens when a blocked duct is not relieved.
It makes the breast feel painful and inflamed, and can make you feel very unwell with flu-like symptoms.
If you do not deal with the early signs of mastitis, it can turn into an infection and you'll need to take antibiotics.
Symptoms of mastitis include:
- a breast that feels hot and tender
- a red patch of skin that's painful to touch
- a general feeling of illness, as if you have flu
- feeling achy, tired and tearful
- a high temperature
If you think you're developing a blocked duct or mastitis, try the following:
- Carry on breastfeeding.

- Check your baby's positioning and attachment. Ask your midwife, health visitor or a breastfeeding specialist to watch a feed.
- Let your baby feed on the tender breast first.
- If the affected breast still feels full after a feed, or your baby cannot feed for some reason, express your milk by hand.
- Warmth can help the milk flow, so a warm flannel, or a warm bath or shower, can help.
- Get as much rest as you can. Go to bed if you can.
- Take paracetamol or ibuprofen to relieve the pain.
Contact your GP or NHS 111 if you feel worse at any time, or if you're no better within 12 to 24 hours.
You may need antibiotics, which will be fine to take while breastfeeding.
Stopping breastfeeding will make your symptoms worse, and may lead to a breast abscess.
Breast abscess
If a mastitis infection is not treated, it can lead to a breast abscess, which may need an operation to drain it.
This can also develop if the mastitis does not respond to frequent feeding plus a course of antibiotics.
You can carry on breastfeeding after an abscess has been drained.
Find out more about breast abscesses
Thrush
If you experience pain in both breasts, often after a period of pain-free breastfeeding, and the pain lasts for up to an hour after a feed, you may have developed thrush.
Find out more about thrush and breastfeeding
Got a breastfeeding question?
Chat to the Start4Life Breastfeeding Friend on Amazon Alexa, Facebook Messenger or Google Home for fast, friendly, trusted NHS advice any time, day or night.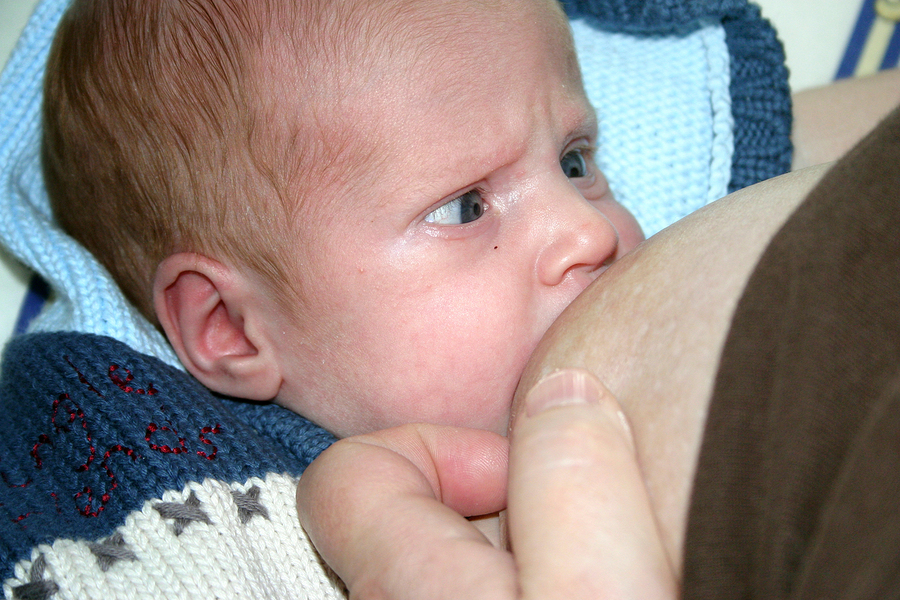
Breastfeeding FAQs: Pain and Discomfort (for Parents)
Breastfeeding is natural, but it takes practice to get it right. Here's how to handle pain and discomfort during nursing.
Is It Normal to Have Cramps While Breastfeeding?
Yes. During the first few days to weeks after delivery, you may feel strong, menstrual-like cramps in your uterus when your milk “lets down” (starts to flow). This is your uterus shrinking back to a smaller size.
Is It Normal for My Breasts to Get Engorged?
During the first 2–5 days after birth, it’s normal to have engorged (very full) breasts as your milk supply increases. But if your baby nurses (or you pump) every 2–3 hours, your breasts should not feel engorged.
Engorgement can lead to sore, painful breasts or a breast infection. So it’s best to try to avoid it. The longer you wait to breastfeed or pump, the more uncomfortable and engorged your breasts may get.
If you can't feed your baby right away, use warm compresses and try to pump or manually express your milk. One way to express milk is to put your thumb on top of your areola and a finger below it. Gently but firmly press your thumb and fingers back against your chest wall. Then compress your fingers together to express (push out) your milk.
One way to express milk is to put your thumb on top of your areola and a finger below it. Gently but firmly press your thumb and fingers back against your chest wall. Then compress your fingers together to express (push out) your milk.
Is It Normal to Feel Pain During or After Breastfeeding?
When babies latch on properly, some moms feel a few moments of discomfort at the very beginning of a nursing session. After that, discomfort should ease. You may feel a gentle tug on your breasts while your baby feeds, but it shouldn’t hurt.
If you feel discomfort during nursing, stop nursing and reposition your baby to get a better latch. Your nipple areola (the ring around the nipple) should be mostly in your baby’s mouth. When babies are latched on wrong, it can hurt or feel like a pinch each time your baby sucks. Over time, this can lead to painful, sore, cracked nipples.
If you have pain during breastfeeding, talk to your doctor or lactation consultant to make sure your baby is properly latched or that something else isn't going on.
What Else Can Cause Breast Pain?
The most common causes of breast pain include:
A plugged milk duct. Sometimes milk ducts get plugged. You may feel pain in an area of your breast or a lump may form under the skin where the duct is plugged. To help unclog the duct and ease pain:
- Take warm showers or use warm compresses on the area. Massage the area several times a day. Then, breastfeed your baby right away.
- Position your baby’s chin so that it points toward the clogged area during feeding. This will help that area of the breast empty sooner.
- Gently massage the lump while your baby feeds. It may take 2 to 3 feedings for the lump to go away. You also can use a manual (hand) or electric pump for a few minutes to help draw out the clogged milk while gently massaging the area.
- Apply cold compresses (ice wrapped in a thin towel) between feedings.
- If the lump doesn't go away within a couple of days, or if you have a fever, chills, aches, or red streaking, call your doctor.

Mastitis. This is an inflammation of the breast. If your breasts are sore; have red streaks; or have a hard, red area, you may have mastitis. Some women also get a fever and chills. If you think you have mastitis, call your doctor. In the meantime, continue to breastfeed or pump to drain the milk from your breasts. Switch between warm compresses and gentle massage right before breastfeeding and then apply cold compresses after a session. Mastitis caused by an infection may need treatment with antibiotics.
Oral thrush. Sometimes babies develop a yeast infection in the mouth called oral thrush. Babies with this have cracked skin in the corners of the mouth, and whitish or yellowish patches on the lips, tongue, or inside the cheeks. The infection can spread to your breast and cause:
- shooting or burning breast pain either during or after feedings
- pain deep within your breast
- strong pain in the breasts or nipples that doesn't get better after your baby properly latches on or you reposition your baby
- nipples that are cracked, itchy, burning, or are pink, red, shiny, flaky, or have a rash with little blisters
Call your doctor if you or your baby have any of these symptoms.
Inverted or flat nipples. Women who have inverted nipples (nipples that turn in rather than stick out) or flat nipples (that don't become as erect as they should when a baby is nursing) may have a harder time breastfeeding or have nipple pain. If either is the case, talk to your doctor or a lactation consultant about ways to make nursing easier and reduce any pain.
How Can I Ease Breast or Nipple Pain?
During Feedings
- Nurse first on the side that's less sore and vary breastfeeding positions.
- Make sure your baby latches onto your breasts correctly. If breastfeeding is too painful, it may be more comfortable to drain your breasts by pumping the milk.
- If you have sore nipples, ask a lactation consultant or your health care provider if a nipple shield is a good idea. Nipple shields go over the areola and nipple during a feeding to protect sore or cracked nipples. They should only be used when recommended by your care team as they can sometimes affect milk supply.

- Gently break the suction when removing your baby from your breast. Slip your finger in the side of your baby's mouth, between the gums, and then turn your finger a quarter turn to do so.
- At the end of a feeding, massage some breast milk onto your nipples, and then let them air dry.
Between Feedings
- Gently massage the sore area before nursing.
- Use wet or dry heat on your breasts (a warm shower, water bottle, heating pad, or warm washcloth) right before feeding. But if you have a yeast infection in your breast, you'll need to keep your nipples dry because yeast thrives on moisture. Get plenty of rest and fluids.
- Put ice packs or cool compresses on engorged breasts after feedings.
- Make the area where you feed your baby comfortable. Sit in a glider or a cozy chair with armrests. Footstools and pillows can give extra support. Some women like wraparound nursing pillows or "husband" back pillows with arms on each side for nursing in bed.

If breastfeeding is painful or uncomfortable for you, callyour doctor or lactation consultant for help.
Why does my breast hurt when I feed
Mammology
Breastfeeding gives a young mother pleasure and helps to realize the happiness of motherhood. In cases where the chest hurts after feeding, it is necessary to immediately make an appointment with a mammologist in order not to miss the development of serious diseases in the earliest stages.
Causes of chest pain during feeding.
response to the release of the hormone oxytocin. Under its influence, there is a strong contraction of the muscle fibers of the lactiferous passages, as a result of which an additional portion of milk is released. nine0003
Mothers feel pain at this time, which they characterize as squeezing or stabbing. In nulliparous or emotionally labile women, the reflex to oxytocin can manifest itself even at the mere thought of a child or at the moment when she takes the baby in her arms. Usually, after three months of lactation, this reaction gradually weakens.
Usually, after three months of lactation, this reaction gradually weakens.
Laktostasis. Very often, the chest of a nursing mother hurts when, due to poor patency of the milk ducts, thick milk or a very large amount of it, stagnation occurs in the milk lobules. At the same time, painful seals are felt in the mammary gland. The skin above them may be warmer and bluish due to venous congestion. With lactostasis, it is imperative to express the breast so that the seals disappear. Otherwise, mastitis can quickly develop. nine0003
Rapid breast filling with milk. During active sucking, in response to irritation of the nipple of the mammary gland, a large amount of the hormones prolactin and oxytocin are released, which stimulate the production of a new portion of milk. In such cases, not only does the chest hurt after feeding, but it also quickly fills with milk, swells and thickens. This phenomenon indicates the normal process of lactation.
Thrush. With candidal stomatitis in an infant, colonies of the fungus can penetrate the skin of the nipple of the mother's breast, and then into the milky passages with the development of thrush. At the same time, the colonies of the fungus are practically invisible, and the main clinical sign is the increased sensitivity of the nipples. Cutting or piercing stabbing pain, itching in the mammary glands are not cured by the usual antiseptics. It is very characteristic that the chest of a nursing mother hurts more precisely after the end of feeding. nine0003
With candidal stomatitis in an infant, colonies of the fungus can penetrate the skin of the nipple of the mother's breast, and then into the milky passages with the development of thrush. At the same time, the colonies of the fungus are practically invisible, and the main clinical sign is the increased sensitivity of the nipples. Cutting or piercing stabbing pain, itching in the mammary glands are not cured by the usual antiseptics. It is very characteristic that the chest of a nursing mother hurts more precisely after the end of feeding. nine0003
Mastitis. As a result of inflammation of the area of lactostasis or when pathogenic microbes penetrate through the fissures of the nipple into the lactiferous lobule, a serous and then purulent process occurs, manifested by severe throbbing pain. The skin over the pathological focus becomes red and hot, often the body temperature rises. The mother needs urgent help from a gynecologist and a surgeon, as in advanced cases, an abscess of the mammary gland quickly develops.
Teat cracks due to improper technique of attaching the baby to the breast during feeding. The pain in the chest is most pronounced during feeding, and after it gradually subsides.
Compression of the chest by an incorrectly fitted bra, during prolonged exposure to an uncomfortable body position (for example, while sleeping on the stomach). In any case, do not delay the visit to the doctor, only he will be able to establish the correct cause of the pain and give the necessary recommendations or prescribe treatment.
More articles on this topic
Laktostasis in a nursing mother
The disease occurs when breast milk cannot pass through the ducts of the mammary gland due to their blockage. It is produced, but cannot go outside. Because of this, pain may occur.
Mammology
Breast cancer
Unfortunately, today many women suffer from breast cancer. This is a malignant formation. In most cases, this disease occurs in women over 40 years of age. However, he occasionally visits teenage girls. nine0003
This is a malignant formation. In most cases, this disease occurs in women over 40 years of age. However, he occasionally visits teenage girls. nine0003
Mammology
Laktostasis
This is a stoppage of milk flow from the milk ducts. As a result of this phenomenon, the formation of milk stagnation occurs. Peripheral tissues become compacted and edematous. Places of compaction turn red and become painful.
Mammology
ᐈ Breast pain during GV (breastfeeding) • Induration in a nursing mother
“Advise a mammologist!”
If you are a breastfeeding mother, you probably don't have much time. The child “hangs” on the chest, you get tired like never before in your life, you don’t often manage to sleep normally. What to say about the "campaigns" to the doctors. nine0003
It's much easier to go online, type in a symptom in a search engine, ask for advice on the mommies forum.
However, who guarantees that the advice will be correct and the condition will not worsen? The mammologists of our center understand your concerns and are ready to solve all the issues that arise with breastfeeding mothers.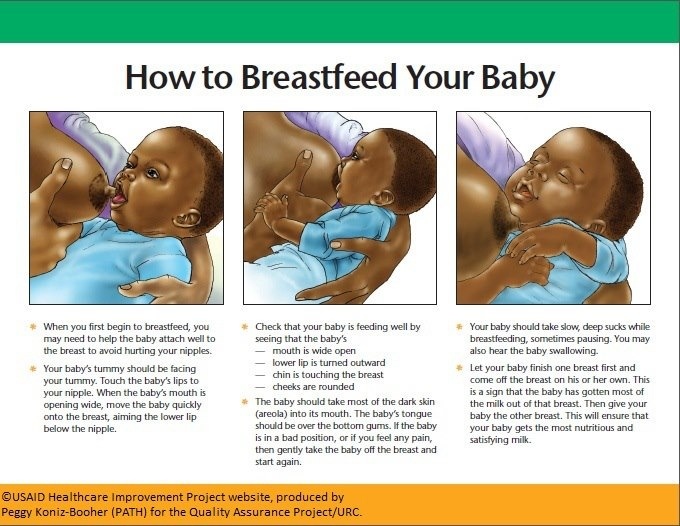
You are breastfeeding. What's going wrong?
Not enough milk
| You think you don't have enough milk. |
| Violation of the rhythm of feeding, improper attachment, overwork. |
| The child is restless, gains or loses weight poorly. |
| Breastfeed more frequently, consult a mammologist and lactation consultant. nine0087 |
Too much milk
| | You think there is too much milk. |
| Individual features, excess prolactin. |
| Too much milk is produced. |
| Change the rhythm of feeding, freeze excess milk, consult a mammologist and endocrinologist. |
Teat fissure
| Pain during feeding, skin defect, blood. |
| Heavy workload, slow recovery. |
| Restrict feeding to this breast for the duration of treatment, express adequately when filling, consult a physician for anti-inflammatories, antibiotics and physiotherapy as indicated. |
Milk stasis
| What's bothering you? | Pain and distension in the chest. |
| Possible causes? | Ejection of milk is uneven in different parts of the gland, there is no muscular wall in the milk ducts, and the outward movement of milk is also uneven. The ducts may be compressed or twisted. |
| How does it manifest itself? | Painful, tight-elastic lump in the breast, does not disappear after feeding, without fever and redness. nine0087 |
| What to do? | Change position during feeding, pumping, applying ice, contacting a mammologist, doing ultrasound, microflora culture (bacteria culture), secretion cytology |
| What worries you? | Depends on the stage - first, a painful focus of compaction, a decrease in the amount of milk, an increase in body temperature up to 38 degrees. nine0002 Further, the focus increases, there is swelling of the skin, axillary lymph nodes, high temperature, impurities in the milk. Further, redness joins, swelling increases, weakness, drowsiness, palpitations, the amount of impurities increases. |
| Possible causes | Unemptied stagnation, curdling of milk and clogging of the duct, penetration of infection through cracks leads to mastitis. |
| How does it manifest itself? | Depends on the stage - painful, stony density, swollen gland, redness of the skin, increased body temperature, symptoms of general intoxication, lactation is sharply reduced. nine0087 |
| What to do? | Seek immediate medical attention, often requiring hospitalization and surgical treatment. |
There is a lump in the chest, it does not hurt
| What worries | Abruptly appeared soft and painless mass in the mammary gland, the condition is not disturbed. |
| Possible causes | Lactocele is an acute accumulation of milk in an overstretched duct.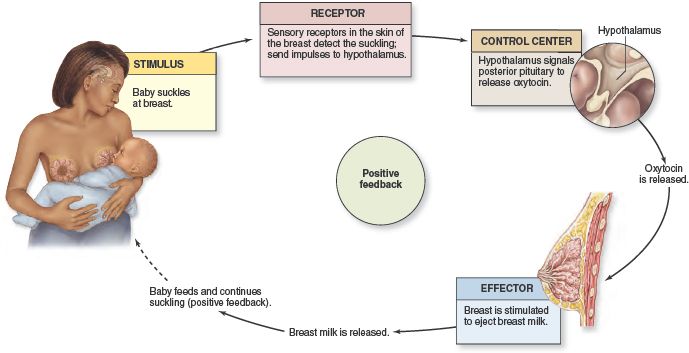 nine0087 nine0087 |
| How it manifests itself | The formation is soft-elastic, painless, appeared acutely, lactation is preserved. |
| What to do | Contact a mammologist, you need ultrasound, aspiration of contents with cytology. |
Breast lump, spotting
| Painless, firm mass without clear contours in the presence of normal lactation. Enlarged axillary lymph nodes on one or both sides. Bloody discharge from the nipples of one or both glands. nine0003 | |
| Possible causes? | Suspicion of an oncological process due to hormonal changes during lactation. |
| How does it manifest itself? | The formation is dense, painless, axillary lymph nodes are enlarged, lactation is preserved, there is bloody discharge from the nipple. |
| What to do? | Contact a mammologist, you need ultrasound, mammography, biopsy, cytology, histology, comprehensive examination. |
How not to waste a breastfeeding mother's precious time? The CMC offers:
• Consultations of a competent mammologist with more than 15 years of experience with nursing mothers.
• Assistance in organizing breastfeeding - for ordinary issues we involve our consultant, in difficult situations - with the participation of our mammologist.
• Complete examination in 1-2 visits – we perform ultrasound, mammography, cultures, cytology and histology. nine0003
• Treatment of breastfeeding according to world standards: we perform therapeutic fine needle biopsy, therapeutic massage and pumping for lactostasis, conservative and surgical treatment.
1. What should a breastfeeding mother eat?
It is best if your diet is complete, balanced in proteins, fats and carbohydrates.